First Response & Advanced Resuscitation Learning Modules 2 and 3 Based on ILCOR and ANZCOR 2016
|
|
|
- Betty Hoover
- 5 years ago
- Views:
Transcription
1 First Response & Advanced Resuscitation Learning Modules 2 and 3 Based on ILCOR and ANZCOR 2016
2 Learning objectives Following completion of the theoretical & practical components of this module, the participant will be able to demonstrate their ability to: Assess a newborn infant s transition to extra-uterine life & determine the need for resuscitation. Initiate First Response interventions including face mask ventilation and external chest compressions. Initiate Advanced Resuscitation interventions including intubation, insertion of a laryngeal mask airway, establishing umbilical venous access and administration of adrenaline and volume expanders.
3 ARC & NZRC Newborn Life Support Flow Chart
4 Transition to extra-uterine life Very few newborns require resuscitation Most will respond to simple interventions First Response interventions are therefore most important & time critical Resuscitation at birth in Australia in 2015 Suction or oxygen therapy 7.8% Positive pressure ventilation through mask 7% Intubation & positive pressure ventilation 0.6% Cardiac compressions & positive pressure ventilation 0.3% No intervention (other than drying and stimulation) 81% Australian Institute of Health and Welfare
5 Preparation for resuscitation Anticipation of need Based on risk assessment Equipment Checked and ready for use Environment Warm and clean Skilled personnel Able to form a team, nominate leadership and develop a plan of action
6 Cord clamping & cord milking ILCOR and the ANZCOR suggest: Delayed cord clamping for seconds if: Uncomplicated term or preterm birth, and Not requiring immediate resuscitation For compromised newborns: Insufficient evidence for optimal timing of cord clamping in term and preterm depressed newborns Insufficient evidence of benefit of cord milking, especially if <28 weeks. Not recommended.
7 Monitoring Pulse oximetry is recommended: When the need for resuscitation is anticipated When CPAP or positive pressure is used When persistent cyanosis is suspected When supplemental oxygen is used Place the oximeter sensor on the right wrist or hand (pre-ductal oxygen saturation) ECG monitoring: May be used as an adjunct to auscultation and pulse oximetry (if readily available)
8 Pre-ductal pulse oximetry (SpO 2 ) Place oximeter sensor on the right hand or wrist Measure of arterial oxygen saturation in vessels originating from the aorta before mixing with pulmonary blood at the level of the ductus arteriosus
9 Strategies to maintain normal core temperature: C Very preterm newborns (<32 weeks): Place (wet & warm) into a polyethylene bag or under a polyethylene sheet Radiant warmer Additional measures (alone or in combination): Covering the head (except the face) with a hat/bedding Ambient room temperature o C Exothermic warming mattress
10 A: Assess and Airway At all stages ask: Do you need help? 1 minute Assessment Term gestation? Breathing or crying? Good tone? NO Actions Maintain normal temperature Ensure open airway Stimulate Assessment HR below 100/min? Gasping or apnoea? YES Stay with mother NO Actions Positive pressure ventilation Oxygen saturation (SpO 2 ) monitoring Routine care: Prevent heat loss Ongoing evaluation NO Assessment Laboured breathing or persistent cyanosis?
11 If meconium liquor is present Clear the oro-pharynx if obvious meconium If the newborn is vigorous: Endotracheal suctioning is discouraged because it does not alter outcome and may cause harm If the newborn is not vigorous: No evidence of the value of routine or repeated endotracheal suctioning to prevent meconium aspiration Likely to cause further delays in resuscitation Tracheal intubation for suctioning should only be performed for suspected tracheal obstruction.
12 B: Breathing At all stages ask: Do you need help? Assessment * Heart rate below100/min? Gasping or apnoeic? YES Actions * Positive pressure ventilation SpO 2 monitoring Assessment Heart rate below 100/min? NO NO YES Actions Ensure open airway Reduce face mask leaks Consider increasing pressure &/or oxygen Assessment Laboured breathing or Persistent cyanosis YES Actions Ensure open airway SpO 2 monitoring Consider CPAP Post resuscitation care * Endotracheal intubation may be considered at several stages NO
13 Manual ventilation devices A T-piece device, a self inflating bag and a flow inflating bag are all acceptable devices to ventilate newborn infants either via a face mask, laryngeal mask or endotracheal tube. (ANZCOR, 2016)
14 PEEP during resuscitation Without PEEP: Lung aeration is not achieved as quickly Functional residual capacity (FRC) is not established With PEEP: FRC is established and maintained Oxygenation is improved ANZCOR (2016) recommend: PEEP of 5-8 cm H 2 O during resuscitation of newborn infants if appropriate equipment available
15 Initial settings: T-piece device Gas flow Set at 10 L/min (8 L/min if using cylinders) Maximum pressure relief valve Set at 50 cm H 2 O Peak inspiratory pressure (PIP) Set at 30 cm H 2 O (term newborn) Set at cm H 2 O (preterm <32 weeks) Positive end expiratory pressure (PEEP) Set at 5-8 cm H 2 O
16 Summary of settings by gestation Initial Term <35 weeks <32 weeks settings PIP cmh 2 O PEEP cmh 2 O Air/oxygen 21% 21-30% 21-30% Avoid high O 2 initially (65%-100%) Use room air if air/oxygen blend not available
17 Oxygen use in resuscitation All newborns Oxygen should be used judiciously, guided by SpO 2 Introduce supplemental oxygen if lower end of target saturations are not met, despite respiratory support Avoid hyperoxaemia Avoid hypoxaemia If external chest compressions are required: Increase oxygen concentration to 100% Oxygen concentration should be weaned as soon as the heart rate has recovered and target saturations are being met.
18 Target saturations for newborn infants during resuscitation Time after birth in minutes Targeted pre-ductal oxygen saturations for newborn infants during resuscitation 1 minute 60 70% 2 minutes 65 85% 3 minutes 70 90% 4 minutes 75 90% 5 minutes 80 90% 10 minutes 85 90% ANZCOR 2, 2016, Guideline 13.4
19 Centile charts with targeted preductal SpO 2 in the first 10 mins Time after birth in minutes Targeted pre-ductal oxygen saturation (SpO 2 ) for newborns during resuscitation 1 minute 60 70% 2 minutes 65 85% 3 minutes 70 90% 4 minutes 75 90% 5 minutes 80 90% 10 minutes 85 90% Adapted from Dawson et al., 2010 and ANZCOR, 2016
20 N.B The relationship between PaO 2 and SpO 2 is not linear In air FiO 2 > 0.21 SpO 2 95% = P? PaO 2 Adapted from: Sola, Chow & Rogido, 2005, An Pediatr 62(3):
21 Positive pressure ventilation Optimal positive pressure ventilation requires: 1. An appropriate sized face mask 2. A good seal between the mask and the face to minimise leak The two-point top hold is one method shown to reduce mask leak when using the Laerdal round mask 4
22 Ventilation rate and pressure Rate: inflations per minute Peak inflating pressure (PIP): Variable and should be individualised Effective ventilation may be achieved with progressively lower pressures and rates Avoid hyperventilation (excessive PIP &/or rate) Can lead to dangerously low CO 2 levels (<30 mmhg) Can depress respiratory drive Can reduce cerebral blood flow
23 Assessing the effectiveness of positive pressure ventilation Re-assess the heart rate every 30 seconds The effectiveness of ventilation is confirmed by: 1. An increase in the heart rate above 100/min. 2. A slight rise and fall of the chest and upper abdomen with each inflation. 3. An improvement in oxygenation (assessed by pulse oximetry).
