Breast Treatment System REFERENCE MANUAL
|
|
|
- Hilda Walton
- 5 years ago
- Views:
Transcription
1 Breast Treatment System REFERENCE MANUAL This manual may not be reproduced in whole or in part, by mimeograph or any other means, without the written permission of Diacor, Inc. The MammoRx Breast Treatment System is intended for use only by physicians qualified in radiation oncology and experienced in breast cancer treatment, or by technologists at the specific direction of such a qualified physician. It is the sole responsibility of the physician to judge whether the use of the MammoRx Breast Treatment System is clinically appropriate, whether the initial treatment plan is adequate to achieve his or her clinical goals, and whether the daily treatments are administered as prescribed. Diacor and MammoRx are trademarks of Diacor, Inc. Portalcast is a registered trademark of Diacor, Inc. Poloroid is a registered trademark of Poloroid Corporation. Copyright 2000 Diacor, Inc. DIACOR, 3191 SOUTH 3300 EAST, SALT LAKE CITY, UTAH / FAX
2 MammoRx Breast Treatment System Components A. MammoRx Positioning Board with arm supports and head holder. B. MammoRx Caliper with inclinometer. C. MammoRx Breast Setup Calculator, Printer and Case. D. MammoRx Simulation and Treatment Video. E. MammoRx Reference Manuals. F. MammoRx Miscellaneous Parts.
3 CONTENTS INTRODUCTION FOR THE PHYSICIAN ii PART 1. OVERVIEW 1 PART 2. SETUP PROCEDURES POSITIONING THE PATIENT FOR SETUP SETUP FOR TANGENT AND SUPRACLAVICULAR FIELDS Setup for Supraclavicular Fields Setup for Tangent Fields SETUP FOR TANGENT-ONLY FIELDS 15 PART 3. TREATMENT PROCEDURES POSITIONING THE PATIENT FOR TREATMENT TREATING THE PATIENT USING SUPRACLAVICULAR AND TANGENT FIELDS TREATING THE PATIENT USING TANGENT-ONLY FIELDS 21 APPENDIX A WORKSHEETS 22 A.1 BREAST SIMULATION WORKSHEET 23 A.2 PATIENT SETUP DIAGRAM - LEFT 24 A.3 PATIENT SETUP DIAGRAM - RIGHT 25 APPENDIX B ASSUMPTIONS 26 B.1 SETUP ASSUMPTIONS 26 B.2 GANTRY ANGLE CONVENTIONS 27 i
4 INTRODUCTION FOR THE PHYSICIAN Certain clinical decisions must be made well before the initial setup for treatment begins. Once you have decided to irradiate the breast, you must then decide whether it is necessary to also irradiate the internal mammary chain, the axillary apical nodes, and the supraclavicular nodes. It is of great value to ask the surgeons, with whom you work to place a metallic clip at the apex of their axillary dissections to assist you in designing the coverage of the axillary apex, when such coverage is required. If, in your judgment, it is not necessary to irradiate the supraclavicular nodes and the apex of the axilla, use the two-field technique (tangents only). This method not only is far quicker for both the patient and the technologist, but it also eliminates many of the potential sources of error and morbidity. If you have decided to treat the internal mammary (IM) nodes, you must choose whether this will be done as part of the tangential fields or as a separate direct anterior field treated with electrons and/or photons. Localization of these nodes always involves an element of uncertainty, and their treatment may add to the morbidity of the treatment, primarily depending upon how much lung and heart must be included in the field. The position of the sternum on the simulator films may be sufficient to give assurance of adequate coverage (Figure 1). A planning CT scan may be used for more accurate determination of the anatomy and to visualize enlarged nodes. If lymphoscintigraphy is available, it can be used to localize the AP projection of the nodes and their depth below the skin surface. Remember that, if the margin of coverage around the IM nodes is critical, the final determination of adequate dose delivery must be made from an appropriate isodose distribution with representation of relevant anatomic structures, especially heart and lung. ii
5 Note: The internal mammary nodes may or may not fall within the tangent fields depending on the individual patient anatomy and the amount of lung and heart you feel can be included safely within the field. iii
6 PART 1. OVERVIEW The MammoRx system provides a method of rapidly and comfortably preparing a patient for treatment of the breast or chest wall and regional nodes. The system does not include a slant board nor is a slant board recommended except in special cases for the reason illustrated in Figures 2A and 2B. A "beam-splitter" (central axis block) is used to define the inferior edge of the supraclavicular (SC) field. This forms a vertical plane which abuts with the superior edge of the tangential chest wall fields. After the SC field is set-up, the tangential fields are determined by measuring their separation and angle with a special digital caliper. These measurements, along with the estimated field width are entered into a computer that determines the set-up parameters, including the gantry angles and the necessary lateral shift of the table position from the set-up point on the medial border. The medial tangential field is set up according to the calculated parameters. A couch angle of 5 degrees is used to create a coplanar match of the superior edge of the tangential fields with the inferior edge of the SC field, and the collimator is adjusted to provide the necessary angulation along the chest wall. A bead chain is hung from the head of the simulator with its shadow projecting near the match line to define a vertical plane through the match line on the simulator films of the tangential fields. The projected shadow of the bead chain enables the construction of custom blocks to define this plane. The collimator and gantry angles of the lateral tangent are adjusted to provide a coplanar match of the deep borders of the opposed tangential fields, which is necessary to account for the opposing couch angulation of 5 degrees (10 degrees total). Day-to-day treatment is performed by setting up the SC field first and marking the match line at its inferior edge. The plane is remarked for each day's treatment. Day-to-day variation acts to wash out any dose inhomogeneity, but the daily juxtaposition of the SC and tangential field remains optimal. 1
7 The tangential fields are set up with reference to the tattooed "setup point" at the medial margin by using a lateral shift from this point to reach the treatment isocenter. Recorded gantry and collimator angles as well as couch angulation are used with custom blocks to block back the superior field margins to match the inferior edge of the SC field. During clinical trials of the MammoRx System, 80% of set-ups were considered clinically acceptable after only one set of simulator films, a major improvement over previous techniques at the testing facilities*. *Results will depend on site-specific circumstances. 2
8 3
9 PART 2. SETUP PROCEDURES 2. 1 POSITIONING THE PATIENT FOR SETUP 1. Place the MammoRx board on the table with the pins for the arm and forearm supports snug against the table. Do not use he headrest yet. 2. Position the patient on the board with her arms by her sides and with her shoulder joint over the pivot of the arm support. 3. Straighten the patient on the table. 4. Check the straightness of the patient's position by aligning the sagittal laser or the field cross-hairs with her sternal notch and xiphoid. You may also use the fluoroscope to be sure she is lying as straight as possible. 5. Raise the patient's arm and place it into the arm support and wrist support. The MammoRx board assembly may be moved longitudinally along the table edge if necessary. 6. Adjust the arm support and shoulder to find a position that is comfortable for the patient but places her arm out of the way of the tangent fields. Make sure the upper arm is well cradled and not binding in the arm support. 7. Raise the patient's head and slip the head platform and headrest into place. Put the platform into the set of holes closest to the patient's head position. Choose a headrest that is comfortable but keeps the chin up. 8. Now invite the patient to move slightly in whatever way will make her feel straight, stable, and comfortable. 9. Make sure the patient's position is still satisfactory and the MammoRx arm and forearm support pins are snug against the table. Then record the head and arm positions from the board in the setup-instruction portion of the Breast Simulation Worksheet. A sample of this worksheet is provided in Appendix A. 10. Emphasize to the patient the importance of memorizing this position so that she can repeat it for each treatment. 4
10 2. 2 SETUP FOR TANGENT AND SUPRACLAVICULAR FIELDS Setup for Supraclavicular Fields 1. The physician should use the red marking pen supplied with the MammoRx system to put preliminary marks on the patient's skin to show the intended borders of the supraclavicular field: medial, lateral, superior, and especially the position of the intended match line at the inferior border of the supraclavicular field (the match line is where the supraclavicular and tangent fields abut). Note: The ink from the red marking pen is easily removed from the skin while the ink from the green marking pen is more lasting and less easily removed. 2. Set up the supraclavicular field at a target-skin distance (TSD) of 80 or 100 centimeters, as applicable for your treatment machine. Keep in mind that the field will be treated with a half-field (beamsplitter) block, as shown in Figures 2A and Rotate the gantry to an angle of 10 to 15 degrees to move the beam exit point off the spinal cord and esophagus. 4. Recheck the TSD and check the borders. Apply BB markers where any separate calculation points are desired for the supraclavicular node area and the axilla. 5. Use fluoroscopy or radiography to inspect the borders. The medial border should be off the spinal cord and the lateral border should be approximately at the humeral head, or as otherwise clinically indicated, depending on the degree of axillary coverage required (Figure 3). 6. Take a film for the patient's permanent record and have the physician inspect the film and the field projected on the patient. 7. When the borders of the field are acceptable to the physician, mark the field on the patient's skin with the green marking pen. Use the horizontal line formed by the laser isocenter lights and/or field light as a reference and mark the extension of the match line across the midline and well into the axilla. 5
11 6
12 8. Take any necessary measurements, such as the TSD to the supraclavicular and axillary calculation points, and record the measurements on the Breast Simulation Worksheet. 9. If a beamsplitter block alone will not be adequate for the treatment, the physician should mark the additional blocking required on the supraclavicular field (Figure 3) Setup for Tangent Fields 1. The physician should use the red marking pen supplied with the MammoRx system to put preliminary marks on the patient's skin to show the intended medial, lateral, and inferior borders of the area to be included in the tangential fields. The superior border is the previously- marked match line. 2. Rotate the gantry to vertical and position the central axis of the beam on the intended medial border (Figure 4). 3. Set the field length to match the inferior mark and extend 3 to 4 centimeters superior to the match line (this extra length will be blocked later). Use a preliminary TSD of 77 or 97, as applicable for 80- and 100- centimeter TAD machines, respectively. Note: You should be aware of the maximum working length of any wedges you are using. Do not exceed these limits. 4. Mark the central axis on the patient's skin. The central axis is referred to as the AP setup point. 5. Estimate the required field width based on breast size (a moderate-sized breast requires a field width of approximately 10 centimeters). Set the field width in accordance with your estimate. 6. As an aid to block alignment on the tangential ports, tape BB markers along the match line. Start the BB markers at the medial border of the supraclavicular field and continue them into the axilla. Space the BB markers approximately 5 centimeters apart (Figure 5). 7. Apply a BB marker at the setup point and at the intended lateral border in the axial plane of the setup point. (Figure 5). 1 Contact Diacor Inc. for information on the Portalcast Block Cutting and Casting System. 7
