Penetrating chest trauma with lung perforation accounts for 5%
|
|
|
- Ronald Erik Riley
- 6 years ago
- Views:
Transcription
1 EAST 2013 POSTER PAPER Vented versus unvented chest seals for treatment of pneumothorax and prevention of tension pneumothorax in a swine model Bijan S. Kheirabadi, PhD, Irasema B. Terrazas, MS, Alexandra Koller, BS, Paul B. Allen, DSc, PA-C, Harold G. Klemcke, PhD, Victor A. Convertino, PhD, Michael A. Dubick, PhD, Robert T. Gerhardt, MD, MPH, and Lorne H. Blackbourne, MD, San Antonio, Texas BACKGROUND: Unvented chest seals (CSs) are currently recommended for the management of penetrating thoracic injuries in the battlefield. Since no supporting data exist, we compared the efficacy of a preferred unvented with that of a vented CS in a novel swine model of pneumothorax (PTx). METHODS: An open chest wound was created in the left thorax of spontaneously air-breathing anesthetized pigs (n = 8). A CS was applied over the injury, then tension PTx was induced by incremental air injections (0.2 L) into the pleural cavity via a cannula that was also used to measure intrapleural pressure (IP). Both CS were tested on each pig in series. Tidal volume (V T ), respiratory rate, IP, heart rate, mean arterial pressure, cardiac output, central venous pressure, pulmonary arterial pressure, venous and peripheral oxygen saturations (SvO 2, SpO 2 ) were recorded. Tension PTx was defined as a mean IP equal to or greater than +1 mm Hg plus significant (20Y30%) deviation in baseline levels of the previously mentioned parameters and confirmed by chest x-ray study. PaO 2 and PaCo 2 were also measured. RESULTS: PTx produced immediate breathing difficulty and significant rises in IP and pulmonary arterial pressure and falls in V T, SpO 2, and SvO 2. Both CSs returned these parameters to near baseline within 5 minutes of application. After vented CS was applied, serial air injections up to 2 L resulted in no significant change in the previously mentioned parameters. After unvented CS application, progressive deterioration of all respiratory parameters and onset of tension PTx were observed in all subjects after approximately 1.4-L air injection. CONCLUSION: Both vented and unvented CSs provided immediate improvements in breathing and blood oxygenation in our model of penetrating thoracic trauma. However, in the presence of ongoing intrapleural air accumulation, the unvented CS led to tension PTx, hypoxemia, and possible respiratory arrest, while the vented CS prevented these outcomes. (J Trauma Acute Care Surg. 2013;75: 150Y156. Copyright * 2013 by Lippincott Williams & Wilkins) KEY WORDS: Pneumothorax; chest seals; tension pneumothorax; combat casualty care; swine. Penetrating chest trauma with lung perforation accounts for 5% to 6% of battlefield injuries. 1 In combat, hemopneumothorax (HemoPTx) is the second leading cause of potentially preventable prehospital death and the third leading cause of mortality overall. 2 Unlike civilian trauma in which pneumothorax (PTx) and Hemo PTx are mostly caused by blunt mechanisms (e.g., motor vehicle collisions 3 ), in combat, these injury sequelae result primarily from gunshot wounds, explosive shrapnel, or blast overpressure injuries to the respiratory airways. 2,4 The prehospital management of patients with penetrating chest wounds poses significant difficulties in the battlefield. The open, sucking chest wound may act as a one-way valve, allowing air to enter the chest with every breath but not to escape. Air accumulates in the intrapleural space and forms a pneumothorax (PTx). Another source of PTx is internal air leaks from disrupted bronchioalveolar structures if the lungs sustain Submitted: December 7, 2012, Revised: February 4, 2013, Accepted: March 8, From the US Army Institute of Surgical Research, FortSam Houston, San Antonio, Texas. This study was presented as a poster at the 26th annual meeting of the Eastern Association for the Surgery of Trauma (EAST), January 15Y19, 2013, in Scottsdale, Arizona. The opinions or assertions expressed herein are the private views of the authors and are not to be construed as official or as reflecting the views of the US Department of Defense. Address for reprints: Bijan S. Kheirabadi, PhD, 3650 Chambers Pass, BHT2, Bldg 3610, Fort Sam Houston, TX 78234; Bijan.S.Kheirabadi.civ@mail.mil. DOI: /TA.0b013e afe 150 direct damage. The presence of PTx reduces physiologic negative pressure and functional residual capacity, rendering spontaneous breathing progressively difficult and inefficient. Positive-pressure ventilation may hasten development of tension PTx in an occluded chest wound with underlying lung injury and airway leak. 3,5 The traditional treatment of an open chest wound (open PTx) was to place a sterile occlusive dressing on the injury and tape it to the skin on three sides, leaving one side open to allow air to escape from the chest while blocking external air from entering. While effective, no corroborating evidence existed in support of this or any other technique, and the prevailing recommendation of Committee on Tactical Combat Casualty Care was to use a completely occlusive (unvented) chest seal (CS) with close monitoring of casualties for development of tension physiology. 6 Therefore, medical manufacturers responded by developing contemporary chest seals. As many as 15 different types of disposable adhesive CSs have been introduced into the market. Some possess a one-way venting valve that allows air to escape from the pleural cavity, but the preponderance of CS entering the current market are occlusive and have no venting valve. Most CSs meet physical requirements for military use (e.g., light weight, small size, durable, and adhesive under extreme temperature), but their functional capacities to treat PTx or HemoPTx and to prevent tension physiology are unknown. Thus, it is very difficult to identify and recommend the most clinically effective products for battlefield application. J Trauma Acute Care Surg
2 Report Documentation Page Form Approved OMB No Public reporting burden for the collection of information is estimated to average 1 hour per response, including the time for reviewing instructions, searching existing data sources, gathering and maintaining the data needed, and completing and reviewing the collection of information. Send comments regarding this burden estimate or any other aspect of this collection of information, including suggestions for reducing this burden, to Washington Headquarters Services, Directorate for Information Operations and Reports, 1215 Jefferson Davis Highway, Suite 1204, Arlington VA Respondents should be aware that notwithstanding any other provision of law, no person shall be subject to a penalty for failing to comply with a collection of information if it does not display a currently valid OMB control number. 1. REPORT DATE 01 JUL REPORT TYPE N/A 3. DATES COVERED - 4. TITLE AND SUBTITLE Vented versus unvented chest seals for treatment of pneumothorax and prevention of tension pneumothorax in a swine model. 6. AUTHOR(S) Kheirabadi B. S., Terrazas I. B., Koller A., Allen P. B., Klemcke H. G., Convertino V. A., Dubick M. A., Gerhardt R. T., Blackbourne L. H., 7. PERFORMING ORGANIZATION NAME(S) AND ADDRESS(ES) United States Army Institute of Surgical Research, JBSA Fort Sam Houston, TX 5a. CONTRACT NUMBER 5b. GRANT NUMBER 5c. PROGRAM ELEMENT NUMBER 5d. PROJECT NUMBER 5e. TASK NUMBER 5f. WORK UNIT NUMBER 8. PERFORMING ORGANIZATION REPORT NUMBER 9. SPONSORING/MONITORING AGENCY NAME(S) AND ADDRESS(ES) 10. SPONSOR/MONITOR S ACRONYM(S) 12. DISTRIBUTION/AVAILABILITY STATEMENT Approved for public release, distribution unlimited 13. SUPPLEMENTARY NOTES 14. ABSTRACT 15. SUBJECT TERMS 11. SPONSOR/MONITOR S REPORT NUMBER(S) 16. SECURITY CLASSIFICATION OF: 17. LIMITATION OF ABSTRACT UU a. REPORT unclassified b. ABSTRACT unclassified c. THIS PAGE unclassified 18. NUMBER OF PAGES 7 19a. NAME OF RESPONSIBLE PERSON Standard Form 298 (Rev. 8-98) Prescribed by ANSI Std Z39-18
3 J Trauma Acute Care Surg Kheirabadi et al. The purposes of this study were to (1) develop an open PTx wound model in swine with progression to tension PTx and (2) use that model to compare the effectiveness of two popular CSs in the US military (vented Bolin vs. unvented Halo) for treatment of PTx and prevention of tension PTx, 7 thereby aiding with the selection of the best device. MATERIALS AND METHODS This study was approved by the Animal Care and Use Committee of the US Army Institute of Surgical Research. All animals received care and were used in strict compliance with The Guide for the Care and Use of Laboratory Animals. 8 Animal Preparation and Instrumentation Female Yorkshire pigs (approximately 40 kg, n = 12) were induced with an intramuscular injection of tiletaminezolazepam (Telazol, 4Y6 mg/kg), intubated, and secured on the table in a supine position. During instrumentation, animals were mechanically ventilated with positive pressure air at 8 ml/kg per breath to 10 ml/kg per breath and 8 breaths per minute to 12 breaths per minute to maintain end-tidal PCO 2 of 40 T 5mmHg. Anesthesiawasprovidedwith1%to3%isoflurane.Maintenance fluid (lactated Ringer s solution at 3Y5 ml/kg/h) was administered through an ear vein catheter, and urine output was collected via a Foley catheter and was measured. Body temperature was monitored via a rectal probe and maintained at 37-C to 39-C. A pulse oximeter was attached to the tongue or cheek for measuring peripheral oxygen saturation levels (SpO 2 ). The right carotid artery was cannulated for continuous recording of blood pressure, heart rate (HR), and blood sampling. The right external jugular vein was cannulated to insert a Swan-Ganz catheter (oximetric PA catheter) into the right side of the heart for continuous measurement of central venous pressure, (CVP), pulmonary arterial pressure (PAP), mixed venous oxygen saturation (SvO 2 ), and cardiac output (CO). A radiopaque (stainless steel) J-wire was inserted into the jugular vein and extended into the inferior vena cava as a guide for locating the mediastinum on the chest x-ray study. After instrumentation, the animal was placed in sternal recumbent position and secured. Automatic respiration was discontinued, anesthetic gas was reduced, and the animal was allowed to breathe spontaneously (medical air) for the rest of the experiment. Chest Injury and Intrapleural Pressure Measurement Before chest injury, a 14-gauge catheter was inserted percutaneously into the left pleural space at the sixth intercostal space. This catheter was used for incremental air injection (0.2 L per injection) into the pleural cavity and intrapleural pressure (IP) measurement with a digital monometer (NETECH, DigiMano, Fig. 1A). To produce a chest injury, an incision was made through the dermis at the left fifth intercostal space on the axillary line. A hole was then created by blunt dissection into the pleural cavity and an 11.5-mm Thoracoport with a sleeve was inserted into the chest wall without injuring the lung. The trocar was then removed, but the sleeve was left in place creating an open track between the pleural cavity and outside (Fig. 1A). Following chest injury, the hole was plugged with a rubber stopper and excess air was evacuated with a syringe reestablishing the baseline negative IPs (j1.5 mm Hg expiration and j5 mm Hg inspiration) that were measured before the chest injury. Next, a 15-minute stabilization was allowed, and then baseline values for hemodynamic and respiratory parameters (tidal volume [V T ] and respiration rate [RR]) were recorded, and an arterial blood sample for blood gas analysis and a baseline chest x-ray images were obtained (Fig. 1B). Experimental Design After performing four-model development experiments, eight pigs were tested according to the methods described previously. The mediastinum in pigs, unlike in humans, is variably fenestrated (incomplete), allowing air communication from one hemithorax to the other. 9,10 Because of this variability in mediastinum among pigs, both CSs were tested on each animal in series (paired designed test). The order of CSs was reversed after each experiment. Figure 1. Experimental model of PTx and tension PTx in pigs. A, A test subject (sternal recumbency) after intrapleural cannulation and creation of an open chest wound. B, A baseline chest x-ray image after the chest wound was plugged, and excess air was withdrawn from pleural space (normal IP, IP). Note the J-wire, placed in inferior vena cava as a reference for mediastinum position. S-G C, Swan-Ganz catheter. * 2013 Lippincott Williams & Wilkins 151