24 If the heart rate is not improving with positive pressure ventilation Check the ventilation technique Is there a face mask leak? Is the airway patent? Increase the peak inflating pressure Increase the PIP in 5 cmh 2 O increments: cm H 2 O if necessary Increase oxygen according to SpO 2 targets Increase to 100% if the heart rate is <60/min
25 C:Circulation At all stages ask: Do you need help? Assessment Heart rate below 60/min? YES Actions * Three chest compressions to each breath 100% oxygen + Intubation or laryngeal mask Venous access YES Assessment Heart rate below 60/min? YES * Endotracheal intubation should be considered + Ensure the O 2 has been increased to 100% if the heart rate is <60/min
26 Techniques for ECC in newborns Hand encircling, two thumb (recommended technique) Two finger technique (only if single operator)
27 Consider endotracheal intubation at any time, if expertise is available Estimated endotracheal size internal diameter can also be calculated as gestation age in weeks divided by 10 Estimated depth of insertion Rule of 6 Birth weight in kg + 6cm Endotracheal size & depth of insertion (oral tube) Corrected gestation (Weeks) ETT size (Guide: GA 10) Actual weight (kg) ETT mark at the lip (cm) mm mm mm
28 Confirming tracheal intubation An exhaled CO 2 detector is a reliable method to confirm endotracheal tube placement in neonates who have spontaneous circulation False positive/negative results may occur if: Insufficient inflations (tidal volume) delivered There is very low or absent pulmonary blood flow Contaminated with adrenaline or surfactant Do not re-intubate unnecessarily.
29 Verify ETT position with an exhaled CO 2 detector (e.g. Pedi-Cap ) Give 6 positive pressure inflations, then interpret INSPIRATION EXPIRATION GOLD IS GOOD
30 Laryngeal mask airway (LMA) Consider if: Face mask ventilation is unsuccessful Tracheal intubation is unsuccessful or not feasible Term or near term infant Size 1 LMA suitable for infants 34 weeks, >2000g
31 D:Drugs At all stages ask: Do you need help? Assessment + Heart rate below 60/min? YES Actions * IV Adrenaline: 1:10,000 Dose: ml/kg Consider volume expansion * Endotracheal intubation should be performed + Ensure the O 2 has been increased to 100% if the heart rate is <60/min Remember to document all interventions & the newborn s response
32 Adrenaline Route Umbilical vein Peripheral IV Intraosseous Endotracheal tube (ETT) Adrenaline 1:10,000 solution Dose ml/kg (10-30 mcg/kg) ml/kg ( mcg/kg) Use 1:10,000 Intravenous route recommended - will require venous access (insertion of an umbilical venous catheter, peripheral intravenous cannula or intraosseous needle)
33 Medications: Adrenaline Adrenaline should be given intravenously Dose can be repeated every few minutes if the heart rate remains <60/min despite effective IPPV & ECC Intraosseous adrenaline Should be considered if delay/difficulty in obtaining IV/UV access Endotracheal adrenaline May be considered if delay in obtaining IV/IO access If endotracheal route is used, up to ten times the IV/IO dose can be given
34 Medications: Volume expanders Intravascular fluids should be considered: If fetal blood loss is suspected and/or The newborn appears to be in shock (pale, poor perfusion, weak pulses) The newborn has not responded to other resuscitation measures (especially if the HR is not improving) Normal saline should be used initially, but: O-negative red blood cell replacement is the priority in the setting of massive blood loss or suspected blood loss. Dose: 10 ml/kg, IV over several minutes. May need to be repeated.
35 For more information on: Intubation Use of an exhaled CO 2 detector Use of a laryngeal mask airway (LMA) Intravenous, umbilical and intraosseous access Medications Discontinuation &/or withdrawal of resuscitation Resuscitation in special circumstances Post resuscitation care and stabilisation See the Learning Resources section of the NeoResus web site at
36 Australian & New Zealand Committee on Resuscitation (ANZCOR) Section Neonatal Guidelines Published January 2016 Available for download at
37 Key references 1. Australian Institute of Health and Welfare Australia s mothers and babies in brief. Perinatal statistics series no.33. Cat no. PER 91. Canberra: AIHW. 2. Australian & New Zealand Resuscitation Councils. (2016). Section 13: Neonatal Guidelines. Accessed 24 February 2018 from: 3. Perlman JM, Kattwinkel J, Wyckoff et al. Part 7: Neonatal Resuscitation 2015 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations. Circulation, 2015; 132 (Supp 1): S204-S Wood, FE, Morley, CJ, Dawson JA et al. (2008). Improved techniques reduce face mask leak during simulated neonatal resuscitation: Study 2. Arch Disease Child, Fetal Neonatal Ed; 93:F
38 Disclaimer This teaching program has been developed by the Paediatric Infant Perinatal Emergency Retrieval Service (PIPER) Victoria as an educational program around neonatal care. Whilst appreciable care has been taken in the preparation of this material, PIPER shall not be held responsible for any act or omission which may result in injury or death to any baby as a result of reliance on this material.
39 Copyright This presentation was developed by Dr Rosemarie Boland and Dr Marta Thio on behalf of the Victorian Newborn Resuscitation Project (2018). The material is copyright NeoResus. This presentation may be downloaded for personal use but remains the intellectual property of NeoResus and as such, may not be reproduced or used for another training program without the written permission of the Victorian Newborn Resuscitation Project Executive. Please contact us at
Learning objectives. First Response Learning Module 2 Based on ILCOR and ANZCOR 2016
 First Response Learning Module 2 Based on ILCOR and ANZCOR 2016 Learning objectives Following completion of the theoretical & practical components of this module, the participant will be able to demonstrate
First Response Learning Module 2 Based on ILCOR and ANZCOR 2016 Learning objectives Following completion of the theoretical & practical components of this module, the participant will be able to demonstrate
First Response Learning Module 2 Based on ILCOR and ANZCOR Victorian Newborn Resuscitation Project Updated March 2018
 First Response Learning Module 2 Based on ILCOR and ANZCOR 2016 Learning objectives Following completion of the theoretical & practical components of this module, the participant will be able to demonstrate
First Response Learning Module 2 Based on ILCOR and ANZCOR 2016 Learning objectives Following completion of the theoretical & practical components of this module, the participant will be able to demonstrate
Operating & troubleshooting a self inflating bag. Victorian Newborn Resuscitation Project Updated February 2012
 Operating & troubleshooting a self inflating bag Six key steps to success Step 1 Choose the correct size self inflating bag for newborn resuscitation: a 240 ml bag Step 2 Choose the correct sized mask
Operating & troubleshooting a self inflating bag Six key steps to success Step 1 Choose the correct size self inflating bag for newborn resuscitation: a 240 ml bag Step 2 Choose the correct sized mask
RESUSCITATION. If baby very floppy and heart rate slow, assist breathing immediately. If baby not breathing adequately by 90 sec, assist breathing
 RESUSCITATION Check equipment daily, and before resuscitation Follow Resuscitation Council UK Guidelines www.resus.org.uk DRY AND COVER Cord clamping see Cord clamping below >28 weeks gestation, dry baby,
RESUSCITATION Check equipment daily, and before resuscitation Follow Resuscitation Council UK Guidelines www.resus.org.uk DRY AND COVER Cord clamping see Cord clamping below >28 weeks gestation, dry baby,
Objectives. Fetal Physiology. Fetal Physiology. Resuscitation and Stabilization of the Newborn. Which Babies Require Resuscitation?
