Blood gas analysis: effect of air bubbles in syringe and delay in estimation
|
|
|
- Bryan Taylor
- 6 years ago
- Views:
Transcription
1 BRTSH MEDCAL JOURNAL VOLUME MARCH CLNCAL RESEARCH Blood gas analysis: effect of air bubbles in syringe and delay in estimation C K BSWAS, J M RAMOS, B AGROYANNS, D N S KERR Abstract Two common sources of error in blood ph and blood gas analysis were studied. The effect of delay in estimation was studied in 10 volunteers and 40 patients. Syringes were stored at 0 C, (crushed ice), 4 C (refrigerator) and 22 C (room temperature). The pressure of oxygen (Po2) fell significantly by 20 minutes at 4 C and 22 C but did not change significantly at 0 C for up to 30 minutes. Blood ph, pressure of carbon dioxide (Pco,), bicarbonate, total carbon dioxide (Tco2), and base excess did not change significantly for up to 30 minutes at 4 C and 22 C and up to 60 minutes at 0 C. The effect of air bubbles in the syringe was studied by leaving a single bubble or froth in contact with the blood for one to five minutes in 40 patients. Po2 rose significantly after two minutes' contact with froth and two minutes' contact with the air bubble, and Pco2 fell significantly after three minutes' contact with the air bubble. Size of the bubble had little effect on rates of change. Blood ph, bicarbonate, Tco2, and base excess did not change significantly after up to five minutes' contact. For accurate estimation of Po, and Pco2 it is necessary to avoid frothing, to expel all air bubbles within two minutes, and to inject the sample into the machine within 10 minutes or store the syringe in crushed ice. The requirements for blood ph and base excess measurement are less exacting. ntroduction Determination of blood gases is essential in critically ill patients. Critical illness is not confined to "normal laboratory working University Department of Medicine, Royal Victoria nfirmary, Newcastle upon Tyne NE1 4LP C K BSWAS, MB, MRCP, regional research registrar J M RAMOS, MD, honorary research fellow B AGROYANNS, MD, honorary research fellow D N S KERR, MS, FRCP, professor of medicine hours," so that most samples must be handled by the emergency service. deally, all areas of the hospital which manage seriously ill patients should be equipped with automatic blood gas analysis equipment regularly maintained by technical staff, and all junior staff should be trained in its use.' Since such machines cost over to buy and several thousand pounds a year to maintain, however, probably many samples in British hospitals will be dealt with by central laboratories using services operated by medical laboratory scientific officers. Samples are drawn by junior staff and must be transported to the laboratory, where they may await the attention of the medical laboratory scientific officer engaged in other duties. nstructions to medical staff on handling samples include: "avoid drawing air into the syringe," "expel any air bubbles as quickly as possible," and "transport the syringe in crushed ice if any delay is anticipated." Little quantitative information is usually provided on the importance of these sources of error or the limits beyond which samples become unacceptable. We tested the beliefs of junior medical staff about the importance of these precautions by administering a questionnaire to 10 doctors in three large hospitals in Newcastle who had qualified from 10 different British medical schools. Their estimate of the safe storage time at room temperature varied from five to 60 minutes, two being happy to leave the sample for one hour; six expected little or no improvement in storage time from the use of crushed ice. Nine were well aware of the importance of expelling air bubbles but five had an exaggerated impression of the importance of this source of error. Much information is already available on the errors resulting from storing blood at different temperatures,2 adding air to shed blood,3 and adding anticoagulants.4 None of the papers giving reassuring results discusses the reproducibility of the measurement or the "type 2 error"-that is, the chance that a significant change in the blood ph or blood gases could have been obscured by laboratory error. We therefore re-examined the question using an accurate ph meter, the Corning 168 blood gas analyser. Patients and methods Blood gases were measured in samples of venous blood taken from 70 hospital patients. A Venflon needle was inserted into the median cubital vein in the forearm to facilitate anaerobic collection of the
2 924 serial blood samples. Syringe dead space was filled with heparin solution (Pularin, heparin injection BP 1000 U/ml, Duncan Flockhart and Co Ltd) 1000 units/ml. The quantity of heparin was estimated by weighing 10 syringes empty and then filling the dead space. For a 2 ml syringe 44 ± 19 U of heparin was needed to fill the dead space, whereas 72 ± 15 U was needed for a 5 ml syringe. The dilution effect of this heparin was about 2% for the 2 ml syringe and less than 1 % for the 5 ml syringe, well below the level at which dilution produces a measurable effect on pressure of carbon dioxide (PcoQ), pressure of oxygen (Po2), or blood ph4 Blood samples with a higher Po2 were drawn from 10 patients in renal failure undergoing haemodialysis. The blood samples were drawn from the arterial line during haemodialysis and were therefore derived from the arteriovenous fistula. A further 10 samples of arterialised venous blood were drawn from the back of the hand of healthy volunteers (staff from the department of medicine) after the hands had been warmed at 43 C to produce maximum vasodilatation. The heparinised samples were injected into the Corning analyser and blood analysed for ph by a glass ph electrode with a flat membrane, a dialysis reference membrane, a 4M KC1 bridge, and an Ag/AgCl reference electrode regulated by temperature; for Po2 by an electrode, comprising a glass-platinum cathode, an Ag/AgCl anode, an electrolyte filling solution, and an oxygen-permeable membrane; and for Pco2 by an electrode consisting of a glass ph electrode separated from the blood sample by a spacer saturated with electrolyte filling solution and a membrane permeable to gaseous CO2. All measurements were performed at 37 C. True CO2 and Po2 were calculated from a calibration graph derived TABLE -Effect of storage at 0, 40, and 22 C for five minutes compared with 10, 20, and 30 minutes. Results are means ±SE Time (min) Po2 (kpa) p Value Pco0 (kpa) p Value Storage at 0'C ± ± ± ± ± ± ± ±0-14 Storage at 4'C ± ± ± ± ±0-14 p< ± ±0 20 p< ±0-14 Storage at 22'C ± ± ± ± ±0-20 < ± ±0 38 < ±0-16 Conversion: S to traditional units-po2 and Pco2: 1 kpa 7-5 mm Hg. BRTSH MEDCAL JOURNAL VOLUME MARCH 1982 venous blood was analysed at five minutes, one hour, and two hours on samples stored in crushed ice and ice water only. n the third experiment arterialised blood from 10 patients undergoing haemodialysis was drawn from the arterial line of the dialysis circuit and stored at room temperature or at 0 C for up to one hour. For the fourth experiment venous blood was arterialised by warming the hands of volunteers at 43 C for at least 10 minutes; samples were studied at 0'C and at room temperature for up to 30 minutes. Effect of single air bubble in syringe-to simulate the worst conditions likely to be encountered, we introduced 1 ml of air into a syringe and then drew a further 1 ml of blood. This was done with five different syringes in rapid succession. The air bubbles were kept in contact with blood for one, two, three, four, and five minutes before being expelled. To simulate the conditions more likely to be encountered in clinical practice, we repeated this experiment but introduced only 0 1, 0-2, or 0-5 ml of air and then drew blood up to the 2 ml mark. These air bubbles represented 5%, 10%, and 25% of the total volume of the syringe. Each experiment was carried out on 10 patients. Care was taken not to produce froth by shaking the syringe. Blood gases and ph after one, two, three, four, and five minutes' exposure to air were compared with the results in blood not exposed to air. Effect offroth in syringe-a bad fit between the nozzle of the syringe and hub of the needle or a crack in either syringe or needle may result in a stream of fine air bubbles entering the blood sample. To simulate this we drew 0 1 ml of air into a 2 ml syringe, shook it vigorously, and measured blood gas and ph after two minutes; the results were contrasted with those obtained in the same blood sample not exposed to air. Statistics-Student's paired t test was used to compare the mean value after five minutes' storage with those after 10, 20, 30, 60, and 120 minutes' storage. The same test was used to compare the results in blood drawn anaerobically with those in blood-mixed with air for one, two, three, four, and five minutes. Results REPRODUCBLTY Analysis of data from 10 normal people showed that intra-assay error was negligible for all variables tested. The machine error (SD) calculated for a single observation for ph was unit, for Po2 was 0-02 kpa (0-15 mm Hg), and for PCO2 was kpa (0-21 mm Hg). The total errors for the same variables were unit, kpa (0 44 mm Hg), and kpa (1 65 mm Hg). This total error contained a negligible component of machine error in the case of blood gases; it may be regarded effectively as the syringe error. TABLE i-effects of storage at 0 C for five minutes compared with 60 and 120 minutes. Results are means + SE Time (min) Po, (kpa) p Value Pco, (kpa) p Value ph p Value Bicarbonate p Value ± ± ± ± ±0-28 < ± ± ± ±0-26 < ±0-25 < ±0-006 < ±1-37 <0-01 Conversion: S to traditional units-po2 and Pco,: 1 kpa 7-5 mm Hg. from the data of Kelman and Nunn.5 Plasma bicarbonate, total CO2 and base excess were calculated from the results according to the nomogram of Siggaard-Andersen.6 Reproducibility of method-two 5 ml samples were drawn in rapid succession and the syringes immediately placed in crushed ice. Measurement was carried out 15 minutes later when the blood samples were fully cooled, at which time our studies (see below), showed that a few minutes' storage had an insignificant effect on blood ph and blood gases. Analysis was carried out twice from each syringe. The machine error was calculated by comparing the results from a single syringe and the total error by comparing the results from two separate syringes. Effects of temperature and storage-venous or arterialised samples were drawn in heparinised 5 ml syringes. These were stored either at room temperature (22'C), in a refrigerator at 4'C, or in crushed ice and ice water at 0'C. n the first experiment, on 20 patients, venous blood gas analysis was carried out after five, 10, 20, and 30 minutes' storage by each method. n a second experiment, on 10 patients, EFFECT OF STORAGE There was no significant change in the mean value of ph, bicarbonate, total CO,, base excess, or PCO2 when venous blood was stored for up to 30 minutes at any of the three temperatures. Blood ph remained constant at 7-41 ±003 at 0 C and 4'C and at 7A40±0 03 at 22 C. Table shows the results for Pco2; there was the expected upward trend at all three temperatures but it did not achieve significance. Measurable changes did occur with longer storage; they became significant, though very slight, after 120 minutes at 0 C for ph, bicarbonate, and Pco2 (table ). The greatest changes were seen in Po2. At room temperature Po2 fell steadily and the change was highly significant from 20 minutes onwards (table ). There was a similar but much smaller change when syringes were stored in the refrigerator at 4 C (table ). When the syringe was stored in crushed ice there was no significant change at up to 30 minutes but a significant fall from 60 minutes onwards (table ).