4 Kheirabadi et al. J Trauma Acute Care Surg To induce PTx, the plug was removed from the chest hole, and free air movement into the left pleural space was allowed for 5 minutes. The resulting IP, hemodynamic, and respiratory parameters were then recorded. Next, CS 1 was placed over the hole and sealed around the chest wound. Changes in IP, hemodynamic, and respiratory parameters were recorded 5 minutes after CS application (PTx + CS). Next, increments of 200-mL air were injected into the pleural cavity every 5 minutes until either tension PTx developed or air was injected equivalent to 100% of the total lung capacity (TLC). The TLC was estimated to be approximately 55 ml per kilogram of body weight. 11 IP, hemodynamic, and respiratory values were recorded 5 minutes after each air injection. At the conclusion, an arterial blood sample was collected for blood gas measurement. The presence of tension PTx was defined 12 as a mean IP greater than +1 mm Hg and significant deviation from baseline values of at least 4 of the 5 following parameters: 30% rise of PAP, 30% fall of SvO 2, 20% fall of V T, mean arterial pressure (MAP), or CO. Development of tension PTx or lack of it was confirmed with a subsequent chest x-ray study. Once testing of the first CS was completed, it was removed, and the chest wound was plugged again. Any remaining air in the pleural cavity was evacuated with a syringe, and the baseline negative IP was restored. The animal was allowed to recover for at least 15 minutes until it regained normal and stable respiratory and hemodynamic functions. Baseline values for the next test (CS 2) were then recorded and new baseline blood sample and chest x-ray image were obtained. Next, another 5-minute open PTx was allowed and after recording the changes, the CS 2 was applied over the injury. The incremental air injections into pleural cavity were then repeated, and data were recorded as before. The animal was euthanized after final blood sample and x-ray image were obtained. Data Analysis Data are expressed as mean T SEM. Between-group analysis (Halo vs. Bolin) was performed using two-way repeatedmeasures analysis of variance. Bonferroni post test was used to compare replicate means at each PTx level. Within-group (treatment) analysis was performed only on the first three time points using repeated-measures analysis of variance with Dunnett s test as posttest. A p G 0.05 was considered significant. RESULTS Effects of PTx and CSs on Respiratory Function Five minutes of open PTx in the left hemithorax produced asignificantriseinip(p G 0.05) that approached 0 mm Hg as expected (Fig. 2) with subsequent significant reductions in percent SpO 2,SvO 2 (Fig. 3), and PaO 2 levels. The V T and RR were however modestly decreased (Table 1). Covering the chest wounds with either type of CS restored most parameters (i.e., inspiratory IP, SpO 2,SvO 2, and V T ) to near-baseline levels when measured at 5 minutes after application. Subsequent air injection into the chest that mimicked the lung injury and gradual air accumulation in the pleural cavity produced different effects depending on which type of CS was used. With the unvented CS, the IP progressively increased to positive levels with smaller differences between inspiration and expiration IP. The V T gradually declined, but RR remained unchanged. The SpO 2 and SvO 2 gradually but significantly declined as more air was injected, and SvO 2 fell below hypoxic levels (G60%) after 1.2-L to 1.4-L air injection. Breathing became more strenuous, and tension PTx was eventually developed in all subjects when IP reached +10 mm Hg (average). Partial pressures of oxygen (PaO 2 ) and carbon dioxide (PaCO 2 ) in the final blood samples were significantly deranged at the Figure 2. IP measured during inspiration and expiration cycles of pigs subjected to PTx and CS coverage and subsequent air injections. To examine the effectiveness of each CS against PTx, only the data obtained in the first three time points (i.e., baseline, PTx, and PTx + CS) were analyzed. The significant rise of IP as a result of PTx was counteracted by applying either CS. However, further intrapleural air injection could not be managed with unvented Halo CS and resulted in increased IP and the development of tension PTx. Note, the x axis notations in all the figures indicate the start of each event; the results are measured 5 minutes later and are shown in the next time point. For example, PTx was induced at 0 time, the changes in IP are seen at +5 minutes. 152 * 2013 Lippincott Williams & Wilkins
5 J Trauma Acute Care Surg Kheirabadi et al. Figure 3. Peripheral oxygen saturation (SpO 2, measured by pulse oximeter) and mixed venous oxygen saturation (SvO 2, measured by Swan-Ganz catheter) levels of pigs during PTx, CS coverage, and subsequent air injections. The deceases in these oxygenation indicators were restored by either CSs, but further intrapleural air accumulation could not be relieved by unvented CS (Halo) and resulted in hypoxemia. conclusion of the experiments (59 T 5mmHgand68T 3 mm Hg, respectively). In some instances, development of tension PTx coincided with respiratory arrest, during which animals breathing stopped suddenly and cyanosis became quite apparent. In such situations, the experiment was terminated immediately, and CS was removed, allowing PTx to be released, and spontaneous breathing was restored. In contrast, when the vented CS was used, no significant changes in IP, V T,SpO 2,SvO 2 (Figs.2and3andTable1),and respiratory effort of the animals were seen even after the maximum air injection (100% of TLC). The PaO 2 and PaCO 2 in blood samples also remained unchanged during experiments (86 T 6mmHgand55T 3 mm Hg, respectively). Effects of PTx and CSs on Circulatory Function The most prominent and immediate effect of PTx in the left pleural space was a significant increase of PAP measured at 5 minutes (Fig. 4). Little or no change was seen in other circulatory parameters such as CVP (Fig. 4), HR, CO, and MAP (Table 1) at this time. With unvented CS use, however, subsequent air injections into the pleural cavity resulted in gradual and significant increases of PAP, CVP, and HR. The CO and TABLE 1. Respiratory and Circulatory Parameters Measured During PTx Induction and CS Treatment V T, ml RR, breaths/min HR, beats/min MAP, mm Hg CO, L/min PTx Halo Bolin Halo Bolin Halo Bolin Halo Bolin Halo Bolin Baseline T T T 2 33 T T T T T T T 0.4 PTx 147 T 13.2* T 7.2* 29 T 3* 26 T 4* 146 T T T T T T 0.6 PTx + CS 160 T T T 3 35 T T T T T T T 0.5 CS L air T T T 2 36 T T T T T T T 0.5 CS L air 143 T T T 2 36 T T T T T T T 0.5 CS L air T T T 2 36 T T T T T T T 0.5 CS L air T T T 3 36 T T T T T T T 0.4 CS L air T T T 5 34 T T T T T T T 0.5 CS L air T 6.7** T T 3 34 T T T T T T T 0.4 CS L air T 7.8** 160 T T 1 34 T T T T T T T 0.4 CS L air N/A T 7.6 N/A 34 T 3 N/A 155 T 10 N/A 80.5 T 4.39 N/A 5.8 T 0.5 CS L air N/A 168 T 8.5 N/A 33 T 2 N/A 158 T 8 N/A 83.6 T 5.26 N/A 5.8 T 0.5 CS L air N/A T 5.5 N/A 33 T 2 N/A 157T 9 N/A 79.8 T 3.82 N/A 5.9 T 0.5 *p G 0.01 versus baseline of corresponding CS (only the first three measurements were compared). No significant differences were found in the changes of RR, HR, MAP, and CO between Halo and Bolin CS treatment. **p G 0.01 versus Bolin corresponding measures. Data are expressed as mean T SEM. N/A, could not be measured because air infusion was discontinued. * 2013 Lippincott Williams & Wilkins 153
6 Kheirabadi et al. J Trauma Acute Care Surg Figure 4. PAP and CVP of pigs during PTx, CS coverage, and subsequent intrapleural air infusion. Note that PAP rose rapidly in the presence of PTx and returned to baseline after covering with either CS. However, the CVP, measured in the right hemithorax, did not change in response to PTx in the left hemithorax. Further intrapleural air infusion increased both PAP and CVP and led to the development of tension PTx when the chest wounds were covered with unvented CSs. MAP minimally deceased shortly before development of tension PTx. In contrast, with vented CS coverage, air injection up to TLC produced no significant changes in the above circulatory parameters. Tension PTx developed after an average of 1.4-L air injection in all pigs when they were treated with unvented CS but did not occur with vented CS even after injection of 2 L to 2.2 L (TLC) of air. The x-ray images at the conclusion of an unvented CS test showed nearly total collapse of the left lung and significant deviation of the mediastinum to the right side as compared with baseline images (Fig. 5A and B). The mediastinum deviation and lung collapse seen in the x-ray images were considerably less at the conclusion of a vented CS experiment (Fig. 5C and D). DISCUSSION Intrathoracic tension physiology remains a significant contributor to trauma mortality, particularly in cases with penetrating or blast injury mechanisms. The current recommendation for management of penetrating thoracic injuries on the battlefield is to apply occlusive (unvented) CSs. 6 Since no supporting evidence existed, we investigated the effectiveness of a popular unvented CS (Halo) and compared it with a vented CS (Bolin) for treatment of PTx and prevention of tension PTx in a reproducible model of PTx in swine. Tension PTx that can develop in patients with chest/lung injury was replicated in the model by direct injection of air into the pleural cavity through a percutaneous intrapleural cannula that was also used to measure IP. This method was instrumental in determining the volume of air in the chest and the resulting IP that can lead to tension PTx in the presence of different CSs in pigs. The model also allowed easy correction of PTx by plugging the wound track and withdrawing air from the pleural cavity to reestablish physiologic IP and normalize respiratory and hemodynamic functions. Perhaps, the most valuable contribution of this model has been its focus on IP, rather than simply infusing 154 fixed gas volumes, both to induce and to measure the effects of tension PTx and potential mitigation strategies. Positive-pressure ventilation increases the likelihood of developmentoftensionptxinpatientswithlunginjury. 