13 8
14 8. Use the provided caliper to measure (in a vertical plane) the distance between the setup point and the lateral border (SEPARATION) and the angle of the chord that connects these two points (CALIPER ANGLE) (Figure 6). 9. Enter the distance measurement into the calculator as SEPARATION. Enter the estimated field width into the calculator as FIELD WIDTH. Enter the chord angle into the calculator as CALIPER ANGLE. Enter the simulator/ accelerator target-axis distance (TAD) into the calculator as MACHINE TAD. Finally, indicate whether a left or right breast is to be treated by pressing the YES or NO button of the calculator. The calculator will then compute the following setup parameters: Set up TSD Shift Medial simulator angle Lateral simulator angle TSD= SHIFT= MED SIM ANG LAT SIM ANG= 10. Center the beam on the setup point and set the TSD to the value determined by the calculator. 11. Move the field central axis over the breast to be treated (Figure 4) by shifting the table laterally the distance determined by the calculator. 12. Mark the new isocenter on the breast. This is the anterior projection of the treatment isocenter. 13. Rotate the gantry to the medial angle determined by the calculator. The edge of the field should pass through the setup point. If the edge of the field misses the setup point by more than a few millimeters, recheck the field size and all measurements to make sure they are correct. If necessary, return to step Use isocentric table rotation to swing the patient's feet 5 degrees away from the source of the beam. The basis for 5 degrees rotation is explained in Appendix B. 15. Rotate the collimator to achieve the desired beam entrance line, particularly at the upper medial corner (Figure 7 and 8). At this point, the physician should inspect the field projected on the patient. If the field is not satisfactory to the physician, recheck field size and all measurements. If necessary, return to step 8. 9
15 10
16 16. Make sure the amount of "flash" over the nipple is between 1 and 2 centimeters. If it is necessary to adjust the amount of flash, return to step 9, enter a new estimated field width in the calculator, and use new setup parameters. 17. Check the field length. The lower border should be on the intended inferior margin mark and the upper border should be at least 3-4 centimeters above the match line. If it is necessary to change the field length and it cannot be done symmetrically (keeping the same central axis position), return to step 3 and use a new field length with additional extension above the match line. 18. Hang the bead chain from the collimator head so that the shadow of the chain falls within 1 centimeter of the match line, but not overlying the match line. The chain must hang freely. The projection of the chain will show a vertical plane (parallel to the blocked edge of the supraclavicular field) during fluoroscopy and on the films (Figure 8). 19. Use fluoroscopy or radiography to verify that the BB markers along the match line are approximately parallel to the shadow of the chain. Make sure the medial and lateral entrance BB markers both lie upon the deep margin of the field, though they may be separated slightly due to the isocentric table rotation. Also check the amount of lung in the field, the depth of the upper medial corner, and any other clinically important factors. 20. When the physician is satisfied with the medial tangent, mark the field boundaries and the central axis with the green marking pen and record all setup parameters on the Breast Simulation Worksheet. 21. Take a medial tangent film. Use a straightedge to draw on the film the outline of a block that passes through the BB markers and is parallel to the chain (Figure 8). Note: The BB markers probably will not be perfectly aligned. Use the best fit. Do not use a curved line, because this block will define the edge of the beam that abuts the supraclavicular field in a coplanar manner (Figure 8). 22. Without moving the patient, rotate the gantry to the lateral angle determined by the calculator. 11
17 Note: Depending on your simulator, it may be necessary to move the patient laterally to allow sufficient clearance for the gantry. If it is necessary to move the patient, do so carefully with lateral table motion only, and return the patient to her original position after rotating the gantry. 23. Turn the collimator to the opposite (negative) of the angle used for the medial tangent (do not change the isocentric table position yet). The resultant field shows the exit line of the medial tangent. If this exit line is acceptable to the physician as the lateral entrance line, mark it with a dotted line. If the exit line is not acceptable, it is necessary to either return to step 1 and put new marks on the patient's skin or return to step 8 and take new measurements. Note: The most common correction necessary is to move the lateral entrance line either down (deeper) or up (shallower). Empirically, a +2-degree change in the chord angle moves the lateral entrance line approximately 1 centimeter deeper (and vice versa). However, it is still necessary to return to step 9. 12
18 24. Use the isocentric table rotation to swing the patient's feet to 5 degrees away from the source of the beam (10 degrees total). This will cause the projected lateral entrance line to move slightly. 25. Use a minor change in collimator angle to make the entrance line parallel with the entrance line marked in step Adjust the gantry angle until the two lines coincide (only a minor change in gantry angle should be necessary). 27. Record the new collimator and gantry angles on the Breast Simulation Worksheet. These are the final values to be used for treatment. 28. Hang the chain from the collimator head so that the shadow of the chain falls within 1 centimeter of the match line. (It may be necessary to suspend the chain from an IV pole or other temporary attachment point so that it does not rest against the simulator head and hangs freely.) 29. Use fluoroscopy or radiography to make the same checks specified in step Take a lateral tangent film and draw on the film the outline of a block as specified in step Mark the final portals on the patient's skin with the green marking pen and take AP and lateral Polaroid photographs for the patient's chart. 32. Tattoo the setup point, as shown in Figure 9. Make sure you tattoo the setup point rather than the midpoint of the medial entrance line (which is not exactly the same because of collimator rotation). The setup point may not lie exactly on the entrance line, but it is still the key point for future treatment. You may wish to tattoo other points as well (Figure 9). 33. Measure the separation from border to border and from the medial central axis to the lateral central axis, and record these measurements on the Breast Simulation Worksheet. 34. Take the patient's contour, by your usual method, for dosimetry. 13
19 35. Draw the Patient Setup Diagram (a sample is included in Appendix A) and fill in the required information. Mark tattoo placement on the diagram with an X. 36. Fabricate custom blocks. 2 2 Contact Diacor Inc. for information on the Portalcast Block Cutting and Casting System. This system is designed to allow custom blocks to be made quickly and accurately. 14
20 2.3 SETUP FOR TANGENT-ONLY FIELDS 1. The physician should use the red marking pen supplied with the MammoRx system to put preliminary marks on the patient's skin to show the intended medial, lateral, superior, and inferior borders of the tangent treatment area. 2. With the gantry vertical, put the central axis of the field on the midpoint of the intended medial entrance line. Use a preliminary TSD of 77 or 97 as applicable for 80- and 100- centimeter TAD machines, respectively. 3. Adjust the field length to match the superior and inferior marks. Note: You should be aware of the maximum working length of any wedges you are using. Do not exceed these limits. 4. Estimate the required field width based on breast size (a moderate-sized breast requires a field width of approximately 10 centimeters). Set the field width in accordance with your estimate. 5. Mark the central axis, which is referred to as the AP setup point. 6. Apply BB markers on the setup point and on the intended lateral entrance line in the axial plane of the setup point. 7. Use the caliper to measure (in a vertical plane) the distance between setup point and the lateral border (SEPARATION) and the angle of the chord that connects these two points (CALIPER ANGLE) (Figure 6). 8. Enter the distance measurement into the calculator as SEPARATION. Enter the estimated field width into the calculator as FIELD WIDTH. Enter the chord angle into the calculator as CALIPER ANGLE. Enter the simulator/accelerator target-axis distance (TAD) into the calculator as MACHINE TAD. Finally, indicate whether a left or right breast is to be treated by pressing the YES or NO button of the calculator. The calculator will then compute the following setup parameters: Set up TSD Shift Medial simulator angle Lateral simulator angle TSD= SHIFT= MED SIM ANG= LAT SIM ANG= 15
21 9. Center the beam on the setup point and set the TSD to the value determined by the calculator. 10. Move the field central axis over the breast to be treated (Figure 4) by shifting the table laterally the distance determined by the calculator. 11. Mark the new isocenter on the breast. This is the anterior projection of the treatment isocenter. 12. Rotate the gantry to the medial angle calculated by the calculator. The edge of the field should pass through the setup point. If the edge of the field misses the setup point by more than a few millimeters, recheck the field size and all measurements to make sure they are correct. If necessary, return to step Rotate the collimator to achieve the desired beam entrance line, particularly at the upper medial corner (Figures 7 and 8). At this point, the physician should inspect the field projected on the patient. If the field is not satisfactory to the physician, recheck field size and all measurements. If necessary, return to step Make sure the amount of "flash" over the nipple is between 1 and 2 centimeters. If it is necessary to adjust the amount of flash, return to step 8, enter a new estimated field width into the calculator, and use new setup parameters. 15. Check the field length. The upper and lower borders should be on the intended marks. If it is necessary to change the field length and it cannot be done symmetrically (keeping the same central axis position), return to step Use radiography to check the amount of lung in the field, the depth of the upper medial corner, the approximate coincidence of the medial and lateral entrance BB markers, and any other clinically important factors. 17. When the physician is satisfied with the medial tangent, mark the field boundaries and the central axis with the green marking pen and record all setup parameters on the Breast Simulation Worksheet. 18. Mark the central axis and take a film. 19. Without moving the patient, rotate the gantry to the lateral angle determined by the calculator. 16
