Air Traveler s Health: Considerations for Travelers with Pulmonary Disease
|
|
|
- Nicholas Norton
- 5 years ago
- Views:
Transcription
1 Air Traveler s Health: Considerations for Travelers with Pulmonary Disease Sindhu Mukku, MD Assistant Professor of Internal Medicine Department of Internal Medicine Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University Wexner Medical Center Outline 1. Introduction 2. Effect of Altitude on Pulmonary Physiology 3. High Altitude Hypoxia Simulation Testing 4. Traveling with Supplemental Oxygen 5. In-flight Emergencies: What Clinicians Should Know 6. Prevention of Jet-Lag 1
2 Introduction Almost 3 billion people travel by air every year worldwide While in flight emergencies are rare, incidence is on the rise due to increasing number of air travelers, medical tourism, and increased access to low-cost air travel While healthy passengers are able to tolerate the physiologic effects of air travel, passengers with pre-existing conditions may be at risk for adverse events Introduction A common cause of in-flight emergencies is respiratory symptoms, including asthma and COPD exacerbations. Cardiac and neurologic events are the most common cause of in-flight emergencies. Cabin crew may solicit assistance from on-board medical professionals during an in-flight emergency, thus making knowledge of in-flight resources imperative The key steps in preparing your patient for air travel are: 1. Understanding the physiologic effects of altitude 2. Assessing risk in your patient 3. Preparing your patient for travel well in advance to the travel date 2
3 Physiology of Altitude Aircraft generally travel at 30,000-60,000 feet The Federal Aviation Administration (FAA) requires that cabin pressure be maintained at a pressure-equivalent of 8,000 feet The pressure is maintained using a combination of exterior compressed air and re-circulated cabin air As the aircraft ascends and cabin pressure decreases, some passengers may feel popping in the ears, which is due to air escaping from the middle ear and sinuses due to gas expansion Physiology of Altitude At sea level, the barometric pressure is 760 mmhg During ascent, the barometric pressure decreases. The partial pressure of oxygen (PO2) in the atmosphere and the arterial partial pressure of oxygen (PaO2) also decrease proportionally At sea level, we breathe 20.9% oxygen At 8,000 feet, the partial pressure of oxygen drops to the equivalent of breathing 15.1% oxygen at sea level. This translates into a lower PaO2, about 55mmHg In healthy individuals without pulmonary disease, this lower PaO2 is tolerated because the body compensates through a variety of mechanisms 3
4 Symptoms of Hypoxemia at High Altitude Cabin Altitude Symptoms Sea level none 5000 ft Night vision may affected 8000 ft Night vision is affected ft Impaired judgement and memory, decreased alertness, headache, euphoria Above ft Peripheral vision defects unconsciousness 4
5 Effects of Altitude in Pulmonary Disease In passengers with pulmonary disease, these compensatory mechanisms are impaired, thus placing them at risk of further hypoxemia In passengers with COPD, the increased minute ventilation may result in hyperinflation, thus exacerbating dyspnea In passengers with interstitial lung disease, there may be an underlying impairment in gas exchange, which is further exacerbated by hypoxic conditions Assessing Risk for Hypoxemia: Pre-Flight Assessment Patients who may be at risk for hypoxemia during flight include those with: COPD or asthma Severe restrictive lung disease, including those with neuromuscular disease of chest wall deformities Baseline hypercapnia or hypoxemia Cystic fibrosis History of air traveler intolerance due to respiratory symptoms History of recent hospitalization for respiratory illness with last 6 weeks 5
6 Assessing Risk for Hypoxemia: Pre-Flight Assessment Patients who may be at risk for hypoxemia during flight include those with: Recent pneumothorax or thoracic surgery within the last 6 weeks Previous venous thromboembolism Pre-existing requirement for supplemental oxygen or ventilator support Tuberculosis* *Tuberculosis (TB) Recommendations for physicians from the World Health Organization: Physicians should inform all infectious and potentially infectious TB patients that they cannot not travel by air on a commercial flight until they have two negative AFB sputum smears on at least two different occasions. Physicians should inform all MDR-TB and XDR- TB patients that they must not travel by any commercial flight under any circumstances until they are proven to be non-infectious. Physicians should inform public health authorities if an infectious or potentially infectious TB patient intends to travel against medical advice. 6
7 *Tuberculosis (TB) Physicians should immediately inform the relevant public health authority when they are aware that an infectious or potentially infectious TB patient may have exceptional circumstances requiring commercial air travel. In the U.S., this require submission of documentation to the Federal Aviation Administration (FAA), who will then make a decision regarding the specific case. Pre-flight Assessment A pre-flight assessment should be performed in those who are at risk of inflight hypoxia This assessment should include: History and physical exam Spirometry (do not perform in those with active tuberculosis) Assessment of baseline, resting SpO2 Arterial blood gas if hypercapnea is known or suspected 7
8 Predicting In-flight Hypoxia SaO2 PaO These values are approximate. Each patient s physiology is unique and therefore predicting the degree of hypoxia/hypoxemia while in flight based on resting oxygen saturations at sea level can be unreliable. Predicting In-flight Hypoxia: Hypoxia Altitude Simulation Test (HAST) In-flight hypoxia should be considered in those with underlying pulmonary disease or in those who have risk factors for adverse pulmonary events If the pre-flight SpO2 is greater than 95% on room air at rest, then no further testing/evaluation is required 8
9 Predicting In-flight Hypoxia: Hypoxia Altitude Simulation Test (HAST) If the pre-flight SpO2 is 92-95% and the patient has risk factors hypercapnea FEV1 <50% predicted lung cancer cardiac or cerebrovascular disease Recent COPD exacerbation or hospital admission for COPD or CHF exacerbation recently On ventilatory support If the pre-flight SpO2 is less than 92%, prescribe supplemental O2 (no testing needed) Hast: Pre-procedure Patients should wear comfortable clothing, take regular medications, and refrain for exercising prior to procedure The patient s resting heart rate and oxygen saturation will be recorded The patient will be monitored through out the procedure with ECG and pulse oximetry. The respiratory therapist will also monitor for changing symptoms The patient will also wear a nasal cannula underneath the reservoir mask. In the case that the SpO2 drops to < 90% during the test, the nasal cannula with supplemental oxygen can be applied 9
10 HAST: The Procedure- Part 1 The first part of the procedure is to obtain values at rest The patient will breathe 15.1 O 2 through a tightfitting mask (like a non-rebreather mask) or mouth-piece for 10 minutes If the oxygen saturation decreases to less than 89% during the test, the supplemental oxygen is applied. The respiratory therapist will titrate the supplemental oxygen by 1lpm every minute to at least 90% for the remainder of the test. The oxygen prescription will be based on the level of the supplemental oxygen that is necessary to keep the oxygen saturation at or above 90% for the duration of the test. HAST: The Procedure- Part 2 The second part of the procedure is obtaining values with exertion The patient will continue to breath 15% oxygen via a non-rebreather mask If the patient required supplemental oxygen for part 1 (at rest), this will be continued with exercise The patient will exercise on a cycle ergometer or treadmill for 6 minutes, with the respiratory therapist adjusting the resistance to a low level If the oxygen saturation decreases to less than 89% during the test, the supplemental oxygen is applied. The respiratory therapist will titrate the supplemental oxygen by 1lpm every minute to at least 90% for the remainder of the test. 10
11 HAST: The Procedure Alternatively, an arterial blood gas (ABG) is obtained prior to the test The test is performed as outlined previously An ABG is obtained after the test: If PaO2 is less than 50 mmhg, then oxygen is applied at 2lpm (if the patient was not previously on oxygen) or at a level that is double dose of the usual supplemental oxygen prescription The test is repeated on supplemental oxygen to ensure that hypoxia is treated If the PaO2 is between mmhg, then the test may be repeated with exertion and measurements are re-obtained HAST: The Procedure 11