1 In this model, however, it was found to be protective because (a) there were no injuries to the lung and (b) positive-pressure ventilation by the automatic respirator overcame the positive IP and aerated the lungs efficiently. Therefore, experiments in this study were performed in spontaneously air breathing pigs, which also allowed observation of each animal s respiration efforts and measurement of their normal V T and RR and subsequent changes. This was consistent with prehospital care of combat casualties who are generally not intubated by medics. The position of the anesthetized animals also affected their respiratory efficiency. The supine position generally makes breathing more difficult for four-legged animals and is known to be associated with hypoxia and an increase in pulmonary vascular shunting. 13 Therefore, the experiments were performed after placing the pigs in a sternal recumbent position. Creating an open chest wound in the left thorax (free air movement in both directions) caused an immediate PTx that became evident as an increase in animal s respiration effort and partial collapse of its left lung (x-ray image). This PTx was associated with an immediate rise of IP (approaching 0 mm Hg), rapid increase in PAP, and rapid decreases in V T and oxygen saturation measures (SpO 2 and SvO 2 ). Hemodynamic measures (i.e., MAP, HR, CO), however, were not significantly changed 5 minutes after PTx. In this study, the duration of open chest wounds and PTx was limited to 5 minutes to mimic the time lapse that such chest injuries may be covered with a CS in the field. Longer PTx condition without CS application could have produced more significant effects on hemodynamic function. Application of CSs (with or without venting valve) 5 minutes after PTx eased breathing efforts, reestablished negative IP, and restored most respiratory and circulatory measures. Introduction of air into the pleural cavity, simulating airway leakage, produced widely different results. The unvented * 2013 Lippincott Williams & Wilkins
7 J Trauma Acute Care Surg Kheirabadi et al. Figure 5. Representative chest x-ray images of a pig subjected to PTx and treated with different CSs. The baseline (A) and final image (B) of the pig s lung when tension PTx was developed with unvented CS treatment. Note the significant deviation of the mediastinum after 1.4-L air injection. The baseline (C) and final image (D) of the same pig when treated with a vented CS and injected with maximum air volume (approximately 2.0 L). CS application led to the development of tension PTx (confirmed by chest x-ray images) in all instances after approximately 1.4-L air injection. This was associated with a steady increase in pulmonary vascular resistance (PAP j), decrease in lung capacity to support oxygenation (hypoxemia), and occasional respiratory arrest. In contrast, application of vented CS maintained IP near-normal levels despite repeated air injections (up to 2 L) and prevented tension PTx as defined previously. However, the chest x-ray images showed some degree of lung collapse and deviation of the mediastinum. These findings were consistent with a previous report where a one-way valve dressing was compared with occlusive gauze dressing in a canine model of open chest wound. Under spontaneously breathing condition, the one-way valve dressing was significantly more protective in preventing severe respiratory decompensation than the occlusive dressing. 14 As mentioned before, tension PTx was diagnosed in this study based on positive IP and significant changes in four of the following five parameters: V T, PAP, SvO 2, CO, and MAP. The two early predictors of tension PTx often were the 20% reduction in V T and 30% rise in PAP. The only noninvasive indicator of tension PTx was the declining SpO 2 as measured by pulse oximeter that paralleled with the changes in SvO 2. One parameter that frequently did not reach the critical level (20%,) was MAP. This was consistent with the conclusion that significant hypoxemia occurs early and precedes hypotension in swine with tension PTx. 15 HR was elevated from the time of the injury with only small increases before tension PTx occurred. Other investigators have used a 20% decrease of MAP or a 20% increase of HR as indicators of tension PTx in a similar model of PTx in swine but in a supine position. 16 Given these indicators, two vented CSs (Asherman and Bolin) were tested and found to be both protective against tension PTx, with no significant difference between the two products. This study has some limitations that need be addressed. First, penetrating chest trauma is often associated with lung perforation and air leak into the pleural cavity. The experimental model developed here, however, did not include lung injury, and air was introduced into pleural cavity via a catheter. Although this method may create a confounding variable and does not accurately mimic the penetrating open chest injury, we think that the model is still valid for evaluating CSs and determining their effects on treating PTx and tension PTx regardless of the source of PTx. Moreover, creating a reproducible lung injury with consistent airway leak is difficult and will require invasive chest procedure that could adversely impact the animal s spontaneous * 2013 Lippincott Williams & Wilkins 155
8 Kheirabadi et al. J Trauma Acute Care Surg respiration. Second, the model also did not include hemothorax, another important component of penetrating chest trauma, which increases the risk of tension physiology. This was not included to simplify the model and focus this initial study on PTx and tension PTx and the impacts of CS on these injury sequelae. How the presence of blood and air in pleural cavity will be mitigated by CSVprimarily vented CS since unvented CS are more likely to failvis the subject of our next study in which increasing volumes of blood as well as air will be injected. Third, the present model represents penetrating chest trauma in spontaneously breathing subjects, which is more relevant to combat casualties in the field. In the civilian setting where most patients sustain blunt chest trauma and have no open chest wounds, CS application is unnecessary. The risk of tension PTx may be higher in these patients if they get intubated and positively ventilated before arriving at hospitals. SUMMARY AND CONCLUSION We have developed a reproducible open PTx model in spontaneously air breathing pigs in the sternal recumbent position. This model was used to compare the effectiveness of an unvented CS, a more preferred and used in the US military, with a vented CS for treatment of PTx and prevention of tension PTx. We observed that both vented and unvented CSs provided immediate improvement in respiratory function and increased blood oxygenation when applied over open chest wounds. However, in the presence of additional PTx, the use of the unvented CS led to tension PTx, hypoxemia, and possible respiratory arrest. We contend that these observations are likely to translate to human patients and the application of an unvented CS without continued monitoring and the availability of a medical practitioner skilled in the identification and management of tension PTx and HemoPTx may actually increase morbidity and mortality. In contrast, the vented CS prevented increased IP and protected our subjects from tension PTx and its consequences. While further investigation into this issue is warranted, we recommend in the interim and based on these data and previous reports 14,16 that vented CS should be preferably used during combat casualty care, particularly in the interval before the presence of experienced emergency medical practitioners. AUTHORSHIP All authors were involved in the design of the study, methodology development, and preparation and review of the manuscript. B.S.K., I.B.T. and A.K. performed the surgical procedures, treatments, data collection, and analysis. B.S.K. drafted the manuscript. R.T.G., H.G.K. and M.A.D. contributed in interpretation, discussion, commentary, and editing of the manuscript. The study was initiated and conducted under L.H.B. s leadership with his continued support. ACKNOWLEDGMENT We sincerely thank our Veterinary Support Branch for their continued support in conducting these experiments, particularly Mrs. Shawn Chamrad for her excellent assistance in providing anesthesia. We also greatly appreciate the technical assistance by Dr. Adekoye Sanni. DISCLOSURE The funding for this work was provided solely by the US Army Medical Research and Materiel Command. REFERENCES 1. Peoples GE, Gerlinger T, Craig R, Burlingame B. Combat casualties in Afghanistan cared for by a single team during the initial phase of operation enduring freedom. Mil Med. 2005;170:462Y McPherson JJ, Feigin DS, Bellamy RF. Prevalence of tension pneumothorax in fatally wounded combat casualties. J Trauma. 2006;60:573Y Barton ED, Epperson M, Hoyt DB, et al. Prehospital needle aspiration and tube thoracostomy in trauma victims: a six-year experience with aeromedical crews. J Emerg Med. 1995;13:155Y Di Bartolomeo S, Sanson G, Nardi G, et al. A population-based study on pneumothorax in severely traumatized patients. JTrauma. 2001;51:677Y Leigh-Smith S, Harris T. Tension pneumothoraxvtime for a rethink? Emerg Med J. 2005;22:8Y Available at: Materials/TCCC-Guidelines pdf. Accessed November 30, Available at: NOMLLC-TCCC-Equipment-Evaluation-Summary pdf. Accessed November 30, Institute of Laboratory Animal Resources, National Research Council. Guide for the Care and Use of Laboratory Animals. Washington, DC: National Academy Press; Maloney JV Jr, Schmutzer KJ, Raschke E. Paradoxical respiration and pendelluft. J Thorac Cardiovasc Surg. 1961;41:291Y Kilburn KH. Cardiorespiratory effects of large pneumothorax in conscious and anesthetized dogs. J Appl Physiol. 1963;8:279Y Gustman P, Yerger L, Wanner A. Immediate cardiovascular effects of tension pneumothorax. Am Rev Respir Dis. 1983;127:171Y Holcomb JB, McManus JG, Kerr ST, Pusateri AE. Needle versus tube thoracostomy in a swine model of traumatic tension hemopneumothorax. Prehosp Emerg Care. 2009;13:18Y Rutherford RB, Hurt HH, Brickman RD Tubb JM. The pathophysiology of progressive tension pneumothorax. J Trauma. 1968;8:212Y Ruiz E, Lueders J, Peresen C. A one-way valve chest wound dressing: evaluation in a canine model of open chest wounds. Ann Emerg Med. 1993; 22:922, abstract. 15. Barton ED, Rhee P, Hutton KC, et al. The pathophysiology of tension pneumothorax in ventilated swine. J Emerg Med. 1997;15:147Y Arnaud F, Tomori T, Teranishi K, et al. Evaluation of chest seal performance in a swine model: comparison of Asherman vs. Bolin seal. Injury. 2008; 39:1082Y * 2013 Lippincott Williams & Wilkins
A ONE-WAY-VALVE CHEST WOUND DRESSING: EVALUATION IN A CANINE MODEL OF OPEN CHEST WOUNDS
 A ONE-WAY-VALVE CHEST WOUND DRESSING: EVALUATION IN A CANINE MODEL OF OPEN CHEST WOUNDS Ernest Ruiz, M.D., F.A.C.E.P. Assistant Professor of Surgery University of Minnesota Department of Emergency Medicine
A ONE-WAY-VALVE CHEST WOUND DRESSING: EVALUATION IN A CANINE MODEL OF OPEN CHEST WOUNDS Ernest Ruiz, M.D., F.A.C.E.P. Assistant Professor of Surgery University of Minnesota Department of Emergency Medicine
Evaluation of chest seal performance in a swine model. Comparison of Asherman vs. Bolin seal
 Evaluation of chest seal performance in a swine model. Comparison of Asherman vs. Bolin seal Françoise Arnaud 1, Toshiki Tomori 1, Kohsuke Teranishi 1, Joon Yun 2, Richard McCarron 1,3, Richard Mahon 2.
