Imposed Power of Breathing Associated With Use of an Impedance Threshold Device
|
|
|
- Arleen Davidson
- 6 years ago
- Views:
Transcription
1 Imposed Power of Breathing Associated With Use of an Impedance Threshold Device Ahamed H Idris MD, Victor A Convertino PhD, Duane A Ratliff MSc, Donald F Doerr MSc, Keith G Lurie MD, Andrea Gabrielli MD, and Michael J Banner PhD OBJECTIVE: To measure the imposed power of breathing (imposed work of breathing per minute) associated with spontaneous breathing through an active impedance threshold device and a sham impedance threshold device. DESIGN: Prospective randomized blinded protocol. SETTING: University medical center. PATIENTS: Nineteen healthy, normotensive volunteers (10 males, 9 females, age range y, mean SD weight kg for females, 84 8 kg for males). METHODS: The volunteers completed 2 trials of breathing through a face mask fitted with an active impedance threshold device set to open at 7cmH 2 O pressure, or with a sham impedance threshold device, which was identical to the active device except that it did not contain an inspiratory threshold pressure valve diaphragm. Spontaneous breathing frequency (f), tidal volume (V T ), exhaled minute ventilation, inspiratory pressure, and inspiratory time were measured with a respiratory monitor, and the data were directed to a laptop computer for real-time calculation of the imposed power of breathing. RESULTS: There were no significant differences in heart rate, respiratory rate, tidal volume, and minute ventilation, with and without inspiratory impedance. For the sham and active impedance threshold device groups, respectively, the mean SD imposed power of breathing values were J/min and J/min (p < 0.001), the mean SD inspiratory times were s and s(p 0.001), and the mean SD inspiratory airway/mouth pressures were cm H 2 O and cm H 2 O (p < 0.001). CONCLUSIONS: Breathing through an active impedance threshold device requires significantly more power than breathing through a sham device. All subjects tolerated the respiratory work load and were able to complete the study protocol. Key words: respiration, power of breathing, minute ventilation, inspiratory pressure, hypotension. [Respir Care 2007;52(2): ] Ahamed H Idris MD is affiliated with the Departments of Surgery and Emergency Medicine, University of Texas Southwestern Medical Center, Dallas, Texas. Victor A Convertino PhD is affiliated with the United States Army Institute of Surgical Research, Fort Sam Houston, Texas. Duane A Ratliff MSc is affiliated with Bionetics Corporation, at the National Aeronautics and Space Administration, Kennedy Space Center, Florida. Donald F Doerr MSc is affiliated with the Biological and Chemical Laboratories Branch, National Aeronautics and Space Administration, Kennedy Space Center, Florida. Keith G Lurie MD is affiliated with Advanced Circulatory Systems, Eden Prairie, Minnesota, and with the Department of Emergency Medicine, University of Minnesota, Minneapolis, Minnesota. Andrea Gabrielli MD and Michael J Banner PhD are affiliated with the Departments of Anesthesiology, Physiology, and Surgery, College of Medicine, University of Florida, Gainesville, Florida. This research was supported by a Cooperative Research and Development Agreement between the United States Army Institute of Surgical Research, the National Aeronautics and Space Administration (CRDA No. DAMD ), and the National Institutes of Health (Grant HL077887). The views expressed herein are the private views of the authors and are not to be construed as representing those of the National Aeronautics and Space Administration, the Department of Defense, the Department of the Army, or the National Institutes of Health. Ahamed H Idris MD presented a version of this report at the 34th annual Critical Care Congress of the Society of Critical Care Medicine, held January 15 19, 2005, in Phoenix, Arizona. This article is copyright-free because of the federal employment status of certain of the authors. Keith G Lurie MD is a co-inventor of the impedance threshold device and founded Advanced Circulatory Systems to develop the device. The authors report no other conflicts of interest related to the content of this paper. Correspondence: Michael J Banner PhD, Department of Anesthesiology, College of Medicine, University of Florida, PO Box , Gainesville FL RESPIRATORY CARE FEBRUARY 2007 VOL 52 NO 2 177
2 Introduction Table 1. Subject Group Demographic Data* Orthostatic hypotension and frank syncope are debilitating conditions for military personnel, astronauts returning from space, and patients who suffer from clinical autonomic dysfunction. 1 3 One of the challenges to effective treatment of orthostatic intolerance is maintenance of venous return and stroke volume, particularly in the presence of reduced circulatory blood volume. 4 8 Greater negative intrathoracic pressure can be produced by applying resistance during spontaneous inhalation 9 13 and has been associated with elevations in systemic arterial blood pressure and greater organ blood flows in hypovolemic, hypotensive humans, and animals Building on this concept, an inspiratory impedance threshold device was designed to generate more negative intrathoracic pressure (ie, intrapleural, intra-alveolar, and intra-airway pressures are substantially more negative each time the chest expands during the inspiratory phase of breathing) ,17 In a recent experiment, we demonstrated that during spontaneous inhalation through an impedance threshold device, stroke volume, cardiac output, and mean arterial blood pressure increased in human subjects during a squat-stand test maneuver and is an effective countermeasure against orthostatic hypotension and intolerance. 18 For the impedance threshold device to be clinically useful, the effort required for breathing through the device should not require excessive work of breathing (WOB) per minute. WOB per min is the power of breathing (POB). The objectives of this study were to measure and compare the inspiratory imposed POB (POB I ) and other respiratory variables in subjects breathing through an active or a sham impedance threshold device. POB I is the imposed work load per minute on the respiratory muscles by the sham or active impedance threshold device during spontaneous inhalation. Subjects Methods Nineteen healthy, normotensive, nonsmoking adults were recruited to participate in the present investigation (10 males, 9 females). Demographic data for the subjects are presented in Table 1. A complete medical history and physical examination that included a resting 12-lead electrocardiogram and clinical orthostatic examination (supine/ seated/standing consecutive blood pressure measurements) were obtained with each of the potential subjects. Because of potential effects on cardiovascular function, the subjects refrained from any exercise and stimulants such as caffeine and other nonprescription drugs for 48 hours prior to testing. During an orientation period that preceded each experiment, all subjects were made familiar with the laboratory, the protocol, and the procedures. The experimental procedures and protocols were reviewed and approved by the Human Investigative Review Board of the Kennedy Space Center for the use of human subjects. Each subject gave written informed voluntary consent to participate in the experiments. Protocol Female Male Age (y) Height (cm) Weight (kg) Heart rate (beats/min) Systolic blood pressure (mm Hg) Diastolic blood pressure (mm Hg) *19 subjects (9 female, 10 male). Values are mean SD. Each subject completed 2 tests: 1. During spontaneous breathing through a face mask with an impedance threshold device (Advanced Circulatory Systems, Eden Prairie, Minnesota) set with an inspiratory threshold pressure valve setting of 7 cm H 2 O (pressure at which the valve opens, allowing air inflow) 2. During a control session, breathing through the same face mask with a sham impedance threshold device (ie, no inspiratory threshold pressure valve) The 7 cm H 2 O pressure setting was chosen, because at this impedance pressure level spontaneous breathing was shown to be tolerable and resulted in increases in arterial blood pressure, heart rate, stroke volume, and cardiac output in human subjects 18 and in animal models. 19 While subjects acclimated to breathing through the valve, peak sinusoidal flow rates varied from 0.1 L/s to 0.7 L/s. Each subject had his or her own disposable face mask. The order of treatment was selected using a computer-generated randomization list so that 9 subjects (5 males and 4 females) underwent testing with the active impedance threshold device first, and the remaining 10 subjects (5 males and 5 females) underwent testing with the sham impedance threshold device (control condition) first. Each subject, with the face mask and impedance threshold device in place, was instructed to start breathing with natural but deep breaths and to breathe continuously through the impedance threshold device for 2 min. Breathing frequency (f), tidal volume (V T ), exhaled minute ventilation (V E), face-mask inspiratory pressure, and inspiratory time (T I ) were measured with a respiratory monitor (NICO, Respironics, Wallingford, Connecticut). The monitor was supplemented with a laptop computer, using specialized soft- 178 RESPIRATORY CARE FEBRUARY 2007 VOL 52 NO 2