12 HAST: Other Considerations A physician should be available during the test to respond to any significant events during the test (for example, significant cardiac arrhythmia, severe dyspnea, loss of consciousness, severe chest pain.) Should the patient have any significant adverse symptoms during the test, the test should be stopped. The physician should be called if symptoms persist despite stopping the test and recovery. If the patient needs greater than 6lpm supplemental oxygen during part 1 of the test (resting), then part 2 (exercise) should not be performed Other Considerations for Air Travel Check the altitude of the layover airports and also destination Most airlines do not provide supplemental oxygen For example, United Airlines does not provide supplemental oxygen, except on flights to Guam from Tokyo Patients CANNOT check-in full oxygen tanks; some airlines will allow empty tanks to be checked-in 12
13 Other Considerations for Air Travel An FAA-approved portable oxygen concentrator (POC) can be carried in-flight for supplemental oxygen needs Most airlines require at least 48 hour notice that the passenger will be traveling with supplemental oxygen Make sure that the POC has enough battery charge for the duration of the flight PLUS three hours Physicians may need to fill out a medical necessity form for POCs Patient should travel with their oxygen prescription at all times. It is also advisable that they carry all prescription medications in their carry-on luggage Pulmonary Disease- Specific Considerations Asthma: It is advised that the patient carry their inhalers and space in their carry-on luggage COPD: It is advised that the patient carry their inhalers and space in their carry-on luggage. If there is significant walking involved at layover airports Cystic fibrosis: It is advised that the patient divide their medications between the carry-on and check-in luggage. Physiotherapy can be done during layovers. Due to the sensitive nature of some medications, consultation with a pharmacist about proper storage prior to travel is advised. 13
14 In-flight Emergencies In-flight emergencies are rare FAA requires that all flights weighing 7500 lbs or more have at least one flight attendant that is trained to use an AED and enhanced emergency medical kit Flight attendants must be certified in CPR and AED use The Aerospace Medical Association Air Transport Medicine Committee determines what is in the emergency kit In-flight Emergency Medical Kit Medications Epinephrine 1:1000 Antihistamine, injectable (Inj) D50, 50 ml Nitroglycerin tabs or spray Major analgesic, inj or oral Sedative anti-convulsant, inj Anti-emetic, inj Bronchodilator inhaler Corticosteroid, inj Diuretic, inj Medication for post-partum bleeding Normal saline Acetylsalicylic acid, oral Oral beta blocker List of all medications 14
15 Supplies Sphygmomanometer Oral airway Syringes, various sizes Needles, various gauges IV catheters, various sizes Antiseptic wipes Gloves Sharps disposal box Urinary catheter IV fluid system Venous tourniquet Sponge gauze Tape adhesive Surgical mask In-flight Emergency Medical Kit Flashlight and batteries Non-mercury thermometer Emergency tracheal catheter Umbilical cord clamp BLS card ACLS card Responding to In-flight Emergency In the case of an in-flight medical emergency, the flight crew may ask for the assistance of a medical professional The following tips may help guide your interaction in an inflight emergency: Introduce yourself to the cabin crew and state your qualifications (nurse, physician, etc) Ask the patient for permission to provide care Elicit a history and perform a physical exam If the situation is critical, you may request the flight crew to consider re-routing the flight to the nearest airport in order to get expeditious medical help. You may help the ground medical crew in the transition as needed. Keep a written medical record of your encounter Only provide treatments or perform procedures for which you are qualified Source: Management/Be-Prepared-for-In-Flight-Medical- Emergencies/ 15
16 Responding to In-flight Emergencies Medical-Legal Liability Air Carrier Access Act of 1998 requires that volunteers must be "medically qualified," render care in good faith, and receive no monetary compensation to be protected under this Act. "an individual shall not be liable for damages in any action brought in a Federal or State court arising out of the acts or omissions of the individual in providing or attempting to provide assistance in the case of an inflight medical emergency unless the individual, while rendering such assistance, is guilty of gross negligence or willful misconduct." Jet Lag Jet lag usually occurs about one or two days after travel across two or more time zones Symptoms include excessive daytime sleepiness, insomnia during usual sleeping hours, fatigue, constipation Jet lag is more apparent with eastward travel Generally, it will take one day per each time zone traveled eastward to recover from jet lag and 1.5 days per each time zone traveled traveled westward Jet lag is distinguished from travel fatigue in that jet lag is related to time zones crossed whereas travel fatigue is fatigue, headache, weariness related to to travel itself Travel fatigue usually occurs during long-distance northsouth travel 16
17 Prevention of Jet Lag Goal is to prevent insomnia and excessive fatigue This is done by trying to align a traveler s internal circadian rhythm with the light-dark cycle at the destination For trips less than three days, it may not be beneficial to try to align these clocks For eastward travel longer than three days, it is recommended that a combination of timed light exposure and melatonin be used Timed Light Exposure In essence, the circadian rhythm is trained prior to travel Bright light therapy is started up to three days prior to travel The source of light can be outdoor light or a light box For eastward traveling, traveler will wake up one hour early per day and expose themselves to bright light for at least 1 hour. This is repeated for three days, trying to awaken earlier each successive day Likewise, traveler should try to go to bed one hour earlier each day 17
18 Timed Light Exposure At the destination, the goal is to expose the internal clock to bright light mid-day (avoiding bright light first thing in the morning), and then slowly waking up earlier each day There are numerous applications on smartphones that can help start timed light exposure prior to travel and also at the destination Timed Melatonin Melatonin is considered a dietary supplement by the FDA and therefore can be purchased without prescription Melatonin should be taken upon arrival at the destination, at desired bedtime The dose of melatonin ranges from 0.5 to 10 mg Higher doses do not necessarily produce quicker or more intense effects 18
19 Jet lag: Other Strategies Zolpidem has also shown to produce sleep and assist with insomnia at destination Benzodiazepines are not recommended to aid with jet lag symptoms such as insomnia Caffeine can be used in moderation for daytime fatigue Naps during the day should be limited to 30 minutes, so that the nighttime sleep is not affected Naps should be be no later than 8 hours prior to bedtime Airplane Medical Emergencies Christopher Paul, MD Assistant Professor-Clinical Department of Emergency Medicine The Ohio State University Wexner Medical Center 19
20 Almost 900 million air travelers in U.S. alone in 2015 (2015, DOT report) 2013 NEJM Study: 44,000 in-flight medical emergencies each year Cardiac Arrest, 0.3% of medical emergencies but responsible for 86% of deaths in-flight In-flight Medical Emergencies In-flight Medical Emergencies The FAA requires all American commercial airlines weighing 7,500 pounds or more and serviced by at least one flight attendant to carry an automatic external defibrillator (AED) and an enhanced emergency medical kit (EMK). AED use during the commercial flight environment has been validated as safe and effective Flight attendants must be CPR and AED certified every 2 years. 20
21 Airplane Physics Humans do not physiologically function well at altitude (>8,000-10,000 ft) without proper acclimatization Average passenger jet cruising altitude is 30,000-40,000 ft (Mt. Everest - 29,029 ft) FAA requires all flight in U.S. above 15,000 ft to be pressurized Hypoxia is biggest factor (due to reduced partial pressure of gases), along with rate of ascent and individual physiology; Barotrauma, DCS, Altitude Sickness Most U.S. are pressurized to around 8,000 ft. This creates best balance of passenger comfort and reduced stress on aircraft fuselage Physics of Flight Boyle s Law or The Pressure-Volume Law Pressure at Sea Level = 760 mmhg/14.7 psi Pressure at 30,000 ft = mmhg/4.37 psi 21
22 Physics of Flight 30,000 ft Sea Level Oxygen = 21% Nitrogen = 78% Other = 1% Oxygen = 21% Nitrogen = 78% Other = 1% Altitude-Related Illness Hypoxia Altitude Illness Barotrauma In-flight Medical Emergencies Decompression Sickness (DCS) Medical-Related Illness 22
23 Altitude-Related Illness Hypoxia - lack of oxygen to the tissues; Brain is most important usually not an issue concern if sudden loss of cabin pressure Symptoms: lightheadedness, HA, vision loss, fainting (syncope) within seconds to minutes Treatment: Oxygen! Grab the mask as quickly as possible Altitude-related illness Altitude Illness - physiologic effects on humans due to relative hypoxia from sudden changes in elevation Sea level to 7,000-8,000 ft in short amount of time (minutes) Not usually life-threatening Symptoms: HA, malaise, nausea (+/-) vomiting, lightheadedness Treatment: Supportive care; hydration, antiemetics,acetaminophen / ibuprofen for HA 23