 Objectives Resuscitation and Stabilization of the Newborn June 7, 2018 Angela N. Burton, NNP-BC Henry Ford Health System Review the physiology of fetal / neonatal circulation and first breaths. Review
Objectives Resuscitation and Stabilization of the Newborn June 7, 2018 Angela N. Burton, NNP-BC Henry Ford Health System Review the physiology of fetal / neonatal circulation and first breaths. Review
birth: a transition better guidelines better outcomes the birth experience a challenging transition the fountains of life: 2/8/2018
 better guidelines better outcomes neonatal resuscitation Anne G. Wlodaver, MD neonatology OU medical center the birth experience a challenging transition birth requires major and sudden transitions some
better guidelines better outcomes neonatal resuscitation Anne G. Wlodaver, MD neonatology OU medical center the birth experience a challenging transition birth requires major and sudden transitions some
NOTE: If not used, provider must document reason(s) for deferring mechanical ventilation in a patient with an advanced airway
 APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
Neonatal tidal volume targeted ventilation
 Neonatal tidal volume targeted ventilation Colin Morley Retired Professor of Neonatal Medicine, Royal Women s Hospital, Melbourne, Australia. Honorary Visiting Fellow, Dept Obstetrics and Gynaecology,
Neonatal tidal volume targeted ventilation Colin Morley Retired Professor of Neonatal Medicine, Royal Women s Hospital, Melbourne, Australia. Honorary Visiting Fellow, Dept Obstetrics and Gynaecology,
Code Blue III Simulators. ALS and Emergency Care Simulators
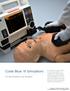 Code Blue III Simulators ALS and Emergency Care Simulators Our Code Blue III system teaches ALS skills using realistic code scenarios. Each step you take is monitored by software providing important feedback,
Code Blue III Simulators ALS and Emergency Care Simulators Our Code Blue III system teaches ALS skills using realistic code scenarios. Each step you take is monitored by software providing important feedback,
Mechanical Ventilation
 Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
Other Oxygen Delivery Systems
 53 Oxygen is the most commonly used drug in the NICU. Excessive use of oxygen is linked to BPD and RDP. At the same time, hypoxemia is equally harmful and is associated with increased risk of mortality.
53 Oxygen is the most commonly used drug in the NICU. Excessive use of oxygen is linked to BPD and RDP. At the same time, hypoxemia is equally harmful and is associated with increased risk of mortality.
Capnography in the Veterinary Technician Toolbox. Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA
 Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
Using the Lifebox oximeter in the neonatal unit. Tutorial 1 the basics
 Using the Lifebox oximeter in the neonatal unit Tutorial 1 the basics Lifebox 2014. 2011. All rights reserved The Lifebox Pulse Oximeter In this tutorial you will learn about: The function of a pulse oximeter
Using the Lifebox oximeter in the neonatal unit Tutorial 1 the basics Lifebox 2014. 2011. All rights reserved The Lifebox Pulse Oximeter In this tutorial you will learn about: The function of a pulse oximeter
Breathing during mask ventilation of preterm infants at birth
 6 Breathing during mask ventilation of preterm infants at birth Corinne J.M. van der Pot Kim Schilleman Stuart B. Hooper Colin J. Morley Frans J. Walther Arjan B. te Pas Submitted Chapter 6 Abstract Objective
6 Breathing during mask ventilation of preterm infants at birth Corinne J.M. van der Pot Kim Schilleman Stuart B. Hooper Colin J. Morley Frans J. Walther Arjan B. te Pas Submitted Chapter 6 Abstract Objective
Basic Life Support Adult
 1/3.4.1 Version 4, 03/2016 Basic Life Support Adult CFR - A EFR Collapse Initiate mobilisation of 3 to 4 practitioners / responders Unresponsive and breathing abnormally or gasping 112 / 999 Go to Primary
1/3.4.1 Version 4, 03/2016 Basic Life Support Adult CFR - A EFR Collapse Initiate mobilisation of 3 to 4 practitioners / responders Unresponsive and breathing abnormally or gasping 112 / 999 Go to Primary
Clinical Skills. Administering Oxygen
 Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
Nottingham Neonatal Service - Clinical Guidelines
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Author: Contact Name and Job Title Directorate & Speciality Date of submission 8 th Feb 2018 Explicit definition
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Author: Contact Name and Job Title Directorate & Speciality Date of submission 8 th Feb 2018 Explicit definition
PRACTICE GUIDELINE EM004 EMERGENCY CENTRE EQUIPMENT
 PRACTICE GUIDELINE EM004 EMERGENCY CENTRE EQUIPMENT This Practice Guideline sets out the minimum recommended equipment for an Emergency Centre. It should be read in conjunction with Practice Guideline
PRACTICE GUIDELINE EM004 EMERGENCY CENTRE EQUIPMENT This Practice Guideline sets out the minimum recommended equipment for an Emergency Centre. It should be read in conjunction with Practice Guideline
Inspire rpap REVOLUTION FROM THE FIRST BREATH
 Inspire rpap TM REVOLUTION FROM THE FIRST BREATH The Inspire rpap The Inspire rpap is a revolutionary, non-invasive system for the initial stabilisation and resuscitation of infants. TM Its innovative,
Inspire rpap TM REVOLUTION FROM THE FIRST BREATH The Inspire rpap The Inspire rpap is a revolutionary, non-invasive system for the initial stabilisation and resuscitation of infants. TM Its innovative,
Greater Manchester, High Peak and East Cheshire Neonatal Transport Service
 Date / PetCO 2 (kpa) Interventions Greater Manchester, High Peak and East Cheshire Neonatal Transport Service - 19 - END TIDAL CARBON DIOXIDE Transport No:... FIRST 10 END CARBON DIOXIDE MEASUREMENTS (taken
Date / PetCO 2 (kpa) Interventions Greater Manchester, High Peak and East Cheshire Neonatal Transport Service - 19 - END TIDAL CARBON DIOXIDE Transport No:... FIRST 10 END CARBON DIOXIDE MEASUREMENTS (taken
Unit 15 Manual Resuscitators
 15-1 Unit 15 Manual Resuscitators GOAL On completion of this unit, the student should comprehend the proper operation of self-inflating resuscitation bags, flow-inflating resuscitation bags and gas-powered
15-1 Unit 15 Manual Resuscitators GOAL On completion of this unit, the student should comprehend the proper operation of self-inflating resuscitation bags, flow-inflating resuscitation bags and gas-powered
VENTILATION STRATEGIES FOR THE CRITICALLY UNWELL