3 BRTSH MEDCAL JOURNAL VOLUME MARCH 1982 We calculated the maximum error that our experiments were likely to have concealed. From the consistency of the results in our preliminary experiments we concluded that there was a less than 5%, chance that storage in crushed ice for 30 minutes introduces an error in Po2 measurement greater than 1 2 kpa (9 mm Hg) or that storage in crushed ice for 60 minutes introduces errors exceeding 0-5 kpa (3-7 mm Hg) for Pco2 and 0 02 units for ph. When blood with a higher Po2 was used the results were similar. At room temperature there was no significant fall in Po2 during the first 10 minutes but the rate of fall thereafter was greater than in venous blood (figs 1 and 2). When the syringe was stored in crushed ice there was no significant fall in Po2 at up to 30 minutes (figs 3 and 4) but TABLE -Changes in Po2 and Pco2 at one, two, three, four, and five minutes after adding 01 ml air compared with 0 minute without air. Results are means Time (min) Po2 (kpa) p Value Pco0 (kpa) p Value ± ± ± ± ±0 30 < ± ±0-32 < ±0 54 < ±0 35 < ±0-52 < ±0-36 < ±0-51 <00005 Conversion: S to traditional units-po, and Pco,: lkpa 7-5 mm Hg P02 (kpa) 10 <u.ul p<0-00 9, 8 O 0 Fig P02 (kpa) Fig * * = ===oft & K_ Fig. 3 Minutes Fig.4 Minutes FG 1-Changes in Po2 when arterialised blood from arteriovenous fistulas of patients with renal failure was stored at 22 C. FG 2-Changes in P02 when arterialised venous blood from warmed hands of normal subjects was stored at 22'C. FG 3-Changes in P02 when arterialised blood from arteriovenous fistulae of patients with renal failure was stored at 0'C. FG 4-Changes in Po2 when arterialised venous blood from warmed hands of normal subjects was stored at 0'C. ndividual results from 10 subjects in each case. Conversion: S to traditional units-po2: lkpa 7-5 mm Hg there was a significant fall between 30 and 60 minutes (fig 3). There was no significant change in Pco2 or ph at up to 30 minutes either at 0 C or at room temperature. EFFECT OF AR BUBBLE There was no significant change in blood ph after five minutes' exposure to air bubbles varying from 5% to 50% of the volume of the syringe. Significant changes occurred in Po2 after two minutes and in Pco2 after three minutes' contact with the air (tables, V, and V). Though the changes after one minute were not significant they followed the same trends as those observed later, suggesting that alterations in these two variables occur within one minute. Figure 5 shows the different sizes of bubbles used; there was surprisingly little difference in the rate of change of Po2 and Pco2 with bubble size. EFFECT OF FROTH There was a substantial change in Pco2 and PO2 within two minutes when blood was exposed to froth (fig 6). Discussion Placing a syringe in the refrigerator at 4 C is clearly not an adequate substitute for placing it in crushed ice. Storage at any temperature above 0 C results in a fall in Po' due to respiration by blood cells, particularly white cells and reticulocytes.7 There are corresponding changes in PCO2 and bicarbonate but these are proportionately smaller because of blood buffering. As would be expected, cooling the blood slows the rate of cell metabolism considerably. Placing the container in a refrigerator surrounded only by air is less effective than immersing it in crushed ice. f the rate of oxidation by blood cells is independent of Po2 the oxygen consumption per volume per minute should be the same in venous and arterial blood. This would be expected to cause a steeper fall in Po2 with arterial blood than with venous blood because of the shape of the oxygen dissociation curve. Since most of our experiments were performed with venous blood, we repeated the storage studies with blood of high Po2 taken from the arteriovenous fistulas of patients with renal failure and from normal subjects with maximally dilated hand veins. The fall in Po2 was indeed steeper but the difference was
4 926 TABLE V-Changes in Po2 and Pco2 one, two, three, four, and five minutes after adding 0-2 ml air compared with 0 minute without air. Results are means Time (min) Po, (kpa) p Value Pco, (kpa) p Value ± ± ± ± ±0-41 < ± ±0-38 < ±0-44 < ±0-36 < ±0-46 < ±0 34 < ±0 44 < Conversion: S to traditional units-po, and Pco,: 1 kpa mm Hg. TABLE v-changes in Po2 and Pco2 one, two, three, four, and five minutes after adding 0-5 ml air compared with 0 minute without air. Results are means Time (min) Po, (kpa) p Value Pco2 (kpa) p Value ± ± ± ± ±0 24 p< ± ±0-22 < ±0-44 < ±0-18 < ±0-45 < ±0-26 < ±047 < Conversion: S to traditional units-po, and Pco,: 1 kpa 7-5 mm Hg. BRTSH MEDCAL JOURNAL VOLUME MARCH 1982 carried out under conditions likely to produce a maximum error: contact between venous blood of low Po2 and high Pco2 in a large air bubble. The error introduced in practice will often be smaller. t is usually possible to draw an arterial blood sample and expel any trapped air bubbles within two minutes, and provided that this is done the sample will be acceptable for blood gas analysis. 5 50* 5* Po2 (kpa) 4 00' 3* Minutes FG 6-Change in Po2 of venous blood after adding 0 1 ml air to 2 ml blood in syringe and shaking vigorously. (Mean ± SD and individual results in 10 patients. Conversion: S to traditional units-po2:lkpa 7-5 mm Hg. The effect of leaving air bubbles in the syringe for longer was studied by Madiedo and colleagues.8 They showed that the continued presence of an air bubble occupying 10% of the blood volume caused a significant rise of Po, within 20 minutes. Our study suggests that some significant change occurs within two minutes. We see no reason to allow air bubbles to remain in the syringe after it is disconnected from the patient, so that this source of error should not arise. Even a modest amount of froth in the syringe gave rise to a substantial error within two minutes, suggesting that any syringe with visible' froth should be regarded as unsuitable for measuring blood Po0, though it remains suitable for measuring blood ph, Pco2, and bicarbonate on the rare occasion when these are required in isolation. not as great as might be expected from theoretical calculations, and the precautions that need to be taken when handling blood of normal or reduced Po, are similar. The rise in Po2 and fall in Pco, when an air bubble is introduced into the syringe represent diffusion of oxygen across the fluid-air barrier. Our studies suggest that when a single air bubble is present in the syringe the rate of this process is not critically dependent on the size of the air bubble-a rather surprising finding, which we cannot explain. A significant change in Po2 was observed after two minutes and in Pco2 after three minutes, but there was a trend in the same direction at one minute. We calculate that there is a less than 5% chance that,the change caused by one minute's contact with a large air bubble will be greater than 0 45 kpa (3 4 mm Hg) for P02 and 0-18 kpa (1-4 mm Hg) for Pco0. Our studies were RECOMMENDATO A stop-watch or watch with a single hand should be available when blood is drawn for blood gas analysis, so that the clinician can check that any trapped air has been expelled within two minutes and can record the storage time before blood is injected into the ph meter. Samples containing froth should be discarded. f medical staff have direct access to a machine and can be sure of injecting the blood within 10 minutes it is acceptable to transport the sample at room temperature. f there is a technician-operated service or there is any other reason to expect delay syringes- should be stored in crushed ice between bloodletting and injection into the machine. Under these conditions the sample is adequate for all purposes for up to 30 minutes. On the rare occasions when the clinician is concerned only with blood ph and bicarbonate and does not require an immediate reply for management of the patient it is acceptable to store blood at room temperature for up to 30 minutes or in crushed ice for up to 60 minutes, and errors are minimal in samples stored in ice for up to 120 minutes.
