New method of chest compression for infants in a single rescuer situation: thumb-index finger technique
|
|
|
- Elvin Booker
- 5 years ago
- Views:
Transcription
1 J Med Dent Sci 2011; 58: Original Article New method of chest compression for infants in a single rescuer situation: thumb-index finger technique Bakhtiyar Zeynalov Fakhraddin 1), Naoki Shimizu 2), Sasa Kurosawa 2), Hirokazu Sakai 2), Katsuyuki Miyasaka 3) and Shuki Mizutani 1) 1) Tokyo Medical & Dental University, Tokyo, Japan 2) National Center for Child Health and Development, Tokyo, Japan 3) Nagano Children s Hospital, Nagano, Japan We introduce a new method of external chest compression (ECC), an essential part of cardiopulmonary resuscitation, using a thumb and index finger method (TIFM) on infants, and compares, this with two standard methods of the two finger method (TFM) and the two-thumb encircling hands method (TTEM). Sixty trained PALS (Pediatric Advanced Life Support) providers were randomly assigned into three groups and provided one-rescuer ECC for a period of five continuous minutes. Results without coaching or feedback were recorded on a recording CPR simulator (Laerdal, Inc). ECC was performed according to the BLS recommendations of the International Liaison Committee on Resuscitation (ILCOR). The quality of ECC in the TFM group deviated considerably from guideline recommendations. The same parameters in the TTEM and new TIFM groups during this study were in accordance with the parameters recommended by the guidelines. Thus, our new TIFM technique of chest compression, in infants was shown to be better than the currently TFM, especially for achieving adequate compression depth and avoiding fatigue, and is equally as effective as the TTEM. We propose this new method (TIFM) should be considered as the method of choice in single rescuer situations. Corresponding Author: Katsuyuki Miyasaka Tokyo Medical and Dental University, Yushima Bunkyo-ku, Tokyo Japan Tel: Fax: katsmiyasaka@me.com Received September 30;Accepted November 12, 2010 Key words: cardiopulmonary resuscitation (CPR); basic life support (BLS); external chest compression (ECC); chest compression quality; fatigue Introduction Training programs for cardiopulmonary resuscitation (CPR) have been implemented worldwide over the last 50 years, and are based on guidelines established by the European Resuscitation Council (ERC) and the American Heart Association (AHA), which are based on recent international consensus [1]. These programs specify course content, management, and guidelines for CPR practice and testing, including criteria for the correct performance of CPR. However, survival rates from cardiac arrest remain poor despite the development of both CPR and electrical defibrillation as treatment modalities over the past 50 years. In an effort to improve cardiac arrest outcomes, recent investigations have focused on the timing and quality of CPR [2, 3, 4]. Tests immediately after a traditional instructor CPR course with lectures, demonstrations, training, and evaluation have demonstrated poor skills performance [5, 6]. It has been discussed whether this is caused by the course content, the instructor, the training technique or something else. Multiple studies have demonstrated that rescuer fatigue can affect chest compression quality, and that the rescuer does not recognize when fatigue affects CPR performance [3, 5, 7]. Current AHA guidelines recommend the two-thumb method (TTEM) for two rescuers and the two finger chest compression method (TFM) for the lone rescuer. It is known, however, that TTEM is better than TFM, as
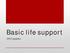
2 16 B. Zeynalov Fakhraddin et al. J Med Dent Sci Figure 1 : New method of external chest compression Figure presents the new method of external chest compression. TFM is prone to fatigue. A better technique for a single rescuer is needed. We have been carrying out a comparative analysis of infant chest compression during CPR and we believe we have found a better alternative to existing standard methods of chest compression during CPR in infants. Materials and methods The study protocol was approved by the institutional clinical investigation review board and informed consent was obtained prior to the study from the volunteers who participated. Subjects Sixty trained PALS providers (18 female, 42 male, 27.8 ± 2.1 years) were randomly assigned to provide one-rescuer CPR for a period of five continuous minutes using three different methods (TFM, TTEM, or TIFM). This prospective study was carried out with a modified CPR simulator (Resusci-Anne with the PC Skill Reporting System, Ver ; Laerdal). This basic life support (BLS) simulator was equipped with functions that can continuously record the rate of compressions, the actual number of compressions per minute, the actual depth and location of compressions, recoil decompression (hand release), and interruption of CPR. Description of the new method A fist is made with the pad of the thumb pressed tightly against the side of the middle phalanx of the index finger. The tip half of the pad of the thumb and the dorsum of the middle phalanx are placed on the front of the sternum, with the thumb placed in the direction of the jugular notch (Figure 1). All other requirements for ECC are the same. Chest compression is applied over the lower part of the sternum at a rate of 100 per minute. Compression and relaxation should take an equal amount of time and compression depth should be 1/3 the anterior-posterior diameter of the chest. Pressure should be released without losing contact. Study protocol Sixty participants were enrolled and randomly divided into three groups. At the beginning of each session, investigators informed participants of the method of chest compression, ratio and depth chosen. Each participant provided one-rescuer CPR over a period of five consecutive minutes. Results were recorded from time 0 to 1 minute (first interval), from 2 to 3 minutes (second interval), and from 4 to 5 minutes (third interval) over a period of five consecutive minutes. Participants were not told the intermediary results. This study was carried out at the National Center for Child Health and Development (NCCHD), Tokyo, and all participants were volunteers who were recruited from new residents who had just completed a BLS and pediatric advanced life support (PALS) provider course at the institution. CPR was performed according to the BLS recommendations proposed by the International Liaison Committee on Resuscitation (ILCOR) with the following
3 New method of chest compression for infants 17 requirements: compression is applied over the lower part of the sternum, compression and relaxation should take an equal amount of time, compression depth should be 1/3 the anterior-posterior diameter of the chest, and the pressure should be released without losing contact. We chose, an ECC duration of five minutes, because this duration has been used in the literature [2, 8, 9]. The quality of chest compressions was evaluated according to international recommendations [1, 10]. In previous studies, the quality was assessed on the basis of rate, correct location of hands and adequate compression depth during a period of five minutes of CPR. The quality of CPR was assessed with additional CPR indices including incomplete recoil, excess depth, suitable and unsuitable ECC, and no error ECC, in percentages. Suitable compression depth has been defined as depth from mm. Attempt level was defined as the minimum depth to detect a compression and has been set as 10 mm. Incomplete recoil is detected if compression is not released above the attempt level. Unsuitable compression depth is defined as depth more than the attempt level, but less than 38 mm. Excessive compression depth was defined as depth more than 51mm (Resusci-Anne with the PC Skill Reporting System, Ver ; Laerdal) [11]. Data aquisition We modified a standard CPR infant manikin to visually monitor and record chest compression quality including depth and timing. Trained CPR providers performed chest compressions targeting 1/3 of chest diameter for five minutes continuously using the two-thumb (TTEM), two finger (TFM), and new method (TIFM) (n=20, n=20, n=20 respectively) without looking at the monitor display. The only exception was in the TFM group. The depth of chest compression was initially too shallow, so we had to give feedback after the first interval to let participants briefly see the compression process on the computer display. This feedback was not given in the other two groups. Statistical Analysis A spreadsheet application (Excel 2008; Microsoft) was used to calculate mean values and their standard deviations. Differences in CPR parameters for outcome evaluation between three groups were assessed using the analysis of Variance (ANOVA). Additionally, differences in CPR parameters between TTEM and TIFM groups were assessed using a t-student test. A p value below 0.05 (p<0.05) was considered as statistically significant. Results Sixty participants (18 females, 42 males) were enrolled. The mean age was 27.8 ± 2.1 years. No significant deviation of chest compression location was observed in any of the three study groups. The rates of chest compression achieved were quite different among the study groups, with a mean of ± 12 per minute in TFM, ± 9.5 per minute in TTEM and 98.7 ± 6.4 per minute in new TIFM. The difference in ECC rate between the TFM and TTEM groups during the study was statistically significant (p<0.05), whereas the average ECC rates shown in the TTEM and TIFM groups were similar. The depth of compression in the three groups is shown in Figure 2. The depth of chest compression in the TFM group was initially extremely shallow (28.4 mm, 27.1 mm, and 26.6 mm at the first, second and third intervals, respectively) and we had to give feedback. The depth of compression initially improved, but the depth of ECC decayed significantly over five minutes (33.3 mm, 30.7 mm, 28.8 mm at the 3 intervals, respectively). The tendency for compression depth to become shallower in this group over time was obvious. Statistically, the difference between depth in the first and the second intervals and between the second and the third was not significant. Chest compression depth changes in TTEM (33.3 mm, 32.9 mm, and 33.0 mm at the 3 intervals, respectively) were not statistically significant. Statistically significant differences in ECC depth between TFM and TTEM were observed (p<0.05). No statistically significant differences in chest compression depth over the time course in the TIFM group (33.4 mm, 33.4 mm, and 33.1 mm at the 3 intervals, respectively) were observed. No statistically significant differences in ECC depth were found between the TIFM and TTEM groups over the same time course (Figure 2). A small percentage of incomplete chest decompression was observed in TFM (3.8%, 9.2%, 8.1% at the first, second and third intervals, respectively) (Figure 3). The proportion of incomplete recoil was greatest in TTEM at 50.3%, 57.3%, and 50.5%, at the 3 intervals, respectively. In contrast, the percentage of incomplete recoil progressively declined during the 5 minute study period in TIFM. It averaged 23% at the end of the first interval, 14.5% at the end of the second interval, and was 9% at the end of the third interval, however these changes were not statistically significant. There was
