Oxygen Therapy. Skinny Little Reference Guide
|
|
|
- Homer Waters
- 6 years ago
- Views:
Transcription
1 Oxygen Therapy Skinny Little Reference Guide
2 This single topic brochure is one of a series extracted from AlphaNet's Big Fat Reference Guide to Alpha-1 (the BFRG), which is available on the AlphaNet website ( Copyright AlphaNet, Inc. 2007
3 OXYGEN THERAPY INTRODUCTION Supplemental oxygen administration may become necessary as an element of the treatment plan in Alpha-1 COPD. As lung destruction progresses, the ability of the lungs to exchange oxygen becomes impaired, resulting in a condition known as hypoxemia, where the levels of oxygen in the blood are lowered. The long-term effects of hypoxemia can be detrimental and life-threatening. KEY LEARNING: Under normal circumstances, the body's drive to breathe is in response to the carbon dioxide levels in the blood. The brain cannot detect low oxygen levels. EFFECTS OF LOW OXYGEN Inadequate levels of oxygen have an effect on a number of systems in the body. In the lungs themselves, a lowered concentration of oxygen in the blood causes the vessels of the lungs to constrict. This results in increased blood pressure in the arteries feeding the lungs known as pulmonary hypertension and also causes the heart to pump harder and strain to get blood through the lungs. Over time, this strain can cause the heart to dilate and weaken, and eventually fail. Known as Cor Pulmonale, this right-sided heart failure can be directly caused by lung disease. Inadequate oxygen levels can lead to an increase in the number of circulating red blood cells in the body. It is the red blood cells, specifically the hemoglobin, that transport oxygen throughout the body. This proliferation (large number of the red blood cells, known as polycythemia), is the body's way of attempting to deliver more oxygen to the tissues and cells. In some individuals, the increased volume of circulating red blood cells can cause blood clots, headaches, and elevated blood pressure. 1
4 CROSS REFERENCE: For definitions of many of the medical terms used in this brochure, you can refer to the Glossary of Terms in the Big Fat Reference Guide at Hypoxemia also can adversely affect brain function and physical capabilities. Attention span and the ability to concentrate may be diminished, along with memory and mood. The ability to utilize abstract reasoning and problem-solving skills can be impaired. Speech may become affected, and simple sensory and motor skills may become problematic. Being able to perform more complex tasks that require gross and fine motor skills can be adversely affected; for instance, driving a car, performing specific tasks of a job, and operating equipment. Poor tolerance to exercise, muscle weakness, and impaired coordination also can be seen. Severe hypoxemia is life-threatening, and can ultimately lead to delirium, coma, and death. BURNING ISSUE: Severe hypoxemia is life-threatening, and can ultimately lead to delirium, coma, and death. BENEFITS OF OXYGEN ADMINISTRATION It is well-documented that the administration of oxygen therapy can reverse the negative effects of hypoxemia and significantly improve survival. Furthermore, clinical studies among individuals with severe COPD have shown a direct correlation between these beneficial effects and the number of hours per day that oxygen therapy is administered. For example, one study compared the health outcomes for patients who received 12 hours of oxygen therapy per day with those who received 19 hours of oxygen therapy per day. This study showed that the negative effects of hypoxemia on the pulmonary vasculature were reversed and survival rates were increased for both groups of patients. However, these beneficial results were even more dramatic for the patients who received longer daily oxygen administrations. GOOD NEWS: In COPD studies, patients with hypoexemia and Cor Pulmonale, have shown treatment with long-term oxygen therapy increased the life span of these individuals by as much as six to seven years. 2
5 Perhaps of greatest importance to the daily life of individuals needing supplemental oxygen, correcting hypoxemia allows increased activity and exercise levels with less shortness of breath. The improvement in shortness of breath with activity is not directly due to the higher oxygen levels in blood but rather to the ability of muscle to continue to use oxygen as fuel without changing to the anaerobic metabolism that it uses when oxygen levels drop too low. Anaerobic metabolism generates much more carbon dioxide in the blood than muscle activity that uses oxygen, called aerobic metabolism. It is the blood s carbon dioxide level that controls the amount of shortness of breath that someone notices. Using supplemental oxygen allows people to exercise longer and harder, leading to better overall fitness and muscle efficiency. Oxygen therapy also helps to restore impaired cognitive capabilities (the ability to think and remember), mental alertness, physical stamina, mood, and the ability to achieve restful sleep. Truly, the benefits of oxygen therapy are numerous and profound. EVALUATING HYPOXEMIA The most accurate method for determining the presence of hypoxemia is a test of "arterial blood gases," also called ABGs. In addition to measuring the oxygen level found in the blood, this test also provides levels for carbon dioxide and other elements, such as blood ph and bicarbonate. The level of carbon dioxide found in the blood is an important factor a physician will consider when recommending the use of supplemental oxygen. Bicarbonate and blood ph levels show how the body may have compensated for any imbalances between oxygen and carbon dioxide levels, and provides further evidence regarding the severity of these imbalances. An ABG test, which involves taking a small sample of blood from the artery in your wrist or from the inner curve of the elbow, is generally used to establish your "baseline" condition. Pulse oximetry is another method for evaluating oxygen saturation of the blood, and is generally used for ongoing evaluations after a "baseline" has been determined. The pulse oximeter is a device that clips onto a fingertip or ear lobe, which is able to "read" the oxygen level directly through the skin. This device is easy to use by anyone, and does not require the assistance of medical personnel. The difference between the results from oximetry and ABG analysis is that oximetry is only able to measure the percentage of the blood that is satu- 3
6 rated with oxygen (percent oxygen saturation). It does not provide the levels for carbon dioxide or for any of the other blood components. Pulse oximetry also differs from an ABG test in that it does not require puncture of the skin. Sometimes determination of the need for supplemental oxygen is made during a hospital stay, when hypoxemia is present due to an acute infection or a pulmonary exacerbation. In these instances, reassessment of the need for supplemental oxygen is recommended after one to three months, since ongoing oxygen therapy may no longer be needed. Once the need for long-term oxygen therapy is established, pulse oximetry may be used routinely to reassess the individual's oxygen needs whenever there is a change in the clinical status or a change in the oxygen prescription. Pulse oximetry can be easily performed and the results are immediately available. It does not require lab analysis, and it can be performed in various settings. For example, if symptoms of hypoxemia develop during exercise or are suspected of occurring during sleep, your physician may want to monitor you under theses conditions. Pulse oximetry can be conducted while you exercise on a treadmill or stationary bicycle, and oxygen saturation can be evaluated during sleep with the use of a portable oximeter and recording device. CRITERIA FOR SUPPLEMENTAL OXYGEN THERAPY Specific blood test criteria have been established for prescribing oxygen therapy and for determining the reimbursement of its costs from Medicare and other third-party payers. The criteria, developed by medical experts, establishes oxygen blood levels that warrant the use of supplemental oxygen. These guidelines describe three specific conditions that necessitate the use of oxygen therapy. When looking at your test results the following information might be helpful: 1. PaO2 is less than or equal to 55 mmhg or hemoglobin oxygen saturation (SaO2) is less than or equal to 88 percent when breathing room air while at rest. 2. PaO2 of mmhg or if SaO2 is equal to or less than 89 percent when associated with specific clinical situations (such as cor pulmonale, congestive heart failure, or polycythemia with a hematocrit of greater than 56 percent). 3. Some individuals do not qualify for oxygen therapy while at rest, but may require supplemental oxygen while walking, exercising, or during sleep. 4
7 Oxygen therapy is indicated in these situations when the SaO2 falls to less than or equal to 88 percent. Also, in order for the costs of supplemental oxygen to be covered by insurance, third-party payers require evidence that the oxygen therapy utilized during exercise or sleep actually improves the individual's hypoxemia. CROSS REFERENCE: To learn more about how to interpret these test results, see the section "Understanding Diagnostic Test Results" in the Big Fat Reference Guide at OXYGEN PRESCRIPTION Your oxygen prescription is written by your physician and should address the use of oxygen at rest, during exercise, and during sleep. Make note that your prescription may include different flow rates for rest, exercise, and sleep. The prescription should indicate the type of oxygen system, the flow rate expressed in liters per minute, and the duration in terms of number of hours per day. The prescription also should include the diagnosis of the disease requiring the use of oxygen therapy, such as Alpha-1 COPD. ACCEPTANCE OF THERAPY For many individuals, the confirmation of the need for oxygen therapy can precipitate feelings of uncertainty, loss, frustration, and fear. Despite the recommendations from their physician, some choose not to comply with the recommendations for therapy. Generally, objections have to do with the individual's perception of how others will react to them. Feelings of appearing to be unacceptable, or of being viewed as "handicapped" are not unusual. CROSS REFERENCE: We talk more about your feelings concerning oxygen therapy in "Coping with Alpha-1 Lung Disease." in the Big Fat Reference Guide at 5