22 Note: Depending on your simulator, it may be necessary to move the patient laterally to allow sufficient clearance for the gantry. If it is necessary to move the patient, do so carefully with lateral table motion only, and return the patient to her original position after rotating the gantry. 20. Turn the collimator to the opposite (negative) of the angle used for the medial tangent. 21. Check the lateral entrance line on the skin and use fluoroscopy to check field position. If both are satisfactory to the physician, mark and proceed. If unsatisfactory, return to step 1 and use new skin marks and/or measurements. Note: Empirically, a +2- degree change in the chest wall angle moves the lateral entrance line downward approximately 1 centimeter (and vice versa). However, it is still necessary to return to step Take a film and record the required data on the Breast Simulation Worksheet. 23. Mark the final portals on the patient's skin with the green marking pen and take AP and lateral Polaroid photographs for the patient's chart. 24. Tattoo as shown in Figure 10. Be sure that you tattoo the setup point, rather than the midpoint of the medial entrance line (which is not exactly the same because of collimator rotation). The setup point may not lie exactly on the entrance line, but it is still the key point for future treatment. You may wish to tattoo other points as well. 25. Measure the separation from border to border and from the medial central axis to the lateral central axis, and record these measurements on the Breast Simulation Worksheet. 26. Take the patient's contour by your usual method for dosimetry. 27. Draw the Patient Setup Diagram (a sample is included in Appendix A) and fill in the required information. Mark tattoo placement on the diagram with an X. 17
23 18
24 PART 3. TREATMENT PROCEDURES 3.1 POSITIONING THE PATIENT FOR TREATMENT 1. Preset the headrest and arm supports at the positions established for this patient during the initial positioning steps. Make sure that the pins for the arm supports are snug against the table edge. 2. Have the patient lie down and put her head in the headrest. Then have her straighten and adjust her shoulders and hips for comfort. 3. Raise the patient's arm and place it into the arm and wrist supports. 4. Pivot the wrist support to find a position that is comfortable for the patient. Make sure the upper arm is well cradled, not binding in the support and is out of the way of the tangential fields. 5. Make sure the patient is straight on the table. 3.2 TREATING THE PATIENT USING SUPRACLAVICULAR ANDTANGENT FIELDS 1. To set up the supraclavicular field, use a TSD of 80 or 100 centimeters, as applicable for your treatment machine. 2. Rotate the gantry medially to an angle of degrees as determined during simulation. 3. Position the supraclavicular central axis and adjust the field size. 4. Put a half-field (beamsplitter) block or the patient's custom block in place. 5. Use the red marking pen to dot the match line across the field. Use either the lateral line laser or lateral table movement to continue the line well into the axilla. 19
25 Note: This line should be reapplied each day. Encourage the patient to remove the line between treatments. This will help to "feather" the match plane dose over the course of the treatment. 6. When you are satisfied with the setup, either take a film or begin the treatment, as appropriate. 7. After treating the supraclavicular field, remove the bearnsplitter, change the field size to the appropriate tangent values, rotate the gantry to vertical, and place the central axis on the tangent setup point at the proper TSD. 8. Shift the table laterally to the new isocenter. 9. Rotate the gantry to the medial tangent treatment angle. 10. Use isocentric table rotation to swing the patient's feet 5 degrees away from the collimator. 11. Rotate the collimator to the proper setting. 12. Put the patient's medial custom block in place. Make sure the blocked edge coincides with the previously marked match line. You may use up to 0.5 centimeter of longitudinal table movement to achieve the proper match line. No other movement (vertical, lateral, collimator, or gantry) should be used. If necessary, consult with the physician or your supervisor. 13. If the portal is within acceptable tolerances of the simulation tattoos, take a film or begin the treatment, as appropriate. Use a wedge or compensator, if appropriate. Note: The problem of acceptable tolerances has no easy answer. Obviously, perfection cannot be expected. Sometimes the setup for a thin, cooperative patient will not vary from the simulation more than a few millimeters over a period of weeks. Other patients offer greater challenges. Alignment along the match line must be done accurately, so a reasonable amount of longitudinal freedom is necessary. The lateral entrance line will be especially variable. It is better to be too careful rather than the opposite. 14. After treating the medial field, move the gantry to the specified lateral angle and move the collimator to the specified angle for the lateral tangent (which because of table rotation is not simply the negative of the medial collimator angle, as is the case for tangent-only treatment.) 20
26 15. Use isocentric table rotation to move the patient's feet to 5 degrees away from the collimator (a total of 10 degrees of movement). 16. Put the patient's lateral custom block in place. Make sure the blocked edge coincides with the previously marked match line. Again, a small amount of longitudinal movement is acceptable to achieve a match. 17. When the port is within acceptable tolerances and on the match line, take a film or begin treatment, as appropriate. Use a wedge or compensator, if appropriate. 3.3 TREATING THE PATIENT USING TANGENT-ONLY FIELDS 1. Set the field size and place the central axis on the setup point at the specified TSD. 2. Shift laterally the calculated amount. 3. Position the gantry and collimator at the predetermined angles for medial tangent. 4. If acceptable, either take a film or begin treatment, as appropriate. Use a wedge or compensator, if appropriate. 5. Without moving the patient, rotate to the lateral gantry angle and the negative of the medial tangent collimator angle. 6. If acceptable, take a film or begin treatment, as appropriate. If appropriate, use a wedge or compensator. 21
27 APPENDIX A WORKSHEETS The following three worksheets are included in this appendix to assist you in recording the necessary patient information. You may copy the worksheet and setup diagrams in whatever quantity you need to meet your departmental requirements, or you may use any portion of them to create your own. You may also purchase them from Diacor, Inc. in 50-page tablets. A.1 BREAST SIMULATION WORKSHEET A.2 PATIENT SETUP DIAGRAM - LEFT A.3 PATIENT SETUP DIAGRAM - RIGHT 22
28
29
30
31 APPENDIX B ASSUMPTIONS B.1 SETUP ASSUMPTIONS Throughout the patient setup procedures we have made two assumptions which detract somewhat from the absolute accuracy of the geometry, but which we feel are justified for the sake of simplicity, reproducibility and avoidance of technologist error. The first assumption is that the angulation of the sternal region of the patient relative to horizontal and therefore the angulation of the collimator usually falls between 10 and 30º. Therefore, this angle was fixed in the equations at 20º(Figure B-1). Table B-1 shows the variation in the TSD, SHIFT, Medial Gantry Angle (MG) and Lateral Gantry Angle (LG) for different values of machine TAD, Separation (S), Field Width (W), Caliper Angle (A), and values of sternal angle (SA) from 0º to 30º. (These values are for a left breast). Note that significant changes in sternal angle result in relatively insignificant changes in TSD, etc. TABLE B-1 It is apparent from these calculations that there are no clinically significant changes in any of the important setup parameters within this range of sternal angles. 26
32 The second assumption is that the isocentric table angulation is fixed at 5º (we recommend you do this). Though this angle does not come into play in the equations for TSD, SHIFT, Medical Gantry Angle, and Lateral Gantry Angle, it does affect the coplanar match of the tangents with the supraclavicular field at the matchline. This angle is used to bring the source of the tangent fields into the match plane. As shown in Figure B-2, the magnitude of this angle depends upon the horizontal distance from the isocenter to the match plane, which is usually from 6 to 12 centimeters. This yields a range of angles from 3.5º to 7º for 100 cm machines and from 4.51º to 8.5º for 80 cm machines. We have chosen 5º as a reasonable approximation. However, you may wish to calculate and use an exact solution for each patient. The choice of 5º also recognizes that some tables may not have individual degree marks on the floor, whereas they will usually have 5º precision. B.2 GANTRY ANGLE CONVENTIONS The most common gantry angle conventions within radiotherapy are those of the Siemens (IEC) and Varian Corporation. The Siemens convention assumes that the machine indicates 0º when the beam is aimed at the floor and 90º when the machine aims at the left side of a supine patient. The Varian convention has 180º when the beam is aimed at the floor and 90º when the beam is aimed at the left side of a supine patient. Therefore, one can convert from the Siemens angles (S) to the Varian angles (V) through the equations (V) = (S), for 0 < (S) < 180 and (V) = (180 - (S)), for 180<(S) < 360 This conversion has been programmed into the MammoRx Breast Setup Calculator. Refer to the operating instructions provided with the MammoRx Breast Treatment System. Acknowledgments: 1. Siddon, R.L., Buck, B.A., Harris, J.R., Svensson, G.K.: Three-Field Technique for Breast Irradiation using Tangential Field Corner Blocks. Int. J. Radiation Oncology Biol. Phys., 9 : , Lichter, A.S., Fraass, B.A., Van de Geijn, J., Padikal, T.N.: A Technique for Breast Matching in Primary Breast Irradiation. Int. J. Radiation Oncology Biol. Phys. 9 : ,
33 28
34 29
Treatment Planning Techniques for Larger Body Habitus Patients for Breast/Chestwall and Regional Lymph Nodal Irradiation
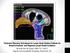 Treatment Planning Techniques for Larger Body Habitus Patients for Breast/Chestwall and Regional Lymph Nodal Irradiation By Ruth Ann M. Good, CMD. R.T. (R)(T) Virginia Commonwealth University, Richmond,
Treatment Planning Techniques for Larger Body Habitus Patients for Breast/Chestwall and Regional Lymph Nodal Irradiation By Ruth Ann M. Good, CMD. R.T. (R)(T) Virginia Commonwealth University, Richmond,
VariSource High Dose Rate Afterloader Procedures. For Performing Breast Brachytherapy with. The SAVI TM Applicator
 VariSource High Dose Rate Afterloader Procedures For Performing Breast Brachytherapy with The SAVI TM Applicator Contents I. CT Evaluation (~1 week prior to insertion) II. SAVI Applicator Implantation
VariSource High Dose Rate Afterloader Procedures For Performing Breast Brachytherapy with The SAVI TM Applicator Contents I. CT Evaluation (~1 week prior to insertion) II. SAVI Applicator Implantation
13 QUALITY ASSURANCE OF A LINEAR ACCELERATOR 13.1 COLLIMATOR ISOCENTER, JAWS, LIGHT FIELD VS INDICATORS, COLLIMATOR ANGLE INDICATORS.
