Intermittent Positive Pressure Breathing (IPPB) Guideline
|
|
|
- Blaise Dorsey
- 5 years ago
- Views:
Transcription
1 Intermittent Positive Pressure Breathing (IPPB) Guideline Full Title of Guideline: Intermittent Positive Pressure Breathing (IPPB) Guidelines for Practice Author (include and role): Regan Bushell, Senior Physiotherapist, Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date): Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis): Changes from previous version (not applicable if this is a new guideline, enter below if extensive): Clinical Support, Physiotherapy Senior Physiotherapists at NUH Trust wide physiotherapists September, 2021 Self-ventilating and tracheostomy patients with reduced lung volumes and/or retention of pulmonary secretions. Exclusion criteria includes an undrained pneumothorax and the guideline describes a number of precautions that require discussion with the medical team prior to the commencement of IPPB. Review of research, minor changes to wording, grammar and spelling errors corrected. Change of contraindication to precaution (removal of chest drain). Well designed non-experimental descriptive studies (ie comparative / correlation and case studies). Expert committee Summary of evidence base this reports or opinions and / or clinical experiences of respected guideline has been created from: authorities. Recommended best practise based on the clinical experience of the guideline developer This guideline has been registered with the trust. However, clinical guidelines are guidelines only. The interpretation and application of clinical guidelines will remain the responsibility of the individual clinician. If in doubt contact a senior colleague or expert. Caution is advised when using guidelines after the review date or outside of the Trust. Page 1 of 9
2 Intermittent Positive Pressure Breathing (IPPB) Guideline for Practice 2018 Version: This replaces the IPPB Guideline for Practice, September 2015 Review Date: September 2021 Contact: Regan Bushell, Senior Physiotherapist, or Eleanor Douglas Lecturer/Practitioner Physiotherapist. Ext: Disclaimer This guideline has been registered with the Nottingham University Hospitals Trust. However, clinical guidelines are guidelines only. The interpretation and application of clinical guidelines will remain the responsibility of the individual clinician. If in any doubt regarding this procedure, contact a senior colleague. Caution is advised when using guidelines after the review date. Please contact the named above with any comments/feedback. Introduction This guideline describes the procedure for the use of Intermittent Positive Pressure Breathing (IPPB) for the purposes of physiotherapy treatment in adult patients. IPPB is a technique used to provide short- term or intermittent mechanical ventilation for the purpose of augmenting lung expansion or assisting ventilation. IPPB uses a pressure-limited ventilator that applies a positive inspiratory pressure, which is triggered by the patient s spontaneous effort. Indications For Use IPPB has been shown to increase Tidal Volume (V T ) and Minute Ventilation (MV), therefore the rate of alveolar ventilation. This can have the effect of improving Pa0 2 levels and reducing PaC0 2. The application of the positive pressure reduces the work of breathing associated with inspiration. IPPB may be of value in the following situations: 1. To augment V T in the presence of hypoventilation due to weakness, fatigue or diminished level of consciousness. 2. Assisting secretion clearance where pathology or fatigue limits the ability to cough or ventilate effectively N.B. Used in isolation, IPPB will have no effect on functional residual capacity (FRC) Page 2 of 9
3 Precautions (Discuss with Specialist Registrar /Consultant prior to use) Un drained pneumothorax Air swallowing (particularly problematic if it occurs in anti-reflux surgery patients) Hypotension due to positive pressure reducing venous return Patient intolerance Maxfax surgery where an oral flap is used Facial fractures Unprotected brain aneurysm (Mr G Dow patients only at QMC campus) Recent oesophageal, pulmonary or anti-reflux surgery Gastric distention with no ng in situ Cardiovascular System Instability (hypotension and arrhythmias) Raised ICP Uncontrolled pain Nausea Bronchospasm Pulmonary oedema Extreme tachypnoea Large airway carcinoma Emphysematous bullae and/or evidence if intrinsic PEEP Unexplained heamoptysis Self -ventilating patients with a known hypoxic drive (if 0 2 machine is to be used) Pneumothorax and lung injury may occur in any patient with indiscriminate and uncontrolled use of IPPB Page 3 of 9
4 Guideline for Practice Action Gain consent from the patient and explain the effects of IPPB Prepare the patient by ensuring analgesia and information is given as required Position the patient according to assessment findings and treatment aims Select interface: full facemask or mouthpiece (a nose clip may be required) or via tracheostomy Assemble IPPB circuit, filling the nebuliser chamber with 5mls of sterile, normal saline. Check the saline amount and expiry date with another qualified member of staff e.g. nurse or physiotherapist Attach circuit to ventilator Connect IPPB ventilator to 0 2 gas supply. Maintain the patients current Fi0 2 where indicated until treatment is ready to commence. The O 2 IPPB ventilator will only provide approximately 40% 0 2 Switch ventilator on and demonstrate function to patient using the red manual override control on the left hand side of the ventilator Rationale Confirms the patient is willing to undertake the treatment Minimises patient discomfort, thereby maximising the effectiveness of the procedure Maximise effectiveness of procedure by optimising gas distribution To ensure appropriate patient ventilator connection and minimise air leaks Drug is given as prescribed and avoids administration errors Provides humidification to the inhaled gas To establish ventilator patient connection To establish driving gas source and maintain adequate Fi0 2 Ensures correct functioning of the ventilator. Establish absence of leaks in the circuit Provides patient reassurance Configure initial settings: Sensitivity or starting effort Inspiratory Flow Rate Inspiratory Pressure Set low to allow patient to breath in easily without increasing work of breathing Commence at mid range. Increase if patient is very breathless, then reduce as able to optimise gas distribution Commence at approximately 10 cmh 2 0 Increasing as necessary according to patient response Prevents the machine cycling automatically All other controls should be switched off Ensures the correct technique and maximises the effectiveness of the treatment Apply interface and commence treatment. Instruct the patient to initiate a breath and then allow the machine to fill their lungs with air, then to breathe out passively Use the red manual override control if the patient needs help Page 4 of 9 Ensure correct technique and maximise