8 Further objections to the use of supplemental oxygen relate to the inconvenience of having to be tethered to an oxygen tank, and the impositions made on lifestyles and plans. Denial and fear of facing the seriousness of the illness, as well as being pressured to come to terms with living with a chronic and progressive condition, also may have an impact on compliance with therapy. Some individuals rationalize they do not want to use supplemental oxygen because they are afraid they will become "addicted" to it. Ironically, by refusing to comply with the prescribed therapy, these individuals may bring about the events they are trying to avoid. If you have been prescribed oxygen therapy, you will want to become well-informed about its benefits, as the benefits are welldocumented and have measurable and appreciable positive effects. When these positive effects are compared with the limitations imposed by feeling fatigued, out-of-breath, and in general, just not feeling well, you may feel that the benefits far exceed your concerns and fears about oxygen therapy. BURNING ISSUE: By refusing to comply with prescribed supplemental oxygen therapy, individuals may bring about the events they are trying to avoid. For those individuals who may be contemplating lung transplantation, acceptance of oxygen therapy as a pre-transplant regimen will be vital for counteracting the effects of ongoing hypoxemia and will help to preserve cardiac function. CHOOSING A HOME THERAPY PROVIDER Before choosing an oxygen delivery system that will meet your needs, you must first choose a company to provide that service. Many companies specialize in providing home care and durable medical equipment. Begin by checking with your health insurance provider, as they may have contracts with specific companies in your area. If you have freedom of choice, the key is to shop for service. Generally, each company provides similar products and systems, but it is their ability to provide exceptional service that can make all the difference. Getting information and feedback from others you may know who are presently receiving oxygen therapy can be helpful. Then, call various companies and compare their services and prices before you make your final decision. Some common questions you might have for these companies are: 6
9 Are you a national company, and how many branches do you have? Where are your branches located? What systems can you provide? What influences the decision to provide one system over another? (Sometimes they may only offer those systems that are more profitable for them.) How often are deliveries made? Will you help make arrangements for oxygen delivery if I should decide to travel? What is the response time in case of an emergency? What is the turn-around time to replace defective equipment? How often will the respiratory therapist come to my home? How often will equipment be checked and/or serviced? What about reimbursement? How much will this cost me? What if I choose to purchase the system? Will you still provide service? Do you have any customer testimonials? Are you licensed and accredited? By which organizations? For example, are you licensed by the individual state, and have you been accredited by Medicare/Medicaid and/or by the Joint Commission on Accreditation of Health Organizations (JCAHO ) (Medicare/Medicaid and JCAHO provide standards that must be adhered to in order to achieve and maintain accreditation.) CHOOSING A SYSTEM Individuals with Alpha-1 COPD are encouraged to remain as active as possible, despite the need for and use of supplemental oxygen. Advances in technology have provided for a variety of systems that can help those requiring oxygen meet their specific need for maintaining an active and healthy lifestyle. Your goal for choosing a system will be to find one that will meet your specific needs for mobility and portability, as well as be efficient and cost-effective. It is important to discuss with your physician and home therapy provider your needs and individual situation. View your choice for home oxygen as you would for selecting any major home appliance. Ask lots of questions. You may have more options to choose from than you realize. Consider all the choices, think about what your specific needs are, and then select the system or systems that will be the best fit for you. 7
10 Equipment associated with home oxygen therapy has two essential components: The container or storage system which holds the oxygen whether compressed gas, liquid, or from a concentrator The delivery system that transports the oxygen from the container into your lungs We discuss a number of the available options for each of these types of components below. Storage Systems There are two types of storage systems: stationary and portable. As new technology has been developed, combined systems offering more flexibility and portability have been made available. As you will see, some of the storage systems also may be used to fill portable systems combining both types. We will highlight the most common systems currently available. Stationary systems Stationary systems provide a large source of oxygen, but restrict movement. The most common and most economical in-home stationary system used is an oxygen concentrator. Concentrators use an electric motor and work by removing nitrogen from room air to make percent oxygen. An oxygen concentrator requires an electrical source, and operates by passing room air through a powder or a membrane to separate oxygen from nitrogen. The oxygen is concentrated and delivered while the nitrogen is periodically released back into the air. Stationary concentrators can be fairly small, weighing anywhere from pounds, and can achieve a liter flow rate of up to five to six liters per minute. A long supply tubing of approximately 50 feet in length is needed to allow for maneuvering around the house and preventing tangles with furniture. Since these systems require a source of electricity, you also will want to have a back-up oxygen supply in case a power failure occurs. These units must be placed in a well-ventilated area and kept away from heat and flames. Concentrators need routine maintenance for inspections, filter changes, and oxygen analysis. Some of the newer models provide an oxygen concentration indicator which measures the oxygen level administered by the concentrator and sounds an alarm if the reading falls below a certain level. Another stationary system is a reservoir for liquid oxygen. Liquid oxygen is gas condensed into a liquid state by extreme cold. Liquid systems have a large reservoir tank which is filled by the oxygen supplier once or twice a month. 8
11 These systems require no electricity, have very few moving parts, and require little maintenance or repair. When dealing with liquid oxygen, caution must be exercised to prevent spills, because liquid oxygen is extremely cold and can injure the skin immediately upon contact. A typical liquid oxygen reservoir weighs 124 pounds when filled and contains 31 liters, or 73 pounds, of liquid. This amount of liquid oxygen is equivalent to 24,950 liters of oxygen in the gas form. At a flow rate of two liters per minute, this amount of oxygen would last 208 hours, or eight days. Because liquid systems continually lose oxygen through evaporation, even when not in use, they are appropriate for regular use at home, or for filling up portable units. They are not suitable as an emergency back-up system. Newer units are now available that reduce the amount of oxygen that is lost into the air, along with improvements in size and stability. Many of these systems also have builtin pulsed delivery or conserving devices. Compressed gas oxygen in large tanks or cylinders is another example of a stationary system. Large steel or aluminum tanks (H, S, and M60 styles), are heavy, cannot be moved easily, and must be safely secured to prevent them from falling over. They are not appropriate for someone who requires continuous-flow oxygen, due to the volume that would be required to meet a continuous need and the prohibitive cost. This system is better suited as a back-up system for a concentrator. Portable systems Oxygen concentrators were once thought of only for individuals who were homebound and relatively inactive. Newer and lighter-weight models have been developed for portable use with electrical capabilities for automobiles and are also outfitted with battery packs. There are even newer concentrators presently available that fill portable cylinders at home, providing accessibility and convenience. This type of concentrator not only compresses oxygen to fill the cylinders, but also provides continuous-flow oxygen for breathing. Small portable liquid oxygen units can be easily filled from the large liquid reservoirs using a direct connection between the two. A small portable unit that has been equipped with a conserving device can allow you to spend longer intervals away from the home and promote a more active lifestyle. This combination of a portable unit/conserving device also can serve as a base reservoir that can be filled at less frequent intervals. A discussion of conserving devices is presented later in this chapter. 9
12 Compressed gas in smaller cylinders can provide portability as well. The following listing outlines the amount of time a given cylinder size would last at a rate of two liters per minute without a conserving device. If a conserving device is used, these time frames would be extended: E-cylinder: up to five hours D-cylinder: up to three hours M9: up to two hours M6: up to one hour E-cylinders are the most common size used as back-up for individuals using concentrators. These cylinders can be easily wheeled on a cart or a stroller, and they weigh about 20 pounds. Smaller tanks can be carried in backpacks, fanny packs, or shoulder bags. Each cylinder is fitted with a regulator that is used for adjusting the flow rate. At a rate of two liters per minute, they only last a few hours. E-cylinders are not appropriate as a sole source of oxygen for continuous, long-term therapy. IT S A FACT: You should be aware that Medicare covers the cost of portable systems only if they are needed for mobility within the home, not for away-from-home activities. Most people use a combination of storage systems as a means for achieving the most economical supply of oxygen, and for promoting an active and full lifestyle. OXYGEN DELIVERY SYSTEMS Oxygen delivery system options include: Nasal cannulas Transtracheal catheters Pulsed delivery systems Face masks Oxygen-conserving devices 10
13 Nasal cannula Low-flow, dual-pronged nasal cannulas are the standard delivery device most people use at home. The nasal cannula is a piece of plastic tubing connected to the oxygen source that ends in two small prongs that rest in the nostrils. The tubing leading to the nostrils rests on the ears. Oxygen is delivered via continuous-flow from the container, which is diluted with room air before it enters the lungs during inspiration. The nasal cannula can provide percent inspired oxygen concentration (FIO2), depending on the oxygen flow rate and the person's respiratory demand. This device is simple, inexpensive, and can be used with flow rates of up to six liters per minute. Keep in mind that humidification is recommended for flow rates greater than four liters per minute as continuous oxygen flow can be drying to the nasal mucous membranes. Humidification also may be necessary at lower flow rates when the climate is dry. The disadvantage of this device is that oxygen is delivered throughout the respiratory cycle, during both inspiration and expiration, which is neither efficient nor cost-effective. Face mask For some individuals, a face mask may be required to deliver a higher concentration of oxygen if ordered by the physician. The mask is made of plastic and fits snugly over the mouth and nose. This device is not always practical for longterm and in-home use, as it is somewhat uncomfortable and can make speaking difficult. The mask also must be removed for eating and drinking. Transtracheal oxygen Transtracheal oxygen (TTO) catheters can provide effective continuous oxygen therapy, even to patients who require extremely high-flow oxygen. This delivery device involves the insertion of a catheter through the skin of the neck into the windpipe (trachea) just below the Adam's apple (vocal cords and larynx). Oxygen enters the trachea via this catheter. Individuals who choose this method of oxygen delivery generally have a strong desire to remain active and are willing to follow specific self-care instructions. This method can be more cosmetically appealing for some people and can help reduce dyspnea during eating. Since the oxygen is being delivered directly into the trachea, and is not diluted by room air, TTO can deliver the required amount of oxygen therapy using a reduced oxygen flow rate. For example, an individual on a flow rate of two liters per minute via nasal cannula might require a flow rate with TTO of one liter per 11