Evaluation of chest seal performance in a swine model. Comparison of Asherman vs. Bolin seal Françoise Arnaud 1, Toshiki Tomori 1, Kohsuke Teranishi 1, Joon Yun 2, Richard McCarron 1,3, Richard Mahon 2.
Imaging the Lung Under Pressure
 DISTRIBUTION STATEMENT A: Approved for public release; distribution is unlimited. Imaging the Lung Under Pressure Peter L. Tyack, Andreas Fahlman, Michael Moore, and Darlene Ketten Woods Hole Oceanographic
DISTRIBUTION STATEMENT A: Approved for public release; distribution is unlimited. Imaging the Lung Under Pressure Peter L. Tyack, Andreas Fahlman, Michael Moore, and Darlene Ketten Woods Hole Oceanographic
VENTILATORS PURPOSE OBJECTIVES
 VENTILATORS PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain a ventilator in the interfacility transfer environment. COGNITIVE OBJECTIVES
VENTILATORS PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain a ventilator in the interfacility transfer environment. COGNITIVE OBJECTIVES
Capnography in the Veterinary Technician Toolbox. Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA
 Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES
 GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
Chest Drains. All Covenant Health Intermediate Care Nursery staff. Needle Aspiration
 Approved by: Chest Drains Gail Cameron Director, Maternal, Neonatal & Child Health Programs Neonatal Nursery Policy & Procedures Manual : April 2013 Next Review April 2016 Dr. Ensenat Medical Director,
Approved by: Chest Drains Gail Cameron Director, Maternal, Neonatal & Child Health Programs Neonatal Nursery Policy & Procedures Manual : April 2013 Next Review April 2016 Dr. Ensenat Medical Director,
Mechanical Ventilation
 PROCEDURE - Page 1 of 5 Purpose Scope Physician's Order Indications Procedure Mechanical Artificial Ventilation refers to any methods to deliver volumes of gas into a patient's lungs over an extended period
PROCEDURE - Page 1 of 5 Purpose Scope Physician's Order Indications Procedure Mechanical Artificial Ventilation refers to any methods to deliver volumes of gas into a patient's lungs over an extended period
The physiological functions of respiration and circulation. Mechanics. exercise 7. Respiratory Volumes. Objectives
 exercise 7 Respiratory System Mechanics Objectives 1. To explain how the respiratory and circulatory systems work together to enable gas exchange among the lungs, blood, and body tissues 2. To define respiration,
exercise 7 Respiratory System Mechanics Objectives 1. To explain how the respiratory and circulatory systems work together to enable gas exchange among the lungs, blood, and body tissues 2. To define respiration,
ONLINE DATA SUPPLEMENT. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg
 APPENDIX 1 Appendix 1. Complete respiratory protocol. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg predicted body weight (PBW)) (NEJM 2000; 342
APPENDIX 1 Appendix 1. Complete respiratory protocol. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg predicted body weight (PBW)) (NEJM 2000; 342
Temporary Flying Restrictions Due to Exogenous Factors
 Army Regulation 40 8 Medical Services Temporary Flying Restrictions Due to Exogenous Factors Headquarters Department of the Army Washington, DC 17 August 1976 UNCLASSIFIED REPORT DOCUMENTATION PAGE Form
Army Regulation 40 8 Medical Services Temporary Flying Restrictions Due to Exogenous Factors Headquarters Department of the Army Washington, DC 17 August 1976 UNCLASSIFIED REPORT DOCUMENTATION PAGE Form
z Interim Report for May 2004 to October 2005 Aircrew Performance and Protection Branch Wright-Patterson AFB, OH AFRL-HE-WP-TP
 AFRL-HE-WP-TP-26-89 Neck Muscle Fatigue with Helmet-Mounted Systems Edward S. Eveland Joseph A. Pellettiere Air Force Research Laboratory LL September 26 z Interim Report for May 24 to October 25 (n 261124
AFRL-HE-WP-TP-26-89 Neck Muscle Fatigue with Helmet-Mounted Systems Edward S. Eveland Joseph A. Pellettiere Air Force Research Laboratory LL September 26 z Interim Report for May 24 to October 25 (n 261124
AFRL-RX-WP-TP
 AFRL-RX-WP-TP-2012-0215 REVERSE PRESSURE CAPABLE FINGER SEAL (PREPRINT) Nathan Gibson and Joe Yanof Honeywell International, Inc. JANUARY 2012. See additional restrictions described on inside pages STINFO
AFRL-RX-WP-TP-2012-0215 REVERSE PRESSURE CAPABLE FINGER SEAL (PREPRINT) Nathan Gibson and Joe Yanof Honeywell International, Inc. JANUARY 2012. See additional restrictions described on inside pages STINFO
Using SolidWorks & CFD to Create The Next Generation Airlocks
 Using SolidWorks & CFD to Create The Next Generation Airlocks Matthew Gaffney Mechanical Engineer Geo-Centers, INC US Army Natick Soldier Center Natick, MA 01760 508-233-5557 Matthew.gaffney@natick.army.mil
Using SolidWorks & CFD to Create The Next Generation Airlocks Matthew Gaffney Mechanical Engineer Geo-Centers, INC US Army Natick Soldier Center Natick, MA 01760 508-233-5557 Matthew.gaffney@natick.army.mil
This article discusses recent literature. Tension pneumothorax: are prehospital guidelines safe and what are the alternatives? Abstract.