24 Altitude-Related Illness Barotrauma - Injuries caused by increased air or water pressure, such as during airplane flights or scuba diving occurs as the cabin is pressurized on ascent; there is still a pressure difference between the air that is trapped in your body (higher pressure) and the air in the cabin (lower pressure) air wants to move from high pressure to low pressure; so it expands expansion of air most often in ears (eustachian tubes) and sinuses; but also in bowels and lungs Symptoms: Ear pain, headaches, sinus pressure, eye pain, bloating, but in rare cases - eardrum rupture, pneumothorax Treatment: Equilibration; clearing your ears, passing flatus (gas), needle decompression Altitude-Related Illness Decompression Sickness (DCS) - when dissolved gases (mainly nitrogen) come out of solution (water/blood) in bubbles and can affect just about any body area including joints, lung, heart, skin and brain very rare in healthy individuals and pressurized spaces below 18,000 ft; some risk if person was recently diving however (within 24hrs) Symptoms: stroke symptoms, neurologic deficits, headache, joint pain, skin pain, chest pain Prevention: breathing100% oxygen prior to takeoff to flush nitrogen out of tissues; not practical, not 100% effective Treatment: 100% O2 until a decompression chamber can be reached; if loss of consciousness with clear risk factors this is a medical emergency 24
25 Medical-Related Illness Approach to the In-flight Medical Emergency Identify yourself and your training/expertise Treat in the seat whenever possible; use of the aisle blocks mobility of flight crew Document your findings and treatments administered Communicate and coordinate with flight crew and ground resources (MedAire, STAT-MD) Do not attempt to practice beyond your expertise Request access to the emergency medical kit (EMK) Use a translator if necessary Medical-Related Illness In a review of recent literature on in-flight emergencies these are stated to be the most common (source: Singapore Med J Jan; 58(1): Near-syncope (lightheadedness) - 37% Respiratory Symptoms % Nausea/Vomiting - 9.5% Cardiac Symptoms - 7.7% Seizures - 5.8% Abdominal Pain - 4.1% 25
26 Medical-Related Illness Syncope - Assess vital signs, cardiovascular exam, and neurological exam. Recommend diversion for hypotension, arrhythmia, or suspected stroke. Altered Mental Status - Assess for toxidromes. Administer oxygen, establish intravenous access and administer normal saline and dextrose 50%. Seizure - Clear space around passenger. Administer sedative/anticonvulsant (benziodiazepine if available). Provide supportive care during post-ictal period. Recommend diversion for status epilepticus. Medical-Related Illness Medical-Related Illness Chest Pain - Assess vital signs. Perform cardiovascular and respiratory exam. Administer oxygen, nitroglycerin, and aspirin. Recommend diversion for arrhythmia, abnormal vital signs, or concern for myocardial infarction. Respiratory Asthma Exacerbation -Administer inhaled bronchodilator and oxygen. Consider intravenous steroid for moderate to severe symptoms. Consider intramuscular epinephrine (0.3 to 0.5 ml of 1:1000 solution) for severe symptoms. PTX - Perform needle thoracostomy for suspected tension pneumothorax (unequal breath sounds, chest pain, dyspnea). Recommend diversion. CHF - Administer oxygen, assess vital signs and establish intravenous access. Administer oral nitroglycerin and intravenous diuretic. Recommend diversion. 26
27 Medical-Related Illness Allergic Reaction - For mild allergic reaction, administer intravenous antihistamine and corticosteroids. For severe allergic reaction/anaphylaxis, administer intramuscular epinephrine (0.3 to 0.5 ml of 1:1000 solution). GI Symptoms - Administer antiemetic. Establish intravenous access and administer normal saline. Pregnancy - Assess vital signs and establish intravenous access. Recommend diversion for abdominal pain or vaginal bleeding. Emergency Medical Kit (EMK) Source: 27
28 Emergency Medical Kit (EMK) Minimum requirements in EMK mandated by FAA Most airlines supplements with a variety of addition medications Automated External Defibrillator (AED) Required by FAA on U.S. Airlines since 2001 Pilot study published in the Oct. 26, 2000 issue of The New England Journal of Medicine, researchers had tracked the results of an American Airlines program in which flight attendants were trained in using AEDs. Devices were used on 200 people who were experiencing cardiac arrest, and 40 percent of those treated with an AED survived 28
29 Automated External Defibrillator (AED) 29
Air Traveler s Health: Considerations for Travelers with Pulmonary Disease
 Air Traveler s Health: Considerations for Travelers with Pulmonary Disease Sindhu Mukku, MD Assistant Professor of Internal Medicine Department of Internal Medicine Division of Pulmonary, Critical Care
Air Traveler s Health: Considerations for Travelers with Pulmonary Disease Sindhu Mukku, MD Assistant Professor of Internal Medicine Department of Internal Medicine Division of Pulmonary, Critical Care
1 out of every 5,555 of drivers dies in car accidents 1 out of every 7692 pregnant women die from complications 1 out of every 116,666 skydives ended
 1 out of every 5,555 of drivers dies in car accidents 1 out of every 7692 pregnant women die from complications 1 out of every 116,666 skydives ended in a fatality in 2000 1 out of every 126,626 marathon
1 out of every 5,555 of drivers dies in car accidents 1 out of every 7692 pregnant women die from complications 1 out of every 116,666 skydives ended in a fatality in 2000 1 out of every 126,626 marathon
SCUBA - self contained underwater breathing apparatus. 5 million sport scuba divers in U.S. 250, ,000 new certifications annually in U.S.
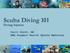 SCUBA - self contained underwater breathing apparatus 5 million sport scuba divers in US 250,000-400,000 new certifications annually in US Diving occurs in oceans, freshwater lakes, rivers and quarries
SCUBA - self contained underwater breathing apparatus 5 million sport scuba divers in US 250,000-400,000 new certifications annually in US Diving occurs in oceans, freshwater lakes, rivers and quarries
Respiratory Signs: Tachypnea (RR>30/min), Desaturation, Shallow breathing, Use of accessory muscles Breathing sound: Wheezing, Rhonchi, Crepitation.
 Respiratory Signs: Tachypnea (RR>30/min), Desaturation, Shallow breathing, Use of accessory muscles Breathing sound: Wheezing, Rhonchi, Crepitation. Paradoxical breathing Hyper-resonance on percussion:
Respiratory Signs: Tachypnea (RR>30/min), Desaturation, Shallow breathing, Use of accessory muscles Breathing sound: Wheezing, Rhonchi, Crepitation. Paradoxical breathing Hyper-resonance on percussion:
Clinical Skills. Administering Oxygen
 Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
MEDICAL DEPARTMENT PASSENGER INFORMATION PHYSICIAN INFORMATION
 MON-FRI 06:00-20:00 EST MEDICAL DEPARTMENT SAT-SUN 06:00-18 :00 EST Email : acmedical@aircanada.ca Fax 1-888-334-7717 (Toll-free from North America) Telephone 1-800-667-4732 (Toll-free from North America)
MON-FRI 06:00-20:00 EST MEDICAL DEPARTMENT SAT-SUN 06:00-18 :00 EST Email : acmedical@aircanada.ca Fax 1-888-334-7717 (Toll-free from North America) Telephone 1-800-667-4732 (Toll-free from North America)
All Programs. CROSS REFERENCE: Initiation, Titration and Discontinuation of Oxygen Therapy for Adult Patients Medical Directive
 1 All Programs SUBJECT: Oxygen Standard of Care for the Adult Patient ISSUING BODY: Nursing Practice Council, Respiratory Therapy Services, Physiotherapy Practice Council and Occupational Therapy Practice
1 All Programs SUBJECT: Oxygen Standard of Care for the Adult Patient ISSUING BODY: Nursing Practice Council, Respiratory Therapy Services, Physiotherapy Practice Council and Occupational Therapy Practice
Physiology of Flight
 Physiology of Flight Physiology of Flight Physiology of flight: how the human body functions during flight Overview 1. Physiological Divisions of the Atmosphere 2. Hypoxia and Hyperventilation 3. Trapped
Physiology of Flight Physiology of Flight Physiology of flight: how the human body functions during flight Overview 1. Physiological Divisions of the Atmosphere 2. Hypoxia and Hyperventilation 3. Trapped
Breathe easier. Patient guide to oxygen therapy
 Breathe easier Patient guide to oxygen therapy Table of contents The facts about COPD The facts about COPD 3 Understanding oxygen therapy 4 Choices in oxygen therapy equipment You have been prescribed
Breathe easier Patient guide to oxygen therapy Table of contents The facts about COPD The facts about COPD 3 Understanding oxygen therapy 4 Choices in oxygen therapy equipment You have been prescribed
Adult, Child and Infant Exam
 CPR Pro for the Professional Rescuer Adult, Child and Infant Exam Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer sheet provided.
CPR Pro for the Professional Rescuer Adult, Child and Infant Exam Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer sheet provided.