3 Fig. 1. A: Impedance threshold valve. B: Schematic cross-section of the impedance threshold device. During spontaneous inhalation, the silicone diaphragm on top is sucked down by the inspiratory effort, which occludes the exhalation orifice and, simultaneously, inspiratory airflow is drawn through the inspiratory threshold pressure valve into the face mask. During exhalation (not shown), the silicone diaphragm rises and exhaled air flows out through the open exhalation valve orifice. Fig. 2. A subject during test measurements. The figure illustrates the impedance threshold device placement on the subjects, who were instrumented for breath-to-breath measurement of respiratory variables. ware (ewob, Convergent Engineering, Gainesville, Florida) for the real-time calculation of POB I, based on measurements obtained from the respiratory monitor. All measurements were made over a 2-min steady-state time period after the subject had been breathing through the impedance threshold device for 5 min. An interval of at least 30 min was imposed between each test so that each experimental session was conducted over a period of less than 60 min. All subjects completed the protocol without difficulty. Breathing With the Impedance Threshold Device The impedance threshold valve (Fig. 1) is composed of a valve that closes when the pressure within the thorax is less than atmospheric pressure and a second valve (termed the inspiratory threshold pressure valve) that opens at a preset negative face-mask pressure. The impedance threshold device is composed of the valve attachment to a face mask, to ensure that a seal exists between the valve and the skin of the subject s face that is sufficient to eliminate any air leakage (Fig. 2). The impedance threshold device was designed to generate a negative inspiratory threshold pressure and to therefore generate substantially more negative intrapleural pressure during spontaneous inhalation. 9 11,17 During each test, the subject was instructed to hold the impedance threshold device in place with the right hand (see Fig. 2). Prior to the study, a plot describing the pressure-flow (resistance) characteristics of the impedance threshold device used in this study was determined under in vitro test conditions (Fig. 3). The pressure-flow plot was obtained using a spontaneously breathing lung model (series 1101 breathing simulator, Hans Rudolph, Kansas City, Missouri). The following programmed variables were used: respiratory system resistance 5 cm H 2 O/L/s, respiratory system compliance 0.08 L/cm H 2 O, f 10 breaths/min, and incremental peak sinusoidal inspiratory flow rates for simulating different spontaneous flow demands. Measurement of Respiratory Variables A pressure/flow sensor from the aforementioned respiratory monitor, positioned between the face mask and impedance threshold device, was used to measure pressure, flow rate, T I,V E, V T, and f. Face-mask pressure was integrated with V T to produce real-time pressure-volume loops, with the inspiratory portion determined to be the RESPIRATORY CARE FEBRUARY 2007 VOL 52 NO 2 179
4 Table 2. Respiratory Variables While Breathing Through Active and Sham Impedance Threshold Devices Active Device* Sham Device* p f (breaths/min) V T (L) V E (L/min) T 1 (s) PIF (L/s) Face-mask pressure (cm H 2 O) WOB I (J/L) POB 1 (J/min) Fig. 3. Plot of the pressure-flow (resistance) characteristics of the impedance threshold device, as used in the study under in vitro test conditions of simulated spontaneous breathing. As simulated peak inspiratory flow rate demand increased (X axis), the pressure drop across the impedance threshold device became more negative. The slope of the line (9.86 cm H 2 O/L/s) relates to the imposed resistance of the impedance threshold device. inspiratory imposed WOB per breath (WOB I ). WOB I values were averaged over 1 min to calculate POB I. All data were stored on a laptop computer for subsequent off-line analysis. Statistical Analysis The data were analyzed using a standard 2-group (male, female) by 2-treatment ( 7 cm H 2 O impedance threshold device, control) mixed model analysis of variance to determine gender differences. Alpha was set at 0.05 for statistical significance. The model was mixed in the sense that subjects were nested within groups by sex and crossed with treatments (ie, one between-subjects factor [gender] and one within-subjects factor [treatment]). All main and subsequent interaction effects were analyzed across 6 dependent effects (f, V T,V E, inspiratory face-mask pressure, T I, and POB I ). The p values were calculated for each independent effect and reflect the probability of obtaining the observed or greater effect given only random departure from the assumption of no effects. Data are presented as mean SD. Demographic Data Results Baseline values for age, height, weight, heart rate, and blood pressures are presented in Table 1. There were no statistically significant differences between the male and female groups for age, heart rate, or diastolic blood pressure. The mean systolic blood pressures were mm Hg and mm Hg for the males and *Values are mean SD. f frequency of spontaneous breaths V T tidal volume V E spontaneous minute ventilation T I inspiratory time PIF peak inspiratory flow WOB I inspiratory imposed resistive work of breathing per breath for the impedance threshold device POB I inspiratory imposed resistive power of breathing (WOB I /min) for the impedance threshold device females, respectively (p 0.018). Male and female groups showed the expected and well-established differences in height and weight. Values for heart rates and blood pressures were within established normal limits. Impedance Threshold Device and Gender Effects Gender did not influence the responses of heart rate (p 0.954), f (p 0.831), V T (p 0.857), V E (p 0.662), inspiratory pressure (p 0.188), T I (p 0.676), or POB I (p 0.145) across treatment during either spontaneous breathing through the impedance threshold device or the control experimental conditions. Based on these analyses, the data were combined and analyzed with t test statistics, with a sample size of 19. Respiratory Effects Between the active device and sham groups there were no significant differences in f, V T,orV E. In the active device group, T I, face-mask pressure, WOB I, and POB I were significantly greater than in the sham group (Table 2). T I increased by 50%, change in face-mask pressure increased by 936%, WOB I increased by 1,157%, and POB I increased by 790%. Although face-mask pressure is governed by the inspiratory threshold pressure valve setting, it was also affected by the peak inspiratory flow rate. Higher inspiratory flow was associated with lower face-mask pressure, and vice versa. Face-mask pressure correlated inversely with inspiratory flow rate demand (r 0.89, p 0.001) (Fig. 4). These findings were consistent with 180 RESPIRATORY CARE FEBRUARY 2007 VOL 52 NO 2
5 Fig. 4. Relationship between peak inspiratory flow rate demand and face-mask negative inspiratory pressure with the active impedance threshold device. Greater negative face-mask pressure is generated as peak inspiratory flow increases, and vice versa. Negative pressure generated with the impedance threshold device is dependent on both the inspiratory pressure threshold valve setting (see Fig. 1) and the peak inspiratory flow rate demand (see Fig. 3). Fig. 5. Relationship between exhaled minute ventilation and imposed power of breathing (POB I ) while breathing through the active impedance threshold device. As minute ventilation increases, the imposed power of breathing increases, and vice versa. in vitro data that demonstrated that the impedance threshold device had an imposed resistance of nearly 10 cm H 2 O/L/s (see Fig. 3). The active device group had a significantly lower peak inspiratory flow than the sham group (see Table 2). POB I correlated directly with V E with the active impedance threshold device (r 0.95, p 0.001) (Fig. 5). Discussion This study demonstrated that POB I with the active impedance threshold device is significantly greater than when breathing through the sham device. In addition, breathing through an active impedance threshold device is associated with significantly longer T I and significantly more negative inspiratory pressure than the sham device, even though the subjects were instructed to breathe the same way through both the sham and active devices. However, there were no significant differences in ventilation variables such as f, V T, and V E, with and without inspiratory impedance. POB I for the active impedance threshold device (approximately 8 J/min) represents an additional work load over and above the normal adult physiologic work load on the respiratory muscles (4 8 J/min). 20 When spontaneously inhaling through the impedance threshold device ( 7 cm H 2 O), the total POB [physiologic POB plus POB I ]) is expected to be approximately J/min. All the healthy volunteers in this study completed the protocol and tolerated breathing through the impedance threshold device. Power is work per unit time (power work per breath f). To put power into a frame of reference, moderate exercise that requires a V E of L requires approximately 80 J/min of power In contrast, the 7 cm H 2 O impedance threshold device requires about J/min of power, which should be well tolerated by most people with normal respiratory function. POB I varied directly with V E, which combines the variables of T I,V T, and f (see Fig. 5). Because both POB I and V E share time as a common denominator, there is a direct relationship between work and volume, which suggests a predominant effect of mechanical impedance, as opposed to ventilatory pattern. A goal of this study was to determine the work load of the impedance threshold device on the respiratory muscles. For this reason, only POB I of the impedance threshold device was measured. Measurement of total POB (physiologic power [elastic and resistive power] plus POB I ) was not a goal of the study. Thus, an esophageal balloon catheter, used for the measurement of esophageal pressure (indirect measurement of intrapleural pressure) and for calculating physiologic POB, was not inserted. 24 In general, respiratory muscle fatigue occurs whenever energy demand (oxygen consumption and blood flow) exceeds energy supply. For the impedance threshold device to be functional, the energy required for its operation should not exceed the energy available in patients to whom it is expected to be applied, such as ill and injured patients with hypotension. It should be noted that the impedance threshold device is contraindicated in patients with pulmonary edema or congestive heart failure, because it could exacerbate those conditions. Impedance threshold devices generate negative facemask pressure as a result of their inspiratory threshold pressure valve setting, and, in part, due to resistance to airflow though the device. The impedance threshold device used in this study had the characteristics of a threshold load and of a resistive load. Elastic work is required to RESPIRATORY CARE FEBRUARY 2007 VOL 52 NO 2 181