 13 QUALITY ASSURANCE OF A LINEAR ACCELERATOR 13.1 COLLIMATOR ISOCENTER, JAWS, LIGHT FIELD VS INDICATORS, COLLIMATOR ANGLE INDICATORS. 13.1.1 TRAINING GOAL 13.1.1.1 Among the responsabilities of a medical
13 QUALITY ASSURANCE OF A LINEAR ACCELERATOR 13.1 COLLIMATOR ISOCENTER, JAWS, LIGHT FIELD VS INDICATORS, COLLIMATOR ANGLE INDICATORS. 13.1.1 TRAINING GOAL 13.1.1.1 Among the responsabilities of a medical
Planning Assignment (3 field rectum)
 Megan Sullivan Clinical Lab Rectum April 25, 2016 Planning Assignment (3 field rectum) Use a CT dataset of the pelvis. Create a CTV by contouring the rectum (start at the anus and stop at the turn where
Megan Sullivan Clinical Lab Rectum April 25, 2016 Planning Assignment (3 field rectum) Use a CT dataset of the pelvis. Create a CTV by contouring the rectum (start at the anus and stop at the turn where
TG-119 IMRT Commissioning Tests Instructions for Planning, Measurement, and Analysis Version 10/21/2009
 TG-119 IMRT Commissioning Tests Instructions for Planning, Measurement, and Analysis Version 10/21/2009 DISCLAIMER: This publication and associated spreadsheets and digital files are based on sources and
TG-119 IMRT Commissioning Tests Instructions for Planning, Measurement, and Analysis Version 10/21/2009 DISCLAIMER: This publication and associated spreadsheets and digital files are based on sources and
Field size and depth dependence of wedge factor for internal wedge of dual energy linear accelerator
 Journal of BUON 8: 55-59, 2003 2003 Zerbinis Medical Publications. Printed in Greece ORIGINAL ARTICLE Field size and depth dependence of wedge factor for internal wedge of dual energy linear accelerator
Journal of BUON 8: 55-59, 2003 2003 Zerbinis Medical Publications. Printed in Greece ORIGINAL ARTICLE Field size and depth dependence of wedge factor for internal wedge of dual energy linear accelerator
Review of fundamental photon dosimetry quantities
 Review of fundamental photon dosimetry quantities Narayan Sahoo Main sources of the materials included in this lecture notes are: (1) Radiation Oncology Physics: A Handbook for Teachers and Students Edited
Review of fundamental photon dosimetry quantities Narayan Sahoo Main sources of the materials included in this lecture notes are: (1) Radiation Oncology Physics: A Handbook for Teachers and Students Edited
Outline. Chapter 11 Treatment Planning Single Beams. Patient dose calculation. Patient dose calculation. Effect of the curved contour surface
 Chapter 11 reatment Planning Single Beams Radiation Dosimetry I Outline Basic terminology Curved contour surface correction (bolus, compensators, wedges) Oblique beam incidence Correction for tissue inhomogeneities
Chapter 11 reatment Planning Single Beams Radiation Dosimetry I Outline Basic terminology Curved contour surface correction (bolus, compensators, wedges) Oblique beam incidence Correction for tissue inhomogeneities
Relative Dosimetry. Photons
 Relative Dosimetry Photons What you need to measure! Required Data (Photon) Central Axis Percent Depth Dose Tissue Maximum Ratio Scatter Maximum Ratio Output Factors S c & S cp! S p Beam profiles Wedge
Relative Dosimetry Photons What you need to measure! Required Data (Photon) Central Axis Percent Depth Dose Tissue Maximum Ratio Scatter Maximum Ratio Output Factors S c & S cp! S p Beam profiles Wedge
Commissioning an IMRT System for MLC Delivery. Gary A. Ezzell., Ph.D. Mayo Clinic Scottsdale
 Commissioning an IMRT System for MLC Delivery Gary A. Ezzell., Ph.D. Mayo Clinic Scottsdale Taking the broad view of commissioning Commissioning elements Validating the dosimetry system Commissioning the
Commissioning an IMRT System for MLC Delivery Gary A. Ezzell., Ph.D. Mayo Clinic Scottsdale Taking the broad view of commissioning Commissioning elements Validating the dosimetry system Commissioning the
Absorption measurements for a carbon fiber couch top and its modelling in a treatment planning system
 Absorption measurements for a carbon fiber couch top and its modelling in a treatment planning system G. Kunz, F. Hasenbalg, P. Pemler 1 1 Klinik für Radio-Onkologie und Nuklearmedizin, Stadtspital Triemli
Absorption measurements for a carbon fiber couch top and its modelling in a treatment planning system G. Kunz, F. Hasenbalg, P. Pemler 1 1 Klinik für Radio-Onkologie und Nuklearmedizin, Stadtspital Triemli
The Royal Australian and New Zealand College of Radiologists. FRANZCR Examination Part I Radiation Oncology. Radiotherapeutic Physics.
 FRANZCR Examination Part I Radiation Oncology Radiotherapeutic Physics Candidate No.: The Royal Australian and New Zealand College of Radiologists FRANZCR Examination Part I Radiation Oncology Radiotherapeutic
FRANZCR Examination Part I Radiation Oncology Radiotherapeutic Physics Candidate No.: The Royal Australian and New Zealand College of Radiologists FRANZCR Examination Part I Radiation Oncology Radiotherapeutic
Guidelines for Using the UMTRI ATD Positioning Procedure for ATD and Seat Positioning
 Guidelines for Using the UMTRI ATD Positioning Procedure for ATD and Seat Positioning July 2002 Insurance Institute for Highway Safety Guidelines for Using the UMTRI ATD Positioning Procedure for ATD and
Guidelines for Using the UMTRI ATD Positioning Procedure for ATD and Seat Positioning July 2002 Insurance Institute for Highway Safety Guidelines for Using the UMTRI ATD Positioning Procedure for ATD and
ANATOMICAL TERMINOLOGY: Body Movement
 ANATOMICAL TERMINOLOGY: Body Movement Fill in the Blank 1. Johnny has just performed a bicep curl (up) in weight training class. What motion did his arm make from the elbow? 2. Anita has just pointed her
ANATOMICAL TERMINOLOGY: Body Movement Fill in the Blank 1. Johnny has just performed a bicep curl (up) in weight training class. What motion did his arm make from the elbow? 2. Anita has just pointed her
Dosimetric Calculations. Lonny Trestrail
 Dosimetric Calculations Lonny Trestrail 20 October 2008 Objectives Dose Distribution Measurements PDD, OCR TAR, SAR, TPR, TMR, SPR, SMR Arc or Rotational Therapy Isodose Curves Point Dose Calculations
Dosimetric Calculations Lonny Trestrail 20 October 2008 Objectives Dose Distribution Measurements PDD, OCR TAR, SAR, TPR, TMR, SPR, SMR Arc or Rotational Therapy Isodose Curves Point Dose Calculations
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 3, NUMBER 4, FALL 2002
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 3, NUMBER 4, FALL 2002 Comparison of monitor unit calculations performed with a 3D computerized planning system and independent hand calculations: Results
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 3, NUMBER 4, FALL 2002 Comparison of monitor unit calculations performed with a 3D computerized planning system and independent hand calculations: Results
Math Review. Overview
 Drawn by Steve Yan, CMD Math Review Shirley Ann Pinegar-Johnston MS RT(R)(T)CMD Overview Drawn by Steve Yan, CMD Divergence & Intensity DIVERGENCE X-rays travel in Straight but Divergent lines INTENSITY
Drawn by Steve Yan, CMD Math Review Shirley Ann Pinegar-Johnston MS RT(R)(T)CMD Overview Drawn by Steve Yan, CMD Divergence & Intensity DIVERGENCE X-rays travel in Straight but Divergent lines INTENSITY
SnapShot IMRT with compensators and FFF beams
 SnapShot IMRT with compensators and FFF beams Vladimir Feygelman, PhD (1) Moffitt Cancer Center, Tampa, FL, USA Disclosure VF has a sponsored research agreement with.decimal. A short history of radiotherapy
SnapShot IMRT with compensators and FFF beams Vladimir Feygelman, PhD (1) Moffitt Cancer Center, Tampa, FL, USA Disclosure VF has a sponsored research agreement with.decimal. A short history of radiotherapy
The Fundamentals of Putting
 The Fundamentals of Putting Episode 1 - Setup and Aiming A proper setup position is a prerequisite of a good putt. Setup includes body posture, gripping the putter, alignment of body relative to the ball
The Fundamentals of Putting Episode 1 - Setup and Aiming A proper setup position is a prerequisite of a good putt. Setup includes body posture, gripping the putter, alignment of body relative to the ball
kvue IGRT Couch top One couch top, multiple treatment solutions For Varian, Elekta, Siemens, Proton and more The Best of Both Worlds
 TM kvue IGRT Couch top One couch top, multiple treatment solutions For Varian, Elekta, Siemens, Proton and more kvue The Best of Both Worlds kvue IGRT COUCH TOP One couch top, multiple treatment solutions
TM kvue IGRT Couch top One couch top, multiple treatment solutions For Varian, Elekta, Siemens, Proton and more kvue The Best of Both Worlds kvue IGRT COUCH TOP One couch top, multiple treatment solutions
Basics of Proton Therapy. Proton Treatment Planning and Beam Optimization
 Basics of Proton Therapy Proton Treatment Planning and Beam Optimization SAM Educational Session, WE D BRB 2 Mark Pankuch, PhD Northwestern Medicine Chicago Proton Center Today s objectives Review the
Basics of Proton Therapy Proton Treatment Planning and Beam Optimization SAM Educational Session, WE D BRB 2 Mark Pankuch, PhD Northwestern Medicine Chicago Proton Center Today s objectives Review the
Constancy checks of well-type ionization chambers with external-beam radiation units
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 16, NUMBER 6, 2015 Constancy checks of well-type ionization chambers with external-beam radiation units Sara L. Hackett, 1a Benjamin Davis, 2 Andrew
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 16, NUMBER 6, 2015 Constancy checks of well-type ionization chambers with external-beam radiation units Sara L. Hackett, 1a Benjamin Davis, 2 Andrew
THE ARENA TABLE OF CONTENTS 6 THE ARENA OVERVIEW Dimensions and Tolerances... 2
 Section 6 THE ARENA TABLE OF CONTENTS 6 THE ARENA... 2 6.1 OVERVIEW... 2 6.1.1 Dimensions and Tolerances... 2 6.2 PLAYING FIELD... 4 6.2.1 Boundaries and Markings... 4 6.2.2 The RACK... 5 6.3 GAME PIECES...
Section 6 THE ARENA TABLE OF CONTENTS 6 THE ARENA... 2 6.1 OVERVIEW... 2 6.1.1 Dimensions and Tolerances... 2 6.2 PLAYING FIELD... 4 6.2.1 Boundaries and Markings... 4 6.2.2 The RACK... 5 6.3 GAME PIECES...