 VENTILATION STRATEGIES FOR THE CRITICALLY UNWELL Dr Nick Taylor Visiting Emergency Specialist Teaching Hospital Karapitiya Senior Specialist and Director ED Training Clinical Lecturer, Australian National
VENTILATION STRATEGIES FOR THE CRITICALLY UNWELL Dr Nick Taylor Visiting Emergency Specialist Teaching Hospital Karapitiya Senior Specialist and Director ED Training Clinical Lecturer, Australian National
AUTOVENT 4000 VENTILATOR
 OVERVIEW AUTOVENT 4000 Only properly trained and approved Escambia County Bureau of Public Safety Paramedics are to use the AutoVent 4000 ventilator manufactured by LSP to transport patients already on
OVERVIEW AUTOVENT 4000 Only properly trained and approved Escambia County Bureau of Public Safety Paramedics are to use the AutoVent 4000 ventilator manufactured by LSP to transport patients already on
2015 Guidelines Summary HeartSine samaritan PAD Automated External Defibrillators
 2015 Guidelines Summary HeartSine samaritan PAD Automated External Defibrillators This document provides a summary of the 2015 guidelines and how the HeartSine samaritan PAD range of products complies
2015 Guidelines Summary HeartSine samaritan PAD Automated External Defibrillators This document provides a summary of the 2015 guidelines and how the HeartSine samaritan PAD range of products complies
MINI- COURSE on Management of OXYGEN in babies with RESPIRATORY DISTRESS
 MINI- COURSE on Management of OXYGEN in babies with RESPIRATORY DISTRESS Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have 5 questions to allow you to
MINI- COURSE on Management of OXYGEN in babies with RESPIRATORY DISTRESS Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have 5 questions to allow you to
Cardiac Arrest General
 Date: November 15, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not
Date: November 15, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not
QUICK REFERENCE GUIDE
 cm H O 2 cm H O 2 cm HO 2 PSI cm H O 2 ON OFF UPPER LIMIT LOWER LIMIT UPPER LIMIT LOWER LIMIT LIFE PULSE HIGH-FREQUENCY VENTILATOR QUICK REFERENCE GUIDE 01388-08.11 MONITOR PIP JET VALVE ALARMS READY SILENCE
cm H O 2 cm H O 2 cm HO 2 PSI cm H O 2 ON OFF UPPER LIMIT LOWER LIMIT UPPER LIMIT LOWER LIMIT LIFE PULSE HIGH-FREQUENCY VENTILATOR QUICK REFERENCE GUIDE 01388-08.11 MONITOR PIP JET VALVE ALARMS READY SILENCE
BLS. Compressions Airway Breaths. Basic Life Support Quick Reference. Critical Concepts
 BLS Basic Life Support Quick Reference C-A-B Compressions Airway Breaths Critical Concepts High-quality CPR improves a victim s chances of survival. The critical characteristics of high-quality CPR include
BLS Basic Life Support Quick Reference C-A-B Compressions Airway Breaths Critical Concepts High-quality CPR improves a victim s chances of survival. The critical characteristics of high-quality CPR include
RCH Simulation Program Skill Stations Initial Responders 1 st 3 mins of resuscitation
 RCH Simulation Program Skill Stations Initial Responders 1 st 3 mins of resuscitation LEARNING OBJECTIVES: By the end of this module, candidates should be able to : (1) Demonstrate resuscitation of an
RCH Simulation Program Skill Stations Initial Responders 1 st 3 mins of resuscitation LEARNING OBJECTIVES: By the end of this module, candidates should be able to : (1) Demonstrate resuscitation of an
RESPIRATORY CARE POLICY AND PROCEDURE MANUAL. a) Persistent hypoxemia despite improved ventilatory pattern and elevated Fl02
 The University of Mississippi AND PROCEDURE MANUAL Effective Date: June 30, 1990 Revised Date: December 2009 MANUAL CODE Page 1 of 5 PREPARED BY: Respiratory Care Policy and Procedure Review Committee
The University of Mississippi AND PROCEDURE MANUAL Effective Date: June 30, 1990 Revised Date: December 2009 MANUAL CODE Page 1 of 5 PREPARED BY: Respiratory Care Policy and Procedure Review Committee
Virginia Beach EMS. Oxylator EMX. Debra H. Brennaman, RN, MPA, NREMT-P
 Virginia Beach EMS Oxylator EMX Debra H. Brennaman, RN, MPA, NREMT-P Oxylator EMX Overview Patient responsive oxygen powered resuscitation / ventilation device intended to provide emergency ventilatory
Virginia Beach EMS Oxylator EMX Debra H. Brennaman, RN, MPA, NREMT-P Oxylator EMX Overview Patient responsive oxygen powered resuscitation / ventilation device intended to provide emergency ventilatory
ANZCOR Guideline 6 Compressions
 ANZCOR Guideline 6 Compressions Who does this guideline apply to? Summary This guideline applies to all persons who are unresponsive and not breathing normally. Who is the audience for this guideline?
ANZCOR Guideline 6 Compressions Who does this guideline apply to? Summary This guideline applies to all persons who are unresponsive and not breathing normally. Who is the audience for this guideline?
The aim of this guideline is to describe the indications and procedure for using high flow nasal prong oxygen
 High flow nasal prong HFNP oxygen therapy o Introduction & aim o Indications o Contraindications o Management equipment setup patient management o Weaning o Complications Introduction Humidified high flow
High flow nasal prong HFNP oxygen therapy o Introduction & aim o Indications o Contraindications o Management equipment setup patient management o Weaning o Complications Introduction Humidified high flow
Changing gas flow during neonatal resuscitation: a manikin study
 8 Changing gas flow during neonatal resuscitation: a manikin study Kim Schilleman Georg M. Schmölzer C. Omar F. Kamlin Colin J. Morley Arjan B. te Pas Peter G. Davis Resuscitation. 2011 Jul;82(7):920-924
8 Changing gas flow during neonatal resuscitation: a manikin study Kim Schilleman Georg M. Schmölzer C. Omar F. Kamlin Colin J. Morley Arjan B. te Pas Peter G. Davis Resuscitation. 2011 Jul;82(7):920-924
VENTILATORS PURPOSE OBJECTIVES
 VENTILATORS PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain a ventilator in the interfacility transfer environment. COGNITIVE OBJECTIVES
VENTILATORS PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain a ventilator in the interfacility transfer environment. COGNITIVE OBJECTIVES
Endotracheal Suctioning: In Line ETT
 Approved by: Endotracheal Suctioning: In Line ETT Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures
Approved by: Endotracheal Suctioning: In Line ETT Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures
HIGH FREQUENCY JET VENTILATION (HFJV): EQUIPMENT PREPRATION
 POLICY The physician orders High Frequency Jet Ventilation (HFJV). The Respiratory Therapist in discussion with the physician will determine blood gas targets and ventilation settings for the treatment