4 18 B. Zeynalov Fakhraddin et al. J Med Dent Sci depth, mm (min) TFM group with feedback TTEM group TIFM group TFM group without feedback Figure 2 : Comparing of compression depth average Figure shows that, in the TFM group compression depth was initially extremely shallow and became shallower over time, even after we gave feedback. Compression depth changes in TTEM and TIFM groups were not significant over the course of the study. Percent * * * (min) TFM group TIFM group TTEM group Figure 3 : Incomplete recoil percentage Figure shows that, the smallest percentage of incomplete chest recoil was observed in TFM group, and greatest in TTEM group. In contrast, this parameter progressively declined during the study period in TIFM group, and difference between TIFM and TTEM groups was a statistically significant (*p<0.05). a statistically significant difference in the proportion of incomplete recoil between TIFM and TTEM (p<0.05) (Figure 3). Unsuitable chest compression percentage average in TTEM and TIFM groups was the 11.6 ± 25.2% and 7.2 ± 12.4% respectively. In case of TFM group, the unsuitable chest compression percentage increased from 7 ± 16.1% in first minute to 50.1 ± 33.9% in second, till 81.2 ± 28.4% in finish of CPR (Figure 4). In Table 1, we show the percentage of excess compression depth. Excessive compression depth was defined as depth more than 51 mm (Resusci-Anne with the PC Skill Reporting System, Ver ; Laerdal). The biggest excess chest compression depth was observed in TTEM. The average was 7.2 ± 22.7% with 9.7 ± 28.1% in the first interval, 6.5 ± 20.9% in the second interval, and 5.4 ± 19.1% in the third interval. In TFM, the excess depth averaged 6.7 ± 21% with 10.1 ± 21% in the first interval, 4.9 ± 21.5% in the second interval, and 5.1 ± 21.2% in the third interval). TIFM showed the least percent of excess depth and averaged 2.2 ± 8.2% with 1.5 ± 5.4% in the first
5 New method of chest compression for infants 19 percent TFM group TIFM group TTEM group (min) Figure 4 : Unsuitable chest compression percentage Figure shows low average percentages of unsuitable chest compressions in TIFM and TTEM groups, over the course of the study. In contrast, this index progressively and rapidly increased over time in TFM group. Table 1 : Materials and final results of CPR study This table summarizes information about chest compressions characteristics, in all groups during study. Information presented as average with standard deviation. Group TFM CPR time, (min) Rate (/minute) Depth (mm) Chest compressions characteristics during CPR Incomplete recoil Excess depth No error ECC Suitable ECC Unsuitable ECC ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± 28.4 Average, SD ± ± ± ± ± ± ± 40.7 TTEM ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± 26.7 Average, SD ± ± ± ± ± ± ± 25.2 TIFM ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± 11.2 Average, SD 98.7 ± ± ± ± ± ± ± 12.4 interval, 3 ± 10.8% in the second interval, and 2.2 ± 8% in the third interval). The differences in excess compression depth among the three groups were not statistically significant. Discussion Good quality external chest compression (ECC) is of paramount importance in CPR. Good ECC can be defined as chest compression with a good quality of force [8, 9], appropriate rate [12], appropriate compression duration and adequate decompression (recoil) time, without unnecessary interruptions or pauses [13]. This has been confirmed in animal studies [14, 15], experimental swine models [16], and in other laboratory studies [2, 17, 18]. Achieving good quality ECC, however, is not easy. Discrepancy between the performance of healthcare professionals and guideline recommendations, particularly for the rate and the depth of compressions has been reported recently [8, 13]. Abella et al. [3] reported that the correct rate of ECC was found only
6 20 B. Zeynalov Fakhraddin et al. J Med Dent Sci 31.4% of the time during in-hospital-resuscitation. Aufderheide et al. [6] reported weak compression depth by healthcare professionals during the assessment of different alternative manual chest compression techniques. Wik et al. reported a mean compression depth of 34 mm and only 28% of compressions were within the recommended depth of mm in out-ofhospital CPR [5]. It was reported that the quality of chest compression often deviated from guideline recommendations [3] in several important parameters, including chest compression depth, compression recoil, percent of chest compressions without error, and percent of suitable and unsuitable compressions. Specifically, the percentage of suitable chest compression was often less than recommended, and compression depth was often far shallower than the accepted minimum. These reports confirm other recent investigations suggesting that CPR quality may be highly variable in actual practice [4, 19]. We found that the depth of compression in standard TFM tended to become shallower over time. The average depth in TFM was only 27.3 mm at the end of the third interval. The difference in ECC depth between TFM and TTEM over the same time course of the study was statistically significant and TTEM clearly was superior in this aspect (p<0.05) (Figure 2). The reason and explanation for the observed difference, in our view, was the physical tiredness of participants, as well as finger pain in TFM, but further study is needed to confirm these speculations. Two manikin studies [20, 21], one animal study [22], and case reports of hemodynamic monitoring in infants [23] also showed that TTEM produces higher coronary perfusion pressures, higher systolic and diastolic arterial pressures and more consistent correct depth and force of compression than TFM. In our study, the depth of compression in TTEM was more acceptable than that of TFM and changes in compression depth over time were more stable. The average depth in TTEM was 33.3 mm in the first interval, 32.9 mm in the second interval, and 33.0 mm in the third interval. These are in accordance with the parameters recommended by AHA [1]. Fatigue during experimental CPR performed by healthcare providers was reported by Ashton A. [7]. He studied two consecutive 3-minute periods of continuous compressions separated by a 30-second time interval on a manikin. While the total number of compressions was maintained (100/min) over both periods of CPR, the number of suitable chest compressions performed decreased from 82 in the first minute to only 27 by the fifth minute. Seven subjects were unable to complete a second three minute interval due to fatigue. The average percentages of suitable chest compressions in TIFM, and TTEM were consistently high at 90.9% and 85.8% respectively. In TFM, this declined progressively over time with 87.6% in the 1st interval, 50.2% in the second interval and 20.1% by the end of the third interval. The differences over time were statistically significant (p<0.05). Why TIFM technique could avoid fatigue? We supposed that: thumb having a skeleton of phalanges, joined by hinge-like joints is opposable and can provide powerful flexion toward the palm of the hand; has two phalanges, so less flexible, but more powerful; has greater breadth in the distal phalanx, than in the proximal phalanx that provide more precise allocation ability on the chest. Index finger is usually the most dexterous and sensitive finger of the hand. In our view, application thumb and index altogether, provide more fine, precise and powerful compression of chest during CPR. The average percentages of unsuitable chest compressions in TIFM and TTEM were low over the course of the study at 7.2% and 11.6%, respectively. The differences between these two groups were not statistically significant. In contrast, this index progressively and rapidly increased over time in TFM, with an average of 46%. These changes were statistically significant (p<0.05) (Figure 4). An analysis of errors in chest compression can be seen in Table 1. The highest percentage of faultless (no-error) compression was obtained in TIFM with an average percentage of 78.9%. In TFM, this index progressively and rapidly decreased over time from 83.6% in the first interval, to 48% in the second interval and 19.1% by the end of the third interval. The average was 50.2%. The high percentage of faultless compression in the first minute of TFM could not be sustained and cumulative fatigue and pain led to a rapid deterioration. We were surprised to find an unexpectedly low percentage of faultless compression in TTEM with an average of 41.6%. The reason, as it turned out, is that TTEM has the highest percentage of incomplete recoil during the study, an average of 52.7% (Figure 3). The importance of the decompression phase during CPR is well known. Incomplete chest recoil during cardiopulmonary resuscitation (CPR) in the decompression phase is purported to decrease venous return, and thereby decrease forward blood flow. We