14 minute. That represents a 50 percent reduction in cost, and a significant increase in the length of time a tank of oxygen would last before needing to be refilled. With the addition of a conserving device, even greater efficiency and savings could be realized. KEY LEARNING: Transtracheal oxygen is not recommended for individuals who require chronic high-dose steroids, since these medications can mask infections and delay the healing process. This method of oxygen delivery is for individuals who have infrequent exacerbations, and who have a caregiver who is willing to participate in their care and problem-solving. Complications of transtracheal oxygen are infrequent and generally mild if the patient is compliant with the care instructions. Complications include: catheter displacement, bacterial cellulitis, and coughing-up blood (hemopytsis). In addition, mucous balls can develop due to the dryness of oxygen, increased sputum production, and from poor adherence to cleaning procedures. OXYGEN CONSERVING DEVICES The primary goal of oxygen-conserving devices is to improve portability and comfort by reducing the size and weight of the oxygen system that you carry around. Furthermore, the reduced frequency of replacing or refilling tanks and cylinders also reduces the overall cost of therapy. Reservoir cannulas Reservoir cannulas operate by storing oxygen in a small chamber during exhalation, which is then delivered during inhalation. They are driven by the person's own inspiratory and expiratory effort, and are generally used for individuals who require higher flow rates to achieve adequate oxygenation. These devices are available in several different configurations. The Oxymizer and the Pendant are two examples of these devices. Overall oxygen consumption is decreased through reduced-flow settings, generally by 25 to 50 percent of traditional continuous-flow nasal cannulas. Although these cannulas are simple to use, reliable, and economical, their particular disadvantage is that they tend to be large and more noticeable. 12
15 Pulsed delivery devices Pulsed delivery devices function by delivering a small amount of 100 percent oxygen at the onset of early inhalation. The device is interposed between the user and the oxygen source, and can be a separate unit or built right into the oxygen reservoir. Because oxygen delivered during early inspiration reaches the alveoli, this device is very effective in promoting oxygenation. An additional advantage is that when individuals exercise and increase their respiratory rate, the amount of oxygen delivered increases as well, since the pulsed delivery follows each inspiration. (This does not apply, however, to a fixed-pulse device or fixed-setting.) These devices sense the start of inhalation either by electronic means or by pressure changes that can be pre-set for specific demands. A fixed-pulse device can be set to deliver oxygen at a set rate along with each breath, or it can be programmed to skip one or more breaths. A demand-pulse device can deliver oxygen throughout inspiration or only during a part of the phase. This device is capable of adjusting to changes in demand. A variable-demand device can deliver oxygen that is adjusted to the rate and length of each inspiration. A physician's prescription is required for the use of these devices, and they must be evaluated under various conditions (i.e., rest, exercise, and sleep) to assure the device is able to meet your specific needs and maintain adequate oxygenation. In general, pulsed devices are not recommended for use during sleep because they may have trouble detecting shallow nighttime breaths. You should be trained on how to operate the system and trouble-shoot if problems arise. Each system should be equipped with a fail-safe mode, where it can be set to full and continuous oxygen flow in the event the device malfunctions or fails. INSURANCE COVERAGE AND COST OF THERAPY The American Lung Association estimates more than one million Americans use home oxygen on a long-term basis. Home oxygen therapy represents a significant national health expenditure, totaling more than one billion dollars annually. It is the most expensive non-surgical treatment reimbursed by Medicare. Home oxygen therapy and related equipment is covered under the durable medical equipment (DME) benefit of the Medicare program. 13
16 GOOD NEWS: Home oxygen therapy is the most expensive non-surgical treatment reimbursed by Medicare. Medicare's payment rules for home oxygen provide for a monthly payment that covers the oxygen equipment and all necessary supplies. Currently, the typical monthly cost is $300. Medicare and most private insurers pay 80 percent of this cost (approximately $240), and the individual or secondary insurers would pay the remaining 20 percent (approximately $60 per month). Although private insurance coverage varies, many companies follow Medicare's guidelines for reimbursement. You should check with your individual insurance company for its rules for coverage and reimbursement practices. It is important to understand that even though your physician may prescribe a specific system for you, your supply company may be challenged to provide that particular system if they receive inadequate reimbursement. Many supply companies may want to supply you with a system that is less costly for them, and one for which they obtain adequate reimbursement from third-party payers. Negotiations between you and the supply company, as well as your physician, may be necessary to resolve these kinds of issues. In general, liquid oxygen systems tend to be more expensive to provide and maintain for service providers, expenses for which they may not be completely reimbursed. Since 1997, cuts to Medicare reimbursement for oxygen therapy have totaled 30 percent, and further reductions in reimbursement rates are likely to occur at some point in the future. These cuts threaten the health and safety of many affected individuals by jeopardizing their ability to pay for and to access services. You may want to familiarize yourself with the issues and become involved in seeking legislative remedies for this problem. By petitioning legislators through letters, phone calls, faxes, or s, further reductions may be stopped or rolled-back so that this life-sustaining therapy can be made more readily available. DIG IN: You may want to familiarize yourself with these Medicare legislative issues and become involved in seeking remedies. 14
17 OXYGEN SAFETY Our discussion of oxygen therapy would not be complete without mention of specific recommendations for the safe use of oxygen. The potential for fire hazard in the presence of oxygen is well-known, although sometimes forgotten or overlooked. In addition, there are some seemingly benign hazards in the home, which can be eliminated by instituting a few simple precautions to create a safe home environment in the presence of oxygen use. Oxygen canisters should be kept at least 5-10 feet away from gas stoves, lighted fireplaces, woodstoves, candles, or other sources of open flames. Do not use electric razors (a possible source of sparks) while using oxygen. Do not use any oil, grease, or petroleum-based products on the equipment, or near you while you use supplemental oxygen, as these materials are highly flammable and will burn readily with the presence of oxygen. Avoid petroleum-based lotions or creams, like Vaseline, on your face or upper chest. Check the ingredients of such products before purchase. If a skin moisturizer is needed, consider using cocoa butter, aloe vera, or other similar products. If lubrication or rehydration is needed for dry nasal passages, there are waterbased products available which your pharmacist or care provider can recommend. Post signs in every room where oxygen is in use, and make sure that absolutely NO SMOKING occurs in the home or in the car when oxygen is in use. Secure an oxygen cylinder to a solidly fixed object to avoid creating a missile out of the tank if it were accidentally knocked over and gas were allowed to escape. Use caution with oxygen tubing so you do not trip over it or become entangled in furniture. Be familiar with the equipment and the safety checks established by the home medical equipment provider. Keep their contact telephone numbers, and the numbers for other emergency services, posted near a phone. Do not attempt to repair broken equipment on your own. Request this service from the oxygen equipment provider. Make sure smoke detectors in the home are working and have fresh batteries installed; perform monthly checks. Have a fire extinguisher, (type ABC) available in the home as well. Develop and practice an escape and rescue plan in the event of a fire. Notify the local fire department, gas and electric companies, and telephone company when home oxygen therapy is instituted. Request a "priority service listing" in the event of a power or telephone failure, or if repairs are necessary on any utility. 15
18 BREATHE EASIER AND LIVE LONGER Supplemental oxygen therapy may become necessary to provide adequate oxygenation when lung function has declined and hypoxemia results. The benefits of oxygen therapy are well documented, and are known to reverse the ill effects of hypoxemia and prolong lifespan. Although there are challenges with therapy, today's oxygen systems are efficient and portable. Your understanding of the need for oxygen and your compliance with therapy is one of the most important ways in which you can manage your lung disease and continue to promote a healthy lifestyle. 16
19 This brochure is produced by AlphaNet as part of its Alpha-1 Disease Management and Prevention (ADMAP) program. AlphaNet is a not-for-profit organization providing disease management services and support to individuals affected by Alpha-1 through a staff of medical professionals and specially trained AlphaNet Coordinators, available 24 hours a day, 7 days a week. To learn more about ADMAP or to find the AlphaNet Coordinator nearest you, visit our website (
20
Oxygen Therapy. COPD Foundation s Slim Skinny Reference Guide (SSRG)
 Oxygen Therapy COPD Foundation s Slim Skinny Reference Guide (SSRG) Oxygen Therapy Ver2.1 BIG FAT REFERENCE GUIDE (BFRG) on Chronic Obstructive Pulmonary Disease (COPD) lu d SR I nc Gs ated Upd23-12 10es
Oxygen Therapy COPD Foundation s Slim Skinny Reference Guide (SSRG) Oxygen Therapy Ver2.1 BIG FAT REFERENCE GUIDE (BFRG) on Chronic Obstructive Pulmonary Disease (COPD) lu d SR I nc Gs ated Upd23-12 10es
On the Go with Oxygen
 On the Go with Oxygen People with chronic lung disease may need oxygen therapy. Oxygen therapy is used to normalize the oxygen level in blood during sleep, rest, activity and during acute illnesses in
On the Go with Oxygen People with chronic lung disease may need oxygen therapy. Oxygen therapy is used to normalize the oxygen level in blood during sleep, rest, activity and during acute illnesses in
Oxygen Therapy. Respiratory Rehabilitation Program. What is oxygen?