POLICY The physician orders High Frequency Jet Ventilation (HFJV). The Respiratory Therapist in discussion with the physician will determine blood gas targets and ventilation settings for the treatment
A V A L A N C H E R E S C U E
 AVALANCHE RESCUE The On-Site Triage And Evacuation Of Avalanche Victims Statistics De Quervain s Mortality Curve 1945 to 1979 and 1979 to 1989 2,611 cases, buried at average 1.06 m After 1 hour 30-40%
AVALANCHE RESCUE The On-Site Triage And Evacuation Of Avalanche Victims Statistics De Quervain s Mortality Curve 1945 to 1979 and 1979 to 1989 2,611 cases, buried at average 1.06 m After 1 hour 30-40%
 Introduction Welcome to COMPREHENSIVE BASIC LIFE SUPPORT Course. BLS is the foundation for saving lives after cardiac arrest. You will learn the skills of highquality cardiopulmonary resuscitation (CPR)
Introduction Welcome to COMPREHENSIVE BASIC LIFE SUPPORT Course. BLS is the foundation for saving lives after cardiac arrest. You will learn the skills of highquality cardiopulmonary resuscitation (CPR)
Minimum equipment list for cardiopulmonary resuscitation Primary dental care
 Minimum equipment list for cardiopulmonary resuscitation Primary dental care Resuscitation Council (UK) 5th Floor Tavistock House North Tavistock Square London WC1H 9HR Tel: 020 7388 4678 Fax: 020 7383
Minimum equipment list for cardiopulmonary resuscitation Primary dental care Resuscitation Council (UK) 5th Floor Tavistock House North Tavistock Square London WC1H 9HR Tel: 020 7388 4678 Fax: 020 7383
Chapter 9 Airway Respirations Metabolism Oxygen Requirements Respiratory Anatomy Respiratory Anatomy Respiratory Anatomy Diaphragm
 1 Chapter 9 Airway 2 Respirations Every cell of the body requires to survive Oxygen must come in and carbon must go out 3 Metabolism Metabolism--Process where the body s cells convert food to Adequate
1 Chapter 9 Airway 2 Respirations Every cell of the body requires to survive Oxygen must come in and carbon must go out 3 Metabolism Metabolism--Process where the body s cells convert food to Adequate
Principles of mechanical ventilation. Anton van Kaam, MD, PhD Emma Children s Hospital AMC Amsterdam, The Netherlands
 Principles of mechanical ventilation Anton van Kaam, MD, PhD Emma Children s Hospital AMC Amsterdam, The Netherlands Disclosure Research grant Chiesi Pharmaceuticals Research grant CareFusion GA: 27 weeks,
Principles of mechanical ventilation Anton van Kaam, MD, PhD Emma Children s Hospital AMC Amsterdam, The Netherlands Disclosure Research grant Chiesi Pharmaceuticals Research grant CareFusion GA: 27 weeks,
I nternational consensus 2and guidelines from
 F392 ORIGINAL ARTICLE Neonatal resuscitation 2: an evaluation of manual ventilation devices and face masks C P F O Donnell, P G Davis, R Lau, P A Dargaville, L W Doyle, C J Morley... See end of article
F392 ORIGINAL ARTICLE Neonatal resuscitation 2: an evaluation of manual ventilation devices and face masks C P F O Donnell, P G Davis, R Lau, P A Dargaville, L W Doyle, C J Morley... See end of article
INTRODUCTION TO BI-VENT (APRV) INTRODUCTION TO BI-VENT (APRV) PROGRAM OBJECTIVES
 INTRODUCTION TO BI-VENT (APRV) INTRODUCTION TO BI-VENT (APRV) PROGRAM OBJECTIVES PROVIDE THE DEFINITION FOR BI-VENT EXPLAIN THE BENEFITS OF BI-VENT EXPLAIN SET PARAMETERS IDENTIFY RECRUITMENT IN APRV USING
INTRODUCTION TO BI-VENT (APRV) INTRODUCTION TO BI-VENT (APRV) PROGRAM OBJECTIVES PROVIDE THE DEFINITION FOR BI-VENT EXPLAIN THE BENEFITS OF BI-VENT EXPLAIN SET PARAMETERS IDENTIFY RECRUITMENT IN APRV USING
Bunnell LifePulse HFV Quick Reference Guide # Bunnell Incorporated
 Bunnell Incorporated n www.bunl.com n 800-800-4358 (HFJV) n info@bunl.com 436 Lawndale Drive n Salt Lake City, Utah 84115 n intl 801-467-0800 n f 801-467-0867 Bunnell LifePulse HFV Quick Reference Guide
Bunnell Incorporated n www.bunl.com n 800-800-4358 (HFJV) n info@bunl.com 436 Lawndale Drive n Salt Lake City, Utah 84115 n intl 801-467-0800 n f 801-467-0867 Bunnell LifePulse HFV Quick Reference Guide
Virginia Office of Emergency Medical Services Scope of Practice - Procedures for EMS Personnel
 Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Oropharyngeal Airway Nasopharyngeal Airway Head
Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Oropharyngeal Airway Nasopharyngeal Airway Head
SimNewB. User Guide.
 EN SimNewB User Guide www.laerdal.com Contents Introduction 4 Items Included & Storage 5 System Overview & Setup 6 Features 7 Airway Features 7 Breathing Features 7 Vascular Features 7 Circulation Features
EN SimNewB User Guide www.laerdal.com Contents Introduction 4 Items Included & Storage 5 System Overview & Setup 6 Features 7 Airway Features 7 Breathing Features 7 Vascular Features 7 Circulation Features
E C C. American Heart Association. Basic Life Support for Healthcare Providers. Written Examinations. March 2011
 E C C American Heart Association Basic Life Support for Healthcare Providers Written Examinations Contents: Examination Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference
E C C American Heart Association Basic Life Support for Healthcare Providers Written Examinations Contents: Examination Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference
Breathing Process: Inhalation
 Airway Chapter 6 Breathing Process: Inhalation Active part of breathing Diaphragm and intercostal muscles contract, allowing the lungs to expand. The decrease in pressure allows lungs to fill with air.
Airway Chapter 6 Breathing Process: Inhalation Active part of breathing Diaphragm and intercostal muscles contract, allowing the lungs to expand. The decrease in pressure allows lungs to fill with air.
PERFORMANCE EVALUATION #34 NAME: 7200 Ventilator Set Up DATE: INSTRUCTOR:
 PERFORMANCE EVALUATION #34 NAME: 7200 Ventilator Set Up DATE: 1. **Identify and name the filters on the 7200ae. 2. **Explain how each filter is sterilized. 3. **Trace the gas flow through the ventilator
PERFORMANCE EVALUATION #34 NAME: 7200 Ventilator Set Up DATE: 1. **Identify and name the filters on the 7200ae. 2. **Explain how each filter is sterilized. 3. **Trace the gas flow through the ventilator
Operating Instructions for Microprocessor Controlled Ventilators
 Page 1 of 5 Operating Instructions for Microprocessor Controlled Ventilators Purpose Audience Scope Physician's Order To provide guidelines for the procedure for the use of microprocessor controlled ventilators.
Page 1 of 5 Operating Instructions for Microprocessor Controlled Ventilators Purpose Audience Scope Physician's Order To provide guidelines for the procedure for the use of microprocessor controlled ventilators.