Espilat Mountaineering Club
 In the name of God Espilat Mountaineering Club May 2013 MEDICAL PROBLEMS IN HIGH MOUNTAIN ENVIRONMENTS Arya Hamedanchi MD, MPH Level one International Anthropometrist International Certificate of Ski Medicine
In the name of God Espilat Mountaineering Club May 2013 MEDICAL PROBLEMS IN HIGH MOUNTAIN ENVIRONMENTS Arya Hamedanchi MD, MPH Level one International Anthropometrist International Certificate of Ski Medicine
On the Go with Oxygen
 On the Go with Oxygen People with chronic lung disease may need oxygen therapy. Oxygen therapy is used to normalize the oxygen level in blood during sleep, rest, activity and during acute illnesses in
On the Go with Oxygen People with chronic lung disease may need oxygen therapy. Oxygen therapy is used to normalize the oxygen level in blood during sleep, rest, activity and during acute illnesses in
Medical Section. Fax : (toll-free) or
 Departure Date: Medical Section Hours of Operation MON-FRI 06:00-20:00 EST SAT-SUN 06:00-18 :00 EST Email : acmedical@aircanada.ca Fax : 1 888 334-7717 (toll-free) or 514 205-7567 Telephone : 1 800 667-4732
Departure Date: Medical Section Hours of Operation MON-FRI 06:00-20:00 EST SAT-SUN 06:00-18 :00 EST Email : acmedical@aircanada.ca Fax : 1 888 334-7717 (toll-free) or 514 205-7567 Telephone : 1 800 667-4732
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Medications POLICY NUMBER: 512. Effective Date: August 31, 2006
 SUBJECT: OXYGEN (O 2 ) THERAPY COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Medications POLICY NUMBER: 512 Effective Date: August 31, 2006 1. GENERAL CONSIDERATIONS A. Individuals
SUBJECT: OXYGEN (O 2 ) THERAPY COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Medications POLICY NUMBER: 512 Effective Date: August 31, 2006 1. GENERAL CONSIDERATIONS A. Individuals
Lung Volumes and Capacities
 Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
Medical Issues in Aviation
 Medical Issues in Aviation Passenger Fitness to Fly Lima, Peru, April 2009 Claude Thibeault MD Medical Advisor Lima 2009 1 Passenger Fitness to Fly Plan - Review real cases based on altitude physiology
Medical Issues in Aviation Passenger Fitness to Fly Lima, Peru, April 2009 Claude Thibeault MD Medical Advisor Lima 2009 1 Passenger Fitness to Fly Plan - Review real cases based on altitude physiology
High Altitude Concerns
 High Altitude Concerns 17 March, 2014 PRESENTED BY: John M. Davenport, Lt. Col., USAF, Ret. International Operators Conference Tampa, FL March 17 20, 2014 Welcome Aviators! High Altitude Concerns Question
High Altitude Concerns 17 March, 2014 PRESENTED BY: John M. Davenport, Lt. Col., USAF, Ret. International Operators Conference Tampa, FL March 17 20, 2014 Welcome Aviators! High Altitude Concerns Question
OXYGEN FOR ADULTS IN ACUTE CARE
 PATIENT GROUP DIRECTION FOR THE ADMINISTRATION OF OXYGEN FOR ADULTS IN ACUTE CARE ALL CLINICAL DIVISIONS ADULT CARE STATEMENT The staff indicated in Staff Group may administer oxygen in the two detailed
PATIENT GROUP DIRECTION FOR THE ADMINISTRATION OF OXYGEN FOR ADULTS IN ACUTE CARE ALL CLINICAL DIVISIONS ADULT CARE STATEMENT The staff indicated in Staff Group may administer oxygen in the two detailed
COALINGA STATE HOSPITAL. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
Medical Aspects of Diving in the Offshore Oil Industry
 Medical Aspects of Diving in the Offshore Oil Industry Dr Stephen Watt Retired Consultant in Respiratory and Hyperbaric Medicine Chairman, Diving Medical Advisory Committee What is diving? Diving = Commuting
Medical Aspects of Diving in the Offshore Oil Industry Dr Stephen Watt Retired Consultant in Respiratory and Hyperbaric Medicine Chairman, Diving Medical Advisory Committee What is diving? Diving = Commuting
American College of Occupational and Preventive Medicine 2011 Annual Meeting, Orlando, Florida, November 2, 2011
 Administrative Information Risk Assessment: Low AEROSPACE/ OCCUPATIONAL MEDICINE BAROMETRIC CONCERNS Dr. John Campbell, MFS Environmental Considerations: None Safety Considerations: None Evaluation: 50
Administrative Information Risk Assessment: Low AEROSPACE/ OCCUPATIONAL MEDICINE BAROMETRIC CONCERNS Dr. John Campbell, MFS Environmental Considerations: None Safety Considerations: None Evaluation: 50
Royal Brompton Hospital Standard Operating Procedure Six Minute Walk Test (6MWT)
 Royal Brompton Hospital Standard Operating Procedure Six Minute Walk Test (6MWT) Scope and Purpose The original purpose of the six minute walk test was to assess exercise tolerance in patients with chronic
Royal Brompton Hospital Standard Operating Procedure Six Minute Walk Test (6MWT) Scope and Purpose The original purpose of the six minute walk test was to assess exercise tolerance in patients with chronic
Respiration (revised 2006) Pulmonary Mechanics
 Respiration (revised 2006) Pulmonary Mechanics PUL 1. Diagram how pleural pressure, alveolar pressure, airflow, and lung volume change during a normal quiet breathing cycle. Identify on the figure the
Respiration (revised 2006) Pulmonary Mechanics PUL 1. Diagram how pleural pressure, alveolar pressure, airflow, and lung volume change during a normal quiet breathing cycle. Identify on the figure the
Office. Hypoxia. Or this. Or even this. Hypoxia E-1. COL Brian W. Smalley DO, MSPH, CPE
 Hypoxia Office COL Brian W. Smalley DO, MSPH, CPE Or this Or even this Hypoxia State of oxygen deficiency in the blood cells and tissues sufficient to cause impairment of function 4 Types Hypoxic Hypemic
Hypoxia Office COL Brian W. Smalley DO, MSPH, CPE Or this Or even this Hypoxia State of oxygen deficiency in the blood cells and tissues sufficient to cause impairment of function 4 Types Hypoxic Hypemic
O-1. American Osteopathic College of Occupational and Preventive Medicine 2013 Mid Year Educational Conference, Phoenix, Arizona February 14-17, 2013
 Administrative Information Risk Assessment: Low AEROSPACE/ OCCUPATIONAL MEDICINE BAROMETRIC CONCERNS Dr. John Campbell, DO, MPH, MFS Environmental Considerations: None Safety Considerations: None Evaluation:
Administrative Information Risk Assessment: Low AEROSPACE/ OCCUPATIONAL MEDICINE BAROMETRIC CONCERNS Dr. John Campbell, DO, MPH, MFS Environmental Considerations: None Safety Considerations: None Evaluation:
Some Diving Physics and Physiology; Barotrauma. Robbert Hermanns Occupational Health Risk Management Services Ltd
 Some Diving Physics and Physiology; Barotrauma Robbert Hermanns Occupational Health Risk Management Services Ltd Oil & Gas UK (EBS) conference th 24 May 2017 Dr Robbert Hermanns MFOM Robbert.hermanns@ohrms.co.uk
Some Diving Physics and Physiology; Barotrauma Robbert Hermanns Occupational Health Risk Management Services Ltd Oil & Gas UK (EBS) conference th 24 May 2017 Dr Robbert Hermanns MFOM Robbert.hermanns@ohrms.co.uk
A V A L A N C H E R E S C U E
 AVALANCHE RESCUE The On-Site Triage And Evacuation Of Avalanche Victims Statistics De Quervain s Mortality Curve 1945 to 1979 and 1979 to 1989 2,611 cases, buried at average 1.06 m After 1 hour 30-40%
AVALANCHE RESCUE The On-Site Triage And Evacuation Of Avalanche Victims Statistics De Quervain s Mortality Curve 1945 to 1979 and 1979 to 1989 2,611 cases, buried at average 1.06 m After 1 hour 30-40%
Breathe easier. Patient guide to oxygen therapy
 Breathe easier Patient guide to oxygen therapy Table of contents The facts about COPD 3 Understanding oxygen therapy 4 Choices in oxygen therapy equipment 5 Safely living with oxygen 8 Traveling with oxygen
Breathe easier Patient guide to oxygen therapy Table of contents The facts about COPD 3 Understanding oxygen therapy 4 Choices in oxygen therapy equipment 5 Safely living with oxygen 8 Traveling with oxygen
Decompression Sickness
 Decompression Sickness Kun-Lun Huang National Defense Medical Center Undersea and Hyperbaric Medical Institute Tri-Service General Hospital Department of Undersea and Hyperbaric Medicine Hazard Diving
Decompression Sickness Kun-Lun Huang National Defense Medical Center Undersea and Hyperbaric Medical Institute Tri-Service General Hospital Department of Undersea and Hyperbaric Medicine Hazard Diving
Breathing Process: Inhalation
 Airway Chapter 6 Breathing Process: Inhalation Active part of breathing Diaphragm and intercostal muscles contract, allowing the lungs to expand. The decrease in pressure allows lungs to fill with air.