 Respiratory Rehabilitation Program What is oxygen? Oxygen Therapy Oxygen is a colourless, tasteless, odorless gas that you need to live. Oxygen is found in the air you breathe at a concentration of 21%.
Respiratory Rehabilitation Program What is oxygen? Oxygen Therapy Oxygen is a colourless, tasteless, odorless gas that you need to live. Oxygen is found in the air you breathe at a concentration of 21%.
OXYGEN THERAPY. Teaching plan
 OXYGEN THERAPY Teaching plan To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may give each learner a copy of the
OXYGEN THERAPY Teaching plan To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may give each learner a copy of the
Oxygen Therapy. What tests can be done to determine the need for oxygen?
 Oxygen Therapy Oxygen is in the air we breathe and is necessary to live. When we breathe in, oxygen enters the lungs and it goes into the blood. When the lungs cannot transfer enough oxygen into the blood,
Oxygen Therapy Oxygen is in the air we breathe and is necessary to live. When we breathe in, oxygen enters the lungs and it goes into the blood. When the lungs cannot transfer enough oxygen into the blood,
Breathe easier. Patient guide to oxygen therapy
 Breathe easier Patient guide to oxygen therapy Table of contents The facts about COPD The facts about COPD 3 Understanding oxygen therapy 4 Choices in oxygen therapy equipment You have been prescribed
Breathe easier Patient guide to oxygen therapy Table of contents The facts about COPD The facts about COPD 3 Understanding oxygen therapy 4 Choices in oxygen therapy equipment You have been prescribed
Home Oxygen Therapy Patient Handbook
 Home Oxygen Therapy Patient Handbook Office Hours 8:30 a.m. to 5:00 p.m. Monday-Friday Emergency Answering Service 24 hours a day, 7 days a week Birmingham Office: (205) 981-2333 5025 Highway 280 Suite
Home Oxygen Therapy Patient Handbook Office Hours 8:30 a.m. to 5:00 p.m. Monday-Friday Emergency Answering Service 24 hours a day, 7 days a week Birmingham Office: (205) 981-2333 5025 Highway 280 Suite
Breathe easier. Patient guide to oxygen therapy
 Breathe easier Patient guide to oxygen therapy Table of contents The facts about COPD 3 Understanding oxygen therapy 4 Choices in oxygen therapy equipment 5 Safely living with oxygen 8 Traveling with oxygen
Breathe easier Patient guide to oxygen therapy Table of contents The facts about COPD 3 Understanding oxygen therapy 4 Choices in oxygen therapy equipment 5 Safely living with oxygen 8 Traveling with oxygen
why did my provider prescribe supplemental oxygen?
 why did my provider prescribe supplemental oxygen? why did my provider prescribe supplemental oxygen? People living with lung disease often have lower than normal levels of oxygen in their blood. When
why did my provider prescribe supplemental oxygen? why did my provider prescribe supplemental oxygen? People living with lung disease often have lower than normal levels of oxygen in their blood. When
HOME OXYGEN THERAPY Why is oxygen important? Who benefits from home oxygen therapy?
 HOME OXYGEN THERAPY This brochure provides brief information for those recently prescribed home oxygen therapy. For more detailed information, contact Lung Foundation Australia to purchase a copy of the
HOME OXYGEN THERAPY This brochure provides brief information for those recently prescribed home oxygen therapy. For more detailed information, contact Lung Foundation Australia to purchase a copy of the
2) an acute situation in which hypoxemia is suspected.
 I. Subject: Oxygen Therapy II. Policy: Oxygen therapy shall be initiated upon a physician's order by health care professionals trained in the set-up and principles of safe oxygen administration. Oxygen
I. Subject: Oxygen Therapy II. Policy: Oxygen therapy shall be initiated upon a physician's order by health care professionals trained in the set-up and principles of safe oxygen administration. Oxygen
FACTSHEET F36 UNDERSTANDING YOUR HOME OXYGEN THERAPY. Why do I need oxygen therapy at home? How will oxygen therapy help me?
 UNDERSTANDING YOUR HOME OXYGEN THERAPY This factsheet aims to give you information about how home oxygen therapy will help you, how it is provided, the equipment involved and how to use it. Why do I need
UNDERSTANDING YOUR HOME OXYGEN THERAPY This factsheet aims to give you information about how home oxygen therapy will help you, how it is provided, the equipment involved and how to use it. Why do I need
Subject: Oxygen DESCRIPTION: POSITION STATEMENT: Original Effective Date: 10/03/00. Reviewed: 08/23/18. Revised: 09/15/18
 09-E0400-00 Original Effective Date: 10/03/00 Reviewed: 08/23/18 Revised: 09/15/18 Subject: Oxygen THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION OF BENEFITS, OR A
09-E0400-00 Original Effective Date: 10/03/00 Reviewed: 08/23/18 Revised: 09/15/18 Subject: Oxygen THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION OF BENEFITS, OR A
Home Oxygen Therapy. Delivering the best in care. UHB is a no smoking Trust
 Home Oxygen Therapy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm What is it?
Home Oxygen Therapy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm What is it?
The Benefits of Supplemental Oxygen
 MEETING MODULE The Benefits of Supplemental Oxygen FACILITATOR GUIDE About the American Lung Association The American Lung Association is the leading organization working to save lives by improving lung
MEETING MODULE The Benefits of Supplemental Oxygen FACILITATOR GUIDE About the American Lung Association The American Lung Association is the leading organization working to save lives by improving lung
Effective Date: September, 2011 Revised: August 17, 2016 OXYGEN, ADMINISTRATION OF
 OXYGEN, ADMINISTRATION OF Purpose: Supplemental oxygen may be required to meet metabolic demands of students who have chronic respiratory or cardiac conditions. Oxygen therapy treats or prevents hypoxia
OXYGEN, ADMINISTRATION OF Purpose: Supplemental oxygen may be required to meet metabolic demands of students who have chronic respiratory or cardiac conditions. Oxygen therapy treats or prevents hypoxia
Health Professional Manual
 Health Professional Manual Session: Long-Term Oxygen Therapy Effect of COPD on oxygen levels Oxygen and oxygen equipment Learning to live with long-term oxygen therapy Adapted from the Living Well with
Health Professional Manual Session: Long-Term Oxygen Therapy Effect of COPD on oxygen levels Oxygen and oxygen equipment Learning to live with long-term oxygen therapy Adapted from the Living Well with
Chapter 9 Airway Respirations Metabolism Oxygen Requirements Respiratory Anatomy Respiratory Anatomy Respiratory Anatomy Diaphragm
 1 Chapter 9 Airway 2 Respirations Every cell of the body requires to survive Oxygen must come in and carbon must go out 3 Metabolism Metabolism--Process where the body s cells convert food to Adequate
1 Chapter 9 Airway 2 Respirations Every cell of the body requires to survive Oxygen must come in and carbon must go out 3 Metabolism Metabolism--Process where the body s cells convert food to Adequate
Have you reached your saturation point yet? By John R. Goodman BS RRT
 Have you reached your saturation point yet? By John R. Goodman BS RRT Oxygen therapy has come quite a long way since its discovery way back in the late 1700 s. Although oxygen had some limited clinical
Have you reached your saturation point yet? By John R. Goodman BS RRT Oxygen therapy has come quite a long way since its discovery way back in the late 1700 s. Although oxygen had some limited clinical
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Medications POLICY NUMBER: 512. Effective Date: August 31, 2006
 SUBJECT: OXYGEN (O 2 ) THERAPY COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Medications POLICY NUMBER: 512 Effective Date: August 31, 2006 1. GENERAL CONSIDERATIONS A. Individuals
SUBJECT: OXYGEN (O 2 ) THERAPY COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Medications POLICY NUMBER: 512 Effective Date: August 31, 2006 1. GENERAL CONSIDERATIONS A. Individuals
Respiratory Signs: Tachypnea (RR>30/min), Desaturation, Shallow breathing, Use of accessory muscles Breathing sound: Wheezing, Rhonchi, Crepitation.