5 BRTSH MEDCAL JOURNAL VOLUME MARCH References Minty BD, Nunn JF. Regional quality control survey of blood gas analysis. Ann Clin Biochem 1977;14: Siggaard-Andersen 0. Sampling and storing of blood for determination of acid base status. Scandj Clin Lab nvest 1961 ;13: shikawa S, Fornier A, Borst C, Segal MS. The effect of air bubbles and time delay on blood gas analysis. Ann Allergy 1974;33: Bradley JG. Errors in the measurement of blood Pco2 due to dilution of the sample with heparin solution. BrJ_ Anaesth 1972;44: Kelman GR, Nunn JF. Nomograms for correction of blood Po2, Pco2 ph and base excess for time and temperature. J Appl Physiol 1966;21: Siggaard-Andersen 0. Titratable acid or base of body fluids. Ann NY Acad Sci 1966;133: Adams AP, Morgan-Hughes JO, Sykes MK. ph and blood-gas analysis. Anaesthesia 1967;22: Madiedo G, Sciacca R, Hause L. Air bubbles and temperature effect on blood gas analysis. J Clin Pathol 1980;33 : (Accepted 23 December 1981) ntravenous naloxone in acute respiratory failure JON AYRES, JOHN REES, TAK LEE, G M COCHRANE Abstract A 58-year-old man presented with acute on chronic respiratory failure. n the acute stage of his illness an infusion of the opiate antagonist naloxone caused an improvement in oxygen saturation as measured by ear oximetry from 74% to 85%, while a saline infusion resulted in a return of oxygen saturation to the original value. When he had recovered from the acute episode the same dose of naloxone had no effect on oxygen saturation. These findings suggest that in acute respiratory failure there may be overproduction of, or increased sensitivity to, endorphins. ntroduction Naloxone restores the ventilatory response to added inspiratory loads in some patients with chronic stable airflow obstruction.' We report on a patient with acute on chronic respiratory failure in whom naloxone improved both oxygen saturation and tidal ventilation, suggesting that endorphins play a part in acute respiratory failure. Case history n 1968 a 46-year-old man presented with recurrent supraventricular tachycardias and was found to have a paralysed right hemidiaphragm, which recovered spontaneously over the subsequent three months. n 1975 he complained of daytime somnolence, which worsened over the next five years, by which time breathlessness limited his exercise tolerance to 50 yards and he was thus admitted to hospital with a respiratory tract infection. He was wheezy and in right heart failure, and had paradoxical movement of the abdominal wall on inspiration. Proximal muscles were weak in his arms and legs. Chest radiography showed that the left hemidiaphragm was paralysed. Results of tests of respiratory function were: forced expiratory volume in one second (predicted ), forced vital capacity ( ), total lung capacity 6-61 ( ), and residual volume ( ). He required mechanical ventilation for one week, after which he was able to breathe spontaneously. Tests of his respiratory and skeletal Department of Thoracic Medicine, Guy's Hospital, London SE1 9RT JON AYRES, MB, MRCP, research registrar JOHN REES, MA, MRCP, senior registrar TAK LEE, MB, mrcp, registrar (present appointment: clinical lecturer, Cardiothoracic nstitute, Brompton Hospital, London SW3) G M COCHRANE, MB, MRCP, consultant muscles after ventilation showed: vital capacity (supine) ; vital capacity (erect) 215 1; maximal inspiratory pressure 19 kpa (19 cm H2O) (predicted > 6 9 kpa (70 cm H2O)); maximal expiratory pressure 7-8 kpa (80 cm H20) (predicted >13-7 kpa (140 cm H20)); and transdiaphragmatic pressure 0-3 kpa (3 cm H20) (predicted >2 5 kpa (25 cm H2O)). Electromyography showed evidence of a myopathy of the intercostal muscles. Creatinine phosphokinase concentration was normal. A polygraphic sleep study showed no nocturnal apnoea but periods of hypopnoea associated with falls in oxygen saturation from 75% to 34%. Crossed auditory evoked potentials were normal. A rocking bed improved his episodes of night-time desaturation. While he was being weaned off the ventilator a bolus of 0 4 mg naloxone intravenously caused an increase in respiratory rate and oxygen saturation (as measured by an ear oximeter). The ph rose from 7-42 to 7-43; oxygen pressure rose from 4-1 to 4 3 kpa (31 to 32 mm Hg); carbon dioxide pressure fell from 8-65 to 8 17 kpa (65 to 61 mm Hg); bicarbonate concentration fell from 36 to 35 mmol(meq)/l; and base excess fell from + 15 to + 14 mmol(meq)/l. A second bolus of 2 mg caused an increase in tidal volume and made him agitated and hot. No opiate drugs had been administered during his admission. nfusions of naloxone (0-2 mg/min) and of physiological saline were compared in a double-blind manner (figure). Five minutes after the / ! 20~ x Mean Naloxone Saline Naloxone Saline Time (minutes) Changes in minute ventilation and oxygen saturation with infusions of naloxone (0-2 mg/min) and saline. beginning of the naloxone infusion minute ventilation rose from a baseline value of /min to /min through an increase in tidal volume, oxygen saturation rising from 74% to 85% over 15 minutes. During saline infusion minute ventilation remained constant and oxygen saturation fell to 75%. When naloxone was restarted oxygen saturation rose to 85% while tidal volume and respiratory rate were unchanged. Minute ventilation fell towards the baseline value on reinfusion of saline. Regular treatment was started with subcutaneous naloxone (2 mg four times daily). A repeat study three weeks later, when he was well,
CHAPTER 3: The respiratory system
 CHAPTER 3: The respiratory system Practice questions - text book pages 56-58 1) When the inspiratory muscles contract, which one of the following statements is true? a. the size of the thoracic cavity
CHAPTER 3: The respiratory system Practice questions - text book pages 56-58 1) When the inspiratory muscles contract, which one of the following statements is true? a. the size of the thoracic cavity
EMERGENCY MEDICINE AND THE LABORATORY. Ehsan Bolvardi(MD)
 EMERGENCY MEDICINE AND THE LABORATORY Ehsan Bolvardi(MD) bolvardie@mums.ac.ir Objective ED and laboratory Inappropriate use of laboratory ABG sampling ABG sampling error Introduction The laboratory is
EMERGENCY MEDICINE AND THE LABORATORY Ehsan Bolvardi(MD) bolvardie@mums.ac.ir Objective ED and laboratory Inappropriate use of laboratory ABG sampling ABG sampling error Introduction The laboratory is
CHAPTER 3: The cardio-respiratory system
 : The cardio-respiratory system Exam style questions - text book pages 44-45 1) Describe the structures involved in gaseous exchange in the lungs and explain how gaseous exchange occurs within this tissue.
: The cardio-respiratory system Exam style questions - text book pages 44-45 1) Describe the structures involved in gaseous exchange in the lungs and explain how gaseous exchange occurs within this tissue.
RESPIRATORY REGULATION DURING EXERCISE
 RESPIRATORY REGULATION DURING EXERCISE Respiration Respiration delivery of oxygen to and removal of carbon dioxide from the tissue External respiration ventilation and exchange of gases in the lung Internal
RESPIRATORY REGULATION DURING EXERCISE Respiration Respiration delivery of oxygen to and removal of carbon dioxide from the tissue External respiration ventilation and exchange of gases in the lung Internal
 Question 1: Define vital capacity. What is its significance? Vital capacity is the maximum volume of air that can be exhaled after a maximum inspiration. It is about 3.5 4.5 litres in the human body. It
Question 1: Define vital capacity. What is its significance? Vital capacity is the maximum volume of air that can be exhaled after a maximum inspiration. It is about 3.5 4.5 litres in the human body. It
Lung Volumes and Capacities
 Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
Collin County Community College. Lung Physiology
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 9 Respiratory System 1 Lung Physiology Factors affecting Ventillation 1. Airway resistance Flow = Δ P / R Most resistance is encountered
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 9 Respiratory System 1 Lung Physiology Factors affecting Ventillation 1. Airway resistance Flow = Δ P / R Most resistance is encountered
Respiratory system & exercise. Dr. Rehab F Gwada
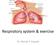 Respiratory system & exercise Dr. Rehab F Gwada Objectives of lecture Outline the major anatomical components & important functions of the respiratory system. Describe the mechanics of ventilation. List
Respiratory system & exercise Dr. Rehab F Gwada Objectives of lecture Outline the major anatomical components & important functions of the respiratory system. Describe the mechanics of ventilation. List
Respiratory physiology II.