Airway Chapter 6 Breathing Process: Inhalation Active part of breathing Diaphragm and intercostal muscles contract, allowing the lungs to expand. The decrease in pressure allows lungs to fill with air.
b. Provide consultation service to physicians referring patients. c. Participate in weekly wound care clinic and biweekly diving medicine clinic.
 Curriculum: 1. Required clinical activities: a. Participate in HBO 2 clinical operations by monitoring daily treatment sessions and emergency on-call treatments at least 4 days/week, b. Provide consultation
Curriculum: 1. Required clinical activities: a. Participate in HBO 2 clinical operations by monitoring daily treatment sessions and emergency on-call treatments at least 4 days/week, b. Provide consultation
Chapter 9 Airway Respirations Metabolism Oxygen Requirements Respiratory Anatomy Respiratory Anatomy Respiratory Anatomy Diaphragm
 1 Chapter 9 Airway 2 Respirations Every cell of the body requires to survive Oxygen must come in and carbon must go out 3 Metabolism Metabolism--Process where the body s cells convert food to Adequate
1 Chapter 9 Airway 2 Respirations Every cell of the body requires to survive Oxygen must come in and carbon must go out 3 Metabolism Metabolism--Process where the body s cells convert food to Adequate
OXYGEN THERAPY. (Non-invasive O2 therapy in patient >8yrs)
 OXYGEN THERAPY (Non-invasive O2 therapy in patient >8yrs) Learning aims Indications and precautions for O2 therapy Targets of therapy Standard notation O2 delivery devices Taps, tanks and tubing Notation
OXYGEN THERAPY (Non-invasive O2 therapy in patient >8yrs) Learning aims Indications and precautions for O2 therapy Targets of therapy Standard notation O2 delivery devices Taps, tanks and tubing Notation
OUTLINE SHEET Respond to an emergency per current American Red Cross standards.
 INTRODUCTION OUTLINE SHEET 2.2-1 PRACTICAL FIRST AID TRAINING/MOCK TRAUMA PAGE 1 of 8 First Aid, in any situation, consists of emergency treatment of the sick or injured before medical help can be obtained.
INTRODUCTION OUTLINE SHEET 2.2-1 PRACTICAL FIRST AID TRAINING/MOCK TRAUMA PAGE 1 of 8 First Aid, in any situation, consists of emergency treatment of the sick or injured before medical help can be obtained.
Air Travel with Respiratory Disease
 Air Travel with Respiratory Disease Introduction Over 25 years ago it was already estimated that more than 5% of air travelers have a chronic respiratory disease Over one billion people travel by air each
Air Travel with Respiratory Disease Introduction Over 25 years ago it was already estimated that more than 5% of air travelers have a chronic respiratory disease Over one billion people travel by air each
ALTITUDE PHYSIOLOGY. Physiological Zones of the Atmosphere. Composition of the Air AIR ATTENDANTS COURSE. Sea Level Pressure
 AIR ATTENDANTS COURSE ALTITUDE PHYSIOLOGY Physical Divisions of the Atmosphere 1200 miles 600 miles EXOSPHERE Physiological Zones of the Atmosphere 50 miles IONOSPHERE SPACE EQUIVALENT ZONE: 50,000 feet
AIR ATTENDANTS COURSE ALTITUDE PHYSIOLOGY Physical Divisions of the Atmosphere 1200 miles 600 miles EXOSPHERE Physiological Zones of the Atmosphere 50 miles IONOSPHERE SPACE EQUIVALENT ZONE: 50,000 feet
Chapter 39. Six Minute Walk Test (6MWT)
 Chapter 39. Six Minute Walk Test (6MWT) 39.1 Introduction This MOP chapter is designed to guide the performance of the 6-minute walk test (6MWT) using standardized procedures and techniques in order to
Chapter 39. Six Minute Walk Test (6MWT) 39.1 Introduction This MOP chapter is designed to guide the performance of the 6-minute walk test (6MWT) using standardized procedures and techniques in order to
REEFTRIP.com. Medical Questionnaire Dive Medical Recreational AS Section Abbott Street, Cairns T: E:
 REEFTRIP.com 100 Abbott Street, Cairns T: 07 4037 2700 E: info@reeftrip.com Medical Questionnaire Dive Medical Recreational AS4005.1 Please complete the following Section 1 1 Surname: Given Names 2 Date
REEFTRIP.com 100 Abbott Street, Cairns T: 07 4037 2700 E: info@reeftrip.com Medical Questionnaire Dive Medical Recreational AS4005.1 Please complete the following Section 1 1 Surname: Given Names 2 Date
Diving Accident Management
 Diving Accident Management From Diving Medicine Online http://scuba-doc.com/ 3/8/2004 Diving Medicine Online 1 Introduction! It is desirable to have a standard approach to the initial management (i.e.
Diving Accident Management From Diving Medicine Online http://scuba-doc.com/ 3/8/2004 Diving Medicine Online 1 Introduction! It is desirable to have a standard approach to the initial management (i.e.
SECOND EUROPEAN CONSENSUS CONFERENCE ON HYPERBARIC MEDICINE THE TREATMENT OF DECOMPRESSION ACCIDENTS IN RECREATIONAL DIVING
 SECOND EUROPEAN CONSENSUS CONFERENCE ON HYPERBARIC MEDICINE THE TREATMENT OF DECOMPRESSION ACCIDENTS IN RECREATIONAL DIVING MARSEILLE, May 8-10, 1996 RECOMMENDATIONS OF THE JURY* QUESTION 1 : Is there
SECOND EUROPEAN CONSENSUS CONFERENCE ON HYPERBARIC MEDICINE THE TREATMENT OF DECOMPRESSION ACCIDENTS IN RECREATIONAL DIVING MARSEILLE, May 8-10, 1996 RECOMMENDATIONS OF THE JURY* QUESTION 1 : Is there
NOTE: If not used, provider must document reason(s) for deferring mechanical ventilation in a patient with an advanced airway
 APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
DRAFT U S E R M A N U A L CAUTION. Model: 19MFA1001 Series. Federal (USA) law restricts this device to sale by or on the order of a physician.
 U S E R M A N U A L Model: 19MFA1001 Series SAVE THESE INSTRUCTIONS Federal (USA) law restricts this device to sale by or on the order of a physician. 300 Held Drive Tel: (+001) 610-262-6090 Northampton,
U S E R M A N U A L Model: 19MFA1001 Series SAVE THESE INSTRUCTIONS Federal (USA) law restricts this device to sale by or on the order of a physician. 300 Held Drive Tel: (+001) 610-262-6090 Northampton,
Administrative Procedures Automated External Defibrillator (AED)
 Administrative Procedures Automated External Defibrillator (AED) PURPOSE: The purpose of these procedures is to give guidance to those employees of the Lynden School District who are trained and willing
Administrative Procedures Automated External Defibrillator (AED) PURPOSE: The purpose of these procedures is to give guidance to those employees of the Lynden School District who are trained and willing
Rescue Swimmer Refresher Course. Practical First Aid Training/Mock Trauma LT 2.2
 Rescue Swimmer Refresher Course Practical First Aid Training/Mock Trauma LT 2.2 Enabling Objectives Respond to an emergency per current American Red Cross standards. Administer CPR per current American
Rescue Swimmer Refresher Course Practical First Aid Training/Mock Trauma LT 2.2 Enabling Objectives Respond to an emergency per current American Red Cross standards. Administer CPR per current American
Acute Mountain Sickness
 Innere Medizin VII / Sportmedizin Acute Mountain Sickness Peter Bärtsch www.klinikum.uni-heidelberg.de/sportmedizin AMS: Clinical Picture Symptoms: - Headache - Loss of appetite, nausea, vomiting - Dizziness
Innere Medizin VII / Sportmedizin Acute Mountain Sickness Peter Bärtsch www.klinikum.uni-heidelberg.de/sportmedizin AMS: Clinical Picture Symptoms: - Headache - Loss of appetite, nausea, vomiting - Dizziness
Guarding for Organized Swim Groups
 Day 2 Inspection Guarding for Organized Swim Groups Organized groups may visit your facility. Day care groups Camps Youth organizations Groups can be part of your facility or an outside group They should
Day 2 Inspection Guarding for Organized Swim Groups Organized groups may visit your facility. Day care groups Camps Youth organizations Groups can be part of your facility or an outside group They should
Oxygen Therapy. What tests can be done to determine the need for oxygen?