 Respiratory Signs: Tachypnea (RR>30/min), Desaturation, Shallow breathing, Use of accessory muscles Breathing sound: Wheezing, Rhonchi, Crepitation. Paradoxical breathing Hyper-resonance on percussion:
Respiratory Signs: Tachypnea (RR>30/min), Desaturation, Shallow breathing, Use of accessory muscles Breathing sound: Wheezing, Rhonchi, Crepitation. Paradoxical breathing Hyper-resonance on percussion:
Reference guide for individual patient education
 Reference guide for individual patient education Integrating Long-Term Home Oxygen Therapy into the COPD patients life Topics: 1. Long-Term home oxygen therapy and oxygen equipment To have a better understanding
Reference guide for individual patient education Integrating Long-Term Home Oxygen Therapy into the COPD patients life Topics: 1. Long-Term home oxygen therapy and oxygen equipment To have a better understanding
Table of Contents. Operating Instructions. Resource v.2 Conserving Regulator
 Operating Instructions Table of Contents Resource v.2 Conserving Regulator Safety Information Device Precautions Introduction Product Features Product Specifications Feature Illustrations Set Up Usage
Operating Instructions Table of Contents Resource v.2 Conserving Regulator Safety Information Device Precautions Introduction Product Features Product Specifications Feature Illustrations Set Up Usage
OXYGEN THERAPY AND QUALITY OF LIFE Oxygen Therapy and Quality of Life
 OXYGEN THERAPY AND QUALITY OF LIFE Oxygen Therapy and Quality of Life Some patients with idiopathic pulmonary fibrosis (IPF) may be prescribed oxygen therapy after being assessed by a doctor. For those
OXYGEN THERAPY AND QUALITY OF LIFE Oxygen Therapy and Quality of Life Some patients with idiopathic pulmonary fibrosis (IPF) may be prescribed oxygen therapy after being assessed by a doctor. For those
Clinical Skills. Administering Oxygen
 Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
The Supplemental Oxygen Guide Version 1.1 Updated 6/26/15 Q&A for Every Supplemental Oxygen User
 The Supplemental Oxygen Guide Version 1.1 Updated 6/26/15 Q&A for Every Supplemental Oxygen User My doctor has just prescribed the use of supplemental oxygen. What do I need to do? Talk with your doctor.
The Supplemental Oxygen Guide Version 1.1 Updated 6/26/15 Q&A for Every Supplemental Oxygen User My doctor has just prescribed the use of supplemental oxygen. What do I need to do? Talk with your doctor.
COALINGA STATE HOSPITAL. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
Home oxygen therapy. Oxygen Team Patient Information Leaflet
 Home oxygen therapy Oxygen Team Patient Information Leaflet Introduction This leaflet is for people who have been referred to the Oxygen Team. It gives information on oxygen therapy, how you use the oxygen,
Home oxygen therapy Oxygen Team Patient Information Leaflet Introduction This leaflet is for people who have been referred to the Oxygen Team. It gives information on oxygen therapy, how you use the oxygen,
BROCKTON AREA MULTI-SERVICES, INC. MEDICAL PROCEDURE GUIDE. Date(s) Reviewed/Revised:
 Page 1 of 6 DEFINITION: Oxygen is a colorless, odorless, and tasteless gas that makes up about 20% of the air we breathe. Oxygen is essential to human, animal, and plant life. This training is intended
Page 1 of 6 DEFINITION: Oxygen is a colorless, odorless, and tasteless gas that makes up about 20% of the air we breathe. Oxygen is essential to human, animal, and plant life. This training is intended
Standards and guidelines for care and management of patients requiring oxygen therapy.
 PURPOSE Standards and guidelines for care and management of patients requiring oxygen therapy. STANDARDS Ongoing management of oxygen therapy requires a prescriber s order. The order must specify oxygen
PURPOSE Standards and guidelines for care and management of patients requiring oxygen therapy. STANDARDS Ongoing management of oxygen therapy requires a prescriber s order. The order must specify oxygen
MedStar Health considers Home Oxygen Therapy medically necessary for the following indications:
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.130.MH Home Oxygen Therapy This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst PPO
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.130.MH Home Oxygen Therapy This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst PPO
Plano Independent School District Health Service Oxygen in Use Administrative Guideline
 Plano Independent School District Health Service in Use Administrative Guideline Purpose This in Use Guideline is provided to schools and school personnel in planning for the safety of students when oxygen
Plano Independent School District Health Service in Use Administrative Guideline Purpose This in Use Guideline is provided to schools and school personnel in planning for the safety of students when oxygen
DRAFT U S E R M A N U A L CAUTION. Model: 19MFA1001 Series. Federal (USA) law restricts this device to sale by or on the order of a physician.
 U S E R M A N U A L Model: 19MFA1001 Series SAVE THESE INSTRUCTIONS Federal (USA) law restricts this device to sale by or on the order of a physician. 300 Held Drive Tel: (+001) 610-262-6090 Northampton,
U S E R M A N U A L Model: 19MFA1001 Series SAVE THESE INSTRUCTIONS Federal (USA) law restricts this device to sale by or on the order of a physician. 300 Held Drive Tel: (+001) 610-262-6090 Northampton,
Breathing Process: Inhalation
 Airway Chapter 6 Breathing Process: Inhalation Active part of breathing Diaphragm and intercostal muscles contract, allowing the lungs to expand. The decrease in pressure allows lungs to fill with air.
Airway Chapter 6 Breathing Process: Inhalation Active part of breathing Diaphragm and intercostal muscles contract, allowing the lungs to expand. The decrease in pressure allows lungs to fill with air.
PA-IPF Newsletter. the
 the F I R S T E D I T I O N PA-IPF Newsletter A P R O J E C T S P O N S O R E D B Y T H E C O M M O N W E A L T H O F P E N N S Y L VA N I A A N D A G E N E R O U S D O N A T I O N F R O M T H E S I M
the F I R S T E D I T I O N PA-IPF Newsletter A P R O J E C T S P O N S O R E D B Y T H E C O M M O N W E A L T H O F P E N N S Y L VA N I A A N D A G E N E R O U S D O N A T I O N F R O M T H E S I M
London Respiratory Team
 London Respiratory Team By email 28 March 2012 Ambulatory Oxygen for London This guide has been produced to help healthcare maximise the benefit of the new oxygen contract for patients and to reduce waste.
London Respiratory Team By email 28 March 2012 Ambulatory Oxygen for London This guide has been produced to help healthcare maximise the benefit of the new oxygen contract for patients and to reduce waste.
PHTY 300 Wk 1 Lectures
 PHTY 300 Wk 1 Lectures Arterial Blood Gas Components The test provides information on - Acid base balance - Oxygenation - Hemoglobin levels - Electrolyte blood glucose, lactate, renal function When initially
PHTY 300 Wk 1 Lectures Arterial Blood Gas Components The test provides information on - Acid base balance - Oxygenation - Hemoglobin levels - Electrolyte blood glucose, lactate, renal function When initially
VENTILATORS PURPOSE OBJECTIVES
 VENTILATORS PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain a ventilator in the interfacility transfer environment. COGNITIVE OBJECTIVES
VENTILATORS PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain a ventilator in the interfacility transfer environment. COGNITIVE OBJECTIVES
Manual: Biphasic Positive Airway Pressure (BiPAP) Ventilation
 RCH@Home Manual: Biphasic Positive Airway Pressure (BiPAP) Ventilation 1. Commonly used terms... 2 1.1 Inspiration... 2 1.2 Expiration... 2 1.3 Breath rate (bpm)... 2 1.4 Ventilation... 2 1.5 Biphasic
RCH@Home Manual: Biphasic Positive Airway Pressure (BiPAP) Ventilation 1. Commonly used terms... 2 1.1 Inspiration... 2 1.2 Expiration... 2 1.3 Breath rate (bpm)... 2 1.4 Ventilation... 2 1.5 Biphasic
MEDICAL DEPARTMENT PASSENGER INFORMATION PHYSICIAN INFORMATION
 MON-FRI 06:00-20:00 EST MEDICAL DEPARTMENT SAT-SUN 06:00-18 :00 EST Email : acmedical@aircanada.ca Fax 1-888-334-7717 (Toll-free from North America) Telephone 1-800-667-4732 (Toll-free from North America)
MON-FRI 06:00-20:00 EST MEDICAL DEPARTMENT SAT-SUN 06:00-18 :00 EST Email : acmedical@aircanada.ca Fax 1-888-334-7717 (Toll-free from North America) Telephone 1-800-667-4732 (Toll-free from North America)
Understanding Tracheostomy Care
 Understanding Tracheostomy Care Inside this guide: This guide will help you learn how to take care of your tracheostomy (trach). It is important to ask questions. You will be given time to learn. Working
Understanding Tracheostomy Care Inside this guide: This guide will help you learn how to take care of your tracheostomy (trach). It is important to ask questions. You will be given time to learn. Working
Capnography in the Veterinary Technician Toolbox. Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA
 Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
when you need oxygen.