 Respiratory physiology II. Learning objectives: 29. Pulmonary gas exchange. 30. Oxygen transport in the blood. 31. Carbon-dioxide transport in the blood. 1 Pulmonary gas exchange The transport mechanism
Respiratory physiology II. Learning objectives: 29. Pulmonary gas exchange. 30. Oxygen transport in the blood. 31. Carbon-dioxide transport in the blood. 1 Pulmonary gas exchange The transport mechanism
2. State the volume of air remaining in the lungs after a normal breathing.
 CLASS XI BIOLOGY Breathing And Exchange of Gases 1. Define vital capacity. What is its significance? Answer: Vital Capacity (VC): The maximum volume of air a person can breathe in after a forced expiration.
CLASS XI BIOLOGY Breathing And Exchange of Gases 1. Define vital capacity. What is its significance? Answer: Vital Capacity (VC): The maximum volume of air a person can breathe in after a forced expiration.
Recommendations for Standards. Monitoring. Cardiopulmonary Bypass
 Recommendations for Standards of Monitoring during Cardiopulmonary Bypass Membership of the working party (2006) Ian Curle Fiona Gibson Jonathan Hyde Alex Shipolini David Smith J P van Besouw Kate Wark
Recommendations for Standards of Monitoring during Cardiopulmonary Bypass Membership of the working party (2006) Ian Curle Fiona Gibson Jonathan Hyde Alex Shipolini David Smith J P van Besouw Kate Wark
The physiological functions of respiration and circulation. Mechanics. exercise 7. Respiratory Volumes. Objectives
 exercise 7 Respiratory System Mechanics Objectives 1. To explain how the respiratory and circulatory systems work together to enable gas exchange among the lungs, blood, and body tissues 2. To define respiration,
exercise 7 Respiratory System Mechanics Objectives 1. To explain how the respiratory and circulatory systems work together to enable gas exchange among the lungs, blood, and body tissues 2. To define respiration,
Respiratory System Study Guide, Chapter 16
 Part I. Clinical Applications Name: Respiratory System Study Guide, Chapter 16 Lab Day/Time: 1. A person with ketoacidosis may hyperventilate. Explain why this occurs, and explain why this hyperventilation
Part I. Clinical Applications Name: Respiratory System Study Guide, Chapter 16 Lab Day/Time: 1. A person with ketoacidosis may hyperventilate. Explain why this occurs, and explain why this hyperventilation
Respiration - Human 1
 Respiration - Human 1 At the end of the lectures on respiration you should be able to, 1. Describe events in the respiratory processes 2. Discuss the mechanism of lung ventilation in human 3. Discuss the
Respiration - Human 1 At the end of the lectures on respiration you should be able to, 1. Describe events in the respiratory processes 2. Discuss the mechanism of lung ventilation in human 3. Discuss the
Point-of-Care Testing: A Cardiovascular Perfusionist s Perspective
 Point-of-Care Testing: A Cardiovascular Perfusionist s Perspective Cory M. Alwardt, PhD, CCP Chief Perfusionist/ECMO Coordinator Assistant Professor of Surgery Mayo Clinic Hospital, Phoenix alwardt.cory@mayo.edu
Point-of-Care Testing: A Cardiovascular Perfusionist s Perspective Cory M. Alwardt, PhD, CCP Chief Perfusionist/ECMO Coordinator Assistant Professor of Surgery Mayo Clinic Hospital, Phoenix alwardt.cory@mayo.edu
CARBON DIOXIDE ELIMINATION FROM SEMICLOSED SYSTEMS
 Brit. J. Anaesth. (1956), 28, 196 CARBON DIOXIDE ELIMINATION FROM SEMICLOSED SYSTEMS BY RUSSELL M. DAVIES, I. R. VERNER Queen Victoria Hospital, East Grinstead AND A. BRACKEN Research and Development Centre,
Brit. J. Anaesth. (1956), 28, 196 CARBON DIOXIDE ELIMINATION FROM SEMICLOSED SYSTEMS BY RUSSELL M. DAVIES, I. R. VERNER Queen Victoria Hospital, East Grinstead AND A. BRACKEN Research and Development Centre,
Introduction. Respiration. Chapter 10. Objectives. Objectives. The Respiratory System
 Introduction Respiration Chapter 10 The Respiratory System Provides a means of gas exchange between the environment and the body Plays a role in the regulation of acidbase balance during exercise Objectives
Introduction Respiration Chapter 10 The Respiratory System Provides a means of gas exchange between the environment and the body Plays a role in the regulation of acidbase balance during exercise Objectives
Gases and Respiration. Respiration Overview I
 Respiration Overview I Respiration Overview II Gas Laws Equation of State: PV = nrt Same volumes of different gases have same # of molecules BTPS: body temp, atmospheric pressure, saturated ATPS: ambient
Respiration Overview I Respiration Overview II Gas Laws Equation of State: PV = nrt Same volumes of different gases have same # of molecules BTPS: body temp, atmospheric pressure, saturated ATPS: ambient
Clinical Skills. Administering Oxygen
 Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
Clinical Skills Administering Oxygen Updated July 2017 Clare Cann Original 2012 Carole Loveridge, Lecturer in Women`s Health Aims and Objectives Aims and Objectives The aim of this module is to facilitate
Exam Key. NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: % of grade in class
 NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: 100 20% of grade in class 1) An arterial blood sample for a patient at sea level is obtained, and the following physiological values
NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: 100 20% of grade in class 1) An arterial blood sample for a patient at sea level is obtained, and the following physiological values
Respiration (revised 2006) Pulmonary Mechanics
 Respiration (revised 2006) Pulmonary Mechanics PUL 1. Diagram how pleural pressure, alveolar pressure, airflow, and lung volume change during a normal quiet breathing cycle. Identify on the figure the
Respiration (revised 2006) Pulmonary Mechanics PUL 1. Diagram how pleural pressure, alveolar pressure, airflow, and lung volume change during a normal quiet breathing cycle. Identify on the figure the
Respiratory System Physiology. Dr. Vedat Evren
 Respiratory System Physiology Dr. Vedat Evren Respiration Processes involved in oxygen transport from the atmosphere to the body tissues and the release and transportation of carbon dioxide produced in
Respiratory System Physiology Dr. Vedat Evren Respiration Processes involved in oxygen transport from the atmosphere to the body tissues and the release and transportation of carbon dioxide produced in
BREATHING AND EXCHANGE OF GASES
 96 BIOLOGY, EXEMPLAR PROBLEMS CHAPTER 17 BREATHING AND EXCHANGE OF GASES MULTIPLE CHOICE QUESTIONS 1. Respiration in insects is called direct because a. The tissues exchange O 2 directly with the air in
96 BIOLOGY, EXEMPLAR PROBLEMS CHAPTER 17 BREATHING AND EXCHANGE OF GASES MULTIPLE CHOICE QUESTIONS 1. Respiration in insects is called direct because a. The tissues exchange O 2 directly with the air in
Some major points on the Effects of Hypoxia
 Some major points on the Effects of Hypoxia Source: Kings College London http://www.kcl.ac.uk/teares/gktvc/vc/dental/year1/lectures/rbmsmajorpoints/effectsofhypoxia.htm Cells obtain their energy from oxygen.
Some major points on the Effects of Hypoxia Source: Kings College London http://www.kcl.ac.uk/teares/gktvc/vc/dental/year1/lectures/rbmsmajorpoints/effectsofhypoxia.htm Cells obtain their energy from oxygen.
NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: % of grade in class
 NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: 100 20% of grade in class 1) An arterial blood sample for a patient at sea level is obtained, and the following physiological values
NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 28, 2016 Total POINTS: 100 20% of grade in class 1) An arterial blood sample for a patient at sea level is obtained, and the following physiological values
Chapter 4: Ventilation Test Bank MULTIPLE CHOICE
 Instant download and all chapters Test Bank Respiratory Care Anatomy and Physiology Foundations for Clinical Practice 3rd Edition Will Beachey https://testbanklab.com/download/test-bank-respiratory-care-anatomy-physiologyfoundations-clinical-practice-3rd-edition-will-beachey/
Instant download and all chapters Test Bank Respiratory Care Anatomy and Physiology Foundations for Clinical Practice 3rd Edition Will Beachey https://testbanklab.com/download/test-bank-respiratory-care-anatomy-physiologyfoundations-clinical-practice-3rd-edition-will-beachey/
Respiratory/Pulmonary Laboratory Experimentation
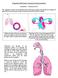 Respiratory/Pulmonary Laboratory Experimentation Introduction Anatomy Review The respiratory system has the dubious honor of being the system that permits the transport of gases from the environment inside
Respiratory/Pulmonary Laboratory Experimentation Introduction Anatomy Review The respiratory system has the dubious honor of being the system that permits the transport of gases from the environment inside
Respiratory Physiology Gaseous Exchange
 Respiratory Physiology Gaseous Exchange Session Objectives. What you will cover Basic anatomy of the lung including airways Breathing movements Lung volumes and capacities Compliance and Resistance in
Respiratory Physiology Gaseous Exchange Session Objectives. What you will cover Basic anatomy of the lung including airways Breathing movements Lung volumes and capacities Compliance and Resistance in
Chapter 17 The Respiratory System: Gas Exchange and Regulation of Breathing
 Chapter 17 The Respiratory System: Gas Exchange and Regulation of Breathing Overview of Pulmonary Circulation o Diffusion of Gases o Exchange of Oxygen and Carbon Dioxide o Transport of Gases in the Blood
Chapter 17 The Respiratory System: Gas Exchange and Regulation of Breathing Overview of Pulmonary Circulation o Diffusion of Gases o Exchange of Oxygen and Carbon Dioxide o Transport of Gases in the Blood
Respiration. The resspiratory system
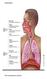 Respiration The resspiratory system The Alveoli The lungs have about 300 million alveoli, with a total crosssec onal area of 50 70 m2.. Each alveolar sac is surrounded by blood capillaries. The walls of
Respiration The resspiratory system The Alveoli The lungs have about 300 million alveoli, with a total crosssec onal area of 50 70 m2.. Each alveolar sac is surrounded by blood capillaries. The walls of
Mechanical Ventilation
 Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
Mechanical Ventilation Chapter 4 Mechanical Ventilation Equipment When providing mechanical ventilation for pediatric casualties, it is important to select the appropriately sized bag-valve mask or endotracheal
QUESTIONNAIRE FOR MEMBERS OF THE PUBLIC
 MAHSC Oxygen Project. Questionnaires for members of the public V1 10-12-2011 QUESTIONNAIRE FOR MEMBERS OF THE PUBLIC We would like to know what you think about oxygen therapy as a member of the public.
MAHSC Oxygen Project. Questionnaires for members of the public V1 10-12-2011 QUESTIONNAIRE FOR MEMBERS OF THE PUBLIC We would like to know what you think about oxygen therapy as a member of the public.
J.A. BAIN AND W.E. SPOEREL~
 PREDICTION OF ARTERIAL CARBON DIOXIDE TENSION DURING CONTROLLED VENTILATION WITH A MODIFIED MAPLESON D SYSTEM* J.A. BAIN AND W.E. SPOEREL~ ThE OBSERVATION that relatively low fresh gas inflows are adequate
PREDICTION OF ARTERIAL CARBON DIOXIDE TENSION DURING CONTROLLED VENTILATION WITH A MODIFIED MAPLESON D SYSTEM* J.A. BAIN AND W.E. SPOEREL~ ThE OBSERVATION that relatively low fresh gas inflows are adequate
BREATHING AND EXCHANGE OF GASES
 96 BIOLOGY, EXEMPLAR PROBLEMS CHAPTER 17 BREATHING AND EXCHANGE OF GASES MULTIPLE CHOICE QUESTIONS 1. Respiration in insects is called direct because a. The cell exchange O 2 directly with the air in the
96 BIOLOGY, EXEMPLAR PROBLEMS CHAPTER 17 BREATHING AND EXCHANGE OF GASES MULTIPLE CHOICE QUESTIONS 1. Respiration in insects is called direct because a. The cell exchange O 2 directly with the air in the
ALVEOLAR - BLOOD GAS EXCHANGE 1
 ALVEOLAR - BLOOD GAS EXCHANGE 1 Summary: These notes examine the general means by which ventilation is regulated in terrestrial mammals. It then moves on to a discussion of what happens when someone over
ALVEOLAR - BLOOD GAS EXCHANGE 1 Summary: These notes examine the general means by which ventilation is regulated in terrestrial mammals. It then moves on to a discussion of what happens when someone over
Capnography in the Veterinary Technician Toolbox. Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA
 Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
Capnography in the Veterinary Technician Toolbox Katie Pinner BS, LVT Bush Advanced Veterinary Imaging Richmond, VA What are Respiration and Ventilation? Respiration includes all those chemical and physical
Clinical and Statistical Evaluation of 1 st Automatic: A Pilot Study
 Clinical and Statistical Evaluation of 1 st Automatic: A Pilot Study Anne Thilde ANDERSEN, Nikolaj Børty NIELSEN, Michael TRUDSLEV, Behamin BAKHSHAIE, Shona PEDERSEN, Ole HEJLESEN Department of Health
Clinical and Statistical Evaluation of 1 st Automatic: A Pilot Study Anne Thilde ANDERSEN, Nikolaj Børty NIELSEN, Michael TRUDSLEV, Behamin BAKHSHAIE, Shona PEDERSEN, Ole HEJLESEN Department of Health
49 Arterial Blood Gases
 49 Arterial Blood Gases E. P. TRULOCK, III Definition Arterial blood gases (ABGs) is a collective term applied to three separate measurements-ph, Pco 2, and Poe -generally made together to evaluate acid-base
49 Arterial Blood Gases E. P. TRULOCK, III Definition Arterial blood gases (ABGs) is a collective term applied to three separate measurements-ph, Pco 2, and Poe -generally made together to evaluate acid-base
GASEOUS EXCHANGE 17 JULY 2013
 GASEOUS EXCHANGE 17 JULY 2013 Lesson Description In this lesson we: Discuss what is gaseous exchange? Consider requirements of an efficient gaseous exchange surface. Look at diversity in gas exchange systems.
GASEOUS EXCHANGE 17 JULY 2013 Lesson Description In this lesson we: Discuss what is gaseous exchange? Consider requirements of an efficient gaseous exchange surface. Look at diversity in gas exchange systems.
RESPIRATORY MUSCLES IN HEALTH AND EMPHYSEMA *
 THE OXYGEN CONSUMPTION AND EFFICIENCY OF THE RESPIRATORY MUSCLES IN HEALTH AND EMPHYSEMA * BY REUBEN M. CHERNIACK t (From The Winnipeg General Hospital and the Departments of Medicine and Physiology and
THE OXYGEN CONSUMPTION AND EFFICIENCY OF THE RESPIRATORY MUSCLES IN HEALTH AND EMPHYSEMA * BY REUBEN M. CHERNIACK t (From The Winnipeg General Hospital and the Departments of Medicine and Physiology and
LAB 7 HUMAN RESPIRATORY LAB. Complete the charts on pgs. 67 and 68 and read directions for using BIOPAC
 66 LAB 7 HUMAN RESPIRATORY LAB Assignments: Due before lab: Quiz: Three Respiratory Interactive Physiology Animations pages 69 73. Complete the charts on pgs. 67 and 68 and read directions for using BIOPAC
66 LAB 7 HUMAN RESPIRATORY LAB Assignments: Due before lab: Quiz: Three Respiratory Interactive Physiology Animations pages 69 73. Complete the charts on pgs. 67 and 68 and read directions for using BIOPAC
CDI Blood Parameter Monitoring System 500 A New Tool for the Clinical Perfusionist
 Original Article Blood Parameter Monitoring System 500 A New Tool for the Clinical Perfusionist David W. Fried, MS Ed, CCP; Joseph J. Leo, BS, CCP; Gabriel J. Mattioni, BS, CCP; Hasratt Mohamed, CCP; Raymond
Original Article Blood Parameter Monitoring System 500 A New Tool for the Clinical Perfusionist David W. Fried, MS Ed, CCP; Joseph J. Leo, BS, CCP; Gabriel J. Mattioni, BS, CCP; Hasratt Mohamed, CCP; Raymond
PHARMACOLOGY LABORATORY 2 PHARMACOKINETIC LABORATORY
 PHARMACOLOGY LABORATORY 2 PHARMACOKINETIC LABORATORY OBJECTIVES: 1. Reinforce the different concepts of pharmacokinetics which were presented in lecture using computer simulation of one and multiple compartment
PHARMACOLOGY LABORATORY 2 PHARMACOKINETIC LABORATORY OBJECTIVES: 1. Reinforce the different concepts of pharmacokinetics which were presented in lecture using computer simulation of one and multiple compartment
PICU Resident Self-Study Tutorial The Basic Physics of Oxygen Transport. I was told that there would be no math!