7 New method of chest compression for infants 21 found higher incomplete decompression in TTEM due to the fact that holding the manikin s thorax with two hands may limit the mobility of joined thumbs. On the other hand, the lowest percentage of incomplete recoil during the ECC was observed in TFM. In our view, this may be due to the desire of the participants to release pressure early to reduce pain sensation upon compression. The average percentage of incomplete decompression during the CPR with TIFM was 15.5%, which is better than TFM and TTEM. The goal of CPR is to provide adequate blood flow to the brain and heart. Chest compression increases pressure within the thorax, forcing blood out to the heart, brain and other organs, and air out of the lungs. The importance of providing uninterrupted chest compressions is emphasized since every interruption causes a dramatic decrease in coronary perfusion pressure [24]. Compressions should be provided at a rate of 100 per minute and the chest should be compressed 1½ 2 inches, with half the time spent compressing the chest and the other half spent allowing the chest to fully recoil (decompress). Full chest-wall recoil is also essential [25]. Negative intrathoracic pressure is produced each time the chest is allowed to fully decompress, drawing blood back into the heart and some quantity of air into the lungs [26]. During the chest-recoil phase, blood flows through the coronary arteries, to provide the heart muscle with blood. Performing CPR with uninterrupted compressions and full chest-wall recoil will optimize blood flow to the heart and brain [25, 26]. TTEM produced the highest percentage of excess depth of compression of the chest (Table 1), averaging 7.2%. The percentage of excess compression depth in TFM was 6.7% and slightly lower than TTEM, but it was 2.2% and lowest in TIFM. Our new thumb index finger method (TIFM) can be considered as a better alternative to the current standard two finger method (TFM). Several limitations of our study should be discussed. First is the possible existence of the Hawthorne effect, as participants were newly trained resident physicians and knew that there were being studied. This Hawthorne effect could have possibly decreased significant deviations from the recommended practice in our study [2, 27]. However, even with the Hawthorne effect, the quality of ECC performed by professional healthcare providers showed significant differences among the three methods we studied and does not affect our conclusion. The differences may be greater if we consider applying our results to bystanders. Second, we studied only 5 consecutive minutes per participant. This can be considered as rather short for a real CPR situation, but we though it is appropriate for our study as nearly 30 % of the participants were female and we did not want the results to be affected by physical stamina. Many previously published CPR studies have adopted the same duration [2, 8, 9]. We found significant differences even with a seemingly short study period. Third, the manikin we used in our study was an unconscious and pulseless infant model. It is debatable if CPR performance on this manikin in this situation can be converted into real clinical practice. While it is an appropriate concern, the issue has been discussed in several previous studies [4, 8, 19]. Our focus was solely on the ECC function of the manikin and one manikin was used for data acquisition. We used the criteria predetermined by the simulator (Resusci-Anne with the PC Skill Reporting System, Ver ; Laerdal) in assessing the quality of ECC. Those criteria have been used on many preciously published papers, and it was felt appropriate for comparing three different methods [6, 8, 9, 20]. While manikins are not human patients, they are used widely in this field. Further observational and randomized controlled studies will be necessary and desirable to confirm these preliminary observations. Conclusions We introduced a new method of chest compression in infants called the thumb-index finger method (TIFM). This method was found to be more useful than the standard two finger method (TFM) as it is less susceptible to fatigue and produced better quality ECC, which is comparable to TTEM used in a two rescuer situation. This new method should be considered as the method of choice in single rescuer situations. Conflict of interest The authors declare that Laerdal Medical Corporation, Japan, provided training and recording devices for the investigators of the study. No financial support that could influence the work was granted to any of the listed authors. Acknowledgements We thank all of the resident doctors of Anesthesia and
8 22 B. Zeynalov Fakhraddin et al. J Med Dent Sci PICU of the National Child Health and Development Center, Tokyo, Japan, for participating in this study and Laerdal Medical Corporation, Japan, for loaning the manikin and recording system to this study. References 1. The International Liaison Committee on Resuscitation (ILCOR). Consensus on Science With Treatment Recommendations for Pediatric and Neonatal Patients: Pediatric Basic and Advanced Life Support Pediatrics 2006; 117; e955-e Benjamin S. Abella; Jason P. Alvarado; Helge Myklebust; et al. Quality of Cardiopulmonary Resuscitation During In- Hospital Cardiac Arrest. JAMA. 2005; 293(3): Abella BS, Sandbo N, Vassilatos P, et al. Chest compression rates during cardiopulmonary resuscitation are suboptimal: a prospective study during in-hospital cardiac arrest. Circulation 2005; 111(4): Boyle AJ, Wilson AM, Connelly K, McGuigan L, Wilson J, Whitbourn R. Improvement in timing and effectiveness of external cardiac compressions with a new non-invasive device: the CPR-Ezy. Resuscitation 2002; 54(1): Wik L, Kramer-Johansen J, Myklebust H, et al. Quality of cardiopulmonary resuscitation during out-of-hospital cardiac arrest. JAMA 2005; 293(3): Aufderheide TP, Pirrallo RG, Yannopoulos D, et al. Incomplete chest wall decompression: a clinical evaluation of CPR performance by EMS personnel and assessment of alternative manual chest compression decompression techniques. Resuscitation 2005; 64(3): Ashton A, McCluskey A, Gwinnutt CL, Keenan AM. Effect of rescuer fatigue on performance of continuous external chest compressions over 3 min. Resuscitation. 2002; 55: Stefan K. Beckersa, Max H. Skorning, Michael Fries, Johannes Bickenbach, Stephan Beuerlein, et al. CPREzyTM improves performance of external chest compressions in simulated cardiac arrest. Resuscitation (2007) 72, Udassi S, Udassi JP, Lamb MA, Theriaque DW, Shuster JJ, Zaritsky AL, Haque IU. Two-thumb technique is superior to two-finger technique during lone rescuer infant manikin CPR. Resuscitation Jun; 81(6): Epub 2010 Mar American Heart Association American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Part 11: Pediatric Basic Life Support. Circulation. 2005; 112:IV-156-IV Operation Manual, Resusci-Anne with the PC Skill Reporting System, Ver ; Laerdal, Halperin HR, Tsitlik JE, Guerci AD, et al. Determinants of blood flow to vital organs during cardiopulmonary resuscitation in dogs. Circulation 1986; 73(3): Greingor JL. Quality of cardiac massage with ratio compression-ventilation 5/1 and 15/2. Resuscitation 2002; 55: Sato Y, Weil MH, Sun S, et al. Adverse effects of interrupting precordial compression during cardiopulmonary resuscitation. Crit Care Med. 1997; 25: Steen S, Liao Q, Pierre L, Paskevicius A, Sjoberg T. The critical importance of minimal delay between chest compressions and subsequent defibrillation: a haemodynamic explanation. Resuscitation. 2003; 58: Yu T., Weil M.H., Tang W., et al. Adverse outcomes of interrupted precordial compression during automated defibrillation. Circulation. 2002; 106: Kern KB. Limiting interruptions of chest compressions during cardiopulmonary resuscitation. Resuscitation. 2003; 58: Koster RW. Limiting hands-off periods during resuscitation. Resuscitation. 2003; 58: Joseph W. Heidenreich, MD, Robert A. Berg, MD, et al. Rescuer Fatigue: Standard versus Continuous Chest- Compression Cardiopulmonary Resuscitation. Academic Emergency Medicine 2006; 13: Whitelaw CC, Slywka B, Goldsmith LJ. Comparison of a two-finger versus two thumb method for chest compressions by healthcare providers in an infant mechanical model. Resuscitation 2000; 43: Dorfsman ML, Menegazzi JJ, Wadas RJ, Auble TE. Two thumb vs two-finger chest compression in an infant model of prolonged cardiopulmonary resuscitation. Acad Emerg Med. 2000; 7: Houri PK, Frank LR, Menegazzi JJ, Taylor R. A randomized, controlled trial of two-thumb vs two-finger chest compression in a swine infant model of cardiac arrest. Prehosp Emerg Care. 1997; 1: David R. Closed chest cardiac massage in the newborn infant. Pediatrics. 1988; 81: Manning JE, Murphy CA Jr., et al. Selective aortic arch perfusion during cardiac arrest: A new resuscitation technique. Ann Emerg Med 21:1,058-1,065, Mathias Zuercher, Ronald W Hilwig, Jon Nysaether, Vinay M Nadkarni, Marc D Berg, Gordon A Ewy, Karl B Kern, et al. Incomplete Chest Recoil During Piglet CPR Worsens Hemodynamics (Circulation. 2007; 116:II_929.) 2007 American Heart Association, Inc. 26. Yannopoulos D, McKnite S, Aufderheide TP, et al. Effects of incomplete chest wall decompression during cardiopulmonary resuscitation on coronary and cerebral perfusion pressures in a porcine model of cardiac arrest. Resuscitation 64(3): , Elding C, Baskett P, Hughes A. The study of the effectiveness of chest compressions using the CPR-plus. Resuscitation 1998; 36(3):
2015 Guidelines Summary HeartSine samaritan PAD Automated External Defibrillators
 2015 Guidelines Summary HeartSine samaritan PAD Automated External Defibrillators This document provides a summary of the 2015 guidelines and how the HeartSine samaritan PAD range of products complies
2015 Guidelines Summary HeartSine samaritan PAD Automated External Defibrillators This document provides a summary of the 2015 guidelines and how the HeartSine samaritan PAD range of products complies
ANZCOR Guideline 6 Compressions
 ANZCOR Guideline 6 Compressions Who does this guideline apply to? Summary This guideline applies to all persons who are unresponsive and not breathing normally. Who is the audience for this guideline?
ANZCOR Guideline 6 Compressions Who does this guideline apply to? Summary This guideline applies to all persons who are unresponsive and not breathing normally. Who is the audience for this guideline?