 Oxygen Therapy Oxygen is in the air we breathe and is necessary to live. When we breathe in, oxygen enters the lungs and it goes into the blood. When the lungs cannot transfer enough oxygen into the blood,
Oxygen Therapy Oxygen is in the air we breathe and is necessary to live. When we breathe in, oxygen enters the lungs and it goes into the blood. When the lungs cannot transfer enough oxygen into the blood,
Essential Skills Course Acute Care Module. Respiratory Day 2 (Arterial Blood Gases) Pre course Workbook
 Essential Skills Course Acute Care Module Respiratory Day 2 (Arterial Blood Gases) Pre course Workbook Acknowledgements This pre course workbook has been complied and updated with reference to the original
Essential Skills Course Acute Care Module Respiratory Day 2 (Arterial Blood Gases) Pre course Workbook Acknowledgements This pre course workbook has been complied and updated with reference to the original
Deborah Dewaay MD Division of General Internal Medicine and Geriatrics Hospital Medicine Acknowledgment: Antine Stenbit MD
 Deborah Dewaay MD Division of General Internal Medicine and Geriatrics Hospital Medicine 2013 Acknowledgment: Antine Stenbit MD Objectives Knowledge: Understand the difference between hypoxia and hypoxemia
Deborah Dewaay MD Division of General Internal Medicine and Geriatrics Hospital Medicine 2013 Acknowledgment: Antine Stenbit MD Objectives Knowledge: Understand the difference between hypoxia and hypoxemia
Subject: Oxygen DESCRIPTION: POSITION STATEMENT: Original Effective Date: 10/03/00. Reviewed: 08/23/18. Revised: 09/15/18
 09-E0400-00 Original Effective Date: 10/03/00 Reviewed: 08/23/18 Revised: 09/15/18 Subject: Oxygen THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION OF BENEFITS, OR A
09-E0400-00 Original Effective Date: 10/03/00 Reviewed: 08/23/18 Revised: 09/15/18 Subject: Oxygen THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION OF BENEFITS, OR A
ISAF OFFSHORE SPECIAL REGULATIONS Appendix E
 Formatted Page - 72 - APPENDIX E Hypothermia WHAT IS IT? A condition in which exposure to cold air and/or water lowers body core temperature. Death can result from too low a brain and heart temperature.
Formatted Page - 72 - APPENDIX E Hypothermia WHAT IS IT? A condition in which exposure to cold air and/or water lowers body core temperature. Death can result from too low a brain and heart temperature.
Diving Medicine USN Diver/SEAL Submarine Overview / Tom Kersch, CAPT, MC!!
 Diving Medicine USN Diver/SEAL Submarine Overview / Tom Kersch, CAPT, MC Diving Medicine USN Diver/SEAL Submarine Overview Tom Kersch CAPT, MC SEAL Deliver Vehicle Team 1 Pearl City, HI 1 Content Attestation
Diving Medicine USN Diver/SEAL Submarine Overview / Tom Kersch, CAPT, MC Diving Medicine USN Diver/SEAL Submarine Overview Tom Kersch CAPT, MC SEAL Deliver Vehicle Team 1 Pearl City, HI 1 Content Attestation
Circulatory And Respiration
 Circulatory And Respiration Composition Of Blood Blood Heart 200mmHg 120mmHg Aorta Artery Arteriole 50mmHg Capillary Bed Venule Vein Vena Cava Heart Differences Between Arteries and Veins Veins transport
Circulatory And Respiration Composition Of Blood Blood Heart 200mmHg 120mmHg Aorta Artery Arteriole 50mmHg Capillary Bed Venule Vein Vena Cava Heart Differences Between Arteries and Veins Veins transport
The physiological functions of respiration and circulation. Mechanics. exercise 7. Respiratory Volumes. Objectives
 exercise 7 Respiratory System Mechanics Objectives 1. To explain how the respiratory and circulatory systems work together to enable gas exchange among the lungs, blood, and body tissues 2. To define respiration,
exercise 7 Respiratory System Mechanics Objectives 1. To explain how the respiratory and circulatory systems work together to enable gas exchange among the lungs, blood, and body tissues 2. To define respiration,
Outdoor Medicine 2010
 Outdoor Medicine 2010 Outdoor Medicine Preparation Priorities Common injuries and illnesses High altitude illness Preparation Itinerary Extra food and water, filter or iodine Clothes base layer, insulation,
Outdoor Medicine 2010 Outdoor Medicine Preparation Priorities Common injuries and illnesses High altitude illness Preparation Itinerary Extra food and water, filter or iodine Clothes base layer, insulation,
EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES
 GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
Civil Air Patrol Auxiliary of the United States Air Force
 Mountain Flying Qualification Course Civil Air Patrol Auxiliary of the United States Air Force Physiological Effects of Altitude Physiological Effects of Altitude OXYGEN DEPRIVATION (HYPOXIA) SINUS PRESSURE
Mountain Flying Qualification Course Civil Air Patrol Auxiliary of the United States Air Force Physiological Effects of Altitude Physiological Effects of Altitude OXYGEN DEPRIVATION (HYPOXIA) SINUS PRESSURE
Hyperbaric Oxygen Therapy
 Hyperbaric Oxygen Therapy WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017 RN.ORG, S.A.,
Hyperbaric Oxygen Therapy WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017 RN.ORG, S.A.,
FIRST AID (CPR) Yerevan Dc. Anna Toplaghaltsyan
 FIRST AID (CPR) Yerevan 2018 Dc. Anna Toplaghaltsyan First aid is The assistance given to any person suffering a sudden illness or injury, with care provided to preserve life, prevent the condition from
FIRST AID (CPR) Yerevan 2018 Dc. Anna Toplaghaltsyan First aid is The assistance given to any person suffering a sudden illness or injury, with care provided to preserve life, prevent the condition from
OXYGEN THERAPY. Teaching plan
 OXYGEN THERAPY Teaching plan To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may give each learner a copy of the
OXYGEN THERAPY Teaching plan To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may give each learner a copy of the
Capnography in the Veterinary Technician Toolbox. Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA
 Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
Nitrous Oxide Sedation
 Princess Margaret Hospital for Children GUIDELINE Nitrous Oxide Sedation Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children GUIDELINE Nitrous Oxide Sedation Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Hyperbaric Oxygen Therapy
 1 RSPT 1410 Medical Gas Therapy Part 2: Wilkins: Chapter 38; p. 891-894 Cairo: Chapter 3, p. 78-81 2 Definitions Hyperbaric oxygen (HBO) therapy is the therapeutic use of oxygen at pressures greater than
1 RSPT 1410 Medical Gas Therapy Part 2: Wilkins: Chapter 38; p. 891-894 Cairo: Chapter 3, p. 78-81 2 Definitions Hyperbaric oxygen (HBO) therapy is the therapeutic use of oxygen at pressures greater than
Mechanical Ventilation
 Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
2) an acute situation in which hypoxemia is suspected.