6 overcome the threshold load ( 7 cm H 2 O), and resistive work is required to overcome the internal flow-resistive components of the valve (approximately 10 cm H 2 O/L/s) to ensure inspiratory flow (see Fig. 3). With increased inspiratory flow demand, increased negative face-mask pressure is generated (see Fig. 4). The greater the flow, the greater the negative pressure, and vice versa. Greater negative inspiratory pressure is associated with greater WOB I and POB I, and, thus, respiratory muscle loading. Care should be taken to ensure that subjects do not inhale at a high inspiratory flow ( 1 L/s) so that excessively large negative pressure and intolerably high work load are not generated. We found that subjects breathing through the active device spontaneously altered their normal breathing pattern and used significantly longer T I than when breathing through the sham device. The longer T I effectively reduced inspiratory flow. Although negative face-mask pressure was much greater with the active device, even the sham device had a face-mask pressure that was less than zero, probably because there was some resistance to airflow imposed by the pressure-relief port, even without the threshold valve in place. The impedance threshold device is intended for use as a countermeasure for orthostasis in astronauts who return to gravity after prolonged microgravity exposure. A study of the effect of inspiratory impedance on orthostasis using the squat-stand test showed that the impedance threshold device preserved cardiac stroke volume and output during orthostatic challenge and reduced symptoms of lightheadedness and blurred vision. 25 It was well tolerated in this population of otherwise healthy individuals with normal respiratory function. It is also intended for use in people who suffer from chronic orthostasis and in people who suffer from acute hypovolemic hypotension. 26 Although work load tolerance is likely to be decreased in people who are injured and have lost blood and may have ischemia, the work load imposed by the impedance threshold device may nevertheless be tolerated because it functions to increase blood flow; however, this needs to be studied. The impedance threshold device is currently being studied with hypotensive patients suffering volume loss. Conclusions The impedance threshold device with an inspiratory opening pressure of 7 cm H 2 O has a POB I of about 8 J/min. While inhaling through this impedance threshold device, the total POB (physiologic POB plus POB I )is expected to be about J/min. Although not specifically measured, all subjects in this study tolerated this respiratory work load well and completed the protocol. ACKNOWLEDGMENTS We are grateful to Neil R Euliano, Convergent Engineering, Gainesville, Florida, for the computer software used for calculating power of breathing, and to Anja Metzger for help in preparing Figure 3. REFERENCES 1. Kapoor WN. Importance of neurocardiogenic causes in the etiology of syncope. In: Blan J-J, Benditt D, Sutton R, editors. Neurally mediated syncope: pathophysiology, investigations, and treatment. Armonk: Future Publishing; 1996: Buckey JC Jr, Lane LD, Levine BD, Watenpaugh DE, Wright SJ, Moore WE, et al. Orthostatic intolerance after spaceflight. J Appl Physiol 1996;81(1): Levine BD, Pawelczyk JA, Ertl AC, Cox JF, Zuckerman JH, Diedrich A, et al. Human muscle sympathetic neural and haemodynamic responses to tilt following spaceflight. J Physiol 2002;538(Pt 1): Bellamy RF. The causes of death in conventional land warfare: implications for combat casualty care research. Mil Med 1984;149(2): Heckbert SR, Vedder NB, Hoffman W, Winn RK, Hudson LD, Jurkovich GJ, et al. Outcome after hemorrhagic shock in trauma patients. J Trauma 1998;45(3): Trunkey DD. Trauma: accidental and intentional injuries account for more years of life lost in the U.S. than cancer and heart disease. Among the prescribed remedies are improved preventive efforts, speedier surgery and further research. Sci Am 1983;249(2): Convertino VA, Cooke WH. Relationship between stroke volume and sympathetic nerve activity: new insights about autonomic mechanisms of syncope. J Gravit Physiol 2002;9(1):P63 P Cooke WH, Ryan KL, Convertino VA. Lower body negative pressure as a model to study progression to acute hemorrhagic shock in humans. J Appl Physiol 2004;96(4): Lurie K, Voelckel W, Plaisance P, Zielinski T, McKnite S, Kor D, et al. Use of an inspiratory impedance threshold valve during cardiopulmonary resuscitation: a progress report. Resuscitation 2000;44(3): Lurie K, Zielinski T, McKnite S, Sukhum P. Improving the efficiency of cardiopulmonary resuscitation with an inspiratory impedance threshold valve. Crit Care Med 2000;28(11 Suppl):N207 N Lurie KG, Voelckel WG, Zielinski T, McKnite S, Lindstrom P, Peterson C, et al. Improving standard cardiopulmonary resuscitation with an inspiratory impedance threshold valve in a porcine model of cardiac arrest. Anesth Analg 2001;93(3): Lurie KG, Zielinski T, Voelckel W, McKnite S, Plaisance P. Augmentation of ventricular preload during treatment of cardiovascular collapse and cardiac arrest. Crit Care Med 2002;30(4 Suppl):S162 S Lurie KG, Zielinski T, McKnite S, Aufderheide T, Voelckel W. Use of an inspiratory impedance valve improves neurologically intact survival in a porcine model of ventricular fibrillation. Circulation 2002;105(1): Lurie KG, Coffeen P, Shultz J, McKnite S, Detloff B, Mulligan K. Improving active compression-decompression cardiopulmonary resuscitation with an inspiratory impedance valve. Circulation 1995; 91(6): Lurie KG, Mulligan KA, McKnite S, Detloff B, Lindstrom P, Lindner KH. Optimizing standard cardiopulmonary resuscitation with an inspiratory impedance threshold valve. Chest 1998;113(4): Plaisance P, Lurie KG, Payen D. Inspiratory impedance during active compression-decompression cardiopulmonary resuscitation: a 182 RESPIRATORY CARE FEBRUARY 2007 VOL 52 NO 2
7 randomized evaluation in patients in cardiac arrest. Circulation 2000; 101(9): Lurie KG, Barnes TA, Zielinski TM, McKnite SH. Evaluation of a prototype inspiratory impedance threshold valve designed to enhance the efficiency of cardiopulmonary resuscitation. Respir Care 2003; 48(1): Convertino VA, Ratliff D, Ryan KL, Doerr DF, Ludwig DA, Muniz GW, et al. Hemodynamics associated with breathing through an inspiratory impedance threshold device in human volunteers. Crit Care Med 2004;32(9 Suppl):S381 S Lurie KG, Zielinski TM, McKnite SH, Idris AH, Yannopoulos D, Raedler CM, et al. Treatment of hypotension in pigs with an inspiratory impedance threshold device: a feasibility study. Crit Care Med 2004;32(7): Milic-Emili J. Work of breathing. In: Crystal RG, West JB, editors. The lung: scientific foundations. New York: Raven Press; 1991: Milic-Emili G, Petit JM, Deroanne R. Mechanical work of breathing during exercise in trained and untrained subjects. J Appl Physiol 1962;17: Margaria R, Milic-Emili G, Petit JM, Cavagna G. Mechanical work of breathing during muscular exercise. J Appl Physiol 1960;15: Roussos C, Campbell EJM. Respiratory muscle energetics. In: Macklem PT, Mead J, editors. Handbook of physiology, Section 3: The respiratory system, vol. 3: Mechanics of breathing. Washington DC: American Physiological Society; 1986: Banner MJ. Respiratory muscle loading and the work of breathing. J Cardiothorac Vasc Anesth 1995;9(2): Convertino VA, Ratliff DA, Crissey J, Doerr DF, Idris AH, Lurie KG. Effects of inspiratory impedance on hemodynamic responses to a squatstand test in human volunteers: implications for treatment of orthostatic hypotension. Eur J Appl Physiol 2005;94(4): Convertino VA, Cooke WH, Lurie KG. Restoration of central blood volume: application of a simple concept and simple device to counteract cardiovascular instability in syncope and hemorrhage. J Gravit Physiol 2005;12: RESPIRATORY CARE FEBRUARY 2007 VOL 52 NO 2 183
Evaluation of a Prototypic Inspiratory Impedance Threshold Valve Designed to Enhance the Efficiency of Cardiopulmonary Resuscitation
 Evaluation of a Prototypic Inspiratory Impedance Threshold Valve Designed to Enhance the Efficiency of Cardiopulmonary Resuscitation Keith G Lurie MD, Thomas A Barnes EdD RRT, Todd M Zielinski PhD, and
Evaluation of a Prototypic Inspiratory Impedance Threshold Valve Designed to Enhance the Efficiency of Cardiopulmonary Resuscitation Keith G Lurie MD, Thomas A Barnes EdD RRT, Todd M Zielinski PhD, and
McHENRY WESTERN LAKE COUNTY EMS SYSTEM FALL 2014 CONTINUING EDUCATION MANDATORY FOR ALL PRIMARY AND PROBATIONARY ALS SYSTEM PROVIDERS.