Guidelines 2005 for Basic Life Support
 Guidelines 2005 for Basic Life Support Anthony J Handley MD FRCP Chief Medical Adviser RLSS UK Honorary Medical Adviser ILSE Honorary Secretary, Medical Committee ILS Honorary Consultant Physician & Cardiologist,
Guidelines 2005 for Basic Life Support Anthony J Handley MD FRCP Chief Medical Adviser RLSS UK Honorary Medical Adviser ILSE Honorary Secretary, Medical Committee ILS Honorary Consultant Physician & Cardiologist,
An Appropriate Compression Pace is Important for Securing the Quality of Hands-only CPR - A manikin study
 Hiroshima J. Med. Sci. Vol. 63, No. 1-3, 7~11, September, 2014 HIJM 63 2 7 An Appropriate Compression Pace is Important for Securing the Quality of Hands-only CPR - A manikin study Yoshitaka SHIMIZU 1,*),
Hiroshima J. Med. Sci. Vol. 63, No. 1-3, 7~11, September, 2014 HIJM 63 2 7 An Appropriate Compression Pace is Important for Securing the Quality of Hands-only CPR - A manikin study Yoshitaka SHIMIZU 1,*),
Basic life support updates
 Basic life support 2010 updates Chest compressions. Airway, Breathing (C-A-B) science indicates the following order: 1. Check the patient for responsiveness and breathing. 2. Call for help and get the
Basic life support 2010 updates Chest compressions. Airway, Breathing (C-A-B) science indicates the following order: 1. Check the patient for responsiveness and breathing. 2. Call for help and get the
Peter J. Kudenchuk, MD University of Washington
 Peter J. Kudenchuk, MD University of Washington CPR-The Science Behind the Hands A/Prof Marcus Ong Senior Consultant, Clinician Scientist & Director of Research Department of Emergency Medicine Singapore
Peter J. Kudenchuk, MD University of Washington CPR-The Science Behind the Hands A/Prof Marcus Ong Senior Consultant, Clinician Scientist & Director of Research Department of Emergency Medicine Singapore
High Quality CPR: Demonstration and Analysis. Conflict of Interest (COI)
 High Quality CPR: Demonstration and Analysis Ankur Doshi, MD, Emergency Medicine, University of Pittsburgh Mark Pinchalk, MS, EMT-P, Patient Care Coordinator, Pittsburgh EMS Robin Roberts, Sr. Account
High Quality CPR: Demonstration and Analysis Ankur Doshi, MD, Emergency Medicine, University of Pittsburgh Mark Pinchalk, MS, EMT-P, Patient Care Coordinator, Pittsburgh EMS Robin Roberts, Sr. Account
The Concept of Q-CPR. The need for Quality CPR
 The need for Quality CPR Push hard, push fast, allow full chest recoil after each compression, and minimise interruptions in chest compressions. 1 Victims of cardiac arrest need immediate CPR. This provides
The need for Quality CPR Push hard, push fast, allow full chest recoil after each compression, and minimise interruptions in chest compressions. 1 Victims of cardiac arrest need immediate CPR. This provides
Academic Grant CPR process monitors provided by Zoll. conflict of interest to declare
 Comparison of Bystander Fatigue and CPR Quality when Using Ui Continuous Chest Compressions Versus 30:2 Compressions to Ventilations: A Randomized Cross over over Trial CAEP Niagara Falls 2012 CAEP St
Comparison of Bystander Fatigue and CPR Quality when Using Ui Continuous Chest Compressions Versus 30:2 Compressions to Ventilations: A Randomized Cross over over Trial CAEP Niagara Falls 2012 CAEP St
EVIDENCE-BASED RESEARCH. Rescuer Fatigue in Cardiopulmonary Resuscitation: A Review of the Literature
 ISSN 1447-4999 EVIDENCE-BASED RESEARCH Rescuer Fatigue in Cardiopulmonary Resuscitation: A Review of the Literature Hendrik Gutwirth BAppSc (Exercise and Sport Science), BAppSc (Sport Science -Tennis),
ISSN 1447-4999 EVIDENCE-BASED RESEARCH Rescuer Fatigue in Cardiopulmonary Resuscitation: A Review of the Literature Hendrik Gutwirth BAppSc (Exercise and Sport Science), BAppSc (Sport Science -Tennis),
2005 Top Ten Major Changes in Treatment Recommendations *
 2005 Top Ten Major Changes in Treatment Recommendations * This document reviews the top ten new treatment recommendations and guidelines for ASHI s basic life support training programs for professional
2005 Top Ten Major Changes in Treatment Recommendations * This document reviews the top ten new treatment recommendations and guidelines for ASHI s basic life support training programs for professional
 Introduction Welcome to COMPREHENSIVE BASIC LIFE SUPPORT Course. BLS is the foundation for saving lives after cardiac arrest. You will learn the skills of highquality cardiopulmonary resuscitation (CPR)
Introduction Welcome to COMPREHENSIVE BASIC LIFE SUPPORT Course. BLS is the foundation for saving lives after cardiac arrest. You will learn the skills of highquality cardiopulmonary resuscitation (CPR)
This presentation should be viewed in its entirety by rescuers being trained for the first time on LUCAS.
 EXCLUSIVELY DISTRIBUTED BY 1 Orientation Guide 2 Refer to the Instructions for Use for complete directions for use, indications, contraindications, warnings, precautions, and potential adverse events.
EXCLUSIVELY DISTRIBUTED BY 1 Orientation Guide 2 Refer to the Instructions for Use for complete directions for use, indications, contraindications, warnings, precautions, and potential adverse events.
Q-CPR Measurement and Feedback Application Note
 Q-CPR Measurement and Feedback Application Note Introduction Consider the following: Research demonstrates that the quality of cardiopulmonary resuscitation (CPR) has a direct effect on survival rate and
Q-CPR Measurement and Feedback Application Note Introduction Consider the following: Research demonstrates that the quality of cardiopulmonary resuscitation (CPR) has a direct effect on survival rate and
The prevalence and magnitude of common CPR problems, their probable root causes, and strategies for the reduction or elimination of these problems
 The prevalence and magnitude of common CPR problems, their probable root causes, and strategies for the reduction or elimination of these problems Robert H Trenkamp Private practice, Hasleiters Retreat,
The prevalence and magnitude of common CPR problems, their probable root causes, and strategies for the reduction or elimination of these problems Robert H Trenkamp Private practice, Hasleiters Retreat,
EMD CPR. The First First Responder. R. Darrell Nelson, MD, FACEP
 EMD CPR The First First Responder R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Baptist Health Medical Director, Davie and Stokes County EMS Assistant Medical Director, Forsyth
EMD CPR The First First Responder R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Baptist Health Medical Director, Davie and Stokes County EMS Assistant Medical Director, Forsyth
UTSW/BioTel EMS System Training Bulletin June 1, 2015 EMS TB Adult CPR Update: Change to Continuous Chest Compressions (CCC)
 UTSW/BioTel EMS System Training Bulletin June 1, 2015 EMS TB 15-005 Adult CPR Update: Change to Continuous Chest Compressions (CCC) 06/01/2015 FINAL-BioTel 1 Purpose To set forth updated ADULT CPR practice
UTSW/BioTel EMS System Training Bulletin June 1, 2015 EMS TB 15-005 Adult CPR Update: Change to Continuous Chest Compressions (CCC) 06/01/2015 FINAL-BioTel 1 Purpose To set forth updated ADULT CPR practice
Once student shouts for help, instructor says, Here s the barrier device. I am going to get the AED. STOP TEST
 Adult CPR and AED Adult Skills CPR Testing and Checklist AED Skills Testing Checklist Student Name Date of Test Hospital Scenario: You are working in a hospital or clinic, and you see a person who has
Adult CPR and AED Adult Skills CPR Testing and Checklist AED Skills Testing Checklist Student Name Date of Test Hospital Scenario: You are working in a hospital or clinic, and you see a person who has
Rescuer Fatigue: Standard versus Continuous Chest-Compression Cardiopulmonary Resuscitation
 Rescuer Fatigue: Standard versus Continuous Chest-Compression Cardiopulmonary Resuscitation Joseph W. Heidenreich, MD, Robert A. Berg, MD, Travis A. Higdon, MD, Gordon A. Ewy, MD, Karl B. Kern, MD, Arthur
Rescuer Fatigue: Standard versus Continuous Chest-Compression Cardiopulmonary Resuscitation Joseph W. Heidenreich, MD, Robert A. Berg, MD, Travis A. Higdon, MD, Gordon A. Ewy, MD, Karl B. Kern, MD, Arthur
CPR Quality During OHCA Transport
 CPR Quality During OHCA Transport Sheldon Cheskes, MD CCFP(EM) FCFP Medical Director, Sunnybrook Centre for Prehospital Medicine Associate Professor, Division of Emergency Medicine, University of Toronto
CPR Quality During OHCA Transport Sheldon Cheskes, MD CCFP(EM) FCFP Medical Director, Sunnybrook Centre for Prehospital Medicine Associate Professor, Division of Emergency Medicine, University of Toronto
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pre course Review Materials Revised Huntsville Hospital Training Center Disclaimer: This document is solely produced by Huntsville
American Heart Association Basic Life Support for Healthcare Providers Pre course Review Materials Revised Huntsville Hospital Training Center Disclaimer: This document is solely produced by Huntsville
Resuscitation 81 (2010) Contents lists available at ScienceDirect. Resuscitation. journal homepage:
 Resuscitation 81 (2010) 53 58 Contents lists available at ScienceDirect Resuscitation journal homepage: www.elsevier.com/locate/resuscitation Simulation and education New visual feedback device improves
Resuscitation 81 (2010) 53 58 Contents lists available at ScienceDirect Resuscitation journal homepage: www.elsevier.com/locate/resuscitation Simulation and education New visual feedback device improves
BLS Guideline 3 COMPRESSIONS
 Australian Resuscitation Advisory Network BLS Guideline 3 COMPRESSIONS Scope Who does this guideline apply to? This guideline applies to all persons are unresponsive to pain and present with absent or
Australian Resuscitation Advisory Network BLS Guideline 3 COMPRESSIONS Scope Who does this guideline apply to? This guideline applies to all persons are unresponsive to pain and present with absent or
BLS. Compressions Airway Breaths. Basic Life Support Quick Reference. Critical Concepts
 BLS Basic Life Support Quick Reference C-A-B Compressions Airway Breaths Critical Concepts High-quality CPR improves a victim s chances of survival. The critical characteristics of high-quality CPR include
BLS Basic Life Support Quick Reference C-A-B Compressions Airway Breaths Critical Concepts High-quality CPR improves a victim s chances of survival. The critical characteristics of high-quality CPR include
High-Functioning EMS CPR Teams. Sally A Taylor - Paramedic Atlantic Partners EMS
 High-Functioning EMS CPR Teams Cardiac Arrest Management Sally A Taylor - Paramedic Atlantic Partners EMS Insanity: Doing the same thing over and over and expecting a different result. John Dryden The
High-Functioning EMS CPR Teams Cardiac Arrest Management Sally A Taylor - Paramedic Atlantic Partners EMS Insanity: Doing the same thing over and over and expecting a different result. John Dryden The
Enhancing 4 th chain: Mechanical chest compression during transportation
 How to Implement New Resuscitation Guidelines Enhancing 4 th chain: Mechanical chest compression during transportation 한림대의료원강동성심병원응급의학과조영석 Contents The Present of Mechanical CPR Device Barriers of High
How to Implement New Resuscitation Guidelines Enhancing 4 th chain: Mechanical chest compression during transportation 한림대의료원강동성심병원응급의학과조영석 Contents The Present of Mechanical CPR Device Barriers of High
12/03/2013. Conflict of interest. ERC 2010 Guidelines. Waar is nog winst te behalen in het reanimatieonderwijs?