Neonatal resusitation 1: A model to measure inspired and expired tidal volumes and assess leak at the face mask
 ADC-FNN Online First, published on May 4, 2005 as 10.1136/adc.2004.064683 Neonatal resusitation 1: A model to measure inspired and expired tidal volumes and assess leak at the face mask Colm P F O Donnell
ADC-FNN Online First, published on May 4, 2005 as 10.1136/adc.2004.064683 Neonatal resusitation 1: A model to measure inspired and expired tidal volumes and assess leak at the face mask Colm P F O Donnell
Automatic Transport Ventilator
 Automatic Transport Ventilator David M. Landsberg, MD, FACP, FCCP, EMT-P Luke J. Gasowski, RRT, NPS, ACCS, CCP-C, FP-C Christopher J. Fullagar, MD, FACEP, EMT-P Stan Goettel, MS, EMT-P Author credits /
Automatic Transport Ventilator David M. Landsberg, MD, FACP, FCCP, EMT-P Luke J. Gasowski, RRT, NPS, ACCS, CCP-C, FP-C Christopher J. Fullagar, MD, FACEP, EMT-P Stan Goettel, MS, EMT-P Author credits /
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress NURSES SETTING UP FOR ANAESTHESIA HOW TO PLAN FOR A SAFE ANAESTHETIC Sandra Forysth, BVSc DipACVA Institute of
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress NURSES SETTING UP FOR ANAESTHESIA HOW TO PLAN FOR A SAFE ANAESTHETIC Sandra Forysth, BVSc DipACVA Institute of
Airways and Resuscitators. CRC 330 Cardiorespiratory Care University of South Alabama
 Airways and Resuscitators CRC 330 Cardiorespiratory Care University of South Alabama Causes of Upper Airway Obstruction CNS depressionanesthesia, drug overdose Cardiac arrest Loss of consciousness Foreign
Airways and Resuscitators CRC 330 Cardiorespiratory Care University of South Alabama Causes of Upper Airway Obstruction CNS depressionanesthesia, drug overdose Cardiac arrest Loss of consciousness Foreign
Introduction to Conventional Ventilation
 Introduction to Conventional Ventilation Dr Julian Eason Consultant Neonatologist Derriford Hospital Mechanics Inspiration diaphragm lowers and thorax expands Negative intrathoracic/intrapleural pressure
Introduction to Conventional Ventilation Dr Julian Eason Consultant Neonatologist Derriford Hospital Mechanics Inspiration diaphragm lowers and thorax expands Negative intrathoracic/intrapleural pressure
Trust Guideline for Neonatal Volume Guarantee Ventilation (VGV)
 A Clinical Guideline For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author
A Clinical Guideline For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author
COALINGA STATE HOSPITAL. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
OXYGEN THERAPY. Catherine Jones June 2017
 OXYGEN THERAPY Catherine Jones June 2017 1 ACKNOWLEDGEMENT 2 LEARNING OUTCOMES To revise why Oxygen is important To identify the indications for Oxygen Therapy To identify problems with administration
OXYGEN THERAPY Catherine Jones June 2017 1 ACKNOWLEDGEMENT 2 LEARNING OUTCOMES To revise why Oxygen is important To identify the indications for Oxygen Therapy To identify problems with administration
Basic life support updates
 Basic life support 2010 updates Chest compressions. Airway, Breathing (C-A-B) science indicates the following order: 1. Check the patient for responsiveness and breathing. 2. Call for help and get the
Basic life support 2010 updates Chest compressions. Airway, Breathing (C-A-B) science indicates the following order: 1. Check the patient for responsiveness and breathing. 2. Call for help and get the
EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES
 GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
3100A Competency Exam
 NAME DATE (Circle the appropriate answer) 3100A Competency Exam 1. Of the following, which best describes the mechanics of ventilation used by the 3100A? a. Active inspiration with passive exhalation b.
NAME DATE (Circle the appropriate answer) 3100A Competency Exam 1. Of the following, which best describes the mechanics of ventilation used by the 3100A? a. Active inspiration with passive exhalation b.
Principles of Mechanical Ventilation: A Graphics-Based Approach
 Principles of Mechanical Ventilation: A Graphics-Based Approach Steven M. Donn, MD, FAAP Professor of Pediatrics Neonatal-Perinatal Medicine C.S. Mott Children s Hospital University of Michigan Health
Principles of Mechanical Ventilation: A Graphics-Based Approach Steven M. Donn, MD, FAAP Professor of Pediatrics Neonatal-Perinatal Medicine C.S. Mott Children s Hospital University of Michigan Health
Standards and guidelines for care and management of patients requiring oxygen therapy.
 PURPOSE Standards and guidelines for care and management of patients requiring oxygen therapy. STANDARDS Ongoing management of oxygen therapy requires a prescriber s order. The order must specify oxygen
PURPOSE Standards and guidelines for care and management of patients requiring oxygen therapy. STANDARDS Ongoing management of oxygen therapy requires a prescriber s order. The order must specify oxygen
Basics of Mechanical Ventilation. Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity
 Basics of Mechanical Ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Overview of topics 1. Goals 2. Settings 3. Modes 4. Advantages and disadvantages
Basics of Mechanical Ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Overview of topics 1. Goals 2. Settings 3. Modes 4. Advantages and disadvantages
Evidence Summary Recommendations for Pediatric Prehospital Protocols
 Evidence Summary Recommendations for Pediatric Prehospital Protocols Emergency Medical Services for Children State Partnership Purpose To provide summaries of existing evidence to address clinically-relevant
Evidence Summary Recommendations for Pediatric Prehospital Protocols Emergency Medical Services for Children State Partnership Purpose To provide summaries of existing evidence to address clinically-relevant
Basic Life Support & Automated External Defibrillation Course. OBJECTIVES
 OBJECTIVES Basic Life Support & Automated External Defibrillation Course www.erc.edu At the end of this course participants should be able to demonstrate: How to assess the collapsed victim. How to perform
OBJECTIVES Basic Life Support & Automated External Defibrillation Course www.erc.edu At the end of this course participants should be able to demonstrate: How to assess the collapsed victim. How to perform
Invasive mechanical ventilation:
 Invasive mechanical ventilation definition mechanical ventilation: using an apparatus to facilitate transport of oxygen and CO2 between the atmosphere and the alveoli for the purpose of enhancing pulmonary
Invasive mechanical ventilation definition mechanical ventilation: using an apparatus to facilitate transport of oxygen and CO2 between the atmosphere and the alveoli for the purpose of enhancing pulmonary
Neonatal resuscitation 2: An evaluation of manual ventilation devices and face masks
 ADC-FNN Online First, published on May 4, 2005 as 10.1136/adc.2004.064691 Neonatal resuscitation 2: An evaluation of manual ventilation devices and face masks Colm P F O Donnell 1, 2, Peter G Davis 1,
ADC-FNN Online First, published on May 4, 2005 as 10.1136/adc.2004.064691 Neonatal resuscitation 2: An evaluation of manual ventilation devices and face masks Colm P F O Donnell 1, 2, Peter G Davis 1,
Mechanical Ventilation
 PROCEDURE - Page 1 of 5 Purpose Scope Physician's Order Indications Procedure Mechanical Artificial Ventilation refers to any methods to deliver volumes of gas into a patient's lungs over an extended period
PROCEDURE - Page 1 of 5 Purpose Scope Physician's Order Indications Procedure Mechanical Artificial Ventilation refers to any methods to deliver volumes of gas into a patient's lungs over an extended period
ONLINE DATA SUPPLEMENT. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg
 APPENDIX 1 Appendix 1. Complete respiratory protocol. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg predicted body weight (PBW)) (NEJM 2000; 342
APPENDIX 1 Appendix 1. Complete respiratory protocol. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg predicted body weight (PBW)) (NEJM 2000; 342
Other diseases or age process
 1 BLS For Healthcare Providers 2 Time is Critical! begins to die in 4 to 6 minutes Brain matter cannot regenerate itself In order to sustain life, the human body must have going in and out and must be
1 BLS For Healthcare Providers 2 Time is Critical! begins to die in 4 to 6 minutes Brain matter cannot regenerate itself In order to sustain life, the human body must have going in and out and must be
Mechanical ven3la3on. Neonatal Mechanical Ven3la3on. Mechanical ven3la3on. Mechanical ven3la3on. Mechanical ven3la3on 8/25/11. What we need to do"
 8/25/11 Mechanical ven3la3on Neonatal Mechanical Ven3la3on Support oxygen delivery, CO2 elimination" Prevent added injury, decrease ongoing injury" Enhance normal development" Mark C Mammel, MD University
8/25/11 Mechanical ven3la3on Neonatal Mechanical Ven3la3on Support oxygen delivery, CO2 elimination" Prevent added injury, decrease ongoing injury" Enhance normal development" Mark C Mammel, MD University
Definition An uninterrupted path between the atmosphere and the alveoli
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Airway Management (Class 9) Airway Definition An uninterrupted path between the atmosphere and the alveoli Methods of opening the airway Positioning Left lateral recumbent
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Airway Management (Class 9) Airway Definition An uninterrupted path between the atmosphere and the alveoli Methods of opening the airway Positioning Left lateral recumbent
SPEMS SKILLS PROFICIENCY CRITERIA Paramedic
 SPEMS SKILLS PROFICIENCY CRITERIA Paramedic The following skills are required at the Paramedic Level: 1. King Airway 2. IV 3. Endotracheal Intubation 4. Adult EZ IO 5. Pedi EZ IO 6. Pleural Decompression
SPEMS SKILLS PROFICIENCY CRITERIA Paramedic The following skills are required at the Paramedic Level: 1. King Airway 2. IV 3. Endotracheal Intubation 4. Adult EZ IO 5. Pedi EZ IO 6. Pleural Decompression