 Time is precious... when you need oxygen. DCare Partners... Working together to build up the unique OxySmart Project to supply and refill the world s smallest and lightest oxygen cylinders. Cramer Decker
Time is precious... when you need oxygen. DCare Partners... Working together to build up the unique OxySmart Project to supply and refill the world s smallest and lightest oxygen cylinders. Cramer Decker
Medical Instruments in the Developing World
 2.2 Ventilators 2.2.1 Clinical Use and Principles of Operation Many patients in an intensive care and the operating room require the mechanical ventilation of their lungs. All thoracic surgery patients,
2.2 Ventilators 2.2.1 Clinical Use and Principles of Operation Many patients in an intensive care and the operating room require the mechanical ventilation of their lungs. All thoracic surgery patients,
OXYGEN THERAPY. (Non-invasive O2 therapy in patient >8yrs)
 OXYGEN THERAPY (Non-invasive O2 therapy in patient >8yrs) Learning aims Indications and precautions for O2 therapy Targets of therapy Standard notation O2 delivery devices Taps, tanks and tubing Notation
OXYGEN THERAPY (Non-invasive O2 therapy in patient >8yrs) Learning aims Indications and precautions for O2 therapy Targets of therapy Standard notation O2 delivery devices Taps, tanks and tubing Notation
The Aide s role in assisting clients with COPD:
 In-Home Aides- Partners in Quality Care July 2013 What does Chronic Obstructive Pulmonary Disease (COPD) mean? Objectives/What You Will Learn: How the lungs works Symptoms of Chronic Obstructive Pulmonary
In-Home Aides- Partners in Quality Care July 2013 What does Chronic Obstructive Pulmonary Disease (COPD) mean? Objectives/What You Will Learn: How the lungs works Symptoms of Chronic Obstructive Pulmonary
Patient Information for the: Humanitarian Device for use in the Control of Air Leaks
 Patient Information for the: Humanitarian Device for use in the Control of Air Leaks Glossary Airway: The tubes in the lungs that pass air to and from the lung tissue. Anesthesia: Technique to make the
Patient Information for the: Humanitarian Device for use in the Control of Air Leaks Glossary Airway: The tubes in the lungs that pass air to and from the lung tissue. Anesthesia: Technique to make the
Mechanical Ventilation
 PROCEDURE - Page 1 of 5 Purpose Scope Physician's Order Indications Procedure Mechanical Artificial Ventilation refers to any methods to deliver volumes of gas into a patient's lungs over an extended period
PROCEDURE - Page 1 of 5 Purpose Scope Physician's Order Indications Procedure Mechanical Artificial Ventilation refers to any methods to deliver volumes of gas into a patient's lungs over an extended period
Unit II Problem 4 Physiology: Diffusion of Gases and Pulmonary Circulation
 Unit II Problem 4 Physiology: Diffusion of Gases and Pulmonary Circulation - Physical principles of gases: Pressure of a gas is caused by the movement of its molecules against a surface (more concentration
Unit II Problem 4 Physiology: Diffusion of Gases and Pulmonary Circulation - Physical principles of gases: Pressure of a gas is caused by the movement of its molecules against a surface (more concentration
A. Evaluation of the written program
 A. Evaluation of the written program Begin your audit with an evaluation of the written respiratory protection program. In addition to the operating procedures describing respirator selection and use in
A. Evaluation of the written program Begin your audit with an evaluation of the written respiratory protection program. In addition to the operating procedures describing respirator selection and use in
Auditing the non-emergency use of a fan or oxygen to relieve breathlessness at rest: Background form
 Auditing the non-emergency use of a fan or oxygen to relieve breathlessness at rest: Background form Background Breathlessness is a common and distressing symptom that can be difficult to treat. Oxygen
Auditing the non-emergency use of a fan or oxygen to relieve breathlessness at rest: Background form Background Breathlessness is a common and distressing symptom that can be difficult to treat. Oxygen
1.2 The structure and functions of the cardio-respiratory system Learning objectives
 1.2 The structure and functions of the cardio-respiratory system Learning objectives To understand the functions of the circulatory system. To be able to identify the differences between veins, arteries
1.2 The structure and functions of the cardio-respiratory system Learning objectives To understand the functions of the circulatory system. To be able to identify the differences between veins, arteries
Complex Care Hub Manual: Oxygen Therapy
 Complex Care Hub Manual: Oxygen Therapy Table of Contents RCH@Home Manual: Oxygen Therapy... 1 1. What is oxygen therapy?... 2 2. Symptoms of low oxygen... 2 3. Giving oxygen at home and in the community...
Complex Care Hub Manual: Oxygen Therapy Table of Contents RCH@Home Manual: Oxygen Therapy... 1 1. What is oxygen therapy?... 2 2. Symptoms of low oxygen... 2 3. Giving oxygen at home and in the community...
Deborah Dewaay MD Division of General Internal Medicine and Geriatrics Hospital Medicine Acknowledgment: Antine Stenbit MD
 Deborah Dewaay MD Division of General Internal Medicine and Geriatrics Hospital Medicine 2013 Acknowledgment: Antine Stenbit MD Objectives Knowledge: Understand the difference between hypoxia and hypoxemia
Deborah Dewaay MD Division of General Internal Medicine and Geriatrics Hospital Medicine 2013 Acknowledgment: Antine Stenbit MD Objectives Knowledge: Understand the difference between hypoxia and hypoxemia
STAYING ACTIVE WHILE USING OXYGEN. Karla Schlichtmann, RRT
 STAYING ACTIVE WHILE USING OXYGEN Karla Schlichtmann, RRT Kschilchtmann@partners.org How do I qualify for oxygen? SpO2 < 88% at rest, patient qualifies SpO2 > 88% at rest, the following saturations must
STAYING ACTIVE WHILE USING OXYGEN Karla Schlichtmann, RRT Kschilchtmann@partners.org How do I qualify for oxygen? SpO2 < 88% at rest, patient qualifies SpO2 > 88% at rest, the following saturations must
Rev. B. Operating Instructions
 780745-00 Rev. B Operating Instructions 780745-00 Rev. B TABLE OF CONTENTS PAGE Warnings, Cautions, and Notes..............................4-7 Definition of Symbols......................................
780745-00 Rev. B Operating Instructions 780745-00 Rev. B TABLE OF CONTENTS PAGE Warnings, Cautions, and Notes..............................4-7 Definition of Symbols......................................
Toolbox Talk. Carbon Monoxide
 Carbon Monoxide Toolbox Talk Carbon monoxide defies all five human senses. You can t see it, smell it, touch it or taste it and you certainly can t hear this potentially deadly gas, which has been called
Carbon Monoxide Toolbox Talk Carbon monoxide defies all five human senses. You can t see it, smell it, touch it or taste it and you certainly can t hear this potentially deadly gas, which has been called
Structures of the Respiratory System include:
 Respiratory System Structures of the Respiratory System include: ü Oral Cavity ü Nasal Cavity ü Pharynx ü Epiglottis ü Larynx ü Trachea ü Diaphragm ü Lung ü Bronchus ü Bronchioles ü Alveolus ü Pulmonary
Respiratory System Structures of the Respiratory System include: ü Oral Cavity ü Nasal Cavity ü Pharynx ü Epiglottis ü Larynx ü Trachea ü Diaphragm ü Lung ü Bronchus ü Bronchioles ü Alveolus ü Pulmonary
Gas Exchange Respiratory Systems
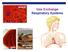 alveoli gills Gas Exchange Respiratory Systems elephant seals 2008-2009 Why do we need a respiratory system? respiration for respiration Need O 2 in for aerobic cellular respiration make ATP Need CO 2
alveoli gills Gas Exchange Respiratory Systems elephant seals 2008-2009 Why do we need a respiratory system? respiration for respiration Need O 2 in for aerobic cellular respiration make ATP Need CO 2
Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams)
 Name Lab Partners Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams) Part 1. Lung Volumes and Capacities Objectives 1. Obtain graphical representation of lung capacities
Name Lab Partners Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams) Part 1. Lung Volumes and Capacities Objectives 1. Obtain graphical representation of lung capacities
PICU Resident Self-Study Tutorial The Basic Physics of Oxygen Transport. I was told that there would be no math!