 Physiology of Oxygen Transport PICU Resident Self-Study Tutorial I was told that there would be no math! INTRODUCTION Christopher Carroll, MD Although cells rely on oxygen for aerobic metabolism and viability,
Physiology of Oxygen Transport PICU Resident Self-Study Tutorial I was told that there would be no math! INTRODUCTION Christopher Carroll, MD Although cells rely on oxygen for aerobic metabolism and viability,
(Received 16 January 1946)
 186 J. Physiol. (I946) I05, I86-I90 6I2.2I5.9 THE ABSORPTION OF FLUIDS FROM THE LUNGS BY F. C. COURTICE AND P. J. PHIPPS From the Experimental Station, Porton and the Laboratory of Physiology, Oxford (Received
186 J. Physiol. (I946) I05, I86-I90 6I2.2I5.9 THE ABSORPTION OF FLUIDS FROM THE LUNGS BY F. C. COURTICE AND P. J. PHIPPS From the Experimental Station, Porton and the Laboratory of Physiology, Oxford (Received
Section Two Diffusion of gases
 Section Two Diffusion of gases Lecture 5: Partial pressure and the composition of gasses in air. Factors affecting diffusion of gases. Ventilation perfusion ratio effect on alveolar gas concentration.
Section Two Diffusion of gases Lecture 5: Partial pressure and the composition of gasses in air. Factors affecting diffusion of gases. Ventilation perfusion ratio effect on alveolar gas concentration.
- How do the carotid bodies sense arterial blood gases? o The carotid bodies weigh 25mg, yet they have their own artery. This means that they have
 - How do the carotid bodies sense arterial blood gases? o The carotid bodies weigh 25mg, yet they have their own artery. This means that they have the highest blood flow of all organs, which makes them
- How do the carotid bodies sense arterial blood gases? o The carotid bodies weigh 25mg, yet they have their own artery. This means that they have the highest blood flow of all organs, which makes them
respiratory cycle. point in the volumes: 500 milliliters. for men. expiration, up to 1200 milliliters extra makes breathing Respiratory
 10 II. RESPIRATORY VOLUMES, CAPACITIES & PULMONARY FUNCTION TESTS Respiratory volume is the term used for various volumes of air moved by or associated with the lungs at a given point in the respiratory
10 II. RESPIRATORY VOLUMES, CAPACITIES & PULMONARY FUNCTION TESTS Respiratory volume is the term used for various volumes of air moved by or associated with the lungs at a given point in the respiratory
Section Three Gas transport
 Section Three Gas transport Lecture 6: Oxygen transport in blood. Carbon dioxide in blood. Objectives: i. To describe the carriage of O2 in blood. ii. iii. iv. To explain the oxyhemoglobin dissociation
Section Three Gas transport Lecture 6: Oxygen transport in blood. Carbon dioxide in blood. Objectives: i. To describe the carriage of O2 in blood. ii. iii. iv. To explain the oxyhemoglobin dissociation
Exploring the relationship between Heart Rate (HR) and Ventilation Rate (R) in humans.
 Exploring the relationship between Heart Rate (HR) and Ventilation Rate (R) in humans. The Research Question In this investigation I will be considering the following general research question: Does increased
Exploring the relationship between Heart Rate (HR) and Ventilation Rate (R) in humans. The Research Question In this investigation I will be considering the following general research question: Does increased
Physiology of Respiration
 Physiology of Respiration External Respiration = pulmonary ventilation breathing involves 2 processes: inspiration expiration Inspiration an active process involves contraction of diaphragm innervated
Physiology of Respiration External Respiration = pulmonary ventilation breathing involves 2 processes: inspiration expiration Inspiration an active process involves contraction of diaphragm innervated
EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES
 GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
GENERAL PROVISIONS: EMS INTER-FACILITY TRANSPORT WITH MECHANICAL VENTILATOR COURSE OBJECTIVES Individuals providing Inter-facility transport with Mechanical Ventilator must have successfully completed
Circulation and Respiration: Vital Signs Student Version
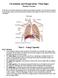 Circulation and Respiration: Vital Signs Student Version In this lab, you will learn about the circulatory and respiratory systems. You will test the capacity of your lungs, measure your blood pressure
Circulation and Respiration: Vital Signs Student Version In this lab, you will learn about the circulatory and respiratory systems. You will test the capacity of your lungs, measure your blood pressure
RESPIRATORY PHYSIOLOGY, PHYSICS AND
 Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Techniques Topic: Respiratory monitoring Date: May 05-07, 2016 Language:
Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Techniques Topic: Respiratory monitoring Date: May 05-07, 2016 Language:
Indications for Mechanical Ventilation. Mechanical Ventilation. Indications for Mechanical Ventilation. Modes. Modes: Volume cycled
 Mechanical Ventilation Eric A. Libré, MD VCU School of Medicine Inova Fairfax Hospital and VHC Indications for Mechanical Ventilation Inadequate ventilatory effort Rising pco2 with resp acidosis (7.25)
Mechanical Ventilation Eric A. Libré, MD VCU School of Medicine Inova Fairfax Hospital and VHC Indications for Mechanical Ventilation Inadequate ventilatory effort Rising pco2 with resp acidosis (7.25)
Product description concerning v-tac
 Product description concerning v-tac v-tac software calculates arterial blood gas values from venous peripheral blood gas measurement, combined with arterial oxygen saturation v-tac Product description
Product description concerning v-tac v-tac software calculates arterial blood gas values from venous peripheral blood gas measurement, combined with arterial oxygen saturation v-tac Product description
Lectures on Medical Biophysics Department of Biophysics, Medical Faculty, Masaryk University in Brno. Biophysics of breathing.
 Lectures on Medical Biophysics Department of Biophysics, Medical Faculty, Masaryk University in Brno Biophysics of breathing. Spirometry 1 Lecture outline Mechanisms of gas exchange between organism and
Lectures on Medical Biophysics Department of Biophysics, Medical Faculty, Masaryk University in Brno Biophysics of breathing. Spirometry 1 Lecture outline Mechanisms of gas exchange between organism and
Contacts. Quick Start Guide
 Contacts Clinical Support Specialist: Phone: Cell Phone: Email: Fresenius Renal Technologies A division of Fresenius Medical Care North America 920 Winter Street Waltham, MA 02451 Technical Service Customer
Contacts Clinical Support Specialist: Phone: Cell Phone: Email: Fresenius Renal Technologies A division of Fresenius Medical Care North America 920 Winter Street Waltham, MA 02451 Technical Service Customer
Respiratory System Lab
 Respiratory System Lab Note: Review the safety materials and wear goggles when working with chemicals. Read the entire exercise before you begin. Take time to organize the materials you will need and set
Respiratory System Lab Note: Review the safety materials and wear goggles when working with chemicals. Read the entire exercise before you begin. Take time to organize the materials you will need and set
Some Clinical Aspects on the Blood Gas Physiology
 Special Article* Some Clinical Aspects on the Blood Gas Physiology Hiroshi Sasamoto Professor and Chairman, Department of Medicine, School of Medicine Keio University, Shinjuku, Tokyo Recent trends on
Special Article* Some Clinical Aspects on the Blood Gas Physiology Hiroshi Sasamoto Professor and Chairman, Department of Medicine, School of Medicine Keio University, Shinjuku, Tokyo Recent trends on
Essential Skills Course Acute Care Module. Respiratory Day 2 (Arterial Blood Gases) Pre course Workbook
 Essential Skills Course Acute Care Module Respiratory Day 2 (Arterial Blood Gases) Pre course Workbook Acknowledgements This pre course workbook has been complied and updated with reference to the original
Essential Skills Course Acute Care Module Respiratory Day 2 (Arterial Blood Gases) Pre course Workbook Acknowledgements This pre course workbook has been complied and updated with reference to the original
Vital Signs Monitoring
 Vital Signs Monitoring Practical Skills Teaching Year 2 Medical Students MB BCh 2013-2014 Contents Introduction to workshop... 4 Overall Session Aim... 5 Intended Learning Outcomes... 5 Workshop Structure
Vital Signs Monitoring Practical Skills Teaching Year 2 Medical Students MB BCh 2013-2014 Contents Introduction to workshop... 4 Overall Session Aim... 5 Intended Learning Outcomes... 5 Workshop Structure
3/24/2009 LAB D.HAMMOUDI.MD. 1. Trachea 2. Thoracic wall 3. Lungs 4. Primary bronchi 5. Diaphragm
 RESPIRATORY PHYSIOLOGY LAB D.HAMMOUDI.MD 1. Trachea 2. Thoracic wall 3. Lungs 4. Primary bronchi 5. Diaphragm 1 KEY WORDS TO KNOW BOYLE S LAW INTERCOSTAL NERVES PHRENIC NERVE DIAPHRAGM EXTERNAL INTERCOSTAL
RESPIRATORY PHYSIOLOGY LAB D.HAMMOUDI.MD 1. Trachea 2. Thoracic wall 3. Lungs 4. Primary bronchi 5. Diaphragm 1 KEY WORDS TO KNOW BOYLE S LAW INTERCOSTAL NERVES PHRENIC NERVE DIAPHRAGM EXTERNAL INTERCOSTAL
SUBCUTANEOUS GAS EQUILIBRATION IN
 Tho'ax (1960), 15, 37. SUBCUTANEOUS GAS EQUILIBRATION IN CLINICAL PRACTICE BY From the Brook General Hospital, Shooters Hill, London When surgical emphysema is deliberately induced by injecting air under
Tho'ax (1960), 15, 37. SUBCUTANEOUS GAS EQUILIBRATION IN CLINICAL PRACTICE BY From the Brook General Hospital, Shooters Hill, London When surgical emphysema is deliberately induced by injecting air under
Initiation and Management of Airway Pressure Release Ventilation (APRV)
 Initiation and Management of Airway Pressure Release Ventilation (APRV) Eric Kriner RRT Pulmonary Critical Care Clinical Specialist Pulmonary Services Department Medstar Washington Hospital Center Disclosures
Initiation and Management of Airway Pressure Release Ventilation (APRV) Eric Kriner RRT Pulmonary Critical Care Clinical Specialist Pulmonary Services Department Medstar Washington Hospital Center Disclosures
Shared Haemodialysis Care Handbook. Name Hospital number: Shared HD Care Nurse: Date: Machine type: Dialysis Unit:
 Shared Haemodialysis Care Handbook Name Hospital number: Shared HD Care Nurse: Machine type: Dialysis Unit: Contents Functions of the kidney/principles of Haemodialysis... 2 Hand washing for dialysis...