 McHENRY WESTERN LAKE COUNTY EMS SYSTEM FALL 2014 CONTINUING EDUCATION MANDATORY FOR ALL PRIMARY AND PROBATIONARY ALS SYSTEM PROVIDERS ResQPOD In a cardiac arrest blood flow to the organs stop. Key to survival
McHENRY WESTERN LAKE COUNTY EMS SYSTEM FALL 2014 CONTINUING EDUCATION MANDATORY FOR ALL PRIMARY AND PROBATIONARY ALS SYSTEM PROVIDERS ResQPOD In a cardiac arrest blood flow to the organs stop. Key to survival
Use of an inspiratory impedance threshold valve during cardiopulmonary resuscitation: a progress report
 Resuscitation 44 (2000) 219 230 www.elsevier.com/locate/resuscitation Short communication Use of an inspiratory impedance threshold valve during cardiopulmonary resuscitation: a progress report Keith Lurie
Resuscitation 44 (2000) 219 230 www.elsevier.com/locate/resuscitation Short communication Use of an inspiratory impedance threshold valve during cardiopulmonary resuscitation: a progress report Keith Lurie
APRV: Moving beyond ARDSnet
 APRV: Moving beyond ARDSnet Matthew Lissauer, MD Associate Professor of Surgery Medical Director, Surgical Critical Care Rutgers, The State University of New Jersey What is APRV? APRV is different from
APRV: Moving beyond ARDSnet Matthew Lissauer, MD Associate Professor of Surgery Medical Director, Surgical Critical Care Rutgers, The State University of New Jersey What is APRV? APRV is different from
Exam Key. NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: % of grade in class
 NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: 100 20% of grade in class 1) An arterial blood sample for a patient at sea level is obtained, and the following physiological values
NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: 100 20% of grade in class 1) An arterial blood sample for a patient at sea level is obtained, and the following physiological values
Presentation Overview. Monitoring Strategies for the Mechanically Ventilated Patient. Early Monitoring Strategies. Early Attempts To Monitor WOB
 Monitoring Strategies for the Mechanically entilated Patient Presentation Overview A look back into the future What works and what may work What s all the hype about the WOB? Are ventilator graphics really
Monitoring Strategies for the Mechanically entilated Patient Presentation Overview A look back into the future What works and what may work What s all the hype about the WOB? Are ventilator graphics really
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Talmor D, Sarge T, Malhotra A, et al. Mechanical ventilation
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Talmor D, Sarge T, Malhotra A, et al. Mechanical ventilation
The Positive Effect of Negative Pressure
 The Positive Effect of Negative Pressure (Future Direction in Resuscitative Care) Brent Parquette, NRP Lucas County EMS, Toledo, OH Toledo, Ohio Lucas County EMS (Toledo, OH) Primary service area: 340
The Positive Effect of Negative Pressure (Future Direction in Resuscitative Care) Brent Parquette, NRP Lucas County EMS, Toledo, OH Toledo, Ohio Lucas County EMS (Toledo, OH) Primary service area: 340
Please, after a carefully reading of given references, answer the following questions:
 Report Session 1: Introduction of Respiratory System Student 1 name: Student 2 name: Questionnaire Please, after a carefully reading of given references, answer the following questions: (1) How gas exchange
Report Session 1: Introduction of Respiratory System Student 1 name: Student 2 name: Questionnaire Please, after a carefully reading of given references, answer the following questions: (1) How gas exchange
The physiological functions of respiration and circulation. Mechanics. exercise 7. Respiratory Volumes. Objectives
 exercise 7 Respiratory System Mechanics Objectives 1. To explain how the respiratory and circulatory systems work together to enable gas exchange among the lungs, blood, and body tissues 2. To define respiration,
exercise 7 Respiratory System Mechanics Objectives 1. To explain how the respiratory and circulatory systems work together to enable gas exchange among the lungs, blood, and body tissues 2. To define respiration,
EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES
 GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE
 Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Pulmonary Function and
Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Pulmonary Function and
B-CARD NO PAUSE SHOULD BE YOUR CAUSE
 B-CARD NO PAUSE SHOULD BE YOUR CAUSE SIMEU Congress, 17-20 November, Symposium Georges Bousignac 1 Cardiac arrest: A new cutting edge treatment method by Dr. Boussignac No Pause Should Be Your Cause 2
B-CARD NO PAUSE SHOULD BE YOUR CAUSE SIMEU Congress, 17-20 November, Symposium Georges Bousignac 1 Cardiac arrest: A new cutting edge treatment method by Dr. Boussignac No Pause Should Be Your Cause 2
VENTILATORS PURPOSE OBJECTIVES
 VENTILATORS PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain a ventilator in the interfacility transfer environment. COGNITIVE OBJECTIVES
VENTILATORS PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain a ventilator in the interfacility transfer environment. COGNITIVE OBJECTIVES
 Introduction Welcome to COMPREHENSIVE BASIC LIFE SUPPORT Course. BLS is the foundation for saving lives after cardiac arrest. You will learn the skills of highquality cardiopulmonary resuscitation (CPR)
Introduction Welcome to COMPREHENSIVE BASIC LIFE SUPPORT Course. BLS is the foundation for saving lives after cardiac arrest. You will learn the skills of highquality cardiopulmonary resuscitation (CPR)
Unit 15 Manual Resuscitators
 15-1 Unit 15 Manual Resuscitators GOAL On completion of this unit, the student should comprehend the proper operation of self-inflating resuscitation bags, flow-inflating resuscitation bags and gas-powered
15-1 Unit 15 Manual Resuscitators GOAL On completion of this unit, the student should comprehend the proper operation of self-inflating resuscitation bags, flow-inflating resuscitation bags and gas-powered
Completed downloadable Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 5th Edition by Cairo
 Completed downloadable Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 5th Edition by Cairo Link full download: http://testbankcollection.com/download/pilbeams-mechanicalventilation-physiological-and-clinical-applications-5th-edition-test-bank-cairo
Completed downloadable Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 5th Edition by Cairo Link full download: http://testbankcollection.com/download/pilbeams-mechanicalventilation-physiological-and-clinical-applications-5th-edition-test-bank-cairo
Training Presentation. TFD-EMS Ver. 1 09/15
 Training Presentation TFD-EMS Ver. 1 09/15 Agenda ResQCPR System: Definition and Labeling IPR Therapy Physiology of Conventional CPR ResQPOD ITD 16 and Instructions for Use ResQPUMP ACD-CPR Device and
Training Presentation TFD-EMS Ver. 1 09/15 Agenda ResQCPR System: Definition and Labeling IPR Therapy Physiology of Conventional CPR ResQPOD ITD 16 and Instructions for Use ResQPUMP ACD-CPR Device and
Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams)
 Name Lab Partners Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams) Part 1. Lung Volumes and Capacities Objectives 1. Obtain graphical representation of lung capacities
Name Lab Partners Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams) Part 1. Lung Volumes and Capacities Objectives 1. Obtain graphical representation of lung capacities
Flight Medical presents the F60
 Flight Medical presents the F60 Reliable Ventilation Across the Spectrum of Care Adult & Pediatric Pressure/Volume Control Basic/Advanced Modes Invasive/NIV High Pressure/Low Flow O2 Up to 12 hours batteries
Flight Medical presents the F60 Reliable Ventilation Across the Spectrum of Care Adult & Pediatric Pressure/Volume Control Basic/Advanced Modes Invasive/NIV High Pressure/Low Flow O2 Up to 12 hours batteries
Initiation and Management of Airway Pressure Release Ventilation (APRV)
 Initiation and Management of Airway Pressure Release Ventilation (APRV) Eric Kriner RRT Pulmonary Critical Care Clinical Specialist Pulmonary Services Department Medstar Washington Hospital Center Disclosures
Initiation and Management of Airway Pressure Release Ventilation (APRV) Eric Kriner RRT Pulmonary Critical Care Clinical Specialist Pulmonary Services Department Medstar Washington Hospital Center Disclosures
NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: % of grade in class
 NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: 100 20% of grade in class 1) An arterial blood sample for a patient at sea level is obtained, and the following physiological values
NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: 100 20% of grade in class 1) An arterial blood sample for a patient at sea level is obtained, and the following physiological values
TESTCHEST RESPIRATORY FLIGHT SIMULATOR SIMULATION CENTER MAINZ
 TESTCHEST RESPIRATORY FLIGHT SIMULATOR SIMULATION CENTER MAINZ RESPIRATORY FLIGHT SIMULATOR TestChest the innovation of lung simulation provides a breakthrough in respiratory training. 2 Organis is the
TESTCHEST RESPIRATORY FLIGHT SIMULATOR SIMULATION CENTER MAINZ RESPIRATORY FLIGHT SIMULATOR TestChest the innovation of lung simulation provides a breakthrough in respiratory training. 2 Organis is the
4/18/12 MECHANISM OF RESPIRATION. Every Breath You Take. Fun Facts
 Objectives MECHANISM OF RESPIRATION Dr Badri Paudel Explain how the intrapulmonary and intrapleural pressures vary during ventilation and relate these pressure changes to Boyle s law. Define the terms
Objectives MECHANISM OF RESPIRATION Dr Badri Paudel Explain how the intrapulmonary and intrapleural pressures vary during ventilation and relate these pressure changes to Boyle s law. Define the terms
Activity 2: Examining the Effect of Changing Airway Resistance on Respiratory Volumes
 1 BGYC34 PhysioEx Lab 7 Respiratory Systems Mechanics Marking Scheme Part 1 Complete PhysioEx lab #7. Hand-in all of the pages associated with the lab. Note that there are 5 activities to be completed.