 Physiology of Oxygen Transport PICU Resident Self-Study Tutorial I was told that there would be no math! INTRODUCTION Christopher Carroll, MD Although cells rely on oxygen for aerobic metabolism and viability,
Physiology of Oxygen Transport PICU Resident Self-Study Tutorial I was told that there would be no math! INTRODUCTION Christopher Carroll, MD Although cells rely on oxygen for aerobic metabolism and viability,
Point-of-Care Testing: A Cardiovascular Perfusionist s Perspective
 Point-of-Care Testing: A Cardiovascular Perfusionist s Perspective Cory M. Alwardt, PhD, CCP Chief Perfusionist/ECMO Coordinator Assistant Professor of Surgery Mayo Clinic Hospital, Phoenix alwardt.cory@mayo.edu
Point-of-Care Testing: A Cardiovascular Perfusionist s Perspective Cory M. Alwardt, PhD, CCP Chief Perfusionist/ECMO Coordinator Assistant Professor of Surgery Mayo Clinic Hospital, Phoenix alwardt.cory@mayo.edu
Liquid Oxygen- Helios & Helios Marathon A Guide for Patients in the Home
 Liquid Oxygen- Helios & Helios Marathon A Guide for Patients in the Home Contact Name: Phone number: Table of Contents Contents Receiving Liquid Oxygen in the Home... 2 Instructions for Liquid Oxygen-Helios
Liquid Oxygen- Helios & Helios Marathon A Guide for Patients in the Home Contact Name: Phone number: Table of Contents Contents Receiving Liquid Oxygen in the Home... 2 Instructions for Liquid Oxygen-Helios
Welcome to the Specialized Medical Services Respiratory training webinar series!
 Welcome to the Specialized Medical Services Respiratory training webinar series! SMS is your Long Term Care (LTC) facility single source for oxygen, medical equipment, respiratory care services and supplies
Welcome to the Specialized Medical Services Respiratory training webinar series! SMS is your Long Term Care (LTC) facility single source for oxygen, medical equipment, respiratory care services and supplies
The physiological functions of respiration and circulation. Mechanics. exercise 7. Respiratory Volumes. Objectives
 exercise 7 Respiratory System Mechanics Objectives 1. To explain how the respiratory and circulatory systems work together to enable gas exchange among the lungs, blood, and body tissues 2. To define respiration,
exercise 7 Respiratory System Mechanics Objectives 1. To explain how the respiratory and circulatory systems work together to enable gas exchange among the lungs, blood, and body tissues 2. To define respiration,
Lung Volumes and Capacities
 Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
1. NAME OF THE MEDICINAL PRODUCT. Medicinal Air, Air Liquide 100%, medicinal gas, compressed. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION
 1. NAME OF THE MEDICINAL PRODUCT Medicinal Air, Air Liquide 100%, medicinal gas, compressed. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Medicinal air 100% at a pressure of 200 bar (15 C). 3. PHARMACEUTICAL
1. NAME OF THE MEDICINAL PRODUCT Medicinal Air, Air Liquide 100%, medicinal gas, compressed. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Medicinal air 100% at a pressure of 200 bar (15 C). 3. PHARMACEUTICAL
Helpful hints for filing
 Helpful hints f filing Oxygen and oxygen-related equipment Overview The following infmation describes the Durable Medical Equipment Medicare Administrative Contracts (DME MAC) medical policy f oxygen and
Helpful hints f filing Oxygen and oxygen-related equipment Overview The following infmation describes the Durable Medical Equipment Medicare Administrative Contracts (DME MAC) medical policy f oxygen and
University of Alabama Office of Environmental Health and Safety. Respirator Protection Training
 University of Alabama Office of Environmental Health and Safety Respirator Protection Training Medical Reasons That Could Prohibit the Use of a Respirator A history of pulmonary or lung problems such as:
University of Alabama Office of Environmental Health and Safety Respirator Protection Training Medical Reasons That Could Prohibit the Use of a Respirator A history of pulmonary or lung problems such as:
AP Biology. Gas Exchange Respiratory Systems. Gas exchange. Why do we need a respiratory system? Optimizing gas exchange. Gas exchange in many forms
 alveoli Gas Exchange Respiratory Systems gills elephant seals 2008-2009 Why do we need a respiratory system? Need O 2 in food respiration for respiration for aerobic cellular respiration make ATP Need
alveoli Gas Exchange Respiratory Systems gills elephant seals 2008-2009 Why do we need a respiratory system? Need O 2 in food respiration for respiration for aerobic cellular respiration make ATP Need
respiratory cycle. point in the volumes: 500 milliliters. for men. expiration, up to 1200 milliliters extra makes breathing Respiratory
 10 II. RESPIRATORY VOLUMES, CAPACITIES & PULMONARY FUNCTION TESTS Respiratory volume is the term used for various volumes of air moved by or associated with the lungs at a given point in the respiratory
10 II. RESPIRATORY VOLUMES, CAPACITIES & PULMONARY FUNCTION TESTS Respiratory volume is the term used for various volumes of air moved by or associated with the lungs at a given point in the respiratory
SCENARIO #2 CARBON MONOXIDE INCIDENT IN AN AUTO SHOP
 SCENARIO #2 CARBON MONOXIDE INCIDENT IN AN AUTO SHOP 169 FIGURE 8-8 A 500 gallon ASME propane tank is used to supply an interior space heater at an automobile repair shop. During extremely cold weather,
SCENARIO #2 CARBON MONOXIDE INCIDENT IN AN AUTO SHOP 169 FIGURE 8-8 A 500 gallon ASME propane tank is used to supply an interior space heater at an automobile repair shop. During extremely cold weather,
Information about oxygen
 Information about oxygen INFORMATION FOR PATIENTS, CARERS AND FAMILIES 1 Why have I been given oxygen? Oxygen is vital for our bodies and having low oxygen levels can make you feel very unwell. There are
Information about oxygen INFORMATION FOR PATIENTS, CARERS AND FAMILIES 1 Why have I been given oxygen? Oxygen is vital for our bodies and having low oxygen levels can make you feel very unwell. There are
Understanding Tracheostomy Care for your Child
 Understanding Tracheostomy Care for your Child 2 Inside this guide: This guide will help you learn how to take care of your child s tracheostomy (trach). It is important to ask questions. You will be given
Understanding Tracheostomy Care for your Child 2 Inside this guide: This guide will help you learn how to take care of your child s tracheostomy (trach). It is important to ask questions. You will be given
Lung Volumes and Capacities
 BIOL242 Lung Volumes and Capacities Measurement of lung volumes provides a tool for understanding normal function of the lungs as well as disease states. The breathing cycle is initiated by expansion of
BIOL242 Lung Volumes and Capacities Measurement of lung volumes provides a tool for understanding normal function of the lungs as well as disease states. The breathing cycle is initiated by expansion of
Definition An uninterrupted path between the atmosphere and the alveoli
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Airway Management (Class 9) Airway Definition An uninterrupted path between the atmosphere and the alveoli Methods of opening the airway Positioning Left lateral recumbent
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Airway Management (Class 9) Airway Definition An uninterrupted path between the atmosphere and the alveoli Methods of opening the airway Positioning Left lateral recumbent
A breath of fresh air
 A breath of fresh air BIG IDEAS You are learning to: Describe the structure of the lungs Explain how the lungs clean themselves Interpret patterns in data Where are the lungs and what do they do? The lungs
A breath of fresh air BIG IDEAS You are learning to: Describe the structure of the lungs Explain how the lungs clean themselves Interpret patterns in data Where are the lungs and what do they do? The lungs
Human Biology Respiratory System
 Human Biology Respiratory System Respiratory System Responsible for process of breathing Works in cooperation with Circulatory system Three types: 1. Internal Respiration 2. External Respiration 3. Cellular
Human Biology Respiratory System Respiratory System Responsible for process of breathing Works in cooperation with Circulatory system Three types: 1. Internal Respiration 2. External Respiration 3. Cellular
All Programs. CROSS REFERENCE: Initiation, Titration and Discontinuation of Oxygen Therapy for Adult Patients Medical Directive
 1 All Programs SUBJECT: Oxygen Standard of Care for the Adult Patient ISSUING BODY: Nursing Practice Council, Respiratory Therapy Services, Physiotherapy Practice Council and Occupational Therapy Practice
1 All Programs SUBJECT: Oxygen Standard of Care for the Adult Patient ISSUING BODY: Nursing Practice Council, Respiratory Therapy Services, Physiotherapy Practice Council and Occupational Therapy Practice
Being discharged from hospital with oxygen
 Being discharged from hospital with oxygen Turnberg Building Respiratory Medicine 0161 206 0865 All Rights Reserved 2018. Document for issue as handout. What is supplemental oxygen therapy? Oxygen is needed
Being discharged from hospital with oxygen Turnberg Building Respiratory Medicine 0161 206 0865 All Rights Reserved 2018. Document for issue as handout. What is supplemental oxygen therapy? Oxygen is needed
B. A clinical emergency exists in which a profound hypoxia is determined to be present.
 I. Subject: Oxyhood-Oxygen Therapy for Neonates II. Policy: Oxygen therapy by oxyhood shall be initiated upon a physician's order by nurses and Respiratory Therapy personnel trained in the principles of
I. Subject: Oxyhood-Oxygen Therapy for Neonates II. Policy: Oxygen therapy by oxyhood shall be initiated upon a physician's order by nurses and Respiratory Therapy personnel trained in the principles of
OXYGEN THERAPY. Catherine Jones June 2017
 OXYGEN THERAPY Catherine Jones June 2017 1 ACKNOWLEDGEMENT 2 LEARNING OUTCOMES To revise why Oxygen is important To identify the indications for Oxygen Therapy To identify problems with administration
OXYGEN THERAPY Catherine Jones June 2017 1 ACKNOWLEDGEMENT 2 LEARNING OUTCOMES To revise why Oxygen is important To identify the indications for Oxygen Therapy To identify problems with administration
CONTENTS. 9. Opening of gas systems containing H 2 S. 1. Introduction. 8. Protection of Personnel.