 Conflict of interest Waar is nog winst te behalen in het reanimatieonderwijs? Unrestricted research grant from the Laerdal Foundation Nicolas MPOTOS Emergency Department, Ghent University Hospital, Belgium
Conflict of interest Waar is nog winst te behalen in het reanimatieonderwijs? Unrestricted research grant from the Laerdal Foundation Nicolas MPOTOS Emergency Department, Ghent University Hospital, Belgium
CPR: Are You a Machine or Do You Need One?
 CPR: Are You a Machine or Do You Need One? Outline Mechanical CPR update Are you a machine? Measuring performance ED/hospital challenges When mechanical CPR could make a difference New Guidelines The evidence
CPR: Are You a Machine or Do You Need One? Outline Mechanical CPR update Are you a machine? Measuring performance ED/hospital challenges When mechanical CPR could make a difference New Guidelines The evidence
Update on chest compressions
 Update on chest compressions Georg M Schmölzer Centre for the Studies of Asphyxia and Resuscitation, Royal Alexandra Hospital, Edmonton, Canada; Dept. of Pediatrics, University of Alberta, Edmonton, Canada
Update on chest compressions Georg M Schmölzer Centre for the Studies of Asphyxia and Resuscitation, Royal Alexandra Hospital, Edmonton, Canada; Dept. of Pediatrics, University of Alberta, Edmonton, Canada
American Heart Association Health Care Provider CPR 2010 Curriculum
 American Heart Association Health Care Provider CPR 2010 Curriculum 1 CPR Overview Compressions are most important part of CPR Push hard and fast Minimize interruptions CAB Assessment Circulation Airway
American Heart Association Health Care Provider CPR 2010 Curriculum 1 CPR Overview Compressions are most important part of CPR Push hard and fast Minimize interruptions CAB Assessment Circulation Airway
Resuscitation Council of Southern Africa
 Resuscitation Council of Southern Africa 72 Sophia Street, Fairland, 2170, Johannesburg, South Africa Tel: 011-478-3989 Fax: 011-678-5087 www.resuscitationcouncil.co.za 30 November 2009 PLEA TO THE SOUTH
Resuscitation Council of Southern Africa 72 Sophia Street, Fairland, 2170, Johannesburg, South Africa Tel: 011-478-3989 Fax: 011-678-5087 www.resuscitationcouncil.co.za 30 November 2009 PLEA TO THE SOUTH
Guide to Compression-only Bystander CPR
 Guide to Compression-only Bystander CPR The Value of CPR During a cardiac arrest, CardioPulmonary Resuscitation (CPR) is important because it is the best treatment until the arrival of a Defibrillator,
Guide to Compression-only Bystander CPR The Value of CPR During a cardiac arrest, CardioPulmonary Resuscitation (CPR) is important because it is the best treatment until the arrival of a Defibrillator,
Basic Life Support Adult
 1/3.4.1 Version 4, 03/2016 Basic Life Support Adult CFR - A EFR Collapse Initiate mobilisation of 3 to 4 practitioners / responders Unresponsive and breathing abnormally or gasping 112 / 999 Go to Primary
1/3.4.1 Version 4, 03/2016 Basic Life Support Adult CFR - A EFR Collapse Initiate mobilisation of 3 to 4 practitioners / responders Unresponsive and breathing abnormally or gasping 112 / 999 Go to Primary
What is the Role of Chest Compression Depth during Out-of-Hospital CPR?
 Resuscitation Outcomes Consortium What is the Role of Chest Compression Depth during Out-of-Hospital CPR? Ian Stiell for The ROC Investigators Co-Authors Ian Stiell University of Ottawa Siobhan Everson-Stewart
Resuscitation Outcomes Consortium What is the Role of Chest Compression Depth during Out-of-Hospital CPR? Ian Stiell for The ROC Investigators Co-Authors Ian Stiell University of Ottawa Siobhan Everson-Stewart
MANAGEMENT OF COLLAPSED ADULT PATIENT
 MANAGEMENT OF COLLAPSED ADULT PATIENT Author Information Dr. Venugopalan P.P. Chief Emergency Medicine Dy Director, MIMS Academy Malabar Institute of Medical Sciences Ltd. P.O. Govindapuram, Calicut, Kerala
MANAGEMENT OF COLLAPSED ADULT PATIENT Author Information Dr. Venugopalan P.P. Chief Emergency Medicine Dy Director, MIMS Academy Malabar Institute of Medical Sciences Ltd. P.O. Govindapuram, Calicut, Kerala
COMMUNITY SAFETY CONSULTANTS AHA CPR COURSE RECORD SHEET
 Revised 5-31-2018 CSC COURSE #: COMMUNTY SAFETY CONSULTANTS AHA CPR COURSE RECORD SHEET Organization: Address: ZP: Date: Start Time: End Time: Total Hours: Total Days: # of nitial students: # of Renewal
Revised 5-31-2018 CSC COURSE #: COMMUNTY SAFETY CONSULTANTS AHA CPR COURSE RECORD SHEET Organization: Address: ZP: Date: Start Time: End Time: Total Hours: Total Days: # of nitial students: # of Renewal
bls guidelines B42EFDD89A9AB6A33D869587D2D61D4E Bls Guidelines 1 / 6
 Bls Guidelines 1 / 6 2 / 6 3 / 6 Bls Guidelines Welcome to the Basic Life Support (BLS) algorithms and training by United Medical Education. Here we will discuss basic life saving interventions for patients
Bls Guidelines 1 / 6 2 / 6 3 / 6 Bls Guidelines Welcome to the Basic Life Support (BLS) algorithms and training by United Medical Education. Here we will discuss basic life saving interventions for patients
The Positive Effect of Negative Pressure
 The Positive Effect of Negative Pressure (Future Direction in Resuscitative Care) Brent Parquette, NRP Lucas County EMS, Toledo, OH Toledo, Ohio Lucas County EMS (Toledo, OH) Primary service area: 340
The Positive Effect of Negative Pressure (Future Direction in Resuscitative Care) Brent Parquette, NRP Lucas County EMS, Toledo, OH Toledo, Ohio Lucas County EMS (Toledo, OH) Primary service area: 340
On-Scene Resuscitation. Brent Myers, MD MPH Director Medical Director Wake County EMS, Raleigh, NC
 L MODULE 7 On-Scene Resuscitation Brent Myers, MD MPH Director Medical Director Wake County EMS, Raleigh, NC Plan For Discussion: Rationale for EMS Providers On-Scene Resuscitation Choreography Check lists
L MODULE 7 On-Scene Resuscitation Brent Myers, MD MPH Director Medical Director Wake County EMS, Raleigh, NC Plan For Discussion: Rationale for EMS Providers On-Scene Resuscitation Choreography Check lists
Introduction. Methods
 Elmer Original Article ress Efficacy of Feed Forward and Feedback Signaling for Inflations and Chest Compression Pressure During Cardiopulmonary Resuscitation in a Newborn Mannequin Peter Andriessen a,
Elmer Original Article ress Efficacy of Feed Forward and Feedback Signaling for Inflations and Chest Compression Pressure During Cardiopulmonary Resuscitation in a Newborn Mannequin Peter Andriessen a,
Other diseases or age process
 1 BLS For Healthcare Providers 2 Time is Critical! begins to die in 4 to 6 minutes Brain matter cannot regenerate itself In order to sustain life, the human body must have going in and out and must be
1 BLS For Healthcare Providers 2 Time is Critical! begins to die in 4 to 6 minutes Brain matter cannot regenerate itself In order to sustain life, the human body must have going in and out and must be
B-CARD NO PAUSE SHOULD BE YOUR CAUSE
 B-CARD NO PAUSE SHOULD BE YOUR CAUSE SIMEU Congress, 17-20 November, Symposium Georges Bousignac 1 Cardiac arrest: A new cutting edge treatment method by Dr. Boussignac No Pause Should Be Your Cause 2
B-CARD NO PAUSE SHOULD BE YOUR CAUSE SIMEU Congress, 17-20 November, Symposium Georges Bousignac 1 Cardiac arrest: A new cutting edge treatment method by Dr. Boussignac No Pause Should Be Your Cause 2
E C C. American Heart Association. Basic Life Support for Healthcare Providers. Written Examinations. March 2011
 E C C American Heart Association Basic Life Support for Healthcare Providers Written Examinations Contents: Examination Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference
E C C American Heart Association Basic Life Support for Healthcare Providers Written Examinations Contents: Examination Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference
AutoPulse. Mechanical CPR. in the Hospital
 AutoPulse Mechanical CPR in the Hospital When Do You Need Mechanical CPR? Justifying the use of mechanical CPR in the pre-hospital setting where the number of rescuers is limited and patients must be
AutoPulse Mechanical CPR in the Hospital When Do You Need Mechanical CPR? Justifying the use of mechanical CPR in the pre-hospital setting where the number of rescuers is limited and patients must be
McHENRY WESTERN LAKE COUNTY EMS SYSTEM FALL 2014 CONTINUING EDUCATION MANDATORY FOR ALL PRIMARY AND PROBATIONARY ALS SYSTEM PROVIDERS.