Shared Haemodialysis Care Handbook Name Hospital number: Shared HD Care Nurse: Machine type: Dialysis Unit: Contents Functions of the kidney/principles of Haemodialysis... 2 Hand washing for dialysis...
Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo
 Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo Link full download: http://testbankair.com/download/test-bank-for-pilbeams-mechanicalventilation-physiological-and-clinical-applications-6th-edition-by-cairo/
Test Bank for Pilbeams Mechanical Ventilation Physiological and Clinical Applications 6th Edition by Cairo Link full download: http://testbankair.com/download/test-bank-for-pilbeams-mechanicalventilation-physiological-and-clinical-applications-6th-edition-by-cairo/
PMT. Smaller species of annelid do not have gills. Explain why these small worms do not need gills to obtain sufficient oxygen
 1. There are many different species of annelid worm. Some are very small, only a few millimetres in length. Others, such as lugworms, are much larger. The drawing shows a lugworm and part of one of its
1. There are many different species of annelid worm. Some are very small, only a few millimetres in length. Others, such as lugworms, are much larger. The drawing shows a lugworm and part of one of its
APPENDIX. working blood volume was also rather large; Evans, Grande, and. equilibrated to the new mixture is partially dependent upon the rate
 612.172-5 APPENDIX A SIMPLIFIED HEART OXYGENATOR CIRCUIT FOR BLOOD- FED HEARTS. By J. YULE BOG-UE and R. A. GREGORY.' SINCE 1934 studies on the carbohydrate metabolism of the blood-fed heart without lungs
612.172-5 APPENDIX A SIMPLIFIED HEART OXYGENATOR CIRCUIT FOR BLOOD- FED HEARTS. By J. YULE BOG-UE and R. A. GREGORY.' SINCE 1934 studies on the carbohydrate metabolism of the blood-fed heart without lungs
Medical Instruments in the Developing World
 2.2 Ventilators 2.2.1 Clinical Use and Principles of Operation Many patients in an intensive care and the operating room require the mechanical ventilation of their lungs. All thoracic surgery patients,
2.2 Ventilators 2.2.1 Clinical Use and Principles of Operation Many patients in an intensive care and the operating room require the mechanical ventilation of their lungs. All thoracic surgery patients,
MEDICAL EQUIPMENT IV MECHANICAL VENTILATORS. Prof. Yasser Mostafa Kadah
 MEDICAL EQUIPMENT IV - 2013 MECHANICAL VENTILATORS Prof. Yasser Mostafa Kadah Mechanical Ventilator A ventilator is a machine, a system of related elements designed to alter, transmit, and direct energy
MEDICAL EQUIPMENT IV - 2013 MECHANICAL VENTILATORS Prof. Yasser Mostafa Kadah Mechanical Ventilator A ventilator is a machine, a system of related elements designed to alter, transmit, and direct energy
HAEMOFILTRATION GUIDELINES
 HAEMOFILTRATION GUIDELINES The treatment mode used for Continuous Renal Replacement Therapy on the Cardiff PICU is Continuous Veno-Venous Haemofiltration (CVVH). CVVH facilitates the continuous Convective
HAEMOFILTRATION GUIDELINES The treatment mode used for Continuous Renal Replacement Therapy on the Cardiff PICU is Continuous Veno-Venous Haemofiltration (CVVH). CVVH facilitates the continuous Convective
VOLUNTARY BREATHHOLDING. I. PULMONARY GAS
 VOLUNTARY BREATHHOLDING. I. PULMONARY GAS EXCHANGE DURING BREATHHOLDING'1 By CHARLES D. STEVENS, EUGENE B. FERRIS, JOSEPH P. WEBB, GEORGE L. ENGEL, AND MYRTLE LOGAN (From the Departments of Internal Medicine
VOLUNTARY BREATHHOLDING. I. PULMONARY GAS EXCHANGE DURING BREATHHOLDING'1 By CHARLES D. STEVENS, EUGENE B. FERRIS, JOSEPH P. WEBB, GEORGE L. ENGEL, AND MYRTLE LOGAN (From the Departments of Internal Medicine
Respiratory Lecture Test Questions Set 3
 Respiratory Lecture Test Questions Set 3 1. The pressure of a gas: a. is inversely proportional to its volume b. is unaffected by temperature changes c. is directly proportional to its volume d. does not
Respiratory Lecture Test Questions Set 3 1. The pressure of a gas: a. is inversely proportional to its volume b. is unaffected by temperature changes c. is directly proportional to its volume d. does not
Section 01: The Pulmonary System
 Section 01: The Pulmonary System Chapter 12 Pulmonary Structure and Function Chapter 13 Gas Exchange and Transport Chapter 14 Dynamics of Pulmonary Ventilation HPHE 6710 Exercise Physiology II Dr. Cheatham
Section 01: The Pulmonary System Chapter 12 Pulmonary Structure and Function Chapter 13 Gas Exchange and Transport Chapter 14 Dynamics of Pulmonary Ventilation HPHE 6710 Exercise Physiology II Dr. Cheatham
exchange of carbon dioxide and of oxygen between the blood and the air in
 M. M. HENRY WILLIAMS, JR.*Cardiorespiratory Laboratory, Grasslands WILLIAMS, JR.* Hospital, Valhalla, New York SOME APPLICATIONS OF PULMONARY PHYSIOLOGY TO CLINICAL MEDICINE During the past ten years a
M. M. HENRY WILLIAMS, JR.*Cardiorespiratory Laboratory, Grasslands WILLIAMS, JR.* Hospital, Valhalla, New York SOME APPLICATIONS OF PULMONARY PHYSIOLOGY TO CLINICAL MEDICINE During the past ten years a
P215 Respiratory System, Part 2
 P15 Respiratory System, Part Gas Exchange Oxygen and Carbon Dioxide constant need for oxygen constant production of carbon dioxide exchange (and movement) lung alveoli pulmonary arteries pulmonary capillaries
P15 Respiratory System, Part Gas Exchange Oxygen and Carbon Dioxide constant need for oxygen constant production of carbon dioxide exchange (and movement) lung alveoli pulmonary arteries pulmonary capillaries
London Respiratory Team
 London Respiratory Team By email 28 March 2012 Ambulatory Oxygen for London This guide has been produced to help healthcare maximise the benefit of the new oxygen contract for patients and to reduce waste.
London Respiratory Team By email 28 March 2012 Ambulatory Oxygen for London This guide has been produced to help healthcare maximise the benefit of the new oxygen contract for patients and to reduce waste.
Measuring Lung Capacity
 Name Class Date Chapter 37 Circulatory and Respiratory Systems Measuring Lung Capacity Introduction The amount of air that you move in and out of your lungs depends on how quickly you are breathing. The
Name Class Date Chapter 37 Circulatory and Respiratory Systems Measuring Lung Capacity Introduction The amount of air that you move in and out of your lungs depends on how quickly you are breathing. The
THE EFFECT OF INTERMITTENT EXPOSURE TO 3% C0 2 ON ACID-BASE BALANCE AND ELECTROLYTE EXCRETION
 THE EFFECT OF INTERMITTENT EXPOSURE TO 3% C0 2 ON ACID-BASE BALANCE AND ELECTROLYTE EXCRETION by K. E. Schaefer C. C. Morgan A. A. Messier and M. J. Jacey SUBMARINE MEDICAL RESEARCH LABORATORY NAVAL SUBMARINE
THE EFFECT OF INTERMITTENT EXPOSURE TO 3% C0 2 ON ACID-BASE BALANCE AND ELECTROLYTE EXCRETION by K. E. Schaefer C. C. Morgan A. A. Messier and M. J. Jacey SUBMARINE MEDICAL RESEARCH LABORATORY NAVAL SUBMARINE
Arterial Punctures Blood Gas Collections (ABG)
 Arterial Punctures Blood Gas Collections (ABG) Danny Grabau, CPT, (NHA) Clinical Core Laboratory Services Phlebotomy Education Assistant Randy Gruhlke, MS, PBT(ASCP) Associate Program Director, Phlebotomy
Arterial Punctures Blood Gas Collections (ABG) Danny Grabau, CPT, (NHA) Clinical Core Laboratory Services Phlebotomy Education Assistant Randy Gruhlke, MS, PBT(ASCP) Associate Program Director, Phlebotomy
Breathing: The normal rate is about 14 to 20 times a minute. Taking in of air is called Inspiration and the forcing out of air is called Expiration.