CHAPTER 4 PRE TREATMENT PATIENT SPECIFIC QUALITY ASSURANCE OF RAPIDARC PLANS
 47 CHAPTER 4 PRE TREATMENT PATIENT SPECIFIC QUALITY ASSURANCE OF RAPIDARC PLANS 4.1 INTRODUCTION Advanced treatment techniques use optimized radiation beam intensities to conform dose distribution to the
47 CHAPTER 4 PRE TREATMENT PATIENT SPECIFIC QUALITY ASSURANCE OF RAPIDARC PLANS 4.1 INTRODUCTION Advanced treatment techniques use optimized radiation beam intensities to conform dose distribution to the
Monitor Unit Calculations Part 1. Return to our first patient. Purpose. 62 yr old woman with Stage IIIB (T1N3M0) NSCLC rt lower lobe Dose prescription
 Monitor Unit Calculations Part 1 George Starkschall, Ph.D. Department of Radiation Physics U.T. M.D. Anderson Cancer Center Return to our first patient 62 yr old woman with Stage IIIB (T1N3M0) NSCLC rt
Monitor Unit Calculations Part 1 George Starkschall, Ph.D. Department of Radiation Physics U.T. M.D. Anderson Cancer Center Return to our first patient 62 yr old woman with Stage IIIB (T1N3M0) NSCLC rt
Proton Therapy QA Tools
 Proton Therapy QA Tools A complete range of tools for absolute dosimetry, machine QA and patient plan verification Introduction During the past years more and more heavy particle therapy centers, especially
Proton Therapy QA Tools A complete range of tools for absolute dosimetry, machine QA and patient plan verification Introduction During the past years more and more heavy particle therapy centers, especially
JAECO/Rancho MultiLink. Mobile Arm Support (MAS) System
 JAECO/Rancho MultiLink Mobile Arm Support (MAS) System Instructions for Setup and Functional Adjustments June 11, 2004 Funded by National Institute for Disability & Rehabilitation Research (NIDRR) Developed
JAECO/Rancho MultiLink Mobile Arm Support (MAS) System Instructions for Setup and Functional Adjustments June 11, 2004 Funded by National Institute for Disability & Rehabilitation Research (NIDRR) Developed
Viva TPS. TS11/15 Total Stations Check and Adjust Procedure. October Summary
 Viva TPS October 2010 TS11/15 Total Stations Summary Leica builds total stations to the highest quality and calibrates each instrument before it leaves the Factory. After the instrument is shipped or used
Viva TPS October 2010 TS11/15 Total Stations Summary Leica builds total stations to the highest quality and calibrates each instrument before it leaves the Factory. After the instrument is shipped or used
ANALYSIS OF OFF-AXIS ENHANCDED DYNAMIC WEDGE DOSIMETRY USING A 2D DIODE ARRAY A CREATIVE PROJECT (3 SEMESTER HOURS) SUBMITTED TO THE GRADUATE SCHOOL
 ANALYSIS OF OFF-AXIS ENHANCDED DYNAMIC WEDGE DOSIMETRY USING A 2D DIODE ARRAY A CREATIVE PROJECT (3 SEMESTER HOURS) SUBMITTED TO THE GRADUATE SCHOOL FOR THE DEGREE MASTER OF ARTS BY CHARLES TRAVIS WEBB
ANALYSIS OF OFF-AXIS ENHANCDED DYNAMIC WEDGE DOSIMETRY USING A 2D DIODE ARRAY A CREATIVE PROJECT (3 SEMESTER HOURS) SUBMITTED TO THE GRADUATE SCHOOL FOR THE DEGREE MASTER OF ARTS BY CHARLES TRAVIS WEBB
Commissioning and quality assurance of a commercial intensity modulated radiotherapy (IMRT) treatment planning system PrecisePLAN
 22 Turkish Journal of Cancer Volume 37, No.1, 2007 Commissioning and quality assurance of a commercial intensity modulated radiotherapy (IMRT) treatment planning system PrecisePLAN SATISH PELAGADE 1, KALPANA
22 Turkish Journal of Cancer Volume 37, No.1, 2007 Commissioning and quality assurance of a commercial intensity modulated radiotherapy (IMRT) treatment planning system PrecisePLAN SATISH PELAGADE 1, KALPANA
Guidelines for Using the UMTRI ATD Positioning Procedure for ATD and Seat Positioning (Version III) December 2003
 Guidelines for Using the UMTRI ATD Positioning Procedure for ATD and Seat Positioning (Version III) December 2003 Insurance Institute for Highway Safety Guidelines for Using the UMTRI ATD Positioning Procedure
Guidelines for Using the UMTRI ATD Positioning Procedure for ATD and Seat Positioning (Version III) December 2003 Insurance Institute for Highway Safety Guidelines for Using the UMTRI ATD Positioning Procedure
A Low Cost Digital Angle Gage, version 3
 A Low Cost Digital Angle Gage, version 3 By R. G. Sparber Copyleft protects this document. 1 Sometimes re-inventing the wheel has advantages. What you see here is just a variation on a sine bar. The accuracy
A Low Cost Digital Angle Gage, version 3 By R. G. Sparber Copyleft protects this document. 1 Sometimes re-inventing the wheel has advantages. What you see here is just a variation on a sine bar. The accuracy
MASTER TRUING STAND TS-3. Optional Dial indicator set with brackets Dial indicator bracket set only
 MASTER TRUING STAND TS-3 3 2 1 3 8 9 4 10 7 6 5 12 13 Optional 1555-1 Dial indicator set with brackets 1556-1 Dial indicator bracket set only 49 11 16 14 15 48 32 31 37 38 20 19 17 18 34 39 21 36 22 33
MASTER TRUING STAND TS-3 3 2 1 3 8 9 4 10 7 6 5 12 13 Optional 1555-1 Dial indicator set with brackets 1556-1 Dial indicator bracket set only 49 11 16 14 15 48 32 31 37 38 20 19 17 18 34 39 21 36 22 33
Axis of rotation is always perpendicular to the plane of movement
 Sports scientists and medical practitioners use formal terms to describe directionality, joint movement, and muscle movement. These universal terms let us use fewer words when describing movement, teaching,
Sports scientists and medical practitioners use formal terms to describe directionality, joint movement, and muscle movement. These universal terms let us use fewer words when describing movement, teaching,
ISO INTERNATIONAL STANDARD
 INTERNATIONAL STANDARD ISO 1940-1 Second edition 2003-08-15 Mechanical vibration Balance quality requirements for rotors in a constant (rigid) state Part 1: Specification and verification of balance tolerances
INTERNATIONAL STANDARD ISO 1940-1 Second edition 2003-08-15 Mechanical vibration Balance quality requirements for rotors in a constant (rigid) state Part 1: Specification and verification of balance tolerances
Stretch Net tubular elastic bandage Illustrated Guide
 Stretch Net tubular elastic bandage Illustrated Guide www.deroyal.com SECTION PAGE SIZE Product Listing... 3 ALL Finger... 5 1-2 Foot.... 6 3-4 Elbow, Forearm, or Knee... 7 3-4 Hand... 8 3-4 Head - Full
Stretch Net tubular elastic bandage Illustrated Guide www.deroyal.com SECTION PAGE SIZE Product Listing... 3 ALL Finger... 5 1-2 Foot.... 6 3-4 Elbow, Forearm, or Knee... 7 3-4 Hand... 8 3-4 Head - Full
DX2/DXX Operating Instructions
 CHECK LINE BY ELECTROMATIC DX2/DXX Operating Instructions CHECK LINE INSTRUMENTS ELECTROMATIC E Q U I P M E N T C O., I N C. 600 Oakland Ave., Cedarhurst, NY 11516 U.S.A. TEL: 516-295-4300 FAX: 516-295-4399
CHECK LINE BY ELECTROMATIC DX2/DXX Operating Instructions CHECK LINE INSTRUMENTS ELECTROMATIC E Q U I P M E N T C O., I N C. 600 Oakland Ave., Cedarhurst, NY 11516 U.S.A. TEL: 516-295-4300 FAX: 516-295-4399
Scleral Fitting Guide
 Scleral Fitting Guide Scleral Lens Design...3 Fitting Philosophy...4 Select a Diagnostic Lens...5 Initial Lens Evaluation...6 Assess Scleral Landing Zone (SLZ), Sagittal Depth, Limbal Clearance, Lens Power...7-10
Scleral Fitting Guide Scleral Lens Design...3 Fitting Philosophy...4 Select a Diagnostic Lens...5 Initial Lens Evaluation...6 Assess Scleral Landing Zone (SLZ), Sagittal Depth, Limbal Clearance, Lens Power...7-10
CLINICAL IMPLEMENTATION OF RAPIDARC Treatment Planning Strategies to Improve Dose Distributions
 CLINICAL IMPLEMENTATION OF RAPIDARC Treatment Planning Strategies to Improve Dose Distributions Rebecca M. Howell, Ph.D., D.A.B.R, The University of Texas at M.D. Anderson Cancer Center Overview 2 Commissioning
CLINICAL IMPLEMENTATION OF RAPIDARC Treatment Planning Strategies to Improve Dose Distributions Rebecca M. Howell, Ph.D., D.A.B.R, The University of Texas at M.D. Anderson Cancer Center Overview 2 Commissioning
Review Supplement Info Waist-to hip Ratio, Gurth Measurements & Skin Fold
 THIS MATERIAL IS A SUPPLEMENTAL TOOL. IT IS NOT INTENDED TO REPLACE INFORMATION PROVIDED IN YOUR TEXT AND/OR STUDENT HAND-BOOKS. Assessing Percent Body Fat: While hydrostatic weighing and the Bod Pod are
THIS MATERIAL IS A SUPPLEMENTAL TOOL. IT IS NOT INTENDED TO REPLACE INFORMATION PROVIDED IN YOUR TEXT AND/OR STUDENT HAND-BOOKS. Assessing Percent Body Fat: While hydrostatic weighing and the Bod Pod are
ZIPWAKE DYNAMIC TRIM CONTROL SYSTEM OUTLINE OF OPERATING PRINCIPLES BEHIND THE AUTOMATIC MOTION CONTROL FEATURES
 ZIPWAKE DYNAMIC TRIM CONTROL SYSTEM OUTLINE OF OPERATING PRINCIPLES BEHIND THE AUTOMATIC MOTION CONTROL FEATURES TABLE OF CONTENTS 1 INTRODUCTION 3 2 SYSTEM COMPONENTS 3 3 PITCH AND ROLL ANGLES 4 4 AUTOMATIC
ZIPWAKE DYNAMIC TRIM CONTROL SYSTEM OUTLINE OF OPERATING PRINCIPLES BEHIND THE AUTOMATIC MOTION CONTROL FEATURES TABLE OF CONTENTS 1 INTRODUCTION 3 2 SYSTEM COMPONENTS 3 3 PITCH AND ROLL ANGLES 4 4 AUTOMATIC
Principles of glider flight
 Principles of glider flight [ Lecture 2: Control and stability ] Richard Lancaster Email: Richard@RJPLancaster.net Twitter: @RJPLancaster ASK-21 illustrations Copyright 1983 Alexander Schleicher GmbH &
Principles of glider flight [ Lecture 2: Control and stability ] Richard Lancaster Email: Richard@RJPLancaster.net Twitter: @RJPLancaster ASK-21 illustrations Copyright 1983 Alexander Schleicher GmbH &
Comparison of ionization chambers of various volumes for IMRT absolute dose verification
 Comparison of ionization chambers of various volumes for IMRT absolute dose verification Leonid B. Leybovich, a) Anil Sethi, and Nesrin Dogan Department of Radiation Oncology, Loyola University Medical
Comparison of ionization chambers of various volumes for IMRT absolute dose verification Leonid B. Leybovich, a) Anil Sethi, and Nesrin Dogan Department of Radiation Oncology, Loyola University Medical
Fix Your Swing Series. Table of Contents
 Fix Your Swing Series Table of Contents 1. Hit More Fairways 2. Fix Your Setup 3. Fix Your Ball Position 4. Fix Your Takeaway 5. Fix Your Backswing 6. Fix the Top of Your Swing 7. Fix Your Downswing 8.