1 BGYC34 PhysioEx Lab 7 Respiratory Systems Mechanics Marking Scheme Part 1 Complete PhysioEx lab #7. Hand-in all of the pages associated with the lab. Note that there are 5 activities to be completed.
Selecting the Ventilator and the Mode. Chapter 6
 Selecting the Ventilator and the Mode Chapter 6 Criteria for Ventilator Selection Why does the patient need ventilatory support? Does the ventilation problem require a special mode? What therapeutic goals
Selecting the Ventilator and the Mode Chapter 6 Criteria for Ventilator Selection Why does the patient need ventilatory support? Does the ventilation problem require a special mode? What therapeutic goals
Mechanical Ventilation. Which of the following is true regarding ventilation? Basics of Ventilation
 Mechanical Ventilation Jeffrey L. Wilt, MD, FACP, FCCP Associate Professor of Medicine Michigan State University Associate Program Director MSU-Grand Rapids Internal Medicine Residency Which of the following
Mechanical Ventilation Jeffrey L. Wilt, MD, FACP, FCCP Associate Professor of Medicine Michigan State University Associate Program Director MSU-Grand Rapids Internal Medicine Residency Which of the following
NOTE: If not used, provider must document reason(s) for deferring mechanical ventilation in a patient with an advanced airway
 APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
APPENDIX: TITLE: Mechanical Ventilator Use REVISED: November 1, 2017 I. Introduction: Mechanical Ventilation is the use of an automated device to deliver positive pressure ventilation to a patient. Proper
Mechanical Ventilation
 PROCEDURE - Page 1 of 5 Purpose Scope Physician's Order Indications Procedure Mechanical Artificial Ventilation refers to any methods to deliver volumes of gas into a patient's lungs over an extended period
PROCEDURE - Page 1 of 5 Purpose Scope Physician's Order Indications Procedure Mechanical Artificial Ventilation refers to any methods to deliver volumes of gas into a patient's lungs over an extended period
SUPPLEMENTARY APPENDIX. Ary Serpa Neto MD MSc, Fabienne D Simonis MD, Carmen SV Barbas MD PhD, Michelle Biehl MD, Rogier M Determann MD PhD, Jonathan
 1 LUNG PROTECTIVE VENTILATION WITH LOW TIDAL VOLUMES AND THE OCCURRENCE OF PULMONARY COMPLICATIONS IN PATIENTS WITHOUT ARDS: a systematic review and individual patient data metaanalysis SUPPLEMENTARY APPENDIX
1 LUNG PROTECTIVE VENTILATION WITH LOW TIDAL VOLUMES AND THE OCCURRENCE OF PULMONARY COMPLICATIONS IN PATIENTS WITHOUT ARDS: a systematic review and individual patient data metaanalysis SUPPLEMENTARY APPENDIX
Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo
 Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo Link full download: http://testbankair.com/download/test-bank-for-pilbeams-mechanicalventilation-physiological-and-clinical-applications-6th-edition-by-cairo/
Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo Link full download: http://testbankair.com/download/test-bank-for-pilbeams-mechanicalventilation-physiological-and-clinical-applications-6th-edition-by-cairo/
INTRODUCTION TO BI-VENT (APRV) INTRODUCTION TO BI-VENT (APRV) PROGRAM OBJECTIVES
 INTRODUCTION TO BI-VENT (APRV) INTRODUCTION TO BI-VENT (APRV) PROGRAM OBJECTIVES PROVIDE THE DEFINITION FOR BI-VENT EXPLAIN THE BENEFITS OF BI-VENT EXPLAIN SET PARAMETERS IDENTIFY RECRUITMENT IN APRV USING
INTRODUCTION TO BI-VENT (APRV) INTRODUCTION TO BI-VENT (APRV) PROGRAM OBJECTIVES PROVIDE THE DEFINITION FOR BI-VENT EXPLAIN THE BENEFITS OF BI-VENT EXPLAIN SET PARAMETERS IDENTIFY RECRUITMENT IN APRV USING
Circulation and Respiration: Vital Signs Student Version
 Circulation and Respiration: Vital Signs Student Version In this lab, you will learn about the circulatory and respiratory systems. You will test the capacity of your lungs, measure your blood pressure
Circulation and Respiration: Vital Signs Student Version In this lab, you will learn about the circulatory and respiratory systems. You will test the capacity of your lungs, measure your blood pressure
RESPIRATORY MUSCLES IN HEALTH AND EMPHYSEMA *
 THE OXYGEN CONSUMPTION AND EFFICIENCY OF THE RESPIRATORY MUSCLES IN HEALTH AND EMPHYSEMA * BY REUBEN M. CHERNIACK t (From The Winnipeg General Hospital and the Departments of Medicine and Physiology and
THE OXYGEN CONSUMPTION AND EFFICIENCY OF THE RESPIRATORY MUSCLES IN HEALTH AND EMPHYSEMA * BY REUBEN M. CHERNIACK t (From The Winnipeg General Hospital and the Departments of Medicine and Physiology and
Key words: intrahospital transport; manual ventilation; patient-triggered ventilation; respiratory failure
 Intrahospital Transport of Critically Ill Patients Using Ventilator With Patient- Triggering Function* Toshiaki Nakamura, MD; Yuji Fujino, MD; Akinori Uchiyama, MD; Takashi Mashimo, MD; and Masaji Nishimura,
Intrahospital Transport of Critically Ill Patients Using Ventilator With Patient- Triggering Function* Toshiaki Nakamura, MD; Yuji Fujino, MD; Akinori Uchiyama, MD; Takashi Mashimo, MD; and Masaji Nishimura,
PICU Resident Self-Study Tutorial The Basic Physics of Oxygen Transport. I was told that there would be no math!
 Physiology of Oxygen Transport PICU Resident Self-Study Tutorial I was told that there would be no math! INTRODUCTION Christopher Carroll, MD Although cells rely on oxygen for aerobic metabolism and viability,
Physiology of Oxygen Transport PICU Resident Self-Study Tutorial I was told that there would be no math! INTRODUCTION Christopher Carroll, MD Although cells rely on oxygen for aerobic metabolism and viability,
RESPIRATORY REGULATION DURING EXERCISE
 RESPIRATORY REGULATION DURING EXERCISE Respiration Respiration delivery of oxygen to and removal of carbon dioxide from the tissue External respiration ventilation and exchange of gases in the lung Internal
RESPIRATORY REGULATION DURING EXERCISE Respiration Respiration delivery of oxygen to and removal of carbon dioxide from the tissue External respiration ventilation and exchange of gases in the lung Internal
ONLINE DATA SUPPLEMENT. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg
 APPENDIX 1 Appendix 1. Complete respiratory protocol. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg predicted body weight (PBW)) (NEJM 2000; 342
APPENDIX 1 Appendix 1. Complete respiratory protocol. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg predicted body weight (PBW)) (NEJM 2000; 342
Why we should care (I)
 What the $*!# is Lung Protective Ventilation and Why Should I be Using it in the OR? Disclosures KATHERINE PALMIERI, MD, MBA 64 TH ANNUAL POSTGRADUATE SYMPOSIUM UNIVERSITY OF KANSAS MEDICAL CENTER DEPARTMENT
What the $*!# is Lung Protective Ventilation and Why Should I be Using it in the OR? Disclosures KATHERINE PALMIERI, MD, MBA 64 TH ANNUAL POSTGRADUATE SYMPOSIUM UNIVERSITY OF KANSAS MEDICAL CENTER DEPARTMENT
Pulmonary Circulation Linda Costanzo Ph.D.