 Tension pneumothorax: are prehospital guidelines safe and what are the alternatives? Phil Simons is a HART Paramedic for South East Coast Ambulance Service Email for correspondence: mailto:phil.simons@secamb.nhs.uk
Tension pneumothorax: are prehospital guidelines safe and what are the alternatives? Phil Simons is a HART Paramedic for South East Coast Ambulance Service Email for correspondence: mailto:phil.simons@secamb.nhs.uk
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Talmor D, Sarge T, Malhotra A, et al. Mechanical ventilation
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Talmor D, Sarge T, Malhotra A, et al. Mechanical ventilation
War Surgery Dr. Abdulwahid INTRODUCTION: AIRWAY, BREATHING
 War Surgery Dr. Abdulwahid INTRODUCTION: AIRWAY, BREATHING The aims of war surgery: Save life Avoid infectious complications Save limbs Minimize residual disability The outcome is influenced by: Type of
War Surgery Dr. Abdulwahid INTRODUCTION: AIRWAY, BREATHING The aims of war surgery: Save life Avoid infectious complications Save limbs Minimize residual disability The outcome is influenced by: Type of
AFRL-RH-WP-TR
 AFRL-RH-WP-TR-2016-0040 C-130J BREATHING RESISTANCE STUDY George W. Miller Air Force Research Laboratory Wright-Patterson Air Force Base, OH 45433 May 2016 Final Report STINFO COPY AIR FORCE RESEARCH LABORATORY
AFRL-RH-WP-TR-2016-0040 C-130J BREATHING RESISTANCE STUDY George W. Miller Air Force Research Laboratory Wright-Patterson Air Force Base, OH 45433 May 2016 Final Report STINFO COPY AIR FORCE RESEARCH LABORATORY
Initiation and Management of Airway Pressure Release Ventilation (APRV)
 Initiation and Management of Airway Pressure Release Ventilation (APRV) Eric Kriner RRT Pulmonary Critical Care Clinical Specialist Pulmonary Services Department Medstar Washington Hospital Center Disclosures
Initiation and Management of Airway Pressure Release Ventilation (APRV) Eric Kriner RRT Pulmonary Critical Care Clinical Specialist Pulmonary Services Department Medstar Washington Hospital Center Disclosures
Lung Volumes and Capacities
 Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
Introduction. Respiration. Chapter 10. Objectives. Objectives. The Respiratory System
 Introduction Respiration Chapter 10 The Respiratory System Provides a means of gas exchange between the environment and the body Plays a role in the regulation of acidbase balance during exercise Objectives
Introduction Respiration Chapter 10 The Respiratory System Provides a means of gas exchange between the environment and the body Plays a role in the regulation of acidbase balance during exercise Objectives
NOTE: If not used, provider must document reason(s) for deferring mechanical ventilation in a patient with an advanced airway
 APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
Respiratory System. Part 2
 Respiratory System Part 2 Respiration Exchange of gases between air and body cells Three steps 1. Ventilation 2. External respiration 3. Internal respiration Ventilation Pulmonary ventilation consists
Respiratory System Part 2 Respiration Exchange of gases between air and body cells Three steps 1. Ventilation 2. External respiration 3. Internal respiration Ventilation Pulmonary ventilation consists
Mechanical Ventilation
 Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
Pulmonary Circulation
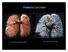 Pulmonary Circulation resin cast of pulmonary arteries resin cast of pulmonary veins Blood Flow to the Lungs Pulmonary Circulation Systemic Circulation Blood supply to the conducting zone provided by the
Pulmonary Circulation resin cast of pulmonary arteries resin cast of pulmonary veins Blood Flow to the Lungs Pulmonary Circulation Systemic Circulation Blood supply to the conducting zone provided by the
Examples of Carter Corrected DBDB-V Applied to Acoustic Propagation Modeling
 Naval Research Laboratory Stennis Space Center, MS 39529-5004 NRL/MR/7182--08-9100 Examples of Carter Corrected DBDB-V Applied to Acoustic Propagation Modeling J. Paquin Fabre Acoustic Simulation, Measurements,
Naval Research Laboratory Stennis Space Center, MS 39529-5004 NRL/MR/7182--08-9100 Examples of Carter Corrected DBDB-V Applied to Acoustic Propagation Modeling J. Paquin Fabre Acoustic Simulation, Measurements,
transients' of large amplitude can be imposed on the arterial, cardiac and Since both coughing and the Valsalva manoeuvre raise intrathoracic pressure
 351 J. Physiol. (I953) I22, 35I-357 EFFECTS OF COUGHING ON INTRATHORACIC PRESSURE, ARTERIAL PRESSURE AND PERIPHERAL BLOOD FLOW BY E. P. SHARPEY-SCHAFER From the Department of Medicine, St Thomas's Hospital
351 J. Physiol. (I953) I22, 35I-357 EFFECTS OF COUGHING ON INTRATHORACIC PRESSURE, ARTERIAL PRESSURE AND PERIPHERAL BLOOD FLOW BY E. P. SHARPEY-SCHAFER From the Department of Medicine, St Thomas's Hospital
Operating Instructions for Microprocessor Controlled Ventilators
 Page 1 of 5 Operating Instructions for Microprocessor Controlled Ventilators Purpose Audience Scope Physician's Order To provide guidelines for the procedure for the use of microprocessor controlled ventilators.
Page 1 of 5 Operating Instructions for Microprocessor Controlled Ventilators Purpose Audience Scope Physician's Order To provide guidelines for the procedure for the use of microprocessor controlled ventilators.
Selecting the Ventilator and the Mode. Chapter 6
 Selecting the Ventilator and the Mode Chapter 6 Criteria for Ventilator Selection Why does the patient need ventilatory support? Does the ventilation problem require a special mode? What therapeutic goals
Selecting the Ventilator and the Mode Chapter 6 Criteria for Ventilator Selection Why does the patient need ventilatory support? Does the ventilation problem require a special mode? What therapeutic goals
TITLE: Preclinical Evaluation of the Effects of Aeromedical Evacuation on Military- Relevant Casualties
 AWARD NUMBER: CDMRP-16-0-DM167040 TITLE: Preclinical Evaluation of the Effects of Aeromedical Evacuation on Military- Relevant Casualties PRINCIPAL INVESTIGATOR: Dr. Richard McCarron RECIPIENT: Naval Medical
AWARD NUMBER: CDMRP-16-0-DM167040 TITLE: Preclinical Evaluation of the Effects of Aeromedical Evacuation on Military- Relevant Casualties PRINCIPAL INVESTIGATOR: Dr. Richard McCarron RECIPIENT: Naval Medical
DoD Coral Reef Protection and Management Program
 DoD Coral Reef Protection and Management Program PROJECT TEAM U.S. NAVY TOM EGELAND (ASN(I&E)) LORRI SCHWARTZ (NAVFAC) ALEX VIANA (NFESC) STEVE SMITH (NFESC) BOSTON UNIV. MARINE PRG. PHILLIP LOBEL MINDY
DoD Coral Reef Protection and Management Program PROJECT TEAM U.S. NAVY TOM EGELAND (ASN(I&E)) LORRI SCHWARTZ (NAVFAC) ALEX VIANA (NFESC) STEVE SMITH (NFESC) BOSTON UNIV. MARINE PRG. PHILLIP LOBEL MINDY
Mechanical Ventilation. Which of the following is true regarding ventilation? Basics of Ventilation
 Mechanical Ventilation Jeffrey L. Wilt, MD, FACP, FCCP Associate Professor of Medicine Michigan State University Associate Program Director MSU-Grand Rapids Internal Medicine Residency Which of the following
Mechanical Ventilation Jeffrey L. Wilt, MD, FACP, FCCP Associate Professor of Medicine Michigan State University Associate Program Director MSU-Grand Rapids Internal Medicine Residency Which of the following
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 1 Chest Trauma LESSON ASSIGNMENT Paragraphs 1-1 through 1-13. LESSON OBJECTIVES After completing this lesson, you should be able to: 1-1. Identify common signs, common treatment,
LESSON ASSIGNMENT LESSON 1 Chest Trauma LESSON ASSIGNMENT Paragraphs 1-1 through 1-13. LESSON OBJECTIVES After completing this lesson, you should be able to: 1-1. Identify common signs, common treatment,
PICU Resident Self-Study Tutorial The Basic Physics of Oxygen Transport. I was told that there would be no math!
 Physiology of Oxygen Transport PICU Resident Self-Study Tutorial I was told that there would be no math! INTRODUCTION Christopher Carroll, MD Although cells rely on oxygen for aerobic metabolism and viability,
Physiology of Oxygen Transport PICU Resident Self-Study Tutorial I was told that there would be no math! INTRODUCTION Christopher Carroll, MD Although cells rely on oxygen for aerobic metabolism and viability,
Prehospital Hemorrhage Control and Resuscitation
 Prehospital Hemorrhage Control and Resuscitation John B. Holcomb, MD, FACS Professor of Surgery Chief, Division of Acute Care Surgery Director, Center for Translational Injury Research University of Texas
Prehospital Hemorrhage Control and Resuscitation John B. Holcomb, MD, FACS Professor of Surgery Chief, Division of Acute Care Surgery Director, Center for Translational Injury Research University of Texas
M2.50-cal. Multishot Capabilities at the US Army Research Laboratory
 ARL-TN-0694 SEP 2015 US Army Research Laboratory M2.50-cal. Multishot Capabilities at the US Army Research Laboratory by Todd Brinkman Approved for public release; distribution is unlimited. NOTICES Disclaimers
ARL-TN-0694 SEP 2015 US Army Research Laboratory M2.50-cal. Multishot Capabilities at the US Army Research Laboratory by Todd Brinkman Approved for public release; distribution is unlimited. NOTICES Disclaimers
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: CHEST TUBES-- ADULTS Nursing DATE: REVIEWED: PAGES: RESPONSIBILITY: RN, LPN 11/86 12/18 1 of 8 PURPOSE: To provide information and establish
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: CHEST TUBES-- ADULTS Nursing DATE: REVIEWED: PAGES: RESPONSIBILITY: RN, LPN 11/86 12/18 1 of 8 PURPOSE: To provide information and establish
INTRODUCTION TO BI-VENT (APRV) INTRODUCTION TO BI-VENT (APRV) PROGRAM OBJECTIVES
 INTRODUCTION TO BI-VENT (APRV) INTRODUCTION TO BI-VENT (APRV) PROGRAM OBJECTIVES PROVIDE THE DEFINITION FOR BI-VENT EXPLAIN THE BENEFITS OF BI-VENT EXPLAIN SET PARAMETERS IDENTIFY RECRUITMENT IN APRV USING
INTRODUCTION TO BI-VENT (APRV) INTRODUCTION TO BI-VENT (APRV) PROGRAM OBJECTIVES PROVIDE THE DEFINITION FOR BI-VENT EXPLAIN THE BENEFITS OF BI-VENT EXPLAIN SET PARAMETERS IDENTIFY RECRUITMENT IN APRV USING
Monitoring, Ventilation & Capnography
 Why do we need to monitor? Monitoring, Ventilation & Capnography Keith Simpson BVSc MRCVS MIET(Electronics) Torquay, Devon. Under anaesthesia animals no longer have the ability to adequately control their