 I. Subject: Oxygen Therapy II. Policy: Oxygen therapy shall be initiated upon a physician's order by health care professionals trained in the set-up and principles of safe oxygen administration. Oxygen
I. Subject: Oxygen Therapy II. Policy: Oxygen therapy shall be initiated upon a physician's order by health care professionals trained in the set-up and principles of safe oxygen administration. Oxygen
Understanding Tracheostomy Care
 Understanding Tracheostomy Care Inside this guide: This guide will help you learn how to take care of your tracheostomy (trach). It is important to ask questions. You will be given time to learn. Working
Understanding Tracheostomy Care Inside this guide: This guide will help you learn how to take care of your tracheostomy (trach). It is important to ask questions. You will be given time to learn. Working
Rodney Shandukani 14/03/2012
 Rodney Shandukani 14/03/2012 OXYGEN THERAPY Aerobic metabolism accounts for 90% of Oxygen consumption by tissues. generates ATP by oxidative phosphorylation. Oxygen cascade: Oxygen exerts a partial pressure,
Rodney Shandukani 14/03/2012 OXYGEN THERAPY Aerobic metabolism accounts for 90% of Oxygen consumption by tissues. generates ATP by oxidative phosphorylation. Oxygen cascade: Oxygen exerts a partial pressure,
Revisiting respiratory failure
 Clinical corner Revisiting respiratory failure by Richard D. Pinson, MD, FACP, CCS The diagnosis and documentation of respiratory failure continues to be challenging for coders, documentation specialists,
Clinical corner Revisiting respiratory failure by Richard D. Pinson, MD, FACP, CCS The diagnosis and documentation of respiratory failure continues to be challenging for coders, documentation specialists,
BC EMR Evaluation Checklist Femur Fracture
 Call Details: Called to the parking lot at Home Depot for a 33 year old male hit by a car. Instructions to role players: You are a 33 year old male who was putting bags in your truck when another car backed
Call Details: Called to the parking lot at Home Depot for a 33 year old male hit by a car. Instructions to role players: You are a 33 year old male who was putting bags in your truck when another car backed
Virginia Office of Emergency Medical Services Scope of Practice - Procedures for EMS Personnel
 Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Oropharyngeal Airway Nasopharyngeal Airway Head
Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Oropharyngeal Airway Nasopharyngeal Airway Head
CHAPTER 3: TAKING ACTION AND CARING FOR BREATHING EMERGENCIES Multiple Choice
 CHAPTER 3: TAKING ACTION AND CARING FOR BREATHING EMERGENCIES Multiple Choice Circle the correct answer. 1. One of the first steps to follow in an emergency is a. Transporting the victim to the hospital.
CHAPTER 3: TAKING ACTION AND CARING FOR BREATHING EMERGENCIES Multiple Choice Circle the correct answer. 1. One of the first steps to follow in an emergency is a. Transporting the victim to the hospital.
MEDICAL INFORMATION FORM (MEDIF) FOR AIR TRAVEL
 INFORMATION SHEET FOR PASSENGER REQUIRING SPECIAL ASSISTANCE PART 1 - TO BE COMPLETED BY THE PASSENGER PLEASE COMPLETE THE FORM IN CAPITAL LETTERS A Last Name/First Name/Title B Passenger Name Record (PNR)
INFORMATION SHEET FOR PASSENGER REQUIRING SPECIAL ASSISTANCE PART 1 - TO BE COMPLETED BY THE PASSENGER PLEASE COMPLETE THE FORM IN CAPITAL LETTERS A Last Name/First Name/Title B Passenger Name Record (PNR)
E. Emergency Incident Rehabilitation
 E. Emergency Incident Rehabilitation Review of Injury/Illness: DHS/EMS personnel may be assigned to assist with disasters, exercises, and other emergency operations throughout the United States. This protocol
E. Emergency Incident Rehabilitation Review of Injury/Illness: DHS/EMS personnel may be assigned to assist with disasters, exercises, and other emergency operations throughout the United States. This protocol
Student Guide Preview. BasicPlus. CPR, AED, and First Aid For Adults
 Student Guide Preview BasicPlus CPR, AED, and First Aid For Adults BasicPlus CPR, AED, and First Aid For Adults Student Guide Version 7.0 Purpose of this Guide This MEDIC First Aid BasicPlus Version 7.0
Student Guide Preview BasicPlus CPR, AED, and First Aid For Adults BasicPlus CPR, AED, and First Aid For Adults Student Guide Version 7.0 Purpose of this Guide This MEDIC First Aid BasicPlus Version 7.0
I. Pharmacology Simulation Scenario: Tension Pneumothorax
 I. Pharmacology Simulation Scenario: Tension Pneumothorax II. Target Audience: 1 st and 2 nd year medical students III. Learning Objectives A. Primary 1. Develop a plausible differential diagnosis from
I. Pharmacology Simulation Scenario: Tension Pneumothorax II. Target Audience: 1 st and 2 nd year medical students III. Learning Objectives A. Primary 1. Develop a plausible differential diagnosis from
Pomona College Automated External Defibrillator (AED) Program
 Pomona College Automated External Defibrillator (AED) Program Introduction To help ensure the safety and well-being of the Pomona College community and visitors to campus, Pomona College is increasing
Pomona College Automated External Defibrillator (AED) Program Introduction To help ensure the safety and well-being of the Pomona College community and visitors to campus, Pomona College is increasing
Unit 3: The Physiology of Diving and Nitrox
 Unit 3: The Physiology of Diving and Nitrox Narcosis Decompression Sickness Physiological Effects of High Oxygen Levels Physiological Effects of High Oxygen Levels Student Performance: By the end of the
Unit 3: The Physiology of Diving and Nitrox Narcosis Decompression Sickness Physiological Effects of High Oxygen Levels Physiological Effects of High Oxygen Levels Student Performance: By the end of the
Outline What is it and what to expect Pilot physiology Oxygen equipment per FAA Wave windows Relevant FAR s NCSA Rules
 Northern California Soaring Association 2010 Safety Seminar High Altitude Wave Flight Considerations by Mike Voie, CFIG Outline What is it and what to expect Pilot physiology Oxygen equipment per FAA Wave
Northern California Soaring Association 2010 Safety Seminar High Altitude Wave Flight Considerations by Mike Voie, CFIG Outline What is it and what to expect Pilot physiology Oxygen equipment per FAA Wave
ANNEX D: PHYSIOLOGICAL EPISODES
 1. The Navy s definition of a physiological episode (PE) is when a pilot experiences loss in performance related to insufficient oxygen, depressurization, or other factors during flight. For the purposes
1. The Navy s definition of a physiological episode (PE) is when a pilot experiences loss in performance related to insufficient oxygen, depressurization, or other factors during flight. For the purposes
Oxygen Therapy. Respiratory Rehabilitation Program. What is oxygen?
 Respiratory Rehabilitation Program What is oxygen? Oxygen Therapy Oxygen is a colourless, tasteless, odorless gas that you need to live. Oxygen is found in the air you breathe at a concentration of 21%.
Respiratory Rehabilitation Program What is oxygen? Oxygen Therapy Oxygen is a colourless, tasteless, odorless gas that you need to live. Oxygen is found in the air you breathe at a concentration of 21%.