5 initially to coordinate with the ventilator Monitor the patient throughout the treatment: For any signs of distress Synchrony with ventilator Thoracic expansion Cheek filling Air swallowing Abdominal distension Pulse oximetry Cardio-vascular instability Adjust the settings as required to match patient demand, progress and treatment Continue treatment for as long as required. Reduce inspiratory pressure intermittently if using over a prolonged period Add manual techniques as required If a cough is stimulated, discontinue IPPB temporarily Once the treatment has finished restore pre-treatment respiratory support Monitor the patients observations to ensure level of support is still adequate Rinse out the nebuliser chamber with sterile water and dry thoroughly Use a patient hospital label to identify the patients IPPB circuit and store in a plastic bag by the patient s bedside IPPB circuits should be changed on a weekly basis the date of commencement of the use of the circuit should be clearly marked on the hospital label Report any adverse effects or changes in patients overall condition to nursing and/or medical personnel Document procedure, effects and response as per documentation policies effectiveness of intervention Ensure patient safety including adequate Fi0 2 N.B. The BIRD will only supply 40% 0 2 Maximise effectiveness of intervention Prevent hyperventilation and hypocarbia Maximise effectiveness of treatment promotes removal of secretions Allows the patient to expectorate Re-establish respiratory support Maintains patient safety Prevents the potential for bacterial contamination Prevents cross contamination For infection control purposes Patient safety Legal requirement Best Practice Training IPPB will not be performed by physiotherapy or nursing staff who have not been trained and been deemed competent Education will be a mandatory inclusion in the in-service training programme for the Band 5 physiotherapy staff respiratory rotation Education will be offered in the emergency duty induction programme Opportunities will be offered to senior staff wishing to maintain their skills in IPPB Treatment IPPB should only be applied when clinically indicated and then proven to have been effective. All of the mechanical effects of IPPB are short lived, lasting less than an hour after treatment. The therapist must therefore aim to maximise treatment carry over by educating the patient, the carers and the multidisciplinary team. Page 5 of 9
6 Equipment List 1. Oxygen or air gas supply 2. IPPB ventilator (air or oxygen) 3. Ampoule of sterile normal saline (checked and prescribed) 4. IPPB circuit to include: a. Appropriate patient interface (facemask, mouth piece or catheter mount for tracheostomy patients) b. Connector tubing (wide bore tube and narrow bore tube) c. Complete nebuliser unit d. Exhalation valve References AARC Clinical Practice Guideline IPPB (2003) Respiratory Care 48,5: Bott J et al (2009) Guidelines for the physiotherapy management of the adult, medical, spontaneously breathing patient. Thorax 64: (Suppl 1)ii-i151 Bott J and Keilty S and Noone L (1992) IPPB A dying art? Physiotherapy 78, 9: Denehy L and Berney S (2001) The use of positive pressure devices by physiotherapists.eur Respir J 17: Page 6 of 9
7 IPPB Troubleshooting Problem Possible Solution Machine does not function Check it is switched on Check the gas supply is inserted correctly into the wall Machine cycles of its own volition The starting effort may be too low and movement triggers a flow of gas Check that the controlled expiratory time switch is off Patient is unable to trigger the machine Starting effort may be too high Inadequate seal at the interface If using a mouthpiece a nose clip may be required Machine keeps delivering a breath and Inspiratory pressure may be set too high does not stop Loss of a seal at the interface may lead to the pre-set pressure not being reached Machine seems to deliver a jerky breath / patient resists the inspiratory flow Starting effort may be too low, therefore the patient is unable to synchronise with the sudden breath Inspiratory flow rate is too high, therefore the patient is unable to synchronise with a rapid breath Poor patient technique Patient complaining of breathlessness/ difficulty breathing in or not getting enough Starting effort may be too high leading to increased work of breathing air Inspiratory flow rate may be too low, not matching the patients requirements Inspiratory pressure may be too low not matching the patients requirements Patient complaining of the machine blowing Inspiratory pressure set too high too hard Patient grimacing/ cheeks filling / active Patient may be in pain expiration (abdominals contracting) Poor technique Unsuitable ventilator settings Poor thoracic expansion despite IPPB Inspiratory pressure may be set too low (may need increasing if patient has reduced lung compliance) Inappropriate/ inadequate patient positioning Inspiratory flow needs reducing to improve gas distribution and prolong inspiratory time Patient still unable to clear secretions? VT sufficient for an effective cough? Presence of secretions? Adequate humidification/hydration? Intact cough reflex Page 7 of 9
8 APPENDIX 1 Disposable IPPB Circuit Exhalation valve Wide bore and narrow bore tubing Mouthpiece Nebuliser IPPB Ventilator On/Off switch Starting effort dial Inspiratory pressure dial Red manual over-ride control (not seen) Port for connecting IPPB circuit Inspiratory pressure gauge Controlled expiratory time (switch to off) Inspiratory flow rate dial Page 8 of 9
9 Intermittent positive pressure breathing (IPPB) Guideline
Nitrous Oxide Sedation
 Princess Margaret Hospital for Children GUIDELINE Nitrous Oxide Sedation Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children GUIDELINE Nitrous Oxide Sedation Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Basics of Mechanical Ventilation. Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity
 Basics of Mechanical Ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Overview of topics 1. Goals 2. Settings 3. Modes 4. Advantages and disadvantages
Basics of Mechanical Ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Overview of topics 1. Goals 2. Settings 3. Modes 4. Advantages and disadvantages
Clinical guideline for Ventilator Hyperinflation as a physiotherapy technique, in adult mechanically ventilated patients
 Title of Guideline Contact Name Division and Speciality Clinical guideline for Ventilator Hyperinflation as a physiotherapy technique, in adult mechanically ventilated patients Rebecca Storer (Band 7 Physiotherapist,
Title of Guideline Contact Name Division and Speciality Clinical guideline for Ventilator Hyperinflation as a physiotherapy technique, in adult mechanically ventilated patients Rebecca Storer (Band 7 Physiotherapist,
Day-to-day management of Tracheostomies & Laryngectomies
 Suctioning Suctioning the airway is an essential part of routine care of the tracheostomy and laryngectomy patient. Sputum is continually produced in health and our native airways deal with this load without
Suctioning Suctioning the airway is an essential part of routine care of the tracheostomy and laryngectomy patient. Sputum is continually produced in health and our native airways deal with this load without
Section 2.9 Decannulation
 Bite- sized training from the GTC Section 2.9 Decannulation This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative. The GTC has developed
Bite- sized training from the GTC Section 2.9 Decannulation This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative. The GTC has developed
Health Professional Info
 Health Professional Info Mouthpiece Ventilation (MPV) What is MPV? MPV is a less intrusive form of noninvasive ventilation that uses a portable home mechanical ventilator (HMV) with a single-limb open-circuit
Health Professional Info Mouthpiece Ventilation (MPV) What is MPV? MPV is a less intrusive form of noninvasive ventilation that uses a portable home mechanical ventilator (HMV) with a single-limb open-circuit
EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES
 GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
Operating Instructions for Microprocessor Controlled Ventilators
 Page 1 of 5 Operating Instructions for Microprocessor Controlled Ventilators Purpose Audience Scope Physician's Order To provide guidelines for the procedure for the use of microprocessor controlled ventilators.
Page 1 of 5 Operating Instructions for Microprocessor Controlled Ventilators Purpose Audience Scope Physician's Order To provide guidelines for the procedure for the use of microprocessor controlled ventilators.