Why do we need to monitor? Monitoring, Ventilation & Capnography Keith Simpson BVSc MRCVS MIET(Electronics) Torquay, Devon. Under anaesthesia animals no longer have the ability to adequately control their
Internal Waves and Mixing in the Aegean Sea
 Internal Waves and Mixing in the Aegean Sea Michael C. Gregg Applied Physics Laboratory, University of Washington 1013 NE 40 th St. Seattle, WA 98105-6698 phone: (206) 543-1353 fax: (206) 543-6785 email:
Internal Waves and Mixing in the Aegean Sea Michael C. Gregg Applied Physics Laboratory, University of Washington 1013 NE 40 th St. Seattle, WA 98105-6698 phone: (206) 543-1353 fax: (206) 543-6785 email:
SUPPLEMENTARY APPENDIX. Ary Serpa Neto MD MSc, Fabienne D Simonis MD, Carmen SV Barbas MD PhD, Michelle Biehl MD, Rogier M Determann MD PhD, Jonathan
 1 LUNG PROTECTIVE VENTILATION WITH LOW TIDAL VOLUMES AND THE OCCURRENCE OF PULMONARY COMPLICATIONS IN PATIENTS WITHOUT ARDS: a systematic review and individual patient data metaanalysis SUPPLEMENTARY APPENDIX
1 LUNG PROTECTIVE VENTILATION WITH LOW TIDAL VOLUMES AND THE OCCURRENCE OF PULMONARY COMPLICATIONS IN PATIENTS WITHOUT ARDS: a systematic review and individual patient data metaanalysis SUPPLEMENTARY APPENDIX
VENTILATION AND PERFUSION IN HEALTH AND DISEASE. Dr.HARIPRASAD VS
 VENTILATION AND PERFUSION IN HEALTH AND DISEASE Dr.HARIPRASAD VS Ventilation Total ventilation - total rate of air flow in and out of the lung during normal tidal breathing. Alveolar ventilation -represents
VENTILATION AND PERFUSION IN HEALTH AND DISEASE Dr.HARIPRASAD VS Ventilation Total ventilation - total rate of air flow in and out of the lung during normal tidal breathing. Alveolar ventilation -represents
EMD CPR. The First First Responder. R. Darrell Nelson, MD, FACEP
 EMD CPR The First First Responder R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Baptist Health Medical Director, Davie and Stokes County EMS Assistant Medical Director, Forsyth
EMD CPR The First First Responder R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Baptist Health Medical Director, Davie and Stokes County EMS Assistant Medical Director, Forsyth
Stability & Control Aspects of UCAV Configurations
 Stability & Control Aspects of UCAV Configurations Paul Flux Senior Aerodynamicist BAE SYSTEMS Air Programmes Report Documentation Page Form Approved OMB No. 0704-0188 Public reporting burden for the collection
Stability & Control Aspects of UCAV Configurations Paul Flux Senior Aerodynamicist BAE SYSTEMS Air Programmes Report Documentation Page Form Approved OMB No. 0704-0188 Public reporting burden for the collection
UNITED STATES MARINE CORPS FIELD MEDICAL TRAINING BATTALION Camp Lejeune, NC
 UNITED STATES MARINE CORPS FIELD MEDICAL TRAINING BATTALION Camp Lejeune, NC 28542-0042 FMST 504 Conduct Triage TERMINAL LEARNING OBJECTIVES 1. Given multiple casualties in a tactical environment, conduct
UNITED STATES MARINE CORPS FIELD MEDICAL TRAINING BATTALION Camp Lejeune, NC 28542-0042 FMST 504 Conduct Triage TERMINAL LEARNING OBJECTIVES 1. Given multiple casualties in a tactical environment, conduct
Tactical Emergency Casualty Care (TECC) First Care Provider Guidelines
 Adopted from The Committee for TECC: Current as of June 2016 DIRECT THREAT CARE (DTC) / HOT ZONE GUIDELINES 1. In the presence of a direct threat to life, take definitive action towards mitigating that
Adopted from The Committee for TECC: Current as of June 2016 DIRECT THREAT CARE (DTC) / HOT ZONE GUIDELINES 1. In the presence of a direct threat to life, take definitive action towards mitigating that
Advanced Ventilator Modes. Shekhar T. Venkataraman M.D. Professor Critical Care Medicine and Pediatrics University of Pittsburgh School of Medicine
 Advanced Ventilator Modes Shekhar T. Venkataraman M.D. Shekhar T. Venkataraman M.D. Professor Critical Care Medicine and Pediatrics University of Pittsburgh School of Medicine Advanced modes Pressure-Regulated
Advanced Ventilator Modes Shekhar T. Venkataraman M.D. Shekhar T. Venkataraman M.D. Professor Critical Care Medicine and Pediatrics University of Pittsburgh School of Medicine Advanced modes Pressure-Regulated
excellence in care Procedure Management of patients with difficult oxygenation. For Review Aug 2015
 Difficult Oxygenation HELI.CLI.12 Purpose This procedure describes the processes and procedures for a lung protective strategy in the mechanical ventilation of patients that are difficult to oxygenate
Difficult Oxygenation HELI.CLI.12 Purpose This procedure describes the processes and procedures for a lung protective strategy in the mechanical ventilation of patients that are difficult to oxygenate
Closed Loop Control of Oxygen Delivery and Oxygen Generation
 AFRL-SA-WP-SR-2017-0024 Closed Loop Control of Oxygen Delivery and Oxygen Generation Dr. Jay Johannigman 1, Richard Branson 1, Thomas C. Blakeman 1, Dario Rodriquez 1,2 1 University of Cincinnati; 2 Aeromedical
AFRL-SA-WP-SR-2017-0024 Closed Loop Control of Oxygen Delivery and Oxygen Generation Dr. Jay Johannigman 1, Richard Branson 1, Thomas C. Blakeman 1, Dario Rodriquez 1,2 1 University of Cincinnati; 2 Aeromedical
Circulatory And Respiration
 Circulatory And Respiration Composition Of Blood Blood Heart 200mmHg 120mmHg Aorta Artery Arteriole 50mmHg Capillary Bed Venule Vein Vena Cava Heart Differences Between Arteries and Veins Veins transport
Circulatory And Respiration Composition Of Blood Blood Heart 200mmHg 120mmHg Aorta Artery Arteriole 50mmHg Capillary Bed Venule Vein Vena Cava Heart Differences Between Arteries and Veins Veins transport
General indications for ex vivo lung perfusion (EVLP) are
 Ex Vivo Lung Perfusion Marcelo Cypel, MD, MSc, and Shaf Keshavjee, MD, MSc The number of patients listed for lung transplantation largely exceeds the number of available transplantable organs because of
Ex Vivo Lung Perfusion Marcelo Cypel, MD, MSc, and Shaf Keshavjee, MD, MSc The number of patients listed for lung transplantation largely exceeds the number of available transplantable organs because of
Chapter 4: Ventilation Test Bank MULTIPLE CHOICE
 Instant download and all chapters Test Bank Respiratory Care Anatomy and Physiology Foundations for Clinical Practice 3rd Edition Will Beachey https://testbanklab.com/download/test-bank-respiratory-care-anatomy-physiologyfoundations-clinical-practice-3rd-edition-will-beachey/
Instant download and all chapters Test Bank Respiratory Care Anatomy and Physiology Foundations for Clinical Practice 3rd Edition Will Beachey https://testbanklab.com/download/test-bank-respiratory-care-anatomy-physiologyfoundations-clinical-practice-3rd-edition-will-beachey/
REPORT DOCUMENTATION PAGE
 REPORT DOCUMENTATION PAGE Form Approved OMB NO. 0704-0188 The public reporting burden for this collection of information is estimated to average 1 hour per response, including the time for reviewing instructions,
REPORT DOCUMENTATION PAGE Form Approved OMB NO. 0704-0188 The public reporting burden for this collection of information is estimated to average 1 hour per response, including the time for reviewing instructions,
AN EXPERIMENTAL INVESTIGATION OF SPILLING BREAKERS
 AN EXPERIMENTAL INVESTIGATION OF SPILLING BREAKERS Prof. James H. Duncan Department of Mechanical Engineering University of Maryland College Park, Maryland 20742-3035 phone: (301) 405-5260, fax: (301)
AN EXPERIMENTAL INVESTIGATION OF SPILLING BREAKERS Prof. James H. Duncan Department of Mechanical Engineering University of Maryland College Park, Maryland 20742-3035 phone: (301) 405-5260, fax: (301)
Hypoxia Following Rapid Decompression to 18,288 m (60,000 ft) Attributable to Alveolar Hypoventilation
 Hypoxia Following Rapid Decompression to 18,288 m (60,000 ft) Attributable to Alveolar Hypoventilation Desmond M Connolly PhD QinetiQ Aircrew Systems Senior Medical Officer Timothy J D Oyly BSc Amanda
Hypoxia Following Rapid Decompression to 18,288 m (60,000 ft) Attributable to Alveolar Hypoventilation Desmond M Connolly PhD QinetiQ Aircrew Systems Senior Medical Officer Timothy J D Oyly BSc Amanda
AT Kelly Torso. Directions for Use
 AT Kelly Torso Directions for Use 260-00001 2 Table of Contents Recommends 4 Items Included 5 Skills Taught 5 Preparing the Manikin for Use 6 Head 6 Lungs 6 Abdominal Thrust 6 Instructions for Use 6 Airway
AT Kelly Torso Directions for Use 260-00001 2 Table of Contents Recommends 4 Items Included 5 Skills Taught 5 Preparing the Manikin for Use 6 Head 6 Lungs 6 Abdominal Thrust 6 Instructions for Use 6 Airway
Let s talk about Capnography
 Let s talk about Capnography This is one of a series of articles by Keith Simpson BVSc MRCVS MIET (Electronics) discussing the practical aspects of some common monitoring techniques. Capnometry is the
Let s talk about Capnography This is one of a series of articles by Keith Simpson BVSc MRCVS MIET (Electronics) discussing the practical aspects of some common monitoring techniques. Capnometry is the
SECOND EUROPEAN CONSENSUS CONFERENCE ON HYPERBARIC MEDICINE THE TREATMENT OF DECOMPRESSION ACCIDENTS IN RECREATIONAL DIVING
 SECOND EUROPEAN CONSENSUS CONFERENCE ON HYPERBARIC MEDICINE THE TREATMENT OF DECOMPRESSION ACCIDENTS IN RECREATIONAL DIVING MARSEILLE, May 8-10, 1996 RECOMMENDATIONS OF THE JURY* QUESTION 1 : Is there
SECOND EUROPEAN CONSENSUS CONFERENCE ON HYPERBARIC MEDICINE THE TREATMENT OF DECOMPRESSION ACCIDENTS IN RECREATIONAL DIVING MARSEILLE, May 8-10, 1996 RECOMMENDATIONS OF THE JURY* QUESTION 1 : Is there
Respiratory Physiology. Adeyomoye O.I
 Respiratory Physiology By Adeyomoye O.I Outline Introduction Hypoxia Dyspnea Control of breathing Ventilation/perfusion ratios Respiratory/barometric changes in exercise Intra-pulmonary & intra-pleural
Respiratory Physiology By Adeyomoye O.I Outline Introduction Hypoxia Dyspnea Control of breathing Ventilation/perfusion ratios Respiratory/barometric changes in exercise Intra-pulmonary & intra-pleural
Clinical Skills. Administering Oxygen
 Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
Activity 2: Examining the Effect of Changing Airway Resistance on Respiratory Volumes
 1 BGYC34 PhysioEx Lab 7 Respiratory Systems Mechanics Marking Scheme Part 1 Complete PhysioEx lab #7. Hand-in all of the pages associated with the lab. Note that there are 5 activities to be completed.