 McHENRY WESTERN LAKE COUNTY EMS SYSTEM FALL 2014 CONTINUING EDUCATION MANDATORY FOR ALL PRIMARY AND PROBATIONARY ALS SYSTEM PROVIDERS ResQPOD In a cardiac arrest blood flow to the organs stop. Key to survival
McHENRY WESTERN LAKE COUNTY EMS SYSTEM FALL 2014 CONTINUING EDUCATION MANDATORY FOR ALL PRIMARY AND PROBATIONARY ALS SYSTEM PROVIDERS ResQPOD In a cardiac arrest blood flow to the organs stop. Key to survival
2. Women may experience others signs/symptoms in addition to the common ones. What are the additional symptoms?
 Name: Sports Medicine II Date: Block 3A Caring for Cardiac Emergencies CPR/AED for the Professional Rescuer Notes Questions/Main Ideas Notetaking Column 1. Name some signs and symptoms of a heart attack.
Name: Sports Medicine II Date: Block 3A Caring for Cardiac Emergencies CPR/AED for the Professional Rescuer Notes Questions/Main Ideas Notetaking Column 1. Name some signs and symptoms of a heart attack.
AMERICAN HEART ASSOCIATION UPDATES:
 INTRODUCTION TO CPR AMERICAN HEART ASSOCIATION UPDATES: October 18, 2010 If a bystander is not trained in CPR, the bystander should provide compression-only CPR (see below) for the adult victim who suddenly
INTRODUCTION TO CPR AMERICAN HEART ASSOCIATION UPDATES: October 18, 2010 If a bystander is not trained in CPR, the bystander should provide compression-only CPR (see below) for the adult victim who suddenly
THE SYSTEM FOR HIGH-QUALITY CPR
 AutoPulse THE SYSTEM FOR HIGH-QUALITY CPR RESUSCITATION ON THE MOVE Since we had the AutoPulse, we could carry the patient down three flights of stairs while continuing chest compressions. He survived,
AutoPulse THE SYSTEM FOR HIGH-QUALITY CPR RESUSCITATION ON THE MOVE Since we had the AutoPulse, we could carry the patient down three flights of stairs while continuing chest compressions. He survived,
EMD CPR. The First First Responder. R. Darrell Nelson, MD, FACEP. Emergency Medicine Wake Forest University Baptist Health
 EMD CPR The First First Responder R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Baptist Health The First, First Responder Objectives 1. Why does EMD matter? 2. Review Role of EMD
EMD CPR The First First Responder R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Baptist Health The First, First Responder Objectives 1. Why does EMD matter? 2. Review Role of EMD
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
How to Perform CPR. The CABs of CPR are Circulation, Airway and Breathing. C - Circulation (Chest Compressions)
 How to Perform CPR Learning how to perform cardio-pulmonary resuscitation (CPR) saves lives. While no statistics are available on the exact number of lives sudden cardiac arrest claims per year, approximately
How to Perform CPR Learning how to perform cardio-pulmonary resuscitation (CPR) saves lives. While no statistics are available on the exact number of lives sudden cardiac arrest claims per year, approximately
Basic Life Support. Based on UK Resuscitation Guidelines (2010)
 Basic Life Support Based on UK Resuscitation Guidelines (2010) Clinical Skills and Simulation Team With acknowledgements also to Basic Life Support Faculty - SoNMS PowerPoint content last updated 26/05/2015
Basic Life Support Based on UK Resuscitation Guidelines (2010) Clinical Skills and Simulation Team With acknowledgements also to Basic Life Support Faculty - SoNMS PowerPoint content last updated 26/05/2015
B.L.S احیای پایھ کودکان American Heart Association
 B.L.S احیای پایھ 2010 American Heart Association کودکان زنجیره حیاتی کودکان 1.prevention, 2.early CPR, 3.prompt access to the emergency response system, 4.rapid PALS, 5. integrated post cardiac arrest
B.L.S احیای پایھ 2010 American Heart Association کودکان زنجیره حیاتی کودکان 1.prevention, 2.early CPR, 3.prompt access to the emergency response system, 4.rapid PALS, 5. integrated post cardiac arrest
Training Presentation. TFD-EMS Ver. 1 09/15
 Training Presentation TFD-EMS Ver. 1 09/15 Agenda ResQCPR System: Definition and Labeling IPR Therapy Physiology of Conventional CPR ResQPOD ITD 16 and Instructions for Use ResQPUMP ACD-CPR Device and
Training Presentation TFD-EMS Ver. 1 09/15 Agenda ResQCPR System: Definition and Labeling IPR Therapy Physiology of Conventional CPR ResQPOD ITD 16 and Instructions for Use ResQPUMP ACD-CPR Device and
Influence of rescuer strength and shift cycle time on chest compression quality
 SIGNA VITAE 2017; 13(1): 70-74 Influence of rescuer strength and shift cycle time on chest compression quality HYUNJONG KIM 1, JE SUNG YOU 2, SUNG PHIL CHUNG 2 1 Department of Emergency Medicine, Inje
SIGNA VITAE 2017; 13(1): 70-74 Influence of rescuer strength and shift cycle time on chest compression quality HYUNJONG KIM 1, JE SUNG YOU 2, SUNG PHIL CHUNG 2 1 Department of Emergency Medicine, Inje
Supplement Study Guide for. Basic Life Support (BLS) for Healthcare Providers
 for Basic Life Support (BLS) for Healthcare Providers Table of Contents Objectives... 3 One Rescuer Adult CPR Sequence... 4 One Rescuer Child CPR Sequence (1 year to Puberty)... Error! Bookmark not defined.
for Basic Life Support (BLS) for Healthcare Providers Table of Contents Objectives... 3 One Rescuer Adult CPR Sequence... 4 One Rescuer Child CPR Sequence (1 year to Puberty)... Error! Bookmark not defined.
COALINGA STATE HOSPITAL. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
Canadian Red Cross Summary First Aid Technical Changes for 2011 Implementation
 Canadian Red Cross Summary First Aid Technical Changes for 2011 Implementation Wound Care Second part of a SFA course On the first day and included in EFA To meet legislative requirements Assessment and
Canadian Red Cross Summary First Aid Technical Changes for 2011 Implementation Wound Care Second part of a SFA course On the first day and included in EFA To meet legislative requirements Assessment and
Ain't Nobody Got Time for That Epi, Fool: ACLS in the 20-Teens Comes of Age Disclosures Updated Syllabus
 Ain't Nobody Got Time for That Epi, Fool: ACLS in the 20-Teens Comes of Age JASON PERSOFF, MD, SFHM UNIVERSITY OF COLORADO HOSPITAL MEDICINE GROUP Disclosures Nothing to disclose Will present topics that
Ain't Nobody Got Time for That Epi, Fool: ACLS in the 20-Teens Comes of Age JASON PERSOFF, MD, SFHM UNIVERSITY OF COLORADO HOSPITAL MEDICINE GROUP Disclosures Nothing to disclose Will present topics that
2016 EFR CPR & AED Instructor Guide Errata Revision to 12/11 EFR CPR & AED English Instructor Guide (product #79215, English, Vision 1.