Mechanical Ventilation
 Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
Virginia Beach EMS. Oxylator EMX. Debra H. Brennaman, RN, MPA, NREMT-P
 Virginia Beach EMS Oxylator EMX Debra H. Brennaman, RN, MPA, NREMT-P Oxylator EMX Overview Patient responsive oxygen powered resuscitation / ventilation device intended to provide emergency ventilatory
Virginia Beach EMS Oxylator EMX Debra H. Brennaman, RN, MPA, NREMT-P Oxylator EMX Overview Patient responsive oxygen powered resuscitation / ventilation device intended to provide emergency ventilatory
Mechanical Ventilation
 PROCEDURE - Page 1 of 5 Purpose Scope Physician's Order Indications Procedure Mechanical Artificial Ventilation refers to any methods to deliver volumes of gas into a patient's lungs over an extended period
PROCEDURE - Page 1 of 5 Purpose Scope Physician's Order Indications Procedure Mechanical Artificial Ventilation refers to any methods to deliver volumes of gas into a patient's lungs over an extended period
Manual: Biphasic Positive Airway Pressure (BiPAP) Ventilation
 RCH@Home Manual: Biphasic Positive Airway Pressure (BiPAP) Ventilation 1. Commonly used terms... 2 1.1 Inspiration... 2 1.2 Expiration... 2 1.3 Breath rate (bpm)... 2 1.4 Ventilation... 2 1.5 Biphasic
RCH@Home Manual: Biphasic Positive Airway Pressure (BiPAP) Ventilation 1. Commonly used terms... 2 1.1 Inspiration... 2 1.2 Expiration... 2 1.3 Breath rate (bpm)... 2 1.4 Ventilation... 2 1.5 Biphasic
VENTILATORS PURPOSE OBJECTIVES
 VENTILATORS PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain a ventilator in the interfacility transfer environment. COGNITIVE OBJECTIVES
VENTILATORS PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain a ventilator in the interfacility transfer environment. COGNITIVE OBJECTIVES
AUTOVENT 4000 VENTILATOR
 OVERVIEW AUTOVENT 4000 Only properly trained and approved Escambia County Bureau of Public Safety Paramedics are to use the AutoVent 4000 ventilator manufactured by LSP to transport patients already on
OVERVIEW AUTOVENT 4000 Only properly trained and approved Escambia County Bureau of Public Safety Paramedics are to use the AutoVent 4000 ventilator manufactured by LSP to transport patients already on
Clinical Skills. Administering Oxygen
 Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
PERFORMANCE EVALUATION #34 NAME: 7200 Ventilator Set Up DATE: INSTRUCTOR:
 PERFORMANCE EVALUATION #34 NAME: 7200 Ventilator Set Up DATE: 1. **Identify and name the filters on the 7200ae. 2. **Explain how each filter is sterilized. 3. **Trace the gas flow through the ventilator
PERFORMANCE EVALUATION #34 NAME: 7200 Ventilator Set Up DATE: 1. **Identify and name the filters on the 7200ae. 2. **Explain how each filter is sterilized. 3. **Trace the gas flow through the ventilator
O-Two Self-Study Guide. Equinox Relieve
 O-Two Self-Study Guide Equinox Relieve PRODUCT DESCRIPTION/PRINCIPLES OF OPERATION The Equinox Relieve provides spontaneously breathing patients with a preset mixture of oxygen and nitrous oxide for analgesia
O-Two Self-Study Guide Equinox Relieve PRODUCT DESCRIPTION/PRINCIPLES OF OPERATION The Equinox Relieve provides spontaneously breathing patients with a preset mixture of oxygen and nitrous oxide for analgesia
NOTE: If not used, provider must document reason(s) for deferring mechanical ventilation in a patient with an advanced airway
 APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
patient education program 4156 South 52 nd Street, Omaha, NE ChildrensOmaha.org/HomeHealthcare
 patient education program 4156 South 52 nd Street, Omaha, NE 68117 800-747-7334 402-734-6741 ChildrensOmaha.org/HomeHealthcare We know children CHILDREN S HOME HEALTHCARE Trilogy Ventilator Instructions
patient education program 4156 South 52 nd Street, Omaha, NE 68117 800-747-7334 402-734-6741 ChildrensOmaha.org/HomeHealthcare We know children CHILDREN S HOME HEALTHCARE Trilogy Ventilator Instructions
UNDERSTANDING NEONATAL WAVEFORM GRAPHICS. Brandon Kuehne, MBA, RRT-NPS, RPFT Director- Neonatal Respiratory Services
 UNDERSTANDING NEONATAL WAVEFORM GRAPHICS Brandon Kuehne, MBA, RRT-NPS, RPFT Director- Neonatal Respiratory Services Disclosures Purpose: To enhance bedside staff s knowledge of ventilation and oxygenation
UNDERSTANDING NEONATAL WAVEFORM GRAPHICS Brandon Kuehne, MBA, RRT-NPS, RPFT Director- Neonatal Respiratory Services Disclosures Purpose: To enhance bedside staff s knowledge of ventilation and oxygenation
Selecting the Ventilator and the Mode. Chapter 6
 Selecting the Ventilator and the Mode Chapter 6 Criteria for Ventilator Selection Why does the patient need ventilatory support? Does the ventilation problem require a special mode? What therapeutic goals
Selecting the Ventilator and the Mode Chapter 6 Criteria for Ventilator Selection Why does the patient need ventilatory support? Does the ventilation problem require a special mode? What therapeutic goals
Complex Care Hub Manual: Pressure Ventilation on the LTV 1200
 Complex Care Hub Manual: Pressure Ventilation on the LTV 1200 Table of Contents 1 Mechanical Ventilation... 3 2 Important information for support worker... 3 3 Commonly used terms... 3 3.1 Inspiration...
Complex Care Hub Manual: Pressure Ventilation on the LTV 1200 Table of Contents 1 Mechanical Ventilation... 3 2 Important information for support worker... 3 3 Commonly used terms... 3 3.1 Inspiration...
Instructions/Procedure for Use of the Speaking Valve
 Instructions/Procedure for Use of the Speaking Valve Notes on the use of the speaking valve for ventilator-dependent and non-ventilator dependent patients The speaking valve is a one-way valve that allows
Instructions/Procedure for Use of the Speaking Valve Notes on the use of the speaking valve for ventilator-dependent and non-ventilator dependent patients The speaking valve is a one-way valve that allows
2 PRE USE FUNCTION CHECK 3 OPERATING PROCEDURE 4 SERVICING. 5 CAREvent ALS ACCESSORIES 11
 THE RESUSCITATOR MUST BE THOROUGHLY CLEANED AFTER EACH PATIENT USE. 1. Operate CAREvent ALS Handheld Resuscitator to blow out any contaminant from the patient valve. 2. Ensure CAREvent ALS Handheld Resuscitator
THE RESUSCITATOR MUST BE THOROUGHLY CLEANED AFTER EACH PATIENT USE. 1. Operate CAREvent ALS Handheld Resuscitator to blow out any contaminant from the patient valve. 2. Ensure CAREvent ALS Handheld Resuscitator
Patient Information for the: Humanitarian Device for use in the Control of Air Leaks
 Patient Information for the: Humanitarian Device for use in the Control of Air Leaks Glossary Airway: The tubes in the lungs that pass air to and from the lung tissue. Anesthesia: Technique to make the
Patient Information for the: Humanitarian Device for use in the Control of Air Leaks Glossary Airway: The tubes in the lungs that pass air to and from the lung tissue. Anesthesia: Technique to make the
Standards and guidelines for care and management of patients requiring oxygen therapy.