1 BGYC34 PhysioEx Lab 7 Respiratory Systems Mechanics Marking Scheme Part 1 Complete PhysioEx lab #7. Hand-in all of the pages associated with the lab. Note that there are 5 activities to be completed.
From First Care Provider Trauma
 From First Care Provider Trauma Trauma presents unique challenges to the rescuer. When trauma happens, time is critical; therefore, it s best to have an easy to follow, validated procedure in place. The
From First Care Provider Trauma Trauma presents unique challenges to the rescuer. When trauma happens, time is critical; therefore, it s best to have an easy to follow, validated procedure in place. The
Respiratory Physiology Gaseous Exchange
 Respiratory Physiology Gaseous Exchange Session Objectives. What you will cover Basic anatomy of the lung including airways Breathing movements Lung volumes and capacities Compliance and Resistance in
Respiratory Physiology Gaseous Exchange Session Objectives. What you will cover Basic anatomy of the lung including airways Breathing movements Lung volumes and capacities Compliance and Resistance in
Standards and guidelines for care and management of patients requiring oxygen therapy.
 PURPOSE Standards and guidelines for care and management of patients requiring oxygen therapy. STANDARDS Ongoing management of oxygen therapy requires a prescriber s order. The order must specify oxygen
PURPOSE Standards and guidelines for care and management of patients requiring oxygen therapy. STANDARDS Ongoing management of oxygen therapy requires a prescriber s order. The order must specify oxygen
Tactical Emergency Casualty Care (TECC)
 Tactical Emergency Casualty Care (TECC) Guidelines For First Care Providers Current as of June 2016 DIRECT THREAT CARE (DTC) / HOT ZONE GUIDELINES 1) In the presence of a direct threat to life, take definitive
Tactical Emergency Casualty Care (TECC) Guidelines For First Care Providers Current as of June 2016 DIRECT THREAT CARE (DTC) / HOT ZONE GUIDELINES 1) In the presence of a direct threat to life, take definitive
Tactical Combat Casualty Care Guidelines for All Combatants
 Tactical Combat Casualty Care Guidelines for All Combatants August 2017 (Based on TCCC Guidelines for Medical Personnel 170131) These recommendations are intended to be guidelines only and are not a substitute
Tactical Combat Casualty Care Guidelines for All Combatants August 2017 (Based on TCCC Guidelines for Medical Personnel 170131) These recommendations are intended to be guidelines only and are not a substitute
4/18/12 MECHANISM OF RESPIRATION. Every Breath You Take. Fun Facts
 Objectives MECHANISM OF RESPIRATION Dr Badri Paudel Explain how the intrapulmonary and intrapleural pressures vary during ventilation and relate these pressure changes to Boyle s law. Define the terms
Objectives MECHANISM OF RESPIRATION Dr Badri Paudel Explain how the intrapulmonary and intrapleural pressures vary during ventilation and relate these pressure changes to Boyle s law. Define the terms
Ventilating the Sick Lung Mike Dougherty RRT-NPS
 Ventilating the Sick Lung 2018 Mike Dougherty RRT-NPS Goals and Objectives Discuss some Core Principles of Ventilation relevant to mechanical ventilation moving forward. Compare and Contrast High MAP strategies
Ventilating the Sick Lung 2018 Mike Dougherty RRT-NPS Goals and Objectives Discuss some Core Principles of Ventilation relevant to mechanical ventilation moving forward. Compare and Contrast High MAP strategies
Kelly Legault, Ph.D., P.E. USACE SAJ
 Kelly Legault, Ph.D., P.E. USACE SAJ Report Documentation Page Form Approved OMB No. 0704-0188 Public reporting burden for the collection of information is estimated to average 1 hour per response, including
Kelly Legault, Ph.D., P.E. USACE SAJ Report Documentation Page Form Approved OMB No. 0704-0188 Public reporting burden for the collection of information is estimated to average 1 hour per response, including
Waves, Bubbles, Noise, and Underwater Communications
 Waves, Bubbles, Noise, and Underwater Communications Grant B. Deane Marine Physical Laboratory, Scripps Institution of Oceanography UCSD, La Jolla, CA 92093-0238 phone: (858) 534-0536 fax: (858) 534-7641
Waves, Bubbles, Noise, and Underwater Communications Grant B. Deane Marine Physical Laboratory, Scripps Institution of Oceanography UCSD, La Jolla, CA 92093-0238 phone: (858) 534-0536 fax: (858) 534-7641
CHAPTER 6. Oxygen Transport. Copyright 2008 Thomson Delmar Learning
 CHAPTER 6 Oxygen Transport Normal Blood Gas Value Ranges Table 6-1 OXYGEN TRANSPORT Oxygen Dissolved in the Blood Plasma Dissolve means that the gas maintains its precise molecular structure About.003
CHAPTER 6 Oxygen Transport Normal Blood Gas Value Ranges Table 6-1 OXYGEN TRANSPORT Oxygen Dissolved in the Blood Plasma Dissolve means that the gas maintains its precise molecular structure About.003
The Basics of Ventilator Management. Overview. How we breath 3/23/2019
 The Basics of Ventilator Management What are we really trying to do here Peter Lutz, MD Pulmonary and Critical Care Medicine Pulmonary Associates, Mobile, Al Overview Approach to the physiology of the
The Basics of Ventilator Management What are we really trying to do here Peter Lutz, MD Pulmonary and Critical Care Medicine Pulmonary Associates, Mobile, Al Overview Approach to the physiology of the
Completed downloadable Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 5th Edition by Cairo
 Completed downloadable Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 5th Edition by Cairo Link full download: http://testbankcollection.com/download/pilbeams-mechanicalventilation-physiological-and-clinical-applications-5th-edition-test-bank-cairo
Completed downloadable Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 5th Edition by Cairo Link full download: http://testbankcollection.com/download/pilbeams-mechanicalventilation-physiological-and-clinical-applications-5th-edition-test-bank-cairo
ROUTINE PREOXYGENATION
 EDITORIAL ROUTINE PREOXYGENATION It is a fact of great clinical importance that the body oxygen stores are so small, and if replenishment ceases, they are normally insufficient to sustain life for more
EDITORIAL ROUTINE PREOXYGENATION It is a fact of great clinical importance that the body oxygen stores are so small, and if replenishment ceases, they are normally insufficient to sustain life for more
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress NURSES SETTING UP FOR ANAESTHESIA HOW TO PLAN FOR A SAFE ANAESTHETIC Sandra Forysth, BVSc DipACVA Institute of
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress NURSES SETTING UP FOR ANAESTHESIA HOW TO PLAN FOR A SAFE ANAESTHETIC Sandra Forysth, BVSc DipACVA Institute of
Difficult Oxygenation Distribution: Sydney X Illawarra X Orange X
 HELICOPTER OPERATING PROCEDURE HOP No: C/12 Issued: May 2011 Page: 1 of 5 Revision No: Original Difficult Oxygenation Distribution: Sydney X Illawarra X Orange X TRIM No: 09/300 Document No: D10/9973 X
HELICOPTER OPERATING PROCEDURE HOP No: C/12 Issued: May 2011 Page: 1 of 5 Revision No: Original Difficult Oxygenation Distribution: Sydney X Illawarra X Orange X TRIM No: 09/300 Document No: D10/9973 X
APRV: Moving beyond ARDSnet
 APRV: Moving beyond ARDSnet Matthew Lissauer, MD Associate Professor of Surgery Medical Director, Surgical Critical Care Rutgers, The State University of New Jersey What is APRV? APRV is different from
APRV: Moving beyond ARDSnet Matthew Lissauer, MD Associate Professor of Surgery Medical Director, Surgical Critical Care Rutgers, The State University of New Jersey What is APRV? APRV is different from
6 th Accredited Advanced Mechanical Ventilation Course for Anesthesiologists. Course Test Results for the accreditation of the acquired knowledge
 6 th Accredited Advanced Mechanical Ventilation Course for Anesthesiologists Course Test Results for the accreditation of the acquired knowledge Q. Concerning the mechanics of the newborn s respiratory
6 th Accredited Advanced Mechanical Ventilation Course for Anesthesiologists Course Test Results for the accreditation of the acquired knowledge Q. Concerning the mechanics of the newborn s respiratory
Waves, Turbulence and Boundary Layers
 Waves, Turbulence and Boundary Layers George L. Mellor Program in Atmospheric and Oceanic Sciences Princeton University Princeton NJ 8544-71 phone: (69) 258-657 fax: (69) 258-285 email: glm@splash.princeton.edu
Waves, Turbulence and Boundary Layers George L. Mellor Program in Atmospheric and Oceanic Sciences Princeton University Princeton NJ 8544-71 phone: (69) 258-657 fax: (69) 258-285 email: glm@splash.princeton.edu
TITLE: Assessing the Hydrodynamic Performance of Fouling-Release Surfaces (ONR Research Contract # N WR )
 TITLE: Assessing the Hydrodynamic Performance of Fouling-Release Surfaces (ONR Research Contract # N00014-07-WR-2-0213) INVESTIGATOR: Associate Professor Michael P. Schultz, Naval Architecture & Ocean