 Pulmonary Circulation Linda Costanzo Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The differences between pressures in the pulmonary and systemic circulations. 2. How
Pulmonary Circulation Linda Costanzo Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The differences between pressures in the pulmonary and systemic circulations. 2. How
Mechanics of proportional-assist ventilation
 CHAPTER 10 Mechanics of proportional-assist ventilation A.C. Lua & K.C. Shi School of Mechanical and Aerospace Engineering, Nanyang Technological University, 50, Nanyang Avenue, Singapore 639798. Abstract
CHAPTER 10 Mechanics of proportional-assist ventilation A.C. Lua & K.C. Shi School of Mechanical and Aerospace Engineering, Nanyang Technological University, 50, Nanyang Avenue, Singapore 639798. Abstract
COALINGA STATE HOSPITAL. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 702 Effective Date: August 31, 2006 SUBJECT: CARDIOPULMONARY RESUSCITATION (CPR) 1. PURPOSE: To provide
VENTIlogic LS VENTIlogic plus. 100 % Mobility and Reliability in IV and NIV
 VENTIlogic LS VENTIlogic plus 100 % Mobility and Reliability in IV and NIV VENTIlogic VENTIlog LS Your Requirements for Reliability and Mobility are Our Benchmark. VENTIlogic LS and VENTIlogic plus are
VENTIlogic LS VENTIlogic plus 100 % Mobility and Reliability in IV and NIV VENTIlogic VENTIlog LS Your Requirements for Reliability and Mobility are Our Benchmark. VENTIlogic LS and VENTIlogic plus are
Respiratory Physiology. Adeyomoye O.I
 Respiratory Physiology By Adeyomoye O.I Outline Introduction Hypoxia Dyspnea Control of breathing Ventilation/perfusion ratios Respiratory/barometric changes in exercise Intra-pulmonary & intra-pleural
Respiratory Physiology By Adeyomoye O.I Outline Introduction Hypoxia Dyspnea Control of breathing Ventilation/perfusion ratios Respiratory/barometric changes in exercise Intra-pulmonary & intra-pleural
Introduction. Respiration. Chapter 10. Objectives. Objectives. The Respiratory System
 Introduction Respiration Chapter 10 The Respiratory System Provides a means of gas exchange between the environment and the body Plays a role in the regulation of acidbase balance during exercise Objectives
Introduction Respiration Chapter 10 The Respiratory System Provides a means of gas exchange between the environment and the body Plays a role in the regulation of acidbase balance during exercise Objectives
Respiratory System. Part 2
 Respiratory System Part 2 Respiration Exchange of gases between air and body cells Three steps 1. Ventilation 2. External respiration 3. Internal respiration Ventilation Pulmonary ventilation consists
Respiratory System Part 2 Respiration Exchange of gases between air and body cells Three steps 1. Ventilation 2. External respiration 3. Internal respiration Ventilation Pulmonary ventilation consists
Basics of Mechanical Ventilation. Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity
 Basics of Mechanical Ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Overview of topics 1. Goals 2. Settings 3. Modes 4. Advantages and disadvantages
Basics of Mechanical Ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Overview of topics 1. Goals 2. Settings 3. Modes 4. Advantages and disadvantages
Lung Volumes and Capacities
 Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
transients' of large amplitude can be imposed on the arterial, cardiac and Since both coughing and the Valsalva manoeuvre raise intrathoracic pressure
 351 J. Physiol. (I953) I22, 35I-357 EFFECTS OF COUGHING ON INTRATHORACIC PRESSURE, ARTERIAL PRESSURE AND PERIPHERAL BLOOD FLOW BY E. P. SHARPEY-SCHAFER From the Department of Medicine, St Thomas's Hospital
351 J. Physiol. (I953) I22, 35I-357 EFFECTS OF COUGHING ON INTRATHORACIC PRESSURE, ARTERIAL PRESSURE AND PERIPHERAL BLOOD FLOW BY E. P. SHARPEY-SCHAFER From the Department of Medicine, St Thomas's Hospital
Breathing Process: Inhalation
 Airway Chapter 6 Breathing Process: Inhalation Active part of breathing Diaphragm and intercostal muscles contract, allowing the lungs to expand. The decrease in pressure allows lungs to fill with air.
Airway Chapter 6 Breathing Process: Inhalation Active part of breathing Diaphragm and intercostal muscles contract, allowing the lungs to expand. The decrease in pressure allows lungs to fill with air.
Respiratory Physiology Gaseous Exchange
 Respiratory Physiology Gaseous Exchange Session Objectives. What you will cover Basic anatomy of the lung including airways Breathing movements Lung volumes and capacities Compliance and Resistance in
Respiratory Physiology Gaseous Exchange Session Objectives. What you will cover Basic anatomy of the lung including airways Breathing movements Lung volumes and capacities Compliance and Resistance in
Advanced Ventilator Modes. Shekhar T. Venkataraman M.D. Professor Critical Care Medicine and Pediatrics University of Pittsburgh School of Medicine
 Advanced Ventilator Modes Shekhar T. Venkataraman M.D. Shekhar T. Venkataraman M.D. Professor Critical Care Medicine and Pediatrics University of Pittsburgh School of Medicine Advanced modes Pressure-Regulated
Advanced Ventilator Modes Shekhar T. Venkataraman M.D. Shekhar T. Venkataraman M.D. Professor Critical Care Medicine and Pediatrics University of Pittsburgh School of Medicine Advanced modes Pressure-Regulated
Medical Ventilators. Ryan Sanford Daniel Tajik
 Medical Ventilators Ryan Sanford Daniel Tajik Medical Ventilators Assist patients that have trouble breathing on their own. 2 Oxygen Intake The Respiratory System has the responsibility of providing the
Medical Ventilators Ryan Sanford Daniel Tajik Medical Ventilators Assist patients that have trouble breathing on their own. 2 Oxygen Intake The Respiratory System has the responsibility of providing the
Respiratory Physiology 2
 Respiratory Physiology 2 Session Objectives. What you will cover Gaseous Exchange Control of Breathing Rate Your objectives are State the function of support structures and epithelia of the bronchial tree
Respiratory Physiology 2 Session Objectives. What you will cover Gaseous Exchange Control of Breathing Rate Your objectives are State the function of support structures and epithelia of the bronchial tree
VENTIlogic LS VENTIlogic plus. 100 % Mobility and Reliability in IV and NIV
 VENTIlogic LS VENTIlogic plus 100 % Mobility and Reliability in IV and NIV VENTIlogic LS VENTIlogic plus Your requirements for reliability and mobility are our benchmark. VENTIlogic LS and VENTIlogic plus
VENTIlogic LS VENTIlogic plus 100 % Mobility and Reliability in IV and NIV VENTIlogic LS VENTIlogic plus Your requirements for reliability and mobility are our benchmark. VENTIlogic LS and VENTIlogic plus
Indications for Mechanical Ventilation. Mechanical Ventilation. Indications for Mechanical Ventilation. Modes. Modes: Volume cycled
 Mechanical Ventilation Eric A. Libré, MD VCU School of Medicine Inova Fairfax Hospital and VHC Indications for Mechanical Ventilation Inadequate ventilatory effort Rising pco2 with resp acidosis (7.25)
Mechanical Ventilation Eric A. Libré, MD VCU School of Medicine Inova Fairfax Hospital and VHC Indications for Mechanical Ventilation Inadequate ventilatory effort Rising pco2 with resp acidosis (7.25)
VENTILATION STRATEGIES FOR THE CRITICALLY UNWELL
 VENTILATION STRATEGIES FOR THE CRITICALLY UNWELL Dr Nick Taylor Visiting Emergency Specialist Teaching Hospital Karapitiya Senior Specialist and Director ED Training Clinical Lecturer, Australian National
VENTILATION STRATEGIES FOR THE CRITICALLY UNWELL Dr Nick Taylor Visiting Emergency Specialist Teaching Hospital Karapitiya Senior Specialist and Director ED Training Clinical Lecturer, Australian National
R S A B C CPR. Basic Life Support Flow Chart Check for danger. Check Response. Send for Help. Check Airway. Check for Breathing.
 CPR CPR is the technique of the manual inflation of the lungs with oxygen, and compression of the heart, therefore pumping oxygenated blood around the body, and keeping the vital organs supplied with oxygen.
CPR CPR is the technique of the manual inflation of the lungs with oxygen, and compression of the heart, therefore pumping oxygenated blood around the body, and keeping the vital organs supplied with oxygen.