 PURPOSE Standards and guidelines for care and management of patients requiring oxygen therapy. STANDARDS Ongoing management of oxygen therapy requires a prescriber s order. The order must specify oxygen
PURPOSE Standards and guidelines for care and management of patients requiring oxygen therapy. STANDARDS Ongoing management of oxygen therapy requires a prescriber s order. The order must specify oxygen
Tracheostomy and Ventilator Education Program Module 11: Emergency Preparedness
 Tracheostomy and Ventilator Education Program Module 11: Emergency Preparedness Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who
Tracheostomy and Ventilator Education Program Module 11: Emergency Preparedness Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who
HONG KONG COLLEGE OF ANAESTHESIOLOGISTS TECHNICAL GUIDINES RECOMMENDATIONS ON CHECKING ANAESTHESIA DELIVERY SYSTEMS
 RECOMMENDATIONS ON CHECKING ANAESTHESIA DELIVERY SYSTEMS 1. INTRODUCTION An anaesthesia delivery system includes any machine, equipment or apparatus which supplies gases, vapours, local anaesthesia and/or
RECOMMENDATIONS ON CHECKING ANAESTHESIA DELIVERY SYSTEMS 1. INTRODUCTION An anaesthesia delivery system includes any machine, equipment or apparatus which supplies gases, vapours, local anaesthesia and/or
Medical Instruments in the Developing World
 2.2 Ventilators 2.2.1 Clinical Use and Principles of Operation Many patients in an intensive care and the operating room require the mechanical ventilation of their lungs. All thoracic surgery patients,
2.2 Ventilators 2.2.1 Clinical Use and Principles of Operation Many patients in an intensive care and the operating room require the mechanical ventilation of their lungs. All thoracic surgery patients,
Completed downloadable Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 5th Edition by Cairo
 Completed downloadable Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 5th Edition by Cairo Link full download: http://testbankcollection.com/download/pilbeams-mechanicalventilation-physiological-and-clinical-applications-5th-edition-test-bank-cairo
Completed downloadable Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 5th Edition by Cairo Link full download: http://testbankcollection.com/download/pilbeams-mechanicalventilation-physiological-and-clinical-applications-5th-edition-test-bank-cairo
OXYGEN THERAPY. (Non-invasive O2 therapy in patient >8yrs)
 OXYGEN THERAPY (Non-invasive O2 therapy in patient >8yrs) Learning aims Indications and precautions for O2 therapy Targets of therapy Standard notation O2 delivery devices Taps, tanks and tubing Notation
OXYGEN THERAPY (Non-invasive O2 therapy in patient >8yrs) Learning aims Indications and precautions for O2 therapy Targets of therapy Standard notation O2 delivery devices Taps, tanks and tubing Notation
HIGH FREQUENCY JET VENTILATION (HFJV): EQUIPMENT PREPRATION
 POLICY The physician orders High Frequency Jet Ventilation (HFJV). The Respiratory Therapist in discussion with the physician will determine blood gas targets and ventilation settings for the treatment
POLICY The physician orders High Frequency Jet Ventilation (HFJV). The Respiratory Therapist in discussion with the physician will determine blood gas targets and ventilation settings for the treatment
Selecting and Connecting Breathing Systems
 Selecting and Connecting Breathing Year Group: BVSc3 + Document number: CSL_A03 Equipment for this station: Equipment list: Pen Paper Calculator T-piece (in CSL a strip of white tape is around this system)
Selecting and Connecting Breathing Year Group: BVSc3 + Document number: CSL_A03 Equipment for this station: Equipment list: Pen Paper Calculator T-piece (in CSL a strip of white tape is around this system)
excellence in care Procedure Management of patients with difficult oxygenation. For Review Aug 2015
 Difficult Oxygenation HELI.CLI.12 Purpose This procedure describes the processes and procedures for a lung protective strategy in the mechanical ventilation of patients that are difficult to oxygenate
Difficult Oxygenation HELI.CLI.12 Purpose This procedure describes the processes and procedures for a lung protective strategy in the mechanical ventilation of patients that are difficult to oxygenate
My CoughAssist. A patient guide to CoughAssist T70. Please visit
 Philips Healthcare is part of Royal Philips Electronics Europe, Middle East, Africa +49 7031 463 2254 How to reach us www.philips.com/healthcare healthcare@philips.com Latin America +55 11 2125 0744 Asia
Philips Healthcare is part of Royal Philips Electronics Europe, Middle East, Africa +49 7031 463 2254 How to reach us www.philips.com/healthcare healthcare@philips.com Latin America +55 11 2125 0744 Asia
Mechanical Ventilation. Mechanical Ventilation is a Drug!!! is a drug. MV: Indications for use. MV as a Drug: Outline. MV: Indications for use
 Mechanical Ventilation is a Drug!!! Mechanical Ventilation is a drug I am an employee of Philips Healthcare Hospital Respiratory Care Group and they help me pay for my kids education Jim Laging, RRT, RCP
Mechanical Ventilation is a Drug!!! Mechanical Ventilation is a drug I am an employee of Philips Healthcare Hospital Respiratory Care Group and they help me pay for my kids education Jim Laging, RRT, RCP
Recommendations on Checking Anaesthesia Delivery Systems
 Page 1 of 11 Recommendations on Checking Anaesthesia Delivery Version Effective Date 1 Oct 1992 (reviewed Feb 07, Feb 02) 2 2004 3 Nov 2011 4 Dec 2016 Document No. HKCA T1 v4 Prepared by College Guidelines
Page 1 of 11 Recommendations on Checking Anaesthesia Delivery Version Effective Date 1 Oct 1992 (reviewed Feb 07, Feb 02) 2 2004 3 Nov 2011 4 Dec 2016 Document No. HKCA T1 v4 Prepared by College Guidelines
RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE
 Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Pulmonary Function and
Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Pulmonary Function and
TITLE: Pulse Oximetry COMPETENCY #: Resp #1 NEW COMPETENCY REVISION DATE: 10/18/12 EMPLOYEE NAME. DATE INITIAL RE-EVALUATION ANNUAL (if required) PRN