TITLE: Assessing the Hydrodynamic Performance of Fouling-Release Surfaces (ONR Research Contract # N00014-07-WR-2-0213) INVESTIGATOR: Associate Professor Michael P. Schultz, Naval Architecture & Ocean
Development of Low Volume Shape Memory Alloy Variable Ballast System for AUV Use
 Development of Low Volume Shape Memory Alloy Variable Ballast System for AUV Use Dr. Graeme J Rae Ocean Engineering Program Division of Marine and Environmental Systems Florida Institute of Technology
Development of Low Volume Shape Memory Alloy Variable Ballast System for AUV Use Dr. Graeme J Rae Ocean Engineering Program Division of Marine and Environmental Systems Florida Institute of Technology
Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo
 Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo Link full download: http://testbankair.com/download/test-bank-for-pilbeams-mechanicalventilation-physiological-and-clinical-applications-6th-edition-by-cairo/
Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo Link full download: http://testbankair.com/download/test-bank-for-pilbeams-mechanicalventilation-physiological-and-clinical-applications-6th-edition-by-cairo/
Air-Sea Interaction Spar Buoy Systems
 DISTRIBUTION STATEMENT A: Distribution approved for public release; distribution is unlimited Air-Sea Interaction Spar Buoy Systems Hans C. Graber CSTARS - University of Miami 11811 SW 168 th Street, Miami,
DISTRIBUTION STATEMENT A: Distribution approved for public release; distribution is unlimited Air-Sea Interaction Spar Buoy Systems Hans C. Graber CSTARS - University of Miami 11811 SW 168 th Street, Miami,
Notes on BIPAP/CPAP. M.Berry Emergency physician St Vincent s Hospital, Sydney
 Notes on BIPAP/CPAP M.Berry Emergency physician St Vincent s Hospital, Sydney 2 DEFINITIONS Non-Invasive Positive Pressure Ventilation (NIPPV) Encompasses both CPAP and BiPAP Offers ventilation support
Notes on BIPAP/CPAP M.Berry Emergency physician St Vincent s Hospital, Sydney 2 DEFINITIONS Non-Invasive Positive Pressure Ventilation (NIPPV) Encompasses both CPAP and BiPAP Offers ventilation support
AT Kelly Torso. Directions for Use
 AT Kelly Torso Directions for Use Table of Contents Recommends 4 Items Included 5 Skills Taught 5 Preparing the Manikin for Use 6 Head 6 Lungs 6 Abdominal Thrust 6 Instructions for Use 6 Airway Management
AT Kelly Torso Directions for Use Table of Contents Recommends 4 Items Included 5 Skills Taught 5 Preparing the Manikin for Use 6 Head 6 Lungs 6 Abdominal Thrust 6 Instructions for Use 6 Airway Management
TRANSCUTANEOUS CO2 MONITORING (TCpCO2) PURPOSE
 PURPOSE tcpco2 monitoring provides continuous non invasive monitoring of an infant s ventilatory status. The sensor consists of a Stow-Severinghaus-type electrode. The use of tcpco2 monitoring may facilitate
PURPOSE tcpco2 monitoring provides continuous non invasive monitoring of an infant s ventilatory status. The sensor consists of a Stow-Severinghaus-type electrode. The use of tcpco2 monitoring may facilitate
DEVELOPMENT OF PRIMARY FRAGMENTATION SEPARATION DISTANCES FOR CASED CYLINDRICAL MUNITIONS
 DEVELOPMENT OF PRIMARY FRAGMENTATION SEPARATION DISTANCES FOR CASED CYLINDRICAL MUNITIONS by William H. Zehrt, Jr., P. E. and Michelle M. Crull, PhD, P. E. U. S. Army Engineering and Support Center, Huntsville
DEVELOPMENT OF PRIMARY FRAGMENTATION SEPARATION DISTANCES FOR CASED CYLINDRICAL MUNITIONS by William H. Zehrt, Jr., P. E. and Michelle M. Crull, PhD, P. E. U. S. Army Engineering and Support Center, Huntsville
PROBLEM SET 9. SOLUTIONS April 23, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Endotracheal Suctioning: In Line ETT
 Approved by: Endotracheal Suctioning: In Line ETT Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures
Approved by: Endotracheal Suctioning: In Line ETT Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures
OXYGEN THERAPY. (Non-invasive O2 therapy in patient >8yrs)
 OXYGEN THERAPY (Non-invasive O2 therapy in patient >8yrs) Learning aims Indications and precautions for O2 therapy Targets of therapy Standard notation O2 delivery devices Taps, tanks and tubing Notation
OXYGEN THERAPY (Non-invasive O2 therapy in patient >8yrs) Learning aims Indications and precautions for O2 therapy Targets of therapy Standard notation O2 delivery devices Taps, tanks and tubing Notation
Remote Monitoring of Dolphins and Whales in the High Naval Activity Areas in Hawaiian Waters
 DISTRIBUTION STATEMENT A: Approved for public release; distribution is unlimited. Remote Monitoring of Dolphins and Whales in the High Naval Activity Areas in Hawaiian Waters Whitlow W. L. Au and Marc
DISTRIBUTION STATEMENT A: Approved for public release; distribution is unlimited. Remote Monitoring of Dolphins and Whales in the High Naval Activity Areas in Hawaiian Waters Whitlow W. L. Au and Marc
Neonatal tidal volume targeted ventilation
 Neonatal tidal volume targeted ventilation Colin Morley Retired Professor of Neonatal Medicine, Royal Women s Hospital, Melbourne, Australia. Honorary Visiting Fellow, Dept Obstetrics and Gynaecology,
Neonatal tidal volume targeted ventilation Colin Morley Retired Professor of Neonatal Medicine, Royal Women s Hospital, Melbourne, Australia. Honorary Visiting Fellow, Dept Obstetrics and Gynaecology,
SEP-1 Additional Notes for Abstraction for Version 5.0b
 SEP-1 Additional Notes for Abstraction for Version 5.0b Data Element Administrative Contraindication to Care Blood Culture Collection Date Blood Culture Collection Time Broad Spectrum or Other Antibiotic
SEP-1 Additional Notes for Abstraction for Version 5.0b Data Element Administrative Contraindication to Care Blood Culture Collection Date Blood Culture Collection Time Broad Spectrum or Other Antibiotic
Basics of Mechanical Ventilation. Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity
 Basics of Mechanical Ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Overview of topics 1. Goals 2. Settings 3. Modes 4. Advantages and disadvantages
Basics of Mechanical Ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Overview of topics 1. Goals 2. Settings 3. Modes 4. Advantages and disadvantages
Principles of mechanical ventilation. Anton van Kaam, MD, PhD Emma Children s Hospital AMC Amsterdam, The Netherlands
 Principles of mechanical ventilation Anton van Kaam, MD, PhD Emma Children s Hospital AMC Amsterdam, The Netherlands Disclosure Research grant Chiesi Pharmaceuticals Research grant CareFusion GA: 27 weeks,
Principles of mechanical ventilation Anton van Kaam, MD, PhD Emma Children s Hospital AMC Amsterdam, The Netherlands Disclosure Research grant Chiesi Pharmaceuticals Research grant CareFusion GA: 27 weeks,
Medical Ventilators. Presented by: Edwin Lim
 Medical Ventilators Presented by: Edwin Lim 1 Presentation Outline Respiration and You Medical Ventilators: Why? How? Current Medical Ventilators The Future 2 The Importance of Oxygen People can survive
Medical Ventilators Presented by: Edwin Lim 1 Presentation Outline Respiration and You Medical Ventilators: Why? How? Current Medical Ventilators The Future 2 The Importance of Oxygen People can survive
Respiration (revised 2006) Pulmonary Mechanics
 Respiration (revised 2006) Pulmonary Mechanics PUL 1. Diagram how pleural pressure, alveolar pressure, airflow, and lung volume change during a normal quiet breathing cycle. Identify on the figure the
Respiration (revised 2006) Pulmonary Mechanics PUL 1. Diagram how pleural pressure, alveolar pressure, airflow, and lung volume change during a normal quiet breathing cycle. Identify on the figure the
Respiratory Physiology 2
 Respiratory Physiology 2 Session Objectives. What you will cover Gaseous Exchange Control of Breathing Rate Your objectives are State the function of support structures and epithelia of the bronchial tree
Respiratory Physiology 2 Session Objectives. What you will cover Gaseous Exchange Control of Breathing Rate Your objectives are State the function of support structures and epithelia of the bronchial tree
Simulation 10: 27 Year-Old Male Trauma Patient
 Simulation 10: 27 Year-Old Male Trauma Patient Flow Chart Opening Scenario Section 1 Type: IG Handed off 27 YO male with blunt chest trauma/pulmonary contusions on PC A/C ventilation; PIP = 30 cm H2O,
Simulation 10: 27 Year-Old Male Trauma Patient Flow Chart Opening Scenario Section 1 Type: IG Handed off 27 YO male with blunt chest trauma/pulmonary contusions on PC A/C ventilation; PIP = 30 cm H2O,
RESPIRATORY PHYSIOLOGY. Anaesthesiology Block 18 (GNK 586) Prof Pierre Fourie
 RESPIRATORY PHYSIOLOGY Anaesthesiology Block 18 (GNK 586) Prof Pierre Fourie Outline Ventilation Diffusion Perfusion Ventilation-Perfusion relationship Work of breathing Control of Ventilation 2 This image
RESPIRATORY PHYSIOLOGY Anaesthesiology Block 18 (GNK 586) Prof Pierre Fourie Outline Ventilation Diffusion Perfusion Ventilation-Perfusion relationship Work of breathing Control of Ventilation 2 This image