 2016 EFR CPR & AED Instructor Guide Errata Revision to 12/11 EFR CPR & AED English Instructor Guide (product #79215, English, Vision 1.0) Cover and inside cover, bottom of page, change version and copyright
2016 EFR CPR & AED Instructor Guide Errata Revision to 12/11 EFR CPR & AED English Instructor Guide (product #79215, English, Vision 1.0) Cover and inside cover, bottom of page, change version and copyright
Association of arterial blood pressure and CPR quality in a child using three different compression techniques, a case report
 Sainio et al. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine 2013, 21:51 CASE REPORT Open Access Association of arterial blood pressure and CPR quality in a child using three different
Sainio et al. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine 2013, 21:51 CASE REPORT Open Access Association of arterial blood pressure and CPR quality in a child using three different
https://youtu.be/5r7havfzxek
 CPR https://youtu.be/5r7havfzxek CPR Saves Lives Cardiopulmonary Resuscitation or CPR and defibrillation within 3-5 minutes can save over 50% of cardiac arrest victims CPR followed by AED saves thousands
CPR https://youtu.be/5r7havfzxek CPR Saves Lives Cardiopulmonary Resuscitation or CPR and defibrillation within 3-5 minutes can save over 50% of cardiac arrest victims CPR followed by AED saves thousands
AED Plus AL The Best Support For Rescuers
 AED Plus AL-80166 The Best Support For Rescuers AL-80166 CPR Required The latest American Heart Association (AHA) Guidelines issued in 2010, are clear: successful defibrillation requires high-quality CPR
AED Plus AL-80166 The Best Support For Rescuers AL-80166 CPR Required The latest American Heart Association (AHA) Guidelines issued in 2010, are clear: successful defibrillation requires high-quality CPR
Frequently Asked Questions About AEDs updated 11/2/2015
 Frequently Asked Questions About AEDs updated 11/2/2015 What does AED stand for? AED stands for automated external defibrillator. What s an AED? An AED is a device used to administer an electric shock
Frequently Asked Questions About AEDs updated 11/2/2015 What does AED stand for? AED stands for automated external defibrillator. What s an AED? An AED is a device used to administer an electric shock
University of Warwick institutional repository:
 University of Warwick institutional repository: http://go.warwick.ac.uk/wrap This paper is made available online in accordance with publisher policies. Please scroll down to view the document itself. Please
University of Warwick institutional repository: http://go.warwick.ac.uk/wrap This paper is made available online in accordance with publisher policies. Please scroll down to view the document itself. Please
Hot Topics in Telephone CPR
 Hot Topics in Telephone CPR Bentley J. Bobrow, MD, FACEP Professor, Emergency Medicine Maricopa Medical Center University of Arizona College of Medicine-Phoenix Disclosure PI Arizona HeartRescue Project
Hot Topics in Telephone CPR Bentley J. Bobrow, MD, FACEP Professor, Emergency Medicine Maricopa Medical Center University of Arizona College of Medicine-Phoenix Disclosure PI Arizona HeartRescue Project
community (out -of -hospital); thus, the success of the the willingness to perform CPR and decrease the fear of imperfect CPR performance.
 Review Article Singapore Med J 2011; 52(8) 538 CME Article Basic Cardiac Life Support: 2011 Singapore guidelines Lim S H Department of Emergency Medicine, Singapore General Hospital, Outram Road, Singapore
Review Article Singapore Med J 2011; 52(8) 538 CME Article Basic Cardiac Life Support: 2011 Singapore guidelines Lim S H Department of Emergency Medicine, Singapore General Hospital, Outram Road, Singapore
CPR + AED Topic 6 TECS TECS FIRE & SAFETY TRAINING PTE LTD
 CPR + AED Topic 6 1 Anatomy and physiology of the circulatory system 2 Principles of Resuscitation Principles of resuscitation / Determine if CPR is necessary by examining casualty, which include the following:
CPR + AED Topic 6 1 Anatomy and physiology of the circulatory system 2 Principles of Resuscitation Principles of resuscitation / Determine if CPR is necessary by examining casualty, which include the following:
Cardiac Arrest General
 Date: November 15, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not
Date: November 15, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not
Evaluation System for Chest Compression Training Shinnosuke-kun
 NEW AREAS Evaluation System for Chest Compression Training Shinnosuke-kun Youta KOKUBO*, Ichinosuke MAEDA, Shingo HIBINO and Kouichirou MINAMI ----------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------
NEW AREAS Evaluation System for Chest Compression Training Shinnosuke-kun Youta KOKUBO*, Ichinosuke MAEDA, Shingo HIBINO and Kouichirou MINAMI ----------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------
Basic Life Support (BLS) for the Healthcare Provider
 Essential Medical Training, LLC Providing Quality, Professional Training Basic Life Support (BLS) for the Healthcare Provider Course Study Guide and Agenda 772-781-9249 office 772-382-0607 fax Email: treasurecoastcpr@gmail.com
Essential Medical Training, LLC Providing Quality, Professional Training Basic Life Support (BLS) for the Healthcare Provider Course Study Guide and Agenda 772-781-9249 office 772-382-0607 fax Email: treasurecoastcpr@gmail.com
Save a life CPR Practice. CPR and AED practice for general public
 Save a life CPR Practice CPR and AED practice for general public Connect with the number 92% 25% 1% Percentage of people know how to do CPR in Chinese public Percentage of people know how to do CPR in
Save a life CPR Practice CPR and AED practice for general public Connect with the number 92% 25% 1% Percentage of people know how to do CPR in Chinese public Percentage of people know how to do CPR in
Once student shouts for help, instructor says, Here s the barrier device. I am going to get the AED. STOP TEST
 Adult CPR and AED Adult Skills CPR Testing and Checklist AED Skills Testing Checklist Hospital Scenario: You are working in a hospital or clinic, and you see a person who has suddenly collapsed in the
Adult CPR and AED Adult Skills CPR Testing and Checklist AED Skills Testing Checklist Hospital Scenario: You are working in a hospital or clinic, and you see a person who has suddenly collapsed in the
Optimal chest compression technique for paediatric cardiac arrest victims
 Kim et al. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine (2015) 23:36 DOI 10.1186/s13049-015-0118-y ORIGINAL RESEARCH Open Access Optimal chest compression technique for paediatric
Kim et al. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine (2015) 23:36 DOI 10.1186/s13049-015-0118-y ORIGINAL RESEARCH Open Access Optimal chest compression technique for paediatric
Training BULLETIN A Training and Education Update for PADI Members Worldwide
 Training BULLETIN A Training and Education Update for PADI Members Worldwide FIRST QUARTER 2011 Product No. 01220 In This Issue... Dive Theory Online Link to Divemaster 2 Referral Form Notice 2 EANx RDP
Training BULLETIN A Training and Education Update for PADI Members Worldwide FIRST QUARTER 2011 Product No. 01220 In This Issue... Dive Theory Online Link to Divemaster 2 Referral Form Notice 2 EANx RDP
High Performance CPR. Offline Reading Download as PDF. Welcome. Introduction. Physiology of CPR. High Performance CPR. Positioning.
 High Performance CPR Acknowledgement This training package was created by Crystal Harris, Clare Collihole, Joseph Schar, and Jordan Pring. Please direct any questions to your CSO or Team Leader. Offline
High Performance CPR Acknowledgement This training package was created by Crystal Harris, Clare Collihole, Joseph Schar, and Jordan Pring. Please direct any questions to your CSO or Team Leader. Offline
Adult, Child and Infant Exam
 CPR Pro for the Professional Rescuer Adult, Child and Infant Exam Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer sheet provided.
CPR Pro for the Professional Rescuer Adult, Child and Infant Exam Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer sheet provided.