 : Pulse Oximetry COMPETENCY #: Resp #1 NEW COMPETENCY REVISION : 10/18/12 INITIAL RE-EVALUATION ANNUAL (if required) PRN 1. Verifies physician order. 2. Gathers equipment and supplies. 3. Knocks on door
: Pulse Oximetry COMPETENCY #: Resp #1 NEW COMPETENCY REVISION : 10/18/12 INITIAL RE-EVALUATION ANNUAL (if required) PRN 1. Verifies physician order. 2. Gathers equipment and supplies. 3. Knocks on door
Merlin Training for Vets and Nurses
 Merlin Training for Vets and Nurses Objectives To familiarise users with the controls of Merlin To familiarise users with the pneumatic connections of Merlin To ensure that users understand the behaviour
Merlin Training for Vets and Nurses Objectives To familiarise users with the controls of Merlin To familiarise users with the pneumatic connections of Merlin To ensure that users understand the behaviour
Automatic Transport Ventilator
 Automatic Transport Ventilator David M. Landsberg, MD, FACP, FCCP, EMT-P Luke J. Gasowski, RRT, NPS, ACCS, CCP-C, FP-C Christopher J. Fullagar, MD, FACEP, EMT-P Stan Goettel, MS, EMT-P Author credits /
Automatic Transport Ventilator David M. Landsberg, MD, FACP, FCCP, EMT-P Luke J. Gasowski, RRT, NPS, ACCS, CCP-C, FP-C Christopher J. Fullagar, MD, FACEP, EMT-P Stan Goettel, MS, EMT-P Author credits /
VENTILATION STRATEGIES FOR THE CRITICALLY UNWELL
 VENTILATION STRATEGIES FOR THE CRITICALLY UNWELL Dr Nick Taylor Visiting Emergency Specialist Teaching Hospital Karapitiya Senior Specialist and Director ED Training Clinical Lecturer, Australian National
VENTILATION STRATEGIES FOR THE CRITICALLY UNWELL Dr Nick Taylor Visiting Emergency Specialist Teaching Hospital Karapitiya Senior Specialist and Director ED Training Clinical Lecturer, Australian National
Invasive mechanical ventilation:
 Invasive mechanical ventilation definition mechanical ventilation: using an apparatus to facilitate transport of oxygen and CO2 between the atmosphere and the alveoli for the purpose of enhancing pulmonary
Invasive mechanical ventilation definition mechanical ventilation: using an apparatus to facilitate transport of oxygen and CO2 between the atmosphere and the alveoli for the purpose of enhancing pulmonary
RESPIRATORY CARE POLICY AND PROCEDURE MANUAL. a) Persistent hypoxemia despite improved ventilatory pattern and elevated Fl02
 The University of Mississippi AND PROCEDURE MANUAL Effective Date: June 30, 1990 Revised Date: December 2009 MANUAL CODE Page 1 of 5 PREPARED BY: Respiratory Care Policy and Procedure Review Committee
The University of Mississippi AND PROCEDURE MANUAL Effective Date: June 30, 1990 Revised Date: December 2009 MANUAL CODE Page 1 of 5 PREPARED BY: Respiratory Care Policy and Procedure Review Committee
Medical Ventilators. Presented by: Edwin Lim
 Medical Ventilators Presented by: Edwin Lim 1 Presentation Outline Respiration and You Medical Ventilators: Why? How? Current Medical Ventilators The Future 2 The Importance of Oxygen People can survive
Medical Ventilators Presented by: Edwin Lim 1 Presentation Outline Respiration and You Medical Ventilators: Why? How? Current Medical Ventilators The Future 2 The Importance of Oxygen People can survive
Automatic Transport Ventilators. ICU Quality Ventilation on the Street.
 Automatic Transport Ventilators ICU Quality Ventilation on the Street. Kevin Bowden, March 20 th 2014 Ventilator Definition A ventilator is an automatic mechanical device designed to provide all or part
Automatic Transport Ventilators ICU Quality Ventilation on the Street. Kevin Bowden, March 20 th 2014 Ventilator Definition A ventilator is an automatic mechanical device designed to provide all or part
A guide to completing Bubble PEP
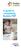 A guide to completing Bubble PEP What is Bubble PEP? PEP stands for Positive Expiratory Pressure (PEP), which means that you blow out against resistance and keep some air in your lungs. Bubble PEP is a
A guide to completing Bubble PEP What is Bubble PEP? PEP stands for Positive Expiratory Pressure (PEP), which means that you blow out against resistance and keep some air in your lungs. Bubble PEP is a
Notes on BIPAP/CPAP. M.Berry Emergency physician St Vincent s Hospital, Sydney
 Notes on BIPAP/CPAP M.Berry Emergency physician St Vincent s Hospital, Sydney 2 DEFINITIONS Non-Invasive Positive Pressure Ventilation (NIPPV) Encompasses both CPAP and BiPAP Offers ventilation support
Notes on BIPAP/CPAP M.Berry Emergency physician St Vincent s Hospital, Sydney 2 DEFINITIONS Non-Invasive Positive Pressure Ventilation (NIPPV) Encompasses both CPAP and BiPAP Offers ventilation support
Unit 15 Manual Resuscitators
 15-1 Unit 15 Manual Resuscitators GOAL On completion of this unit, the student should comprehend the proper operation of self-inflating resuscitation bags, flow-inflating resuscitation bags and gas-powered
15-1 Unit 15 Manual Resuscitators GOAL On completion of this unit, the student should comprehend the proper operation of self-inflating resuscitation bags, flow-inflating resuscitation bags and gas-powered
Ventilator Training Module
 Ventilator Training Module LTV (Lap Top Ventilator) Teaching Script LTV User guides: http://www.carefusion.com/documents/guides/user-guides/rc_ltv-1000_ug_en.pdf http://www.carefusion.com/documents/guides/user-guides/rc_ltv-1100_ug_en.pdf
Ventilator Training Module LTV (Lap Top Ventilator) Teaching Script LTV User guides: http://www.carefusion.com/documents/guides/user-guides/rc_ltv-1000_ug_en.pdf http://www.carefusion.com/documents/guides/user-guides/rc_ltv-1100_ug_en.pdf
EasyFit Lite Nasal Mask, Silicone. Nasal Mask. EasyFit Lite Nasal Mask. Device Description and Instructions for Use. Caution:
 EasyFit Lite Nasal Mask EasyFit Lite Nasal Mask, Silicone Nasal Mask Device Description and Instructions for Use Caution: Federal Law (U.S.A.) restricts this device to sale by or on the order of a physician.
EasyFit Lite Nasal Mask EasyFit Lite Nasal Mask, Silicone Nasal Mask Device Description and Instructions for Use Caution: Federal Law (U.S.A.) restricts this device to sale by or on the order of a physician.