Fix Your Swing Series Table of Contents 1. Hit More Fairways 2. Fix Your Setup 3. Fix Your Ball Position 4. Fix Your Takeaway 5. Fix Your Backswing 6. Fix the Top of Your Swing 7. Fix Your Downswing 8.
Implementing Provisions for Art. 411 of the ICR Ski Jumping
 JUMPING HILLS CONSTRUCTION NORM 2018 Implementing Provisions for Art. 411 of the ICR Ski Jumping Author: Hans-Heini Gasser (SUI) EDITION NOVEMBER 2018 Table of Contents Page 1. Preliminary Remarks 3 2.
JUMPING HILLS CONSTRUCTION NORM 2018 Implementing Provisions for Art. 411 of the ICR Ski Jumping Author: Hans-Heini Gasser (SUI) EDITION NOVEMBER 2018 Table of Contents Page 1. Preliminary Remarks 3 2.
Radiotherapy Treatment Planning and Delivery
 Radiotherapy Treatment Planning and Delivery SCOPE 1: Study of Chemoradiotherapy in Oesophageal Cancer Plus or Minus Erbitux A randomised phase II/III multi-centre clinical trial of definitive chemo-radiation,
Radiotherapy Treatment Planning and Delivery SCOPE 1: Study of Chemoradiotherapy in Oesophageal Cancer Plus or Minus Erbitux A randomised phase II/III multi-centre clinical trial of definitive chemo-radiation,
TEST REPORT BEAMSCAN WITH HALCYON
 TEST REPORT BEAMSCAN WITH HALCYON UZ Leuven, November 20 th, 2017 + = Ideal BEAMSCAN tank dimensions to fit perfectly into the Halcyon bore Fast tank positioning using the Halcyon lasers, no electronics
TEST REPORT BEAMSCAN WITH HALCYON UZ Leuven, November 20 th, 2017 + = Ideal BEAMSCAN tank dimensions to fit perfectly into the Halcyon bore Fast tank positioning using the Halcyon lasers, no electronics
Introduction. Introduction. The CyberKnife SRS/SBRT System. Introduction. Contour Structures. CyberKnife Components
 Introduction The CyberKnife SRS/SBRT System James M. Hevezi,, Ph.D., FACR CyberKnife Unit San Antonio, Texas CyberKnife Components Treatment Delivery (G3 Platform San Antonio) Robot (modified German auto
Introduction The CyberKnife SRS/SBRT System James M. Hevezi,, Ph.D., FACR CyberKnife Unit San Antonio, Texas CyberKnife Components Treatment Delivery (G3 Platform San Antonio) Robot (modified German auto
Structure (Down plane)
 By Lauren Russell Structure (Down plane) The body (toes, knees, hips, wrists and shoulders) is aligned parallel to the intended target line. The torso is tilted over the ball from the hips whilst maintaining
By Lauren Russell Structure (Down plane) The body (toes, knees, hips, wrists and shoulders) is aligned parallel to the intended target line. The torso is tilted over the ball from the hips whilst maintaining
Physics and Quality Assurance
 Disclosure Physics and Quality Assurance Consultancy agreements with Nucletron, Hologic Mahta M. McKee, MS, DABR Department of Radiation Oncology Wake Forest University Health Sciences Agenda Current Treatment
Disclosure Physics and Quality Assurance Consultancy agreements with Nucletron, Hologic Mahta M. McKee, MS, DABR Department of Radiation Oncology Wake Forest University Health Sciences Agenda Current Treatment
High Speed Direct SAD Radiosurgery Beam Scanner
 Open Access Original Article DOI: 10.7759/cureus.20 High Speed Direct SAD Radiosurgery Beam Scanner Walter Nikesch 1, James M. Hevezi 2, Irene Monterroso 3, Daniel Navarro 4, James G. Schwade 5 1. CyberKnife
Open Access Original Article DOI: 10.7759/cureus.20 High Speed Direct SAD Radiosurgery Beam Scanner Walter Nikesch 1, James M. Hevezi 2, Irene Monterroso 3, Daniel Navarro 4, James G. Schwade 5 1. CyberKnife
NIHR Southampton Biomedical Research Centre
 The NIHR Southampton (BRC) has a tight quality assurance system for the writing, reviewing and updating of Standard Operating Procedures. As such, version-controlled and QA authorised Standard Operating
The NIHR Southampton (BRC) has a tight quality assurance system for the writing, reviewing and updating of Standard Operating Procedures. As such, version-controlled and QA authorised Standard Operating
The dose distribution of medium energy electron boosts to the laryngectomy stoma
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 2, NUMBER 1, WINTER 2001 The dose distribution of medium energy electron boosts to the laryngectomy stoma Ellen D. Yorke* Memorial Sloan-Kettering Cancer
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 2, NUMBER 1, WINTER 2001 The dose distribution of medium energy electron boosts to the laryngectomy stoma Ellen D. Yorke* Memorial Sloan-Kettering Cancer
ISO INTERNATIONAL STANDARD. Ergonomics Manual handling Part 1: Lifting and carrying
 INTERNATIONAL STANDARD ISO 11228-1 First edition 2003-05-15 Ergonomics Manual handling Part 1: Lifting and carrying Ergonomie Manutention manuelle Partie 1: Manutention verticale et manutention horizontale
INTERNATIONAL STANDARD ISO 11228-1 First edition 2003-05-15 Ergonomics Manual handling Part 1: Lifting and carrying Ergonomie Manutention manuelle Partie 1: Manutention verticale et manutention horizontale
Anatomy of a Salmon Fly
 Anatomy of a Salmon Fly Aleksy Pawluczuk About the author Aleksy Pawluczuk is a designer, sculptor, and photographer based in Kraków, Poland. He has run his own design, screen print, prepress, and advertising
Anatomy of a Salmon Fly Aleksy Pawluczuk About the author Aleksy Pawluczuk is a designer, sculptor, and photographer based in Kraków, Poland. He has run his own design, screen print, prepress, and advertising
Table of Contents FIRST 2005 FIRST Robotics Competition Manual: Section 3 The Arena rev B Page 1 of 8
 Table of Contents 3 THE ARENA...2 3.1 OVERVIEW...2 3.1.1 Dimensions and Tolerances...3 3.2 PLAYING FIELD...4 3.2.1 Boundaries and Markings...4 3.2.2 Goals...5 3.2.3 Center Goal...5 3.2.4 Tetra Loading
Table of Contents 3 THE ARENA...2 3.1 OVERVIEW...2 3.1.1 Dimensions and Tolerances...3 3.2 PLAYING FIELD...4 3.2.1 Boundaries and Markings...4 3.2.2 Goals...5 3.2.3 Center Goal...5 3.2.4 Tetra Loading
Swimming practical examination support materials
 Swimming Curriculum Council, 2011 This document apart from any third party copyright material contained in it may be freely copied, or communicated on an intranet, for non-commercial purposes by educational
Swimming Curriculum Council, 2011 This document apart from any third party copyright material contained in it may be freely copied, or communicated on an intranet, for non-commercial purposes by educational
DISTRIBUTION: Electronic Recipients List TRANSMITTAL LETTER NO. (13-01) MINNESOTA DEPARTMENT OF TRANSPORTATION. MANUAL: Road Design English Manual
 DISTRIBUTION: Electronic Recipients List MINNESOTA DEPARTMENT OF TRANSPORTATION DEVELOPED BY: Design Standards Unit ISSUED BY: Office of Project Management and Technical Support TRANSMITTAL LETTER NO.
DISTRIBUTION: Electronic Recipients List MINNESOTA DEPARTMENT OF TRANSPORTATION DEVELOPED BY: Design Standards Unit ISSUED BY: Office of Project Management and Technical Support TRANSMITTAL LETTER NO.
ROYAL CANADIAN AIR CADETS PROFICIENCY LEVEL FOUR INSTRUCTIONAL GUIDE SECTION 2 EO M DESCRIBE THE MAGNETIC COMPASS PREPARATION
 ROYAL CANADIAN AIR CADETS PROFICIENCY LEVEL FOUR INSTRUCTIONAL GUIDE SECTION 2 EO M437.02 DESCRIBE THE MAGNETIC COMPASS Total Time: 30 min PREPARATION PRE-LESSON INSTRUCTIONS Resources needed for the delivery
ROYAL CANADIAN AIR CADETS PROFICIENCY LEVEL FOUR INSTRUCTIONAL GUIDE SECTION 2 EO M437.02 DESCRIBE THE MAGNETIC COMPASS Total Time: 30 min PREPARATION PRE-LESSON INSTRUCTIONS Resources needed for the delivery
Only 8% to go. TOTAL 1494 of 1623 ACTIVE INSTITUTIONS (92%) May-09. May-04 Nov-04. May-07. Nov-02 May-03. Nov-05. Nov-06. Nov-07 May-08.