Chapter 4: Ventilation Test Bank MULTIPLE CHOICE
 Instant download and all chapters Test Bank Respiratory Care Anatomy and Physiology Foundations for Clinical Practice 3rd Edition Will Beachey https://testbanklab.com/download/test-bank-respiratory-care-anatomy-physiologyfoundations-clinical-practice-3rd-edition-will-beachey/
Instant download and all chapters Test Bank Respiratory Care Anatomy and Physiology Foundations for Clinical Practice 3rd Edition Will Beachey https://testbanklab.com/download/test-bank-respiratory-care-anatomy-physiologyfoundations-clinical-practice-3rd-edition-will-beachey/
Capnography in the Veterinary Technician Toolbox. Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA
 Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
PROBLEM SET 8. SOLUTIONS April 15, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Respiratory System Physiology. Dr. Vedat Evren
 Respiratory System Physiology Dr. Vedat Evren Respiration Processes involved in oxygen transport from the atmosphere to the body tissues and the release and transportation of carbon dioxide produced in
Respiratory System Physiology Dr. Vedat Evren Respiration Processes involved in oxygen transport from the atmosphere to the body tissues and the release and transportation of carbon dioxide produced in
 http://www.priory.com/cmol/hfov.htm INTRODUCTION The vast majority of patients who are admitted to an Intensive Care Unit (ICU) will need artificial ventilation (Jones et al 1998). The usual means through
http://www.priory.com/cmol/hfov.htm INTRODUCTION The vast majority of patients who are admitted to an Intensive Care Unit (ICU) will need artificial ventilation (Jones et al 1998). The usual means through
LAB 7 HUMAN RESPIRATORY LAB. Complete the charts on pgs. 67 and 68 and read directions for using BIOPAC
 66 LAB 7 HUMAN RESPIRATORY LAB Assignments: Due before lab: Quiz: Three Respiratory Interactive Physiology Animations pages 69 73. Complete the charts on pgs. 67 and 68 and read directions for using BIOPAC
66 LAB 7 HUMAN RESPIRATORY LAB Assignments: Due before lab: Quiz: Three Respiratory Interactive Physiology Animations pages 69 73. Complete the charts on pgs. 67 and 68 and read directions for using BIOPAC
PART SEVEN THE HISTORY AND APPLICATION OF HIGH FREQUENCY OSCILLATORY VENTILATION (HFOV)
 PART SEVEN THE HISTORY AND APPLICATION OF HIGH FREQUENCY OSCILLATORY VENTILATION (HFOV) Reciprocating pistons with an eccentric travel speed, moving to and fro within a cylinder (with a common inlet/outlet),
PART SEVEN THE HISTORY AND APPLICATION OF HIGH FREQUENCY OSCILLATORY VENTILATION (HFOV) Reciprocating pistons with an eccentric travel speed, moving to and fro within a cylinder (with a common inlet/outlet),
Figure 1. A schematic diagram of the human respiratory system.
 Introduction to Respiration In this experiment, you will investigate various aspects of normal breathing, hyperventilation, rebreathing the effect of changing airway resistance and ways in which to measure
Introduction to Respiration In this experiment, you will investigate various aspects of normal breathing, hyperventilation, rebreathing the effect of changing airway resistance and ways in which to measure
Homeostasis and Negative Feedback Concepts and Breathing Experiments 1
 Homeostasis and Negative Feedback Concepts and Breathing Experiments 1 I. Homeostasis and Negative Feedback Homeostasis refers to the maintenance of relatively constant internal conditions. For example,
Homeostasis and Negative Feedback Concepts and Breathing Experiments 1 I. Homeostasis and Negative Feedback Homeostasis refers to the maintenance of relatively constant internal conditions. For example,
Peter J. Kudenchuk, MD University of Washington
 Peter J. Kudenchuk, MD University of Washington CPR-The Science Behind the Hands A/Prof Marcus Ong Senior Consultant, Clinician Scientist & Director of Research Department of Emergency Medicine Singapore
Peter J. Kudenchuk, MD University of Washington CPR-The Science Behind the Hands A/Prof Marcus Ong Senior Consultant, Clinician Scientist & Director of Research Department of Emergency Medicine Singapore
Chapter 9 Airway Respirations Metabolism Oxygen Requirements Respiratory Anatomy Respiratory Anatomy Respiratory Anatomy Diaphragm
 1 Chapter 9 Airway 2 Respirations Every cell of the body requires to survive Oxygen must come in and carbon must go out 3 Metabolism Metabolism--Process where the body s cells convert food to Adequate
1 Chapter 9 Airway 2 Respirations Every cell of the body requires to survive Oxygen must come in and carbon must go out 3 Metabolism Metabolism--Process where the body s cells convert food to Adequate
RESPILAB USER MANUAL
 RESPILAB USER MANUAL Virtual Laboratory for Analysis of Human Respiratory System Version 0.3 April 2006 Alher Mauricio Hernández Miguel Ángel Mañanas Ramón Costa Respilab User Manual Table of Contents
RESPILAB USER MANUAL Virtual Laboratory for Analysis of Human Respiratory System Version 0.3 April 2006 Alher Mauricio Hernández Miguel Ángel Mañanas Ramón Costa Respilab User Manual Table of Contents
Objectives. Respiratory Failure : Challenging Cases in Mechanical Ventilation. EM Knows Respiratory Failure!
 Respiratory Failure : Challenging Cases in Mechanical Ventilation Peter DeBlieux, MD, FAAEM, FACEP LSUHSC University Hospital Pulmonary and Critical Care Medicine Emergency Medicine pdebli@lsuhsc.edu Objectives
Respiratory Failure : Challenging Cases in Mechanical Ventilation Peter DeBlieux, MD, FAAEM, FACEP LSUHSC University Hospital Pulmonary and Critical Care Medicine Emergency Medicine pdebli@lsuhsc.edu Objectives
Physiological Basis of Mechanical Ventilation
 Physiological Basis of Mechanical Ventilation Wally Carlo, M.D. University of Alabama at Birmingham Department of Pediatrics Division of Neonatology wcarlo@peds.uab.edu Fine Tuning Mechanical Ventilation
Physiological Basis of Mechanical Ventilation Wally Carlo, M.D. University of Alabama at Birmingham Department of Pediatrics Division of Neonatology wcarlo@peds.uab.edu Fine Tuning Mechanical Ventilation
Mechanical Ventilation
 Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
How might GRADE work for ILCOR? Summary of specific components of GRADE using example worksheet
 1 How might GRADE work for ILCOR? Summary of specific components of GRADE using example worksheet Associate Professor Peter Morley Director Medical Education Royal Melbourne Hospital University of Melbourne
1 How might GRADE work for ILCOR? Summary of specific components of GRADE using example worksheet Associate Professor Peter Morley Director Medical Education Royal Melbourne Hospital University of Melbourne
Lung recruitment maneuvers
 White Paper Lung recruitment maneuvers Assessment of lung recruitability and performance of recruitment maneuvers using the P/V Tool Pro Munir A Karjaghli RRT, Clinical Application Specialist, Hamilton
White Paper Lung recruitment maneuvers Assessment of lung recruitability and performance of recruitment maneuvers using the P/V Tool Pro Munir A Karjaghli RRT, Clinical Application Specialist, Hamilton
Adult, Child and Infant Exam
 CPR Pro for the Professional Rescuer Adult, Child and Infant Exam Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer sheet provided.
CPR Pro for the Professional Rescuer Adult, Child and Infant Exam Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer sheet provided.
Mechanical Ventilation. Mechanical Ventilation is a Drug!!! is a drug. MV: Indications for use. MV as a Drug: Outline. MV: Indications for use
 Mechanical Ventilation is a Drug!!! Mechanical Ventilation is a drug I am an employee of Philips Healthcare Hospital Respiratory Care Group and they help me pay for my kids education Jim Laging, RRT, RCP
Mechanical Ventilation is a Drug!!! Mechanical Ventilation is a drug I am an employee of Philips Healthcare Hospital Respiratory Care Group and they help me pay for my kids education Jim Laging, RRT, RCP
The Internet Journal of Anesthesiology 2010 : Volume 22 Number 2
 The Internet Journal of Anesthesiology 2010 : Volume 22 Number 2 Intelligent ventilator safety valve prevents accidental ventilator induced lung injury Jan Paul J. Mulier M.D., PhD. Department of Anaesthesiology
The Internet Journal of Anesthesiology 2010 : Volume 22 Number 2 Intelligent ventilator safety valve prevents accidental ventilator induced lung injury Jan Paul J. Mulier M.D., PhD. Department of Anaesthesiology
The comparison of Work Of Breathing methodologies on a patient model
 The comparison of Work Of Breathing methodologies on a patient model E. Koumoundouros 1, J. Santamaria 2 and J. Patterson 3. 1 Department of Electrical and Electronic Engineering, The University of Melbourne,
The comparison of Work Of Breathing methodologies on a patient model E. Koumoundouros 1, J. Santamaria 2 and J. Patterson 3. 1 Department of Electrical and Electronic Engineering, The University of Melbourne,
PROBLEM SET 9. SOLUTIONS April 23, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Circulatory And Respiration
 Circulatory And Respiration Composition Of Blood Blood Heart 200mmHg 120mmHg Aorta Artery Arteriole 50mmHg Capillary Bed Venule Vein Vena Cava Heart Differences Between Arteries and Veins Veins transport
Circulatory And Respiration Composition Of Blood Blood Heart 200mmHg 120mmHg Aorta Artery Arteriole 50mmHg Capillary Bed Venule Vein Vena Cava Heart Differences Between Arteries and Veins Veins transport
Enhancing 4 th chain: Mechanical chest compression during transportation
 How to Implement New Resuscitation Guidelines Enhancing 4 th chain: Mechanical chest compression during transportation 한림대의료원강동성심병원응급의학과조영석 Contents The Present of Mechanical CPR Device Barriers of High
How to Implement New Resuscitation Guidelines Enhancing 4 th chain: Mechanical chest compression during transportation 한림대의료원강동성심병원응급의학과조영석 Contents The Present of Mechanical CPR Device Barriers of High
Biology 347 General Physiology Lab Basic Pulmonary Functions: Respirometry and Factors that Effect Respiration
 Biology 347 General Physiology Lab Basic Pulmonary Functions: Respirometry and Factors that Effect Respiration Objectives Students will measure breathing parameters in a resting subject. Students will
Biology 347 General Physiology Lab Basic Pulmonary Functions: Respirometry and Factors that Effect Respiration Objectives Students will measure breathing parameters in a resting subject. Students will
Oxygen injection sites: Important factors that affect the fraction of inspired oxygen
 Oxygen injection sites: Important factors that affect the fraction of inspired oxygen during non-invasive positive pressure ventilation Bing Dai, MD, Jian Kang, MD, Na Yu, MD, Wei Tan, Hong-Wen Zhao, MD
Oxygen injection sites: Important factors that affect the fraction of inspired oxygen during non-invasive positive pressure ventilation Bing Dai, MD, Jian Kang, MD, Na Yu, MD, Wei Tan, Hong-Wen Zhao, MD
mechanical ventilation Arjun Srinivasan
 Respiratory mechanics in mechanical ventilation Arjun Srinivasan Introduction Mechanics during ventilation PV curves Application in health & disease Difficulties & pitfalls The future. Monitoring Mechanics
Respiratory mechanics in mechanical ventilation Arjun Srinivasan Introduction Mechanics during ventilation PV curves Application in health & disease Difficulties & pitfalls The future. Monitoring Mechanics
Operating Instructions for Microprocessor Controlled Ventilators
 Page 1 of 5 Operating Instructions for Microprocessor Controlled Ventilators Purpose Audience Scope Physician's Order To provide guidelines for the procedure for the use of microprocessor controlled ventilators.