LAB 7 HUMAN RESPIRATORY LAB. Complete the charts on pgs. 67 and 68 and read directions for using BIOPAC
 66 LAB 7 HUMAN RESPIRATORY LAB Assignments: Due before lab: Quiz: Three Respiratory Interactive Physiology Animations pages 69 73. Complete the charts on pgs. 67 and 68 and read directions for using BIOPAC
66 LAB 7 HUMAN RESPIRATORY LAB Assignments: Due before lab: Quiz: Three Respiratory Interactive Physiology Animations pages 69 73. Complete the charts on pgs. 67 and 68 and read directions for using BIOPAC
PROCEDURE (TASK): ROUTINE VENTILATOR CHECK. 5. Verifies current ventilator Insures correspondence between physician's
 PROCEDURE (TASK): ROUTINE VENTILATOR CHECK I. KEY PERFORMANCE ELEMENTS Procedural Element (Step): Description of Performance: 5. Verifies current ventilator Insures correspondence between physician's settings
PROCEDURE (TASK): ROUTINE VENTILATOR CHECK I. KEY PERFORMANCE ELEMENTS Procedural Element (Step): Description of Performance: 5. Verifies current ventilator Insures correspondence between physician's settings
BASIC LIFE SUPPORT - PAEDIATRIC
 BASIC LIFE SUPPORT - PAEDIATRIC First Issued by/date BKW PCT May 2003 Issue Version Purpose of Issue/Description of Change 3 Policy reviewed. No changes in procedure or legislation since policy revised
BASIC LIFE SUPPORT - PAEDIATRIC First Issued by/date BKW PCT May 2003 Issue Version Purpose of Issue/Description of Change 3 Policy reviewed. No changes in procedure or legislation since policy revised
Initiation and Management of Airway Pressure Release Ventilation (APRV)
 Initiation and Management of Airway Pressure Release Ventilation (APRV) Eric Kriner RRT Pulmonary Critical Care Clinical Specialist Pulmonary Services Department Medstar Washington Hospital Center Disclosures
Initiation and Management of Airway Pressure Release Ventilation (APRV) Eric Kriner RRT Pulmonary Critical Care Clinical Specialist Pulmonary Services Department Medstar Washington Hospital Center Disclosures
Standard Operating Procedure
 Standard Operating Procedure SOP ID C04 Version 1.0 Title Approved by Capnography: MobiMed Clinical Effectiveness Group Date Issued 1 st February 2013 Review Date 31 st January 2015 Directorate Clinical
Standard Operating Procedure SOP ID C04 Version 1.0 Title Approved by Capnography: MobiMed Clinical Effectiveness Group Date Issued 1 st February 2013 Review Date 31 st January 2015 Directorate Clinical
Difficult Oxygenation Distribution: Sydney X Illawarra X Orange X
 HELICOPTER OPERATING PROCEDURE HOP No: C/12 Issued: May 2011 Page: 1 of 5 Revision No: Original Difficult Oxygenation Distribution: Sydney X Illawarra X Orange X TRIM No: 09/300 Document No: D10/9973 X
HELICOPTER OPERATING PROCEDURE HOP No: C/12 Issued: May 2011 Page: 1 of 5 Revision No: Original Difficult Oxygenation Distribution: Sydney X Illawarra X Orange X TRIM No: 09/300 Document No: D10/9973 X
Auditing the non-emergency use of a fan or oxygen to relieve breathlessness at rest: Background form
 Auditing the non-emergency use of a fan or oxygen to relieve breathlessness at rest: Background form Background Breathlessness is a common and distressing symptom that can be difficult to treat. Oxygen
Auditing the non-emergency use of a fan or oxygen to relieve breathlessness at rest: Background form Background Breathlessness is a common and distressing symptom that can be difficult to treat. Oxygen
Your patients, our primary focus. Siesta i Whispa anesthesia machine
 Your patients, our primary focus Siesta i Whispa anesthesia machine Functional, and flexible At Dameca we are not just committed to meeting the healthcare needs of today. We also think about tomorrow.
Your patients, our primary focus Siesta i Whispa anesthesia machine Functional, and flexible At Dameca we are not just committed to meeting the healthcare needs of today. We also think about tomorrow.
State-of-the-art anesthesia technology
 State-of-the-art anesthesia technology anesthesia system Get closer to the MRI scanner Superb certified performance in close proximity to strong magnetic fields. Our innovative machine provides benefits
State-of-the-art anesthesia technology anesthesia system Get closer to the MRI scanner Superb certified performance in close proximity to strong magnetic fields. Our innovative machine provides benefits
V8600 Ventilator. Integrated Invasive & Noninvasive Ventilation
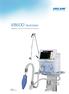 V8600 Ventilator Integrated Invasive & Noninvasive Ventilation 0123 V8600 Ventilator Invasive Ventilation With state-of-the-art turbine technology, V8600 helps achieve sequential ventilation in various
V8600 Ventilator Integrated Invasive & Noninvasive Ventilation 0123 V8600 Ventilator Invasive Ventilation With state-of-the-art turbine technology, V8600 helps achieve sequential ventilation in various
Introduction to Conventional Ventilation
 Introduction to Conventional Ventilation Dr Julian Eason Consultant Neonatologist Derriford Hospital Mechanics Inspiration diaphragm lowers and thorax expands Negative intrathoracic/intrapleural pressure
Introduction to Conventional Ventilation Dr Julian Eason Consultant Neonatologist Derriford Hospital Mechanics Inspiration diaphragm lowers and thorax expands Negative intrathoracic/intrapleural pressure
Figure 1. A schematic diagram of the human respiratory system.
 Introduction to Respiration In this experiment, you will investigate various aspects of normal breathing, hyperventilation, rebreathing the effect of changing airway resistance and ways in which to measure
Introduction to Respiration In this experiment, you will investigate various aspects of normal breathing, hyperventilation, rebreathing the effect of changing airway resistance and ways in which to measure
Astral in AirView: Improving patient care through connectivity. ResMed.com
 Astral in AirView: Improving patient care through connectivity ResMed.com This guide will assist you with: Setting up the ResMed Connectivity Module for Astral 2 Troubleshooting the ResMed Connectivity
Astral in AirView: Improving patient care through connectivity ResMed.com This guide will assist you with: Setting up the ResMed Connectivity Module for Astral 2 Troubleshooting the ResMed Connectivity
Chapter 9 Airway Respirations Metabolism Oxygen Requirements Respiratory Anatomy Respiratory Anatomy Respiratory Anatomy Diaphragm
 1 Chapter 9 Airway 2 Respirations Every cell of the body requires to survive Oxygen must come in and carbon must go out 3 Metabolism Metabolism--Process where the body s cells convert food to Adequate
1 Chapter 9 Airway 2 Respirations Every cell of the body requires to survive Oxygen must come in and carbon must go out 3 Metabolism Metabolism--Process where the body s cells convert food to Adequate
Neonatal tidal volume targeted ventilation
 Neonatal tidal volume targeted ventilation Colin Morley Retired Professor of Neonatal Medicine, Royal Women s Hospital, Melbourne, Australia. Honorary Visiting Fellow, Dept Obstetrics and Gynaecology,
Neonatal tidal volume targeted ventilation Colin Morley Retired Professor of Neonatal Medicine, Royal Women s Hospital, Melbourne, Australia. Honorary Visiting Fellow, Dept Obstetrics and Gynaecology,
COALINGA STATE HOSPITAL. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
R S A B C CPR. Basic Life Support Flow Chart Check for danger. Check Response. Send for Help. Check Airway. Check for Breathing.
 CPR CPR is the technique of the manual inflation of the lungs with oxygen, and compression of the heart, therefore pumping oxygenated blood around the body, and keeping the vital organs supplied with oxygen.