PVDOMICS: Cardiopulmonary Exercise Testing (CPET) Training
 PVDOMICS: Cardiopulmonary Exercise Testing (CPET) Training Cardiovascular Physiology Core Cleveland Clinic, Cleveland OH March 16, 2018 NHLBI Pulmonary Vascular Disease Phenomics Program Funded by the
PVDOMICS: Cardiopulmonary Exercise Testing (CPET) Training Cardiovascular Physiology Core Cleveland Clinic, Cleveland OH March 16, 2018 NHLBI Pulmonary Vascular Disease Phenomics Program Funded by the
Respiratory Physiology. Adeyomoye O.I
 Respiratory Physiology By Adeyomoye O.I Outline Introduction Hypoxia Dyspnea Control of breathing Ventilation/perfusion ratios Respiratory/barometric changes in exercise Intra-pulmonary & intra-pleural
Respiratory Physiology By Adeyomoye O.I Outline Introduction Hypoxia Dyspnea Control of breathing Ventilation/perfusion ratios Respiratory/barometric changes in exercise Intra-pulmonary & intra-pleural
Understanding Tracheostomy Care for your Child
 Understanding Tracheostomy Care for your Child 2 Inside this guide: This guide will help you learn how to take care of your child s tracheostomy (trach). It is important to ask questions. You will be given
Understanding Tracheostomy Care for your Child 2 Inside this guide: This guide will help you learn how to take care of your child s tracheostomy (trach). It is important to ask questions. You will be given
4/13/14. U.S.Sailing Association Safety at Sea Medical Issues
 U.S.Sailing Association Safety at Sea Medical Issues 1 Lieutenant, Operations Division, Emergency Preparedness Disaster Services Oak Park Fire Department fyrebugg@wowway.com 847-648-1148 Author of slides
U.S.Sailing Association Safety at Sea Medical Issues 1 Lieutenant, Operations Division, Emergency Preparedness Disaster Services Oak Park Fire Department fyrebugg@wowway.com 847-648-1148 Author of slides
Working in low oxygen-controlled atmospheres. Risks and Prevention Measures Dr Michel Falcy, INRS FRANCE
 Working in low oxygen-controlled atmospheres Risks and Prevention Measures Dr Michel Falcy, INRS FRANCE Use of low O 2 -controlled atmospheres Nitrogenrefrigerated lorries Cryogenic facilities (sperm banks)
Working in low oxygen-controlled atmospheres Risks and Prevention Measures Dr Michel Falcy, INRS FRANCE Use of low O 2 -controlled atmospheres Nitrogenrefrigerated lorries Cryogenic facilities (sperm banks)
Heat Stress Prevention Written Program Laredo ISD Safety/Risk/Emergency Management Department
 Heat Stress Prevention Written Program Laredo ISD Safety/Risk/Emergency Management Department HEAT STRESSS PROGRAM 2016 LJP/ 1 1.0 Purpose This Heat Stress Prevention Program has been developed to provide
Heat Stress Prevention Written Program Laredo ISD Safety/Risk/Emergency Management Department HEAT STRESSS PROGRAM 2016 LJP/ 1 1.0 Purpose This Heat Stress Prevention Program has been developed to provide
CABIN DEPRESSURIZATION AND SLOW ONSET HYPOXIA CRM, SIMULATOR AND SCENARIO BASED PHYSIOLOGY
 CABIN DEPRESSURIZATION AND SLOW ONSET HYPOXIA CRM, SIMULATOR AND SCENARIO BASED PHYSIOLOGY LESSONS LEARNED FROM 2500 PILOTS TRAINED IN SLOW ONSET HYPOXIA SOUTHERN AEROMEDICAL INSTITUTE DR. PAUL BUZA MEDICAL
CABIN DEPRESSURIZATION AND SLOW ONSET HYPOXIA CRM, SIMULATOR AND SCENARIO BASED PHYSIOLOGY LESSONS LEARNED FROM 2500 PILOTS TRAINED IN SLOW ONSET HYPOXIA SOUTHERN AEROMEDICAL INSTITUTE DR. PAUL BUZA MEDICAL
https://youtu.be/5r7havfzxek
 CPR https://youtu.be/5r7havfzxek CPR Saves Lives Cardiopulmonary Resuscitation or CPR and defibrillation within 3-5 minutes can save over 50% of cardiac arrest victims CPR followed by AED saves thousands
CPR https://youtu.be/5r7havfzxek CPR Saves Lives Cardiopulmonary Resuscitation or CPR and defibrillation within 3-5 minutes can save over 50% of cardiac arrest victims CPR followed by AED saves thousands
Smoke inhalation 2/1/2013. Disclosures. Smoke Inhalation. Case Study
 Disclosures Smoke inhalation Craig Smollin MD Associate Medical Director, California Poison Control Center, SF Assistant Professor of Emergency Medicine University of California, San Francisco No financial
Disclosures Smoke inhalation Craig Smollin MD Associate Medical Director, California Poison Control Center, SF Assistant Professor of Emergency Medicine University of California, San Francisco No financial
RECONSTITUTION AND ADMINISTRATION INSTRUCTIONS FOR HEALTHCARE PROFESSIONALS. Hereditary Angioedema
 RECONSTITUTION AND ADMINISTRATION INSTRUCTIONS FOR HEALTHCARE PROFESSIONALS Hereditary Angioedema TRUST PROVEN PREVENTION WITH CINRYZE Whether your patients are new to treatment or are continuing their
RECONSTITUTION AND ADMINISTRATION INSTRUCTIONS FOR HEALTHCARE PROFESSIONALS Hereditary Angioedema TRUST PROVEN PREVENTION WITH CINRYZE Whether your patients are new to treatment or are continuing their
Wildland Fire School. Heat Illness Prevention Program
 Monterey County Fire Training Officers Association www.mcftoa.org Heat Illness Prevention Program I. Purpose: The purpose of this program is to provide a safe training environment for attendees and participants
Monterey County Fire Training Officers Association www.mcftoa.org Heat Illness Prevention Program I. Purpose: The purpose of this program is to provide a safe training environment for attendees and participants
City of Miami s Public Access Defibrillation Program
 City of Miami s View on line at: www.miamigov.com/fire/pad E-Mail: PADcoordinator@MiamiGov.com Team For Life 53 PAD - Public Access Defibrillator Program Table of Contents Page Index 54 Program Overview
City of Miami s View on line at: www.miamigov.com/fire/pad E-Mail: PADcoordinator@MiamiGov.com Team For Life 53 PAD - Public Access Defibrillator Program Table of Contents Page Index 54 Program Overview
HEAT ILLNESS PREVENTION PLAN
 www.westhillscollege.com HEAT ILLNESS PREVENTION PLAN October, 2008 Status: Last Revised July, 2008 Approved WHCCD Risk Management Committee 10/10/08 WHCCD Board of Trustees approval 12/16/08 HEAT ILLNESS
www.westhillscollege.com HEAT ILLNESS PREVENTION PLAN October, 2008 Status: Last Revised July, 2008 Approved WHCCD Risk Management Committee 10/10/08 WHCCD Board of Trustees approval 12/16/08 HEAT ILLNESS
PREPARATION AND SELF-ADMINISTRATION INSTRUCTIONS FOR PATIENTS
 PREPARATION AND SELF-ADMINISTRATION INSTRUCTIONS FOR PATIENTS Hereditary Angioedema TAKE CONTROL OF HEREDITARY ANGIOEDEMA (HAE) TREATMENT WITH FLEXIBLE ADMINISTRATION Choosing to treat with CINRYZE (C1
PREPARATION AND SELF-ADMINISTRATION INSTRUCTIONS FOR PATIENTS Hereditary Angioedema TAKE CONTROL OF HEREDITARY ANGIOEDEMA (HAE) TREATMENT WITH FLEXIBLE ADMINISTRATION Choosing to treat with CINRYZE (C1
Learning Objectives 9/12/2012. Chapter 30. Environmental Emergencies. Chapter Goal
 Chapter 30 Environmental Emergencies Chapter Goal Use assessment findings to formulate field impression & implement treatment plan for patients with environmentally induced or exacerbated emergencies Define
Chapter 30 Environmental Emergencies Chapter Goal Use assessment findings to formulate field impression & implement treatment plan for patients with environmentally induced or exacerbated emergencies Define
Collin County Community College. Lung Physiology
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 9 Respiratory System 1 Lung Physiology Factors affecting Ventillation 1. Airway resistance Flow = Δ P / R Most resistance is encountered
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 9 Respiratory System 1 Lung Physiology Factors affecting Ventillation 1. Airway resistance Flow = Δ P / R Most resistance is encountered
UNDERSTANDING THE PRINCIPLES OF
 AVIATION MEDICINE IN ACTION: UNDERSTANDING THE PRINCIPLES OF AVIATION MEDICINE IN FLYING OPERATIONS MAJ(DR) Dominic TAN Air Force Medical Service Republic of Singapore Air Force 2 WHAT IS AVIATION MEDICINE
AVIATION MEDICINE IN ACTION: UNDERSTANDING THE PRINCIPLES OF AVIATION MEDICINE IN FLYING OPERATIONS MAJ(DR) Dominic TAN Air Force Medical Service Republic of Singapore Air Force 2 WHAT IS AVIATION MEDICINE
PPL 10 CPR & AED TRAINING & CERTIFICATION
 PPL 10 CPR & AED TRAINING & CERTIFICATION Knowing CPR means knowing how to save lives. The ACT Foundation is working to set up the lifesaving CPR program in every Canadian high school, so that all youth
PPL 10 CPR & AED TRAINING & CERTIFICATION Knowing CPR means knowing how to save lives. The ACT Foundation is working to set up the lifesaving CPR program in every Canadian high school, so that all youth
Aerospace Physiology MARYLAND. Cardiopulmonary Physiology. Musculoskeletal Vestibular Neurological. Respiratory Cardiovascular U N I V E R S I T Y O F
 Cardiopulmonary Physiology Respiratory Cardiovascular Musculoskeletal Vestibular Neurological 2003 David L. Akin - All rights reserved http://spacecraft.ssl.umd.edu The Human Circulatory System Lung Measurements
Cardiopulmonary Physiology Respiratory Cardiovascular Musculoskeletal Vestibular Neurological 2003 David L. Akin - All rights reserved http://spacecraft.ssl.umd.edu The Human Circulatory System Lung Measurements
Tactical Combat Casualty Care Guidelines for All Combatants
 Tactical Combat Casualty Care Guidelines for All Combatants August 2017 (Based on TCCC Guidelines for Medical Personnel 170131) These recommendations are intended to be guidelines only and are not a substitute
Tactical Combat Casualty Care Guidelines for All Combatants August 2017 (Based on TCCC Guidelines for Medical Personnel 170131) These recommendations are intended to be guidelines only and are not a substitute