B. A clinical emergency exists in which a profound hypoxia is determined to be present.
 I. Subject: Oxyhood-Oxygen Therapy for Neonates II. Policy: Oxygen therapy by oxyhood shall be initiated upon a physician's order by nurses and Respiratory Therapy personnel trained in the principles of
I. Subject: Oxyhood-Oxygen Therapy for Neonates II. Policy: Oxygen therapy by oxyhood shall be initiated upon a physician's order by nurses and Respiratory Therapy personnel trained in the principles of
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/46692 holds various files of this Leiden University dissertation Author: Zanten, Henriëtte van Title: Oxygen titration and compliance with targeting oxygen
Cover Page The handle http://hdl.handle.net/1887/46692 holds various files of this Leiden University dissertation Author: Zanten, Henriëtte van Title: Oxygen titration and compliance with targeting oxygen
Instructions/Procedure for Use of the Speaking Valve
 Instructions/Procedure for Use of the Speaking Valve Notes on the use of the speaking valve for ventilator-dependent and non-ventilator dependent patients The speaking valve is a one-way valve that allows
Instructions/Procedure for Use of the Speaking Valve Notes on the use of the speaking valve for ventilator-dependent and non-ventilator dependent patients The speaking valve is a one-way valve that allows
McHENRY WESTERN LAKE COUNTY EMS SYSTEM FALL 2014 CONTINUING EDUCATION MANDATORY FOR ALL PRIMARY AND PROBATIONARY ALS SYSTEM PROVIDERS.
 McHENRY WESTERN LAKE COUNTY EMS SYSTEM FALL 2014 CONTINUING EDUCATION MANDATORY FOR ALL PRIMARY AND PROBATIONARY ALS SYSTEM PROVIDERS ResQPOD In a cardiac arrest blood flow to the organs stop. Key to survival
McHENRY WESTERN LAKE COUNTY EMS SYSTEM FALL 2014 CONTINUING EDUCATION MANDATORY FOR ALL PRIMARY AND PROBATIONARY ALS SYSTEM PROVIDERS ResQPOD In a cardiac arrest blood flow to the organs stop. Key to survival
2005 Top Ten Major Changes in Treatment Recommendations *
 2005 Top Ten Major Changes in Treatment Recommendations * This document reviews the top ten new treatment recommendations and guidelines for ASHI s basic life support training programs for professional
2005 Top Ten Major Changes in Treatment Recommendations * This document reviews the top ten new treatment recommendations and guidelines for ASHI s basic life support training programs for professional
CPR Pro. for the Professional Rescuer. Student Handbook Preview. BLS for Healthcare Providers
 CPR Pro for the Professional Rescuer Student Handbook Preview BLS for Healthcare Providers CPR Pro Student Handbook, Version 7.0 Purpose of this Handbook This ASHI CPR Pro Version 7.0 Student Handbook
CPR Pro for the Professional Rescuer Student Handbook Preview BLS for Healthcare Providers CPR Pro Student Handbook, Version 7.0 Purpose of this Handbook This ASHI CPR Pro Version 7.0 Student Handbook
excellence in care Procedure Management of patients with difficult oxygenation. For Review Aug 2015
 Difficult Oxygenation HELI.CLI.12 Purpose This procedure describes the processes and procedures for a lung protective strategy in the mechanical ventilation of patients that are difficult to oxygenate
Difficult Oxygenation HELI.CLI.12 Purpose This procedure describes the processes and procedures for a lung protective strategy in the mechanical ventilation of patients that are difficult to oxygenate
Children Small Adults Newborns Small Children
 Children Small Adults Newborns Small Children Curt Partain RRT-NPS NICU Respiratory Care Clinical Educator Community Regional Medical Center Fresno, Ca. Oxygen Use: Infants > 35 weeks gestation begin with
Children Small Adults Newborns Small Children Curt Partain RRT-NPS NICU Respiratory Care Clinical Educator Community Regional Medical Center Fresno, Ca. Oxygen Use: Infants > 35 weeks gestation begin with
Neonatal Assisted Ventilation. Haresh Modi, M.D. Aspirus Wausau Hospital, Wausau, WI.