CPR CPR is the technique of the manual inflation of the lungs with oxygen, and compression of the heart, therefore pumping oxygenated blood around the body, and keeping the vital organs supplied with oxygen.
Endotracheal Suctioning: In Line ETT
 Approved by: Endotracheal Suctioning: In Line ETT Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures
Approved by: Endotracheal Suctioning: In Line ETT Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures
Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo
 Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo Link full download: http://testbankair.com/download/test-bank-for-pilbeams-mechanicalventilation-physiological-and-clinical-applications-6th-edition-by-cairo/
Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo Link full download: http://testbankair.com/download/test-bank-for-pilbeams-mechanicalventilation-physiological-and-clinical-applications-6th-edition-by-cairo/
Astral in AirView: Improving patient care through connectivity. ResMed.com
 Astral in AirView: Improving patient care through connectivity ResMed.com Using Astral in AirView via the ResMed Connectivity Module (RCM) Astral is ResMed s portable, invasive and non-invasive life support
Astral in AirView: Improving patient care through connectivity ResMed.com Using Astral in AirView via the ResMed Connectivity Module (RCM) Astral is ResMed s portable, invasive and non-invasive life support
Capnography in the Veterinary Technician Toolbox. Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA
 Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
6 th Accredited Advanced Mechanical Ventilation Course for Anesthesiologists. Course Test Results for the accreditation of the acquired knowledge
 6 th Accredited Advanced Mechanical Ventilation Course for Anesthesiologists Course Test Results for the accreditation of the acquired knowledge Q. Concerning the mechanics of the newborn s respiratory
6 th Accredited Advanced Mechanical Ventilation Course for Anesthesiologists Course Test Results for the accreditation of the acquired knowledge Q. Concerning the mechanics of the newborn s respiratory
RSPT 1060 OBJECTIVES OBJECTIVES OBJECTIVES EQUATION OF MOTION. MODULE C Applied Physics Lesson #1 - Mechanics. Ventilation vs.
 RSPT 1060 MODULE C Applied Physics Lesson #1 - Mechanics OBJECTIVES At the end of this module, the student should be able to define the terms and abbreviations used in the module. draw & explain the equation
RSPT 1060 MODULE C Applied Physics Lesson #1 - Mechanics OBJECTIVES At the end of this module, the student should be able to define the terms and abbreviations used in the module. draw & explain the equation
London Respiratory Team
 London Respiratory Team By email 28 March 2012 Ambulatory Oxygen for London This guide has been produced to help healthcare maximise the benefit of the new oxygen contract for patients and to reduce waste.
London Respiratory Team By email 28 March 2012 Ambulatory Oxygen for London This guide has been produced to help healthcare maximise the benefit of the new oxygen contract for patients and to reduce waste.
Understanding Tracheostomy Care
 Understanding Tracheostomy Care Inside this guide: This guide will help you learn how to take care of your tracheostomy (trach). It is important to ask questions. You will be given time to learn. Working
Understanding Tracheostomy Care Inside this guide: This guide will help you learn how to take care of your tracheostomy (trach). It is important to ask questions. You will be given time to learn. Working
You Are Really Full of Hot Air!
 You Are Really Full of Hot Air! Student Information Page 5B Activity Introduction: You re just full of hot air! How many times has someone said this to you when they didn t quite believe what you were
You Are Really Full of Hot Air! Student Information Page 5B Activity Introduction: You re just full of hot air! How many times has someone said this to you when they didn t quite believe what you were
Medical Ventilators. Ryan Sanford Daniel Tajik
 Medical Ventilators Ryan Sanford Daniel Tajik Medical Ventilators Assist patients that have trouble breathing on their own. 2 Oxygen Intake The Respiratory System has the responsibility of providing the
Medical Ventilators Ryan Sanford Daniel Tajik Medical Ventilators Assist patients that have trouble breathing on their own. 2 Oxygen Intake The Respiratory System has the responsibility of providing the
Respiration Lab Instructions
 Respiration Lab Instructions This laboratory investigation can be performed in any order. Be sure to read all instructions for each section before performing the experiment. PART 1 STUDENT WET SPIROMETER
Respiration Lab Instructions This laboratory investigation can be performed in any order. Be sure to read all instructions for each section before performing the experiment. PART 1 STUDENT WET SPIROMETER
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: ENDO TRACHEAL SUCTIONING OF THE ADULT PATIENT (suc03) Nursing, Respiratory DATE: REVIEWED: PAGES: 11/82 12/18 1 of 5 RESPONSIBILITY: RN,
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: ENDO TRACHEAL SUCTIONING OF THE ADULT PATIENT (suc03) Nursing, Respiratory DATE: REVIEWED: PAGES: 11/82 12/18 1 of 5 RESPONSIBILITY: RN,
OXYGEN FOR ADULTS IN ACUTE CARE
 PATIENT GROUP DIRECTION FOR THE ADMINISTRATION OF OXYGEN FOR ADULTS IN ACUTE CARE ALL CLINICAL DIVISIONS ADULT CARE STATEMENT The staff indicated in Staff Group may administer oxygen in the two detailed
PATIENT GROUP DIRECTION FOR THE ADMINISTRATION OF OXYGEN FOR ADULTS IN ACUTE CARE ALL CLINICAL DIVISIONS ADULT CARE STATEMENT The staff indicated in Staff Group may administer oxygen in the two detailed
GE Healthcare. Centiva/5 Critical Care Ventilator. Meet a new level of expectations
 GE Healthcare Centiva/5 Critical Care Ventilator Meet a new level of expectations Intergrating performance and value Marry form and function In an environment where time and space are tight, the design
GE Healthcare Centiva/5 Critical Care Ventilator Meet a new level of expectations Intergrating performance and value Marry form and function In an environment where time and space are tight, the design
45A, Armthorpe Road, Brampton, Ontario, Canada, L6T 5M4. Made in Canada by O-Two Medical Technologies Inc.
 O-Two eseries Electronic Transport Ventilators O-Two Single Use Open CPAP Systems O-Two CAREvent Range of Automatic Transport Ventilators O-Two CAREvent Range of Automatic Resuscitators O-Two SMART BAG
O-Two eseries Electronic Transport Ventilators O-Two Single Use Open CPAP Systems O-Two CAREvent Range of Automatic Transport Ventilators O-Two CAREvent Range of Automatic Resuscitators O-Two SMART BAG
Objectives. Respiratory Failure : Challenging Cases in Mechanical Ventilation. EM Knows Respiratory Failure!