 Clinical Implementation of the TG-51 Protocol David Followill Radiological Physics Center Houston Texas 2009 AAPM Summer School Educational Objectives Improve your understanding of how to implement TG-51
Clinical Implementation of the TG-51 Protocol David Followill Radiological Physics Center Houston Texas 2009 AAPM Summer School Educational Objectives Improve your understanding of how to implement TG-51
IMRT in clinical practice at the UMC-Utrecht. Utrecht
 3 IMRT in clinical practice at the UMC-Utrecht Utrecht Clinical use of IMRT Improvement of local control without increased incidence of normal tissue complications + Dose escalation in the prostate Step-and
3 IMRT in clinical practice at the UMC-Utrecht Utrecht Clinical use of IMRT Improvement of local control without increased incidence of normal tissue complications + Dose escalation in the prostate Step-and
RESPIRATORY MOTION IN RADIATION THERAPY
 RESPIRATORY MOTION IN RADIATION THERAPY Significant effect on targets in the chest and upper abdominal cavities Can cause difficulty in reproducing radiation planning protocols in radiation treatment sessions
RESPIRATORY MOTION IN RADIATION THERAPY Significant effect on targets in the chest and upper abdominal cavities Can cause difficulty in reproducing radiation planning protocols in radiation treatment sessions
Operating & Maintenance MANUAL
 Operating & Maintenance MANUAL Thank You for purchasing the golf industry s state-of-the-art STEELCLUB Putter Angle Machine. You should find it simple to operate. Please follow the instructions in this
Operating & Maintenance MANUAL Thank You for purchasing the golf industry s state-of-the-art STEELCLUB Putter Angle Machine. You should find it simple to operate. Please follow the instructions in this
S0300-A6-MAN-010 CHAPTER 2 STABILITY
 CHAPTER 2 STABILITY 2-1 INTRODUCTION This chapter discusses the stability of intact ships and how basic stability calculations are made. Definitions of the state of equilibrium and the quality of stability
CHAPTER 2 STABILITY 2-1 INTRODUCTION This chapter discusses the stability of intact ships and how basic stability calculations are made. Definitions of the state of equilibrium and the quality of stability
TRAINING LAB BLOOD AS EVIDENCE BLOOD DROPS FALLING AT AN ANGLE NAME
 TRAINING LAB BLOOD AS EVIDENCE BLOOD DROPS FALLING AT AN ANGLE NAME Background: You just completed studying the behavior of passive blood drops that drip straight down from a wound, but not all blood drops
TRAINING LAB BLOOD AS EVIDENCE BLOOD DROPS FALLING AT AN ANGLE NAME Background: You just completed studying the behavior of passive blood drops that drip straight down from a wound, but not all blood drops
CHAPTER 4 U10 U13 2 PERSON RESCUE AND RESUSCITATION COMPETITION RULES AND PROCEDURES A GENERAL COMPETITION CONDITIONS C ERROR SCHEDULE
 CHAPTER 4 U0 U3 2 PERSON RESCUE AND RESUSCITATION COMPETITION RULES AND PROCEDURES A GENERAL. The 2 person R&R is conducted in the same arena as other R&R events and provides the opportunities to introduce
CHAPTER 4 U0 U3 2 PERSON RESCUE AND RESUSCITATION COMPETITION RULES AND PROCEDURES A GENERAL. The 2 person R&R is conducted in the same arena as other R&R events and provides the opportunities to introduce
Colorado Division of Fire Prevention & Control Driver Operator JPRs (NFPA 1002, 2014 Edition)
 Colorado Division of Fire Prevention & Control Driver Operator JPRs ( Edition) JPR # Task Initial Certification JPR Requirement: 8 Mandatory Renewal JPR Requirement: 100% of All JPRs (including all subsections)
Colorado Division of Fire Prevention & Control Driver Operator JPRs ( Edition) JPR # Task Initial Certification JPR Requirement: 8 Mandatory Renewal JPR Requirement: 100% of All JPRs (including all subsections)
Monitor Unit Calculations Part 2. Calculation of machine setting. Collimator setting
 Monitor Unit Calculations Part 2 George Starkschall, Ph.D. Department of Radiation Physics U.T. M.D. Anderson Cancer Center Calculation of machine setting reference dose machine setting =, reference dose
Monitor Unit Calculations Part 2 George Starkschall, Ph.D. Department of Radiation Physics U.T. M.D. Anderson Cancer Center Calculation of machine setting reference dose machine setting =, reference dose
CHAPTER IV FINITE ELEMENT ANALYSIS OF THE KNEE JOINT WITHOUT A MEDICAL IMPLANT
 39 CHAPTER IV FINITE ELEMENT ANALYSIS OF THE KNEE JOINT WITHOUT A MEDICAL IMPLANT 4.1 Modeling in Biomechanics The human body, apart of all its other functions is a mechanical mechanism and a structure,
39 CHAPTER IV FINITE ELEMENT ANALYSIS OF THE KNEE JOINT WITHOUT A MEDICAL IMPLANT 4.1 Modeling in Biomechanics The human body, apart of all its other functions is a mechanical mechanism and a structure,
MEASURING INSTRUCTIONS Step-by-Step. Lazy-L Pools. Step #1: Measure the Width (A) and the Length (B)
 l i ner MEASURING INSTRUCTIONS Step-by-Step Lazy-L Pools Step #1: Measure the Width (A) and the Length (B) Figure 1 Referring to the illustration of your Lazy-L pool (Figure 1), be sure that the width
l i ner MEASURING INSTRUCTIONS Step-by-Step Lazy-L Pools Step #1: Measure the Width (A) and the Length (B) Figure 1 Referring to the illustration of your Lazy-L pool (Figure 1), be sure that the width
Rotation Centers of the Equine Digit and their Use in Quantifying Conformation
 Presented at the Roth Kinematics Symposium, Stanford University, June 21, 2003. Rotation Centers of the Equine Digit and their Use in Quantifying Conformation John J. Craig, Phd ; Monique F. Craig, BSCE;
Presented at the Roth Kinematics Symposium, Stanford University, June 21, 2003. Rotation Centers of the Equine Digit and their Use in Quantifying Conformation John J. Craig, Phd ; Monique F. Craig, BSCE;
The Fundamentals of Putting
 The Fundamentals of Putting Episode 2 Putter Face and Path Direction The putter face angle at impact and the swing path direction at impact are the critical factors which determine the initial direction
The Fundamentals of Putting Episode 2 Putter Face and Path Direction The putter face angle at impact and the swing path direction at impact are the critical factors which determine the initial direction
O P E R ATING INSTRUCTIONS FOR MODEL SPR-45 Automatic Screen and Stencil Printer
 O P E R ATING INSTRUCTIONS FOR MODEL SPR-45 Automatic Screen and Stencil Printer TABLE OF CONTENTS I. SPECIFICATIONS...3. II. SAFETY INSTRUCTIONS...4. III. INSTALLATION...5. IV. SET-UP...6. V. SYSTEM OPERATION...9.
O P E R ATING INSTRUCTIONS FOR MODEL SPR-45 Automatic Screen and Stencil Printer TABLE OF CONTENTS I. SPECIFICATIONS...3. II. SAFETY INSTRUCTIONS...4. III. INSTALLATION...5. IV. SET-UP...6. V. SYSTEM OPERATION...9.
Please read carefully!
 Vertical Suits - How to Measure document. Please read carefully! Important points: Always get measured by another person Always wear the clothing that you will be wearing under your suit when taking the
Vertical Suits - How to Measure document. Please read carefully! Important points: Always get measured by another person Always wear the clothing that you will be wearing under your suit when taking the
BEGINNING PITCHING TIPS BRYC Softball Updated February 4, 2008
 BEGINNING PITCHING TIPS BRYC Softball Updated February 4, 2008 General 1. Work on sound mechanics before anything else. The earlier a player learns the mechanics, the quicker she will progress in learning
BEGINNING PITCHING TIPS BRYC Softball Updated February 4, 2008 General 1. Work on sound mechanics before anything else. The earlier a player learns the mechanics, the quicker she will progress in learning
APPENDIX C SKI DRILL. followed as in FM 157
 APPENDIX C SKI DRILL Section I. INDIVIDUAL DRILL C-1. General Ski drill and ski training should be given concurrently. Ski drill is kept to the minimum necessary for assembly, organization, instruction,
APPENDIX C SKI DRILL Section I. INDIVIDUAL DRILL C-1. General Ski drill and ski training should be given concurrently. Ski drill is kept to the minimum necessary for assembly, organization, instruction,
Design of a double quadruped for the Tech United soccer robot
 Design of a double quadruped for the Tech United soccer robot M.J. Naber (0571509) DCT report number: 2009.134 Master Open Space project Eindhoven, 21 December 2009 Supervisor dr.ir. P.C.J.N. Rosielle
Design of a double quadruped for the Tech United soccer robot M.J. Naber (0571509) DCT report number: 2009.134 Master Open Space project Eindhoven, 21 December 2009 Supervisor dr.ir. P.C.J.N. Rosielle
1. Bridge 2. Frontal straps (RFS / LFS) 3. Thick sponge padding 4. Occipital mesh 5. Scaled rubber strap 6. Suspension arm 7. Adaptor A 8.
 1. Bridge 2. Frontal straps (RFS / LFS) 3. Thick sponge padding 4. Occipital mesh 5. Scaled rubber strap 6. Suspension arm 7. Adaptor A 8. Adaptor B 9. Adaptor C 10. Extender 11. Metallic tube with protector
1. Bridge 2. Frontal straps (RFS / LFS) 3. Thick sponge padding 4. Occipital mesh 5. Scaled rubber strap 6. Suspension arm 7. Adaptor A 8. Adaptor B 9. Adaptor C 10. Extender 11. Metallic tube with protector
Revisions to the Regulations for Agility Trials
 Revisions to the Regulations for Agility Trials Effective January 2, 2018 Equipment changes may be done prior to January 2, 2018, but must be completed by January 2, 2018 This insert is issued as a supplement
Revisions to the Regulations for Agility Trials Effective January 2, 2018 Equipment changes may be done prior to January 2, 2018, but must be completed by January 2, 2018 This insert is issued as a supplement
SURFACE CASING SELECTION FOR COLLAPSE, BURST AND AXIAL DESIGN FACTOR LOADS EXERCISE
 SURFACE CASING SELECTION FOR COLLAPSE, BURST AND AXIAL DESIGN FACTOR LOADS EXERCISE Instructions Use the example well data from this document or the powerpoint notes handout to complete the following graphs.