 Neonatal Assisted Ventilation Haresh Modi, M.D. Aspirus Wausau Hospital, Wausau, WI. History of Assisted Ventilation Negative pressure : Spirophore developed in 1876 with manual device to create negative
Neonatal Assisted Ventilation Haresh Modi, M.D. Aspirus Wausau Hospital, Wausau, WI. History of Assisted Ventilation Negative pressure : Spirophore developed in 1876 with manual device to create negative
E C C. American Heart Association. BLS for Healthcare Providers. Written Exams. January 12, 2012
 E C C American Heart Association BLS for Healthcare Providers Written Exams Contents: Exam Memo Student Answer Sheet Version C Exam Version C Answer Key Version C Reference Sheet Version D Exam Version
E C C American Heart Association BLS for Healthcare Providers Written Exams Contents: Exam Memo Student Answer Sheet Version C Exam Version C Answer Key Version C Reference Sheet Version D Exam Version
PHTY 300 Wk 1 Lectures
 PHTY 300 Wk 1 Lectures Arterial Blood Gas Components The test provides information on - Acid base balance - Oxygenation - Hemoglobin levels - Electrolyte blood glucose, lactate, renal function When initially
PHTY 300 Wk 1 Lectures Arterial Blood Gas Components The test provides information on - Acid base balance - Oxygenation - Hemoglobin levels - Electrolyte blood glucose, lactate, renal function When initially
Basic Life Support Adult
 1/2.4.1 Version 4, 03/2016 Basic Life Support Adult Collapse If physically unable to ventilate perform compression only CPR Unresponsive and breathing abnormally or gasping 112 / 999 Shout for help 112
1/2.4.1 Version 4, 03/2016 Basic Life Support Adult Collapse If physically unable to ventilate perform compression only CPR Unresponsive and breathing abnormally or gasping 112 / 999 Shout for help 112
Monitoring, Ventilation & Capnography
 Why do we need to monitor? Monitoring, Ventilation & Capnography Keith Simpson BVSc MRCVS MIET(Electronics) Torquay, Devon. Under anaesthesia animals no longer have the ability to adequately control their
Why do we need to monitor? Monitoring, Ventilation & Capnography Keith Simpson BVSc MRCVS MIET(Electronics) Torquay, Devon. Under anaesthesia animals no longer have the ability to adequately control their
Guidelines on Monitoring in Anaesthesia
 Page 1 of 8 Guidelines on Monitoring in Anaesthesia Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUL 2013 5 MAY 2017 Document No. HKCA P1 v5 Prepared by College Guidelines Committee Endorsed
Page 1 of 8 Guidelines on Monitoring in Anaesthesia Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUL 2013 5 MAY 2017 Document No. HKCA P1 v5 Prepared by College Guidelines Committee Endorsed
2016 EFR CPR & AED Instructor Guide Errata Revision to 12/11 EFR CPR & AED English Instructor Guide (product #79215, English, Vision 1.
 2016 EFR CPR & AED Instructor Guide Errata Revision to 12/11 EFR CPR & AED English Instructor Guide (product #79215, English, Vision 1.0) Cover and inside cover, bottom of page, change version and copyright
2016 EFR CPR & AED Instructor Guide Errata Revision to 12/11 EFR CPR & AED English Instructor Guide (product #79215, English, Vision 1.0) Cover and inside cover, bottom of page, change version and copyright
R S A B C CPR. Basic Life Support Flow Chart Check for danger. Check Response. Send for Help. Check Airway. Check for Breathing.
 CPR CPR is the technique of the manual inflation of the lungs with oxygen, and compression of the heart, therefore pumping oxygenated blood around the body, and keeping the vital organs supplied with oxygen.
CPR CPR is the technique of the manual inflation of the lungs with oxygen, and compression of the heart, therefore pumping oxygenated blood around the body, and keeping the vital organs supplied with oxygen.
BASIC LIFE SUPPORT (BLS) PROVIDER HANDBOOK
 BASIC LIFE SUPPORT (BLS) PROVIDER HANDBOOK P R E S E N T E D B Y ADVANCED MEDICAL CERTIFICATION (AMC) W R I T T E N B Y DR. KARL FRITZ DISQUE 1 Copyright 2013 Satori Continuum Publishing All rights reserved.
BASIC LIFE SUPPORT (BLS) PROVIDER HANDBOOK P R E S E N T E D B Y ADVANCED MEDICAL CERTIFICATION (AMC) W R I T T E N B Y DR. KARL FRITZ DISQUE 1 Copyright 2013 Satori Continuum Publishing All rights reserved.
SimBaby. User Guide.
 EN SimBaby User Guide www.laerdal.com Contents Introduction 4 Items Included 5 System Overview & Setup 6 Features 7 Airway Features 7 Breathing Features 7 Cardiovascular Features 7 Vascular Features 7
EN SimBaby User Guide www.laerdal.com Contents Introduction 4 Items Included 5 System Overview & Setup 6 Features 7 Airway Features 7 Breathing Features 7 Cardiovascular Features 7 Vascular Features 7
STANDARDIZED PROCEDURE NEONATAL INTUBATION (Neonatal)
 I. Definition This procedure is done in order to establish access to the airway in order to assist ventilation by the use of either endotracheal tube (ET tube) and bag, ET tube and continuous positive
I. Definition This procedure is done in order to establish access to the airway in order to assist ventilation by the use of either endotracheal tube (ET tube) and bag, ET tube and continuous positive
MEDUMAT Standard a MEDUMAT Standard. The Ventilation Standard for Professionals
 a The Ventilation Standard for Professionals a The Ventilation Standard for Professionals a offers you everything you need for reliable emergency ventilation. Users around the world are impressed by its
a The Ventilation Standard for Professionals a The Ventilation Standard for Professionals a offers you everything you need for reliable emergency ventilation. Users around the world are impressed by its
OXYGEN THERAPY. (Non-invasive O2 therapy in patient >8yrs)
 OXYGEN THERAPY (Non-invasive O2 therapy in patient >8yrs) Learning aims Indications and precautions for O2 therapy Targets of therapy Standard notation O2 delivery devices Taps, tanks and tubing Notation
OXYGEN THERAPY (Non-invasive O2 therapy in patient >8yrs) Learning aims Indications and precautions for O2 therapy Targets of therapy Standard notation O2 delivery devices Taps, tanks and tubing Notation
B.L.S احیای پایھ کودکان American Heart Association
 B.L.S احیای پایھ 2010 American Heart Association کودکان زنجیره حیاتی کودکان 1.prevention, 2.early CPR, 3.prompt access to the emergency response system, 4.rapid PALS, 5. integrated post cardiac arrest
B.L.S احیای پایھ 2010 American Heart Association کودکان زنجیره حیاتی کودکان 1.prevention, 2.early CPR, 3.prompt access to the emergency response system, 4.rapid PALS, 5. integrated post cardiac arrest
PART SEVEN THE HISTORY AND APPLICATION OF HIGH FREQUENCY OSCILLATORY VENTILATION (HFOV)
 PART SEVEN THE HISTORY AND APPLICATION OF HIGH FREQUENCY OSCILLATORY VENTILATION (HFOV) Reciprocating pistons with an eccentric travel speed, moving to and fro within a cylinder (with a common inlet/outlet),
PART SEVEN THE HISTORY AND APPLICATION OF HIGH FREQUENCY OSCILLATORY VENTILATION (HFOV) Reciprocating pistons with an eccentric travel speed, moving to and fro within a cylinder (with a common inlet/outlet),
Once student shouts for help, instructor says, Here s the barrier device. I am going to get the AED. STOP TEST
 Adult CPR and AED Adult Skills CPR Testing and Checklist AED Skills Testing Checklist Student Name Date of Test Hospital Scenario: You are working in a hospital or clinic, and you see a person who has
Adult CPR and AED Adult Skills CPR Testing and Checklist AED Skills Testing Checklist Student Name Date of Test Hospital Scenario: You are working in a hospital or clinic, and you see a person who has
B-CARD NO PAUSE SHOULD BE YOUR CAUSE
 B-CARD NO PAUSE SHOULD BE YOUR CAUSE SIMEU Congress, 17-20 November, Symposium Georges Bousignac 1 Cardiac arrest: A new cutting edge treatment method by Dr. Boussignac No Pause Should Be Your Cause 2
B-CARD NO PAUSE SHOULD BE YOUR CAUSE SIMEU Congress, 17-20 November, Symposium Georges Bousignac 1 Cardiac arrest: A new cutting edge treatment method by Dr. Boussignac No Pause Should Be Your Cause 2