 Respiratory Failure : Challenging Cases in Mechanical Ventilation Peter DeBlieux, MD, FAAEM, FACEP LSUHSC University Hospital Pulmonary and Critical Care Medicine Emergency Medicine pdebli@lsuhsc.edu Objectives
Respiratory Failure : Challenging Cases in Mechanical Ventilation Peter DeBlieux, MD, FAAEM, FACEP LSUHSC University Hospital Pulmonary and Critical Care Medicine Emergency Medicine pdebli@lsuhsc.edu Objectives
Balloon Gastrostomy (BG) Tube
 Balloon Gastrostomy (BG) Tube Post insertion advice Please follow hospital/ Consultant advice for care of the tube and stoma site for the first 28 days (if the BG tube has been placed as a first gastrostomy
Balloon Gastrostomy (BG) Tube Post insertion advice Please follow hospital/ Consultant advice for care of the tube and stoma site for the first 28 days (if the BG tube has been placed as a first gastrostomy
Blease900 Ventilator PATIENT CENTERED VENTILATION
 Blease900 Ventilator PATIENT CENTERED VENTILATIN PATIENT CENTERED VENTILATIN From the first Blease/Manley ventilator sixty years ago, Spacelabs Healthcare has built a heritage of innovative and intuitive
Blease900 Ventilator PATIENT CENTERED VENTILATIN PATIENT CENTERED VENTILATIN From the first Blease/Manley ventilator sixty years ago, Spacelabs Healthcare has built a heritage of innovative and intuitive
3100A Competency Exam
 NAME DATE (Circle the appropriate answer) 3100A Competency Exam 1. Of the following, which best describes the mechanics of ventilation used by the 3100A? a. Active inspiration with passive exhalation b.
NAME DATE (Circle the appropriate answer) 3100A Competency Exam 1. Of the following, which best describes the mechanics of ventilation used by the 3100A? a. Active inspiration with passive exhalation b.
ONLINE DATA SUPPLEMENT. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg
 APPENDIX 1 Appendix 1. Complete respiratory protocol. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg predicted body weight (PBW)) (NEJM 2000; 342
APPENDIX 1 Appendix 1. Complete respiratory protocol. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg predicted body weight (PBW)) (NEJM 2000; 342
Pulmonary Function I (modified by C. S. Tritt, April 10, 2006) Volumes and Capacities
 I. Introduction Pulmonary Function I (modified by C. S. Tritt, April 10, 2006) Volumes and Capacities The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer
I. Introduction Pulmonary Function I (modified by C. S. Tritt, April 10, 2006) Volumes and Capacities The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer
War Surgery Dr. Abdulwahid INTRODUCTION: AIRWAY, BREATHING
 War Surgery Dr. Abdulwahid INTRODUCTION: AIRWAY, BREATHING The aims of war surgery: Save life Avoid infectious complications Save limbs Minimize residual disability The outcome is influenced by: Type of
War Surgery Dr. Abdulwahid INTRODUCTION: AIRWAY, BREATHING The aims of war surgery: Save life Avoid infectious complications Save limbs Minimize residual disability The outcome is influenced by: Type of
Breathing Circuits. Product training
 Breathing Circuits Product training Agenda Introduction to Breathing Circuits Anaesthesia Circuits Intensive Care Circuits Accessories 2 Covidien Introduction 3 Covidien What is a breathing circuit? In
Breathing Circuits Product training Agenda Introduction to Breathing Circuits Anaesthesia Circuits Intensive Care Circuits Accessories 2 Covidien Introduction 3 Covidien What is a breathing circuit? In
Breathing Process: Inhalation
 Airway Chapter 6 Breathing Process: Inhalation Active part of breathing Diaphragm and intercostal muscles contract, allowing the lungs to expand. The decrease in pressure allows lungs to fill with air.
Airway Chapter 6 Breathing Process: Inhalation Active part of breathing Diaphragm and intercostal muscles contract, allowing the lungs to expand. The decrease in pressure allows lungs to fill with air.
Using Common Ventilator Graphics to Provide Optimal Ventilation
 Using Common Ventilator Graphics to Provide Optimal Ventilation David Vines, MHS, RRT, FAARC Associate Professor Chair / Program Director Department of Respiratory Care RUSH UNIVERSITY MEDICAL CENTER Disclosure
Using Common Ventilator Graphics to Provide Optimal Ventilation David Vines, MHS, RRT, FAARC Associate Professor Chair / Program Director Department of Respiratory Care RUSH UNIVERSITY MEDICAL CENTER Disclosure
Lung Volumes and Capacities
 Lung Volumes and Capacities Experiment 19 Measurement of lung volumes provides a tool for understanding normal function of the lungs as well as disease states. The breathing cycle is initiated by expansion
Lung Volumes and Capacities Experiment 19 Measurement of lung volumes provides a tool for understanding normal function of the lungs as well as disease states. The breathing cycle is initiated by expansion
Hallowell EMC 2000 and 2002 Veterinary Ventilator Set-up, Use, and Troubleshooting
 Hallowell EMC 2000 and 2002 Veterinary Ventilator Set-up, Use, and Troubleshooting This is a quick reference for setting up, using, and troubleshooting the Hallowell EMC 2000 and 2002 Small Animal Ventilator.
Hallowell EMC 2000 and 2002 Veterinary Ventilator Set-up, Use, and Troubleshooting This is a quick reference for setting up, using, and troubleshooting the Hallowell EMC 2000 and 2002 Small Animal Ventilator.
E C C. American Heart Association. Basic Life Support for Healthcare Providers. Written Examinations. March 2011
 E C C American Heart Association Basic Life Support for Healthcare Providers Written Examinations Contents: Examination Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference
E C C American Heart Association Basic Life Support for Healthcare Providers Written Examinations Contents: Examination Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference
Name: Oasis: Questions EPCP. Professional Development: ETCO2 Monitoring
 EPCP Professional Development: ET Monitoring Name: Oasis: Questions ET Questions Package 1) Blood entering the pulmonary circuit from the systemic circuit contains on average mmhg. a) 36 b) 46 c) 4 d)
EPCP Professional Development: ET Monitoring Name: Oasis: Questions ET Questions Package 1) Blood entering the pulmonary circuit from the systemic circuit contains on average mmhg. a) 36 b) 46 c) 4 d)
How to use the SAVe II Ventilator
 TRAININGGROUNDS How to use the SAVe II Ventilator Designed to elevate the standard of care and improve triage capabilities simply select the height of the patient to deliver a targeted tidal volume. This
TRAININGGROUNDS How to use the SAVe II Ventilator Designed to elevate the standard of care and improve triage capabilities simply select the height of the patient to deliver a targeted tidal volume. This
Mechanical Ventilation
 Mechanical Ventilation Understanding Modes Rob Chatburn, RRT-NPS, FAARC Research Manager Respiratory Therapy Cleveland Clinic Associate Professor Case Western Reserve University 1 Overview Characteristics
Mechanical Ventilation Understanding Modes Rob Chatburn, RRT-NPS, FAARC Research Manager Respiratory Therapy Cleveland Clinic Associate Professor Case Western Reserve University 1 Overview Characteristics
Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams)
 Name Lab Partners Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams) Part 1. Lung Volumes and Capacities Objectives 1. Obtain graphical representation of lung capacities
Name Lab Partners Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams) Part 1. Lung Volumes and Capacities Objectives 1. Obtain graphical representation of lung capacities