SURFACE CASING SELECTION FOR COLLAPSE, BURST AND AXIAL DESIGN FACTOR LOADS EXERCISE Instructions Use the example well data from this document or the powerpoint notes handout to complete the following graphs.
Structural Design of Tank Weighing Systems
 Structural Design of Tank Weighing Systems 1. Initial observations Some essential rules must be followed when installing load cells in tanks. For example, tanks are frequently subject to weather conditions
Structural Design of Tank Weighing Systems 1. Initial observations Some essential rules must be followed when installing load cells in tanks. For example, tanks are frequently subject to weather conditions
AIRMOUNT VIBRATION ISOLATION
 MOUNT VIBRATION ISOLATION SELECTION AND ISOLATION FORMULA Refer to the selection guide on page 33 for Airmount load and isolation capabilities. Follow this procedure: 1. LOAD CAPACITY Select one or two
MOUNT VIBRATION ISOLATION SELECTION AND ISOLATION FORMULA Refer to the selection guide on page 33 for Airmount load and isolation capabilities. Follow this procedure: 1. LOAD CAPACITY Select one or two
2990 Lorne Scots Royal Canadian Army Cadet Corps Rifle Drill
 2990 Lorne Scots Royal Canadian Army Cadet Corps Rifle Drill Page 1 of 27 TABLE OF CONTENTS PARA ITEM PAGE Section 1 BASIC RIFLE DRILL 1.1 INTRODUCTION 3 1.2 ATTENTION 5 1.3 STAND AT EASE FROM ATTENTION
2990 Lorne Scots Royal Canadian Army Cadet Corps Rifle Drill Page 1 of 27 TABLE OF CONTENTS PARA ITEM PAGE Section 1 BASIC RIFLE DRILL 1.1 INTRODUCTION 3 1.2 ATTENTION 5 1.3 STAND AT EASE FROM ATTENTION
The first thing a jumper must learn is jump vertically off the ground as high as possible.
 HIGH JUMP 2010 The objective of the high jump is to clear a crossbar placed as high as possible by jumping off one foot and landing on the opposite side of the crossbar without dislodging it. The first
HIGH JUMP 2010 The objective of the high jump is to clear a crossbar placed as high as possible by jumping off one foot and landing on the opposite side of the crossbar without dislodging it. The first
Projectile Motion INTRODUCTION. Time-of-flight vs. Initial Velocity. Projectile Motion
 INTRODUCTION In this lab you will study the motion of a freely-falling projectile, namely a small plastic sphere. Projectile motion, for our purposes, is the motion of an object that has been launched
INTRODUCTION In this lab you will study the motion of a freely-falling projectile, namely a small plastic sphere. Projectile motion, for our purposes, is the motion of an object that has been launched
Body Stabilization of PDW toward Humanoid Walking
 Body Stabilization of PDW toward Humanoid Walking Masaki Haruna, Masaki Ogino, Koh Hosoda, Minoru Asada Dept. of Adaptive Machine Systems, Osaka University, Suita, Osaka, 565-0871, Japan ABSTRACT Passive
Body Stabilization of PDW toward Humanoid Walking Masaki Haruna, Masaki Ogino, Koh Hosoda, Minoru Asada Dept. of Adaptive Machine Systems, Osaka University, Suita, Osaka, 565-0871, Japan ABSTRACT Passive
OPERATING MANUAL DOUBLE ACTING DRILLING INTENSIFIER HYDRAULIC TYPE
 Page 1 of 8 OPERATING MANUAL DOUBLE ACTING DRILLING INTENSIFIER HYDRAULIC TYPE Size Series 6.50" 478 Reviewed And Approved By: Signature: Initials: Date: Page 2 of 8 Section OPERATING MANUAL DOUBLE ACTING
Page 1 of 8 OPERATING MANUAL DOUBLE ACTING DRILLING INTENSIFIER HYDRAULIC TYPE Size Series 6.50" 478 Reviewed And Approved By: Signature: Initials: Date: Page 2 of 8 Section OPERATING MANUAL DOUBLE ACTING
ATT-59, Part I. ATT-59/99, SMOOTHNESS OF PAVEMENTS Part I, Manual Profilograph. b) Determining the Profile Index from profilograms
 ATT-59, Part I ATT-59/99, SMOOTHNESS OF PAVEMENTS Part I, Manual Profilograph 1.0 SCOPE This method describes the procedures for: a) Operating the profilograph. b) Determining the Profile Index from profilograms
ATT-59, Part I ATT-59/99, SMOOTHNESS OF PAVEMENTS Part I, Manual Profilograph 1.0 SCOPE This method describes the procedures for: a) Operating the profilograph. b) Determining the Profile Index from profilograms
Appendix 3: SPCM Scoring Form SEATED POSTURAL CONTROL MEASURE January 1994
 Appendix 3: SPCM Scoring Form SEATED POSTURAL CONTROL MEASURE January 1994 SUNNY HILL HEALTH CENTRE FOR CHILDREN 3644 Slocan Street, Vancouver, B.C. V5M 3E8 Yr Mo Day Score Min Max. Name Date of Assessment
Appendix 3: SPCM Scoring Form SEATED POSTURAL CONTROL MEASURE January 1994 SUNNY HILL HEALTH CENTRE FOR CHILDREN 3644 Slocan Street, Vancouver, B.C. V5M 3E8 Yr Mo Day Score Min Max. Name Date of Assessment
Sprocket Selection Guidelines
 Sprocket Selection Guidelines Table 1 Information Necessary to Order Sprockets 1. Chain Size Number, type, or drawing number of the chain to be used on the sprocket. (The suitability of a sprocket depends
Sprocket Selection Guidelines Table 1 Information Necessary to Order Sprockets 1. Chain Size Number, type, or drawing number of the chain to be used on the sprocket. (The suitability of a sprocket depends
FIELD EVENTS DIAGRAMS
 FIELD EVENTS DIAGRAMS Landing System Approach HIGH JUMP The declination in the high jump approach shall not exceed 1:100 (1%). The approach shall consist of a semicircle or rectangle of unvarying surface.
FIELD EVENTS DIAGRAMS Landing System Approach HIGH JUMP The declination in the high jump approach shall not exceed 1:100 (1%). The approach shall consist of a semicircle or rectangle of unvarying surface.
THE development of more advanced techniques in radiotherapy,
 1 A Geant4-based simulation of an accelerator s head used for Intensity Modulated Radiation Therapy F. Foppiano, B. Mascialino, M.G. Pia, M. Piergentili. Abstract We present a Geant4-based simulation,
1 A Geant4-based simulation of an accelerator s head used for Intensity Modulated Radiation Therapy F. Foppiano, B. Mascialino, M.G. Pia, M. Piergentili. Abstract We present a Geant4-based simulation,
WALKING AIDS AND GAIT TRAINING
 WALKING AIDS AND GAIT TRAINING By:Dr. Chaman Lal B.S.PT, DPT, Dip. in sports Injuries, MPPS(PAK), PG in Clinical Electroneurophysiology (AKUH), Registered.EEGT (USA), Member of ABRET, AANEM & ASET (USA).
WALKING AIDS AND GAIT TRAINING By:Dr. Chaman Lal B.S.PT, DPT, Dip. in sports Injuries, MPPS(PAK), PG in Clinical Electroneurophysiology (AKUH), Registered.EEGT (USA), Member of ABRET, AANEM & ASET (USA).
Guidelines for Using the UMTRI ATD Positioning Procedure for ATD and Seat Positioning (Version V)
 Procedure for ATD and Seat Positioning (Version V) December 2004 Insurance Institute for Highway Safety Procedure for ATD and Seat Positioning (Version V) Introduction These guidelines provide a simplified
Procedure for ATD and Seat Positioning (Version V) December 2004 Insurance Institute for Highway Safety Procedure for ATD and Seat Positioning (Version V) Introduction These guidelines provide a simplified
Shoulder Exercises for Combined Labrum Repair Rehabilitation Protocol
 Shoulder Exercises for Combined Labrum Repair Rehabilitation Protocol The exercises illustrated and described in this document should be performed only after instruction by your physical therapist or Dr.
Shoulder Exercises for Combined Labrum Repair Rehabilitation Protocol The exercises illustrated and described in this document should be performed only after instruction by your physical therapist or Dr.
Exposure System Selection
 Principles of Imaging Science II (RAD120) Exposure Systems Exposure System Selection Radiographic exposure is a very complex process Best technique systems manipulate one variable while holding others
Principles of Imaging Science II (RAD120) Exposure Systems Exposure System Selection Radiographic exposure is a very complex process Best technique systems manipulate one variable while holding others
EXPERIMENTAL RESULTS OF GUIDED WAVE TRAVEL TIME TOMOGRAPHY
 18 th World Conference on Non destructive Testing, 16-20 April 2012, Durban, South Africa EXPERIMENTAL RESULTS OF GUIDED WAVE TRAVEL TIME TOMOGRAPHY Arno VOLKER 1 and Hendrik VOS 1 TNO, Stieltjesweg 1,
18 th World Conference on Non destructive Testing, 16-20 April 2012, Durban, South Africa EXPERIMENTAL RESULTS OF GUIDED WAVE TRAVEL TIME TOMOGRAPHY Arno VOLKER 1 and Hendrik VOS 1 TNO, Stieltjesweg 1,
Monitor Unit Verification for Small Fields
 Monitor Unit Verification for Small Fields Patrick Higgins, Ph.D University of Minnesota Department of Radiation Oncology October 10, 2013 The Issues: How do we verify the monitor units calculated by the
Monitor Unit Verification for Small Fields Patrick Higgins, Ph.D University of Minnesota Department of Radiation Oncology October 10, 2013 The Issues: How do we verify the monitor units calculated by the
Electronic Oncology Systems the Management and the Safety Measures. Hansen Chen, Director, TDSI
 Electronic Oncology Systems the Management and the Safety Measures Hansen Chen, Director, TDSI Radiation Oncology Department People Place Equipments Procedures Patients Hansen Chen 2 Radiation Oncology
Electronic Oncology Systems the Management and the Safety Measures Hansen Chen, Director, TDSI Radiation Oncology Department People Place Equipments Procedures Patients Hansen Chen 2 Radiation Oncology