 CONTENTS 1. Introduction. 2. Properties and toxicity of H 2 S. 3. Physical effects of H 2 S. 4. Pyrophoric iron sulphide. 5. Identification of H 2 S hazard. 6. Entry to H 2 S risk area. 7. Detection of
CONTENTS 1. Introduction. 2. Properties and toxicity of H 2 S. 3. Physical effects of H 2 S. 4. Pyrophoric iron sulphide. 5. Identification of H 2 S hazard. 6. Entry to H 2 S risk area. 7. Detection of
CSHCN Services Program Prior Authorization Request for Oxygen Therapy Form and Instructions
 General Information CSHCN Services Program Prior Authorization Request for and Instructions Ensure the most recent version of the Prior Authorization Request for Oxygen Therapy form is submitted. The form
General Information CSHCN Services Program Prior Authorization Request for and Instructions Ensure the most recent version of the Prior Authorization Request for Oxygen Therapy form is submitted. The form
Respiratory System 1
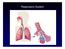 Respiratory System 1 Outline Respiratory structures Gills Air-Breathing Animals Amphibians and Reptiles Mammals Birds Structures and Mechanisms of Breathing 2 Copyright The McGraw-Hill Companies, Inc.
Respiratory System 1 Outline Respiratory structures Gills Air-Breathing Animals Amphibians and Reptiles Mammals Birds Structures and Mechanisms of Breathing 2 Copyright The McGraw-Hill Companies, Inc.
Blood Gas Interpretation
 Blood Gas Interpretation Pa O2 Saturation (SaO 2 ) Oxygen Therapy Monitoring Oxygen content (O( 2 Ct) Venous Oximetry Mixed venous oxygen saturation SvO 2 Surrogate for Systemic oxygen delivery and
Blood Gas Interpretation Pa O2 Saturation (SaO 2 ) Oxygen Therapy Monitoring Oxygen content (O( 2 Ct) Venous Oximetry Mixed venous oxygen saturation SvO 2 Surrogate for Systemic oxygen delivery and
Children s Home Healthcare s. Oxygen Parent Handbook
 Children s Home Healthcare s Information and Instructions For Parents Who Have A Child Who Uses Oxygen Your child s physician prescribed home oxygen therapy for. The current order states that you are to
Children s Home Healthcare s Information and Instructions For Parents Who Have A Child Who Uses Oxygen Your child s physician prescribed home oxygen therapy for. The current order states that you are to
alveoli Chapter 42. Gas Exchange elephant seals gills AP Biology
 alveoli Chapter 42. Gas Exchange gills elephant seals Gas exchange O 2 & CO 2 exchange exchange between environment & cells provides O 2 for aerobic cellular respiration need moist membrane need high
alveoli Chapter 42. Gas Exchange gills elephant seals Gas exchange O 2 & CO 2 exchange exchange between environment & cells provides O 2 for aerobic cellular respiration need moist membrane need high
Collin County Community College. Lung Physiology
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 9 Respiratory System 1 Lung Physiology Factors affecting Ventillation 1. Airway resistance Flow = Δ P / R Most resistance is encountered
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 9 Respiratory System 1 Lung Physiology Factors affecting Ventillation 1. Airway resistance Flow = Δ P / R Most resistance is encountered
Respiratory System Review
 KEY THIS TEST WILL BE COMPLETED IN ONE CLASS PERIOD MONDAY, MARCH 10. 2014 Respiratory System Review Name A. Directions: Fill in the blank with the appropriate vocabulary word or words (several examples
KEY THIS TEST WILL BE COMPLETED IN ONE CLASS PERIOD MONDAY, MARCH 10. 2014 Respiratory System Review Name A. Directions: Fill in the blank with the appropriate vocabulary word or words (several examples
Chapter 11: Respiratory System Review Assignment
 Name: Date: Mark: / 45 Chapter 11: Respiratory System Review Assignment Multiple Choice = 45 Marks Identify the choice that best completes the statement or answers the question. 1. Which of the following
Name: Date: Mark: / 45 Chapter 11: Respiratory System Review Assignment Multiple Choice = 45 Marks Identify the choice that best completes the statement or answers the question. 1. Which of the following
Liquid Medical Oxygen Medicinal gas, cryogenic Package Leaflet: Information for the User
 Liquid Medical Oxygen Medicinal gas, cryogenic Package Leaflet: Information for the User Liquid Medical Oxygen, Oxygen 99.5%, Medicinal gas, cryogenic Read all of this leaflet carefully before you start
Liquid Medical Oxygen Medicinal gas, cryogenic Package Leaflet: Information for the User Liquid Medical Oxygen, Oxygen 99.5%, Medicinal gas, cryogenic Read all of this leaflet carefully before you start
Initiation and Management of Airway Pressure Release Ventilation (APRV)
 Initiation and Management of Airway Pressure Release Ventilation (APRV) Eric Kriner RRT Pulmonary Critical Care Clinical Specialist Pulmonary Services Department Medstar Washington Hospital Center Disclosures
Initiation and Management of Airway Pressure Release Ventilation (APRV) Eric Kriner RRT Pulmonary Critical Care Clinical Specialist Pulmonary Services Department Medstar Washington Hospital Center Disclosures
Pop Quiz. What produces mucus, HCl and pepsinogen in the stomach? List a water soluable vitamin What is a ruminant stomach?
 Pop Quiz What produces mucus, HCl and pepsinogen in the stomach? List a water soluable vitamin What is a ruminant stomach? Respiratory System Review Cellular respiration: obtain glucose and oxygen, get
Pop Quiz What produces mucus, HCl and pepsinogen in the stomach? List a water soluable vitamin What is a ruminant stomach? Respiratory System Review Cellular respiration: obtain glucose and oxygen, get
Nitrous Oxide Oxygen Administration Protocol July 2002
 Nitrous Oxide Oxygen Administration Protocol July 2002 Preamble A patient s self-administration of a nitrous oxide-oxygen mixture can provide relief of acute pain, provided there are no contraindications
Nitrous Oxide Oxygen Administration Protocol July 2002 Preamble A patient s self-administration of a nitrous oxide-oxygen mixture can provide relief of acute pain, provided there are no contraindications
QUESTIONNAIRE FOR MEMBERS OF THE PUBLIC
 MAHSC Oxygen Project. Questionnaires for members of the public V1 10-12-2011 QUESTIONNAIRE FOR MEMBERS OF THE PUBLIC We would like to know what you think about oxygen therapy as a member of the public.
MAHSC Oxygen Project. Questionnaires for members of the public V1 10-12-2011 QUESTIONNAIRE FOR MEMBERS OF THE PUBLIC We would like to know what you think about oxygen therapy as a member of the public.
NOTE: If not used, provider must document reason(s) for deferring mechanical ventilation in a patient with an advanced airway
 APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
MINI- COURSE on Management of OXYGEN in babies with RESPIRATORY DISTRESS
 MINI- COURSE on Management of OXYGEN in babies with RESPIRATORY DISTRESS Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have 5 questions to allow you to
MINI- COURSE on Management of OXYGEN in babies with RESPIRATORY DISTRESS Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have 5 questions to allow you to
Before using or working with the Grab n Go Heliox system, please read and understand the usage and safety instructions provided in this booklet.
 Operating Instructions for the Before using or working with the Grab n Go Heliox system, please read and understand the usage and safety instructions provided in this booklet. Introduction The Praxair
Operating Instructions for the Before using or working with the Grab n Go Heliox system, please read and understand the usage and safety instructions provided in this booklet. Introduction The Praxair
AP Biology. Chapter 42. Gas Exchange. Optimizing gas exchange. Gas exchange. Gas exchange in many forms. Evolution of gas exchange structures
 alveoli Chapter 42. Gas Exchange gills elephant seals Gas exchange & C exchange exchange between environment & cells provides for aerobic cellular respiration need moist membrane need high surface area
alveoli Chapter 42. Gas Exchange gills elephant seals Gas exchange & C exchange exchange between environment & cells provides for aerobic cellular respiration need moist membrane need high surface area