SmartMan Code User Manual Section 5.0 Results
 SmartMan Code User Manual Section 5.0 Results For SmartMan Code, Megacode and Megacode Low Volume Table of Contents SmartMan Code User Manual Section 5.0 Results... 1 SMARTMAN CODE MEGACODE MEGACODE LOW
SmartMan Code User Manual Section 5.0 Results For SmartMan Code, Megacode and Megacode Low Volume Table of Contents SmartMan Code User Manual Section 5.0 Results... 1 SMARTMAN CODE MEGACODE MEGACODE LOW
CPR Professional Skills Notes
 CPR Professional Skills Notes CPR = Cardiopulmonary Resuscitation AED = Automated external defibrillator (vs. manual defibrillator in a hospital) ERS = Emergency Response System BLS = Basic Life Support
CPR Professional Skills Notes CPR = Cardiopulmonary Resuscitation AED = Automated external defibrillator (vs. manual defibrillator in a hospital) ERS = Emergency Response System BLS = Basic Life Support
How might GRADE work for ILCOR? Summary of specific components of GRADE using example worksheet
 1 How might GRADE work for ILCOR? Summary of specific components of GRADE using example worksheet Associate Professor Peter Morley Director Medical Education Royal Melbourne Hospital University of Melbourne
1 How might GRADE work for ILCOR? Summary of specific components of GRADE using example worksheet Associate Professor Peter Morley Director Medical Education Royal Melbourne Hospital University of Melbourne
Bystander s bravery and action can rescue a life of victims. Guideline Training Course
 Guideline 2005 Training Course What can we do for him/her? Sudden Cardiac Arrest (SCA) Recent studies indicate that nearly 20,000 30,000 people each year die of SCA in Japan. (250,000 people in USA) Immediate
Guideline 2005 Training Course What can we do for him/her? Sudden Cardiac Arrest (SCA) Recent studies indicate that nearly 20,000 30,000 people each year die of SCA in Japan. (250,000 people in USA) Immediate
Talking about teaching CPR at schools
 As told before I would like to talk about teaching CPR at schools. I checked a lot of articles about this issue and first I d like to talk about what I found and then hear what you got to say about this
As told before I would like to talk about teaching CPR at schools. I checked a lot of articles about this issue and first I d like to talk about what I found and then hear what you got to say about this
Key statistics from the National Cardiac Arrest Audit 2016/17
 Key statistics from the National Cardiac Arrest Audit 216/17 Supported by Resuscitation Council (UK) and Intensive Care National Audit & Research Centre (ICNARC) Data collection scope (NCAA Version 1.3)
Key statistics from the National Cardiac Arrest Audit 216/17 Supported by Resuscitation Council (UK) and Intensive Care National Audit & Research Centre (ICNARC) Data collection scope (NCAA Version 1.3)
AED Plus. The Best Support For Rescuers
 AED Plus The Best Support For Rescuers CPR Required The latest American Heart Association (AHA) Guidelines issued in 2010, are clear: successful defibrillation requires high-quality CPR performed at the
AED Plus The Best Support For Rescuers CPR Required The latest American Heart Association (AHA) Guidelines issued in 2010, are clear: successful defibrillation requires high-quality CPR performed at the
COMMUNITY SAFETY CONSULTANTS AHA CPR COURSE RECORD SHEET
 Revised 5-31-2018 CSC COURSE #: COMMUNITY SAFETY CONSULTANTS AHA CPR COURSE RECORD SHEET Organization: Address: ZIP: Date: Start Time: End Time: Total Hours: Total Days: # of Initial students: # of Renewal
Revised 5-31-2018 CSC COURSE #: COMMUNITY SAFETY CONSULTANTS AHA CPR COURSE RECORD SHEET Organization: Address: ZIP: Date: Start Time: End Time: Total Hours: Total Days: # of Initial students: # of Renewal
ORIGINAL ARTICLE Emergency & Critical Care Medicine INTRODUCTION
 ORIGINAL ARTICLE Emergency & Critical Care Medicine http://dx.doi.org/10.3346/jkms.2015.30.9.1347 J Korean Med Sci 2015; 30: 1347-1353 Differences in Hands-off Time According to the Position of a Second
ORIGINAL ARTICLE Emergency & Critical Care Medicine http://dx.doi.org/10.3346/jkms.2015.30.9.1347 J Korean Med Sci 2015; 30: 1347-1353 Differences in Hands-off Time According to the Position of a Second
Basic Life Support Adult
 1/2.4.1 Version 4, 03/2016 Basic Life Support Adult Collapse If physically unable to ventilate perform compression only CPR Unresponsive and breathing abnormally or gasping 112 / 999 Shout for help 112
1/2.4.1 Version 4, 03/2016 Basic Life Support Adult Collapse If physically unable to ventilate perform compression only CPR Unresponsive and breathing abnormally or gasping 112 / 999 Shout for help 112
THE AED THAT LEADS THE WAY
 THE AED THAT LEADS THE WAY ARE YOU PREPARED TO HELP IN A HEARTBEAT? It happens in a split second. A person collapses the victim of sudden cardiac arrest (SCA) and the clock starts ticking. You call for
THE AED THAT LEADS THE WAY ARE YOU PREPARED TO HELP IN A HEARTBEAT? It happens in a split second. A person collapses the victim of sudden cardiac arrest (SCA) and the clock starts ticking. You call for
Resuscitation Science
 Resuscitation Science Duration of Ventilations During Cardiopulmonary Resuscitation by Lay Rescuers and First Responders Relationship Between Delivering Chest Compressions and Outcomes Stefanie G. Beesems,
Resuscitation Science Duration of Ventilations During Cardiopulmonary Resuscitation by Lay Rescuers and First Responders Relationship Between Delivering Chest Compressions and Outcomes Stefanie G. Beesems,
Out of Hospital Arrest: How are We Doing in Lane County? By: Joshua Moore, FireFighter EMT-P Eugene Springfield Fire Department
 Out of Hospital Arrest: How are We Doing in Lane County? By: Joshua Moore, FireFighter EMT-P Eugene Springfield Fire Department Objectives: 1. State the 5 links in the AHA Chain of Survival. 2. How has
Out of Hospital Arrest: How are We Doing in Lane County? By: Joshua Moore, FireFighter EMT-P Eugene Springfield Fire Department Objectives: 1. State the 5 links in the AHA Chain of Survival. 2. How has
E C C. American Heart Association. BLS for Healthcare Providers. Written Exams. January 12, 2012
 E C C American Heart Association BLS for Healthcare Providers Written Exams Contents: Exam Memo Student Answer Sheet Version C Exam Version C Answer Key Version C Reference Sheet Version D Exam Version
E C C American Heart Association BLS for Healthcare Providers Written Exams Contents: Exam Memo Student Answer Sheet Version C Exam Version C Answer Key Version C Reference Sheet Version D Exam Version
Defibtech s Latest Advancement The Lifeline ARM Automated Chest Compression (ACC) Device for Professionals
 Defibtech s Latest Advancement The Lifeline ARM Automated Chest Compression (ACC) Device for Professionals Precise operation of the Lifeline ARM helps to ensure high-quality and continuous cardiopulmonary
Defibtech s Latest Advancement The Lifeline ARM Automated Chest Compression (ACC) Device for Professionals Precise operation of the Lifeline ARM helps to ensure high-quality and continuous cardiopulmonary
Basic Life Support (BLS)
 Basic Life Support (BLS) Basic Life Support (BLS) is the foundation for saving lives after cardiac arrest. Participant will learn the skills of high-quality cardiopulmonary resuscitation (CPR) for victims
Basic Life Support (BLS) Basic Life Support (BLS) is the foundation for saving lives after cardiac arrest. Participant will learn the skills of high-quality cardiopulmonary resuscitation (CPR) for victims
Basic Life Support & Automated External Defibrillation Course. OBJECTIVES
 OBJECTIVES Basic Life Support & Automated External Defibrillation Course www.erc.edu At the end of this course participants should be able to demonstrate: How to assess the collapsed victim. How to perform
OBJECTIVES Basic Life Support & Automated External Defibrillation Course www.erc.edu At the end of this course participants should be able to demonstrate: How to assess the collapsed victim. How to perform
Development of Android Based Chest Compression Feedback Application Using the Accelerometer in Smartphone
 Proceedings of the International Conference on Biomedical Engineering and Systems Prague, Czech Republic, August 14-15, 2014 Paper No. 130 Development of Android Based Chest Compression Feedback Application
Proceedings of the International Conference on Biomedical Engineering and Systems Prague, Czech Republic, August 14-15, 2014 Paper No. 130 Development of Android Based Chest Compression Feedback Application
CPR & ECC COURSE MATRIX
 CPR & ECC COURSE MATRIX Course Content Audience Student Materials Instructor Materials Course Completion Card Type Estimated Time (Based on 6:1 Student to Instructor Ratio) Courses for Healthcare Professionals
CPR & ECC COURSE MATRIX Course Content Audience Student Materials Instructor Materials Course Completion Card Type Estimated Time (Based on 6:1 Student to Instructor Ratio) Courses for Healthcare Professionals
Even Better Support For Rescuers
 Even Better Support For Rescuers Beyond the AED Plus In 2002, ZOLL launched the AED Plus defibrillator with Real CPR Help real-time CPR Feedback to let rescuers know, for the first time ever, when they
Even Better Support For Rescuers Beyond the AED Plus In 2002, ZOLL launched the AED Plus defibrillator with Real CPR Help real-time CPR Feedback to let rescuers know, for the first time ever, when they
Response to Basic Emergencies
 UNIT52 Response to Basic Emergencies PROCEDURE ADULT CPR, ONE RESCUER Standard precautions should be followed if at all possible. This means gloves should be worn and a barrier device used. If the victim
UNIT52 Response to Basic Emergencies PROCEDURE ADULT CPR, ONE RESCUER Standard precautions should be followed if at all possible. This means gloves should be worn and a barrier device used. If the victim
A study comparing the usability of fully automatic versus semi-automatic defibrillation by untrained nursing students
 Resuscitation 64 (2005) 41 47 A study comparing the usability of fully automatic versus semi-automatic defibrillation by untrained nursing students Koenraad G. Monsieurs a,, Catherine Vogels b, Leo L.
Resuscitation 64 (2005) 41 47 A study comparing the usability of fully automatic versus semi-automatic defibrillation by untrained nursing students Koenraad G. Monsieurs a,, Catherine Vogels b, Leo L.
Safety Institute USA HEALTH AND SAFETY
 Safety Institute USA HEALTH AND SAFETY Instructors Commonly Asked Questions on the New CPR Program: 1. Q. What is the single most significant change in the New Materials regarding the response to an unconscious
Safety Institute USA HEALTH AND SAFETY Instructors Commonly Asked Questions on the New CPR Program: 1. Q. What is the single most significant change in the New Materials regarding the response to an unconscious