Page 1 of 5 Operating Instructions for Microprocessor Controlled Ventilators Purpose Audience Scope Physician's Order To provide guidelines for the procedure for the use of microprocessor controlled ventilators.
Introduction to Conventional Ventilation
 Introduction to Conventional Ventilation Dr Julian Eason Consultant Neonatologist Derriford Hospital Mechanics Inspiration diaphragm lowers and thorax expands Negative intrathoracic/intrapleural pressure
Introduction to Conventional Ventilation Dr Julian Eason Consultant Neonatologist Derriford Hospital Mechanics Inspiration diaphragm lowers and thorax expands Negative intrathoracic/intrapleural pressure
Pulmonary Circulation
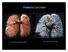 Pulmonary Circulation resin cast of pulmonary arteries resin cast of pulmonary veins Blood Flow to the Lungs Pulmonary Circulation Systemic Circulation Blood supply to the conducting zone provided by the
Pulmonary Circulation resin cast of pulmonary arteries resin cast of pulmonary veins Blood Flow to the Lungs Pulmonary Circulation Systemic Circulation Blood supply to the conducting zone provided by the
3100A Competency Exam
 NAME DATE (Circle the appropriate answer) 3100A Competency Exam 1. Of the following, which best describes the mechanics of ventilation used by the 3100A? a. Active inspiration with passive exhalation b.
NAME DATE (Circle the appropriate answer) 3100A Competency Exam 1. Of the following, which best describes the mechanics of ventilation used by the 3100A? a. Active inspiration with passive exhalation b.
Oxygen Injection Site Affects F IO2 During Noninvasive Ventilation
 Oxygen Injection Site Affects F IO2 During Noninvasive Ventilation Bing Dai MD, Jian Kang MD, Na Yu MD, Wei Tan, and Hong-Wen Zhao MD BACKGROUND: Most portable bi-level positive airway pressure devices
Oxygen Injection Site Affects F IO2 During Noninvasive Ventilation Bing Dai MD, Jian Kang MD, Na Yu MD, Wei Tan, and Hong-Wen Zhao MD BACKGROUND: Most portable bi-level positive airway pressure devices
Measuring Lung Capacity
 Name Class Date Chapter 37 Circulatory and Respiratory Systems Measuring Lung Capacity Introduction The amount of air that you move in and out of your lungs depends on how quickly you are breathing. The
Name Class Date Chapter 37 Circulatory and Respiratory Systems Measuring Lung Capacity Introduction The amount of air that you move in and out of your lungs depends on how quickly you are breathing. The
RSPT 1060 OBJECTIVES OBJECTIVES OBJECTIVES EQUATION OF MOTION. MODULE C Applied Physics Lesson #1 - Mechanics. Ventilation vs.
 RSPT 1060 MODULE C Applied Physics Lesson #1 - Mechanics OBJECTIVES At the end of this module, the student should be able to define the terms and abbreviations used in the module. draw & explain the equation
RSPT 1060 MODULE C Applied Physics Lesson #1 - Mechanics OBJECTIVES At the end of this module, the student should be able to define the terms and abbreviations used in the module. draw & explain the equation
United States Patent 19 Lurie
 United States Patent 19 Lurie US005730 122A 11 Patent Number: 45 Date of Patent: Mar. 24, 1998 54. HEART FAILURE MASK AND METHODS FOR INCREASING NEGATIVE INTRATHORACC PRESSURES 75) Inventor: Keith G. Lurie,
United States Patent 19 Lurie US005730 122A 11 Patent Number: 45 Date of Patent: Mar. 24, 1998 54. HEART FAILURE MASK AND METHODS FOR INCREASING NEGATIVE INTRATHORACC PRESSURES 75) Inventor: Keith G. Lurie,
EMD CPR. The First First Responder. R. Darrell Nelson, MD, FACEP
 EMD CPR The First First Responder R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Baptist Health Medical Director, Davie and Stokes County EMS Assistant Medical Director, Forsyth
EMD CPR The First First Responder R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Baptist Health Medical Director, Davie and Stokes County EMS Assistant Medical Director, Forsyth
Mechanical power and opening pressure. Fellowship training program Intensive Care Radboudumc, Nijmegen
 Mechanical power and opening pressure Fellowship training program Intensive Care Radboudumc, Nijmegen Mechanical power Energy applied to the lung: Ptp * V (Joule) Power = Energy per minute (J/min) Power
Mechanical power and opening pressure Fellowship training program Intensive Care Radboudumc, Nijmegen Mechanical power Energy applied to the lung: Ptp * V (Joule) Power = Energy per minute (J/min) Power
Ventilating the Sick Lung Mike Dougherty RRT-NPS
 Ventilating the Sick Lung 2018 Mike Dougherty RRT-NPS Goals and Objectives Discuss some Core Principles of Ventilation relevant to mechanical ventilation moving forward. Compare and Contrast High MAP strategies
Ventilating the Sick Lung 2018 Mike Dougherty RRT-NPS Goals and Objectives Discuss some Core Principles of Ventilation relevant to mechanical ventilation moving forward. Compare and Contrast High MAP strategies
Lung Volumes and Capacities
 BIOL242 Lung Volumes and Capacities Measurement of lung volumes provides a tool for understanding normal function of the lungs as well as disease states. The breathing cycle is initiated by expansion of
BIOL242 Lung Volumes and Capacities Measurement of lung volumes provides a tool for understanding normal function of the lungs as well as disease states. The breathing cycle is initiated by expansion of
PERFORMANCE EVALUATION #34 NAME: 7200 Ventilator Set Up DATE: INSTRUCTOR:
 PERFORMANCE EVALUATION #34 NAME: 7200 Ventilator Set Up DATE: 1. **Identify and name the filters on the 7200ae. 2. **Explain how each filter is sterilized. 3. **Trace the gas flow through the ventilator
PERFORMANCE EVALUATION #34 NAME: 7200 Ventilator Set Up DATE: 1. **Identify and name the filters on the 7200ae. 2. **Explain how each filter is sterilized. 3. **Trace the gas flow through the ventilator
CARDIOVIT AT-104 ergospirometry
 E D E R I T Z M A N U F A C T U R E D I N A N D S W I G N S E D L A N D CARDIOVIT AT-104 ergospirometry Cardiopulmonary exercise tests (CPET) with touch screen by SCHILLER it s the experience that counts.
E D E R I T Z M A N U F A C T U R E D I N A N D S W I G N S E D L A N D CARDIOVIT AT-104 ergospirometry Cardiopulmonary exercise tests (CPET) with touch screen by SCHILLER it s the experience that counts.
CHAPTER 6. Oxygen Transport. Copyright 2008 Thomson Delmar Learning
 CHAPTER 6 Oxygen Transport Normal Blood Gas Value Ranges Table 6-1 OXYGEN TRANSPORT Oxygen Dissolved in the Blood Plasma Dissolve means that the gas maintains its precise molecular structure About.003
CHAPTER 6 Oxygen Transport Normal Blood Gas Value Ranges Table 6-1 OXYGEN TRANSPORT Oxygen Dissolved in the Blood Plasma Dissolve means that the gas maintains its precise molecular structure About.003