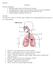 Biology 12 Respiration Divisions of Respiration Breathing: entrance and exit of air into and out of the lungs External Respiration: exchange of gases(o2 and CO2) between air (in alveoli) and blood Internal
Biology 12 Respiration Divisions of Respiration Breathing: entrance and exit of air into and out of the lungs External Respiration: exchange of gases(o2 and CO2) between air (in alveoli) and blood Internal
Respiration Lab Instructions
 Respiration Lab Instructions This laboratory investigation can be performed in any order. Be sure to read all instructions for each section before performing the experiment. PART 1 STUDENT WET SPIROMETER
Respiration Lab Instructions This laboratory investigation can be performed in any order. Be sure to read all instructions for each section before performing the experiment. PART 1 STUDENT WET SPIROMETER
Regulation of Breathing
 Regulation of Breathing Introduction Breathing involves a complex interaction between many important respiratory organs and the blood. Air is brought into the lungs through the active process of inhalation,
Regulation of Breathing Introduction Breathing involves a complex interaction between many important respiratory organs and the blood. Air is brought into the lungs through the active process of inhalation,
AQUADEX FLEXFLOW SYSTEM QUICK REFERENCE GUIDE
 AQUADEX FLEXFLOW SYSTEM QUICK REFERENCE GUIDE AQUADEX FLEXFLOW SYSTEM DISCLAIMER The quick reference guide is not intended to replace CHF Solutions, Inc. Aquadex FlexFlow Direction For Use (DFU). Always
AQUADEX FLEXFLOW SYSTEM QUICK REFERENCE GUIDE AQUADEX FLEXFLOW SYSTEM DISCLAIMER The quick reference guide is not intended to replace CHF Solutions, Inc. Aquadex FlexFlow Direction For Use (DFU). Always
Mechanical Ventilation. Which of the following is true regarding ventilation? Basics of Ventilation
 Mechanical Ventilation Jeffrey L. Wilt, MD, FACP, FCCP Associate Professor of Medicine Michigan State University Associate Program Director MSU-Grand Rapids Internal Medicine Residency Which of the following
Mechanical Ventilation Jeffrey L. Wilt, MD, FACP, FCCP Associate Professor of Medicine Michigan State University Associate Program Director MSU-Grand Rapids Internal Medicine Residency Which of the following
A method for mathematical arterialization of venous blood gas
 A method for mathematical arterialization of venous blood gas v-tac is an advanced software algorithm that converts venous blood gas, combined with an SpO2 measurement, to arterial blood gas values with
A method for mathematical arterialization of venous blood gas v-tac is an advanced software algorithm that converts venous blood gas, combined with an SpO2 measurement, to arterial blood gas values with
Chapter 13 The Respiratory System
 Chapter 13 The Respiratory System by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Atmosphere Tissue cell External respiration Alveoli of lungs 1 Ventilation or gas exchange between the atmosphere
Chapter 13 The Respiratory System by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Atmosphere Tissue cell External respiration Alveoli of lungs 1 Ventilation or gas exchange between the atmosphere
J. Physiol. (I941) I00, I98-21I 6I :6I2.825
 198 J. Physiol. (I941) I00, I9821I 6I2.22.02:6I2.825 THE EFFECT OF OXYGEN LACK ON THE CEREBRAL CIRCULATION BY F. C. COURTICE From the Departments of Physiology and of Surgery, Oxford (Received 24 March
198 J. Physiol. (I941) I00, I9821I 6I2.22.02:6I2.825 THE EFFECT OF OXYGEN LACK ON THE CEREBRAL CIRCULATION BY F. C. COURTICE From the Departments of Physiology and of Surgery, Oxford (Received 24 March
ONLINE DATA SUPPLEMENT. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg
 APPENDIX 1 Appendix 1. Complete respiratory protocol. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg predicted body weight (PBW)) (NEJM 2000; 342
APPENDIX 1 Appendix 1. Complete respiratory protocol. First 24 hours: All patients with ARDS criteria were ventilated during 24 hours with low V T (6-8 ml/kg predicted body weight (PBW)) (NEJM 2000; 342
CHAPTER 6. Oxygen Transport. Copyright 2008 Thomson Delmar Learning
 CHAPTER 6 Oxygen Transport Normal Blood Gas Value Ranges Table 6-1 OXYGEN TRANSPORT Oxygen Dissolved in the Blood Plasma Dissolve means that the gas maintains its precise molecular structure About.003
CHAPTER 6 Oxygen Transport Normal Blood Gas Value Ranges Table 6-1 OXYGEN TRANSPORT Oxygen Dissolved in the Blood Plasma Dissolve means that the gas maintains its precise molecular structure About.003
CHAPTER 17 BREATHING AND EXCHANGE OF GASES
 268 BIOLOGY CHAPTER 17 BREATHING AND EXCHANGE OF GASES 17.1 Respiratory Organs 17.2 Mechanism of Breathing 17.3 Exchange of Gases 17.4 Transport of Gases 17.5 Regulation of Respiration 17.6 Disorders of
268 BIOLOGY CHAPTER 17 BREATHING AND EXCHANGE OF GASES 17.1 Respiratory Organs 17.2 Mechanism of Breathing 17.3 Exchange of Gases 17.4 Transport of Gases 17.5 Regulation of Respiration 17.6 Disorders of
RESPIRATORY PHYSIOLOGY. Anaesthesiology Block 18 (GNK 586) Prof Pierre Fourie
 RESPIRATORY PHYSIOLOGY Anaesthesiology Block 18 (GNK 586) Prof Pierre Fourie Outline Ventilation Diffusion Perfusion Ventilation-Perfusion relationship Work of breathing Control of Ventilation 2 This image
RESPIRATORY PHYSIOLOGY Anaesthesiology Block 18 (GNK 586) Prof Pierre Fourie Outline Ventilation Diffusion Perfusion Ventilation-Perfusion relationship Work of breathing Control of Ventilation 2 This image
Gas exchange. Tissue cells CO2 CO 2 O 2. Pulmonary capillary. Tissue capillaries
 Gas exchange Pulmonary gas exchange Tissue gas exchange CO 2 O 2 O 2 Tissue cells CO2 CO 2 Pulmonary capillary O 2 O 2 CO 2 Tissue capillaries Physical principles of gas exchange Diffusion: continuous
Gas exchange Pulmonary gas exchange Tissue gas exchange CO 2 O 2 O 2 Tissue cells CO2 CO 2 Pulmonary capillary O 2 O 2 CO 2 Tissue capillaries Physical principles of gas exchange Diffusion: continuous
Physiology of the Respiratory System
 Biology 212: Anatomy and Physiology II Physiology of the Respiratory System References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning
Biology 212: Anatomy and Physiology II Physiology of the Respiratory System References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning
breathing oxygen-rich gas mixtures" was made in 1911 by Benedict the London Hospital.
 THE; EFFECT OF INHALATION OF OXYGEN ON THE RATE OF THE PULSE IN HEALTH. BY JOHN PARKINSON, M.D., M.R.C.P., Medical Registrar to the London Hospital. NONE of the early workers on the effect of oxygen on
THE; EFFECT OF INHALATION OF OXYGEN ON THE RATE OF THE PULSE IN HEALTH. BY JOHN PARKINSON, M.D., M.R.C.P., Medical Registrar to the London Hospital. NONE of the early workers on the effect of oxygen on
Errors in Monitoring. BWH Clinical Conference 10/06/04. Copyright 2004, James H Philip, all rights reserved.
 Errors in Monitoring BWH Clinical Conference 10/06/04 Copyright 2004, James H Philip, all rights reserved. Technology Block 2004 10/06/04 James Philip MD Low flow&closed circuit safety&danger 10/06/04
Errors in Monitoring BWH Clinical Conference 10/06/04 Copyright 2004, James H Philip, all rights reserved. Technology Block 2004 10/06/04 James Philip MD Low flow&closed circuit safety&danger 10/06/04
Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams)
 Name Lab Partners Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams) Part 1. Lung Volumes and Capacities Objectives 1. Obtain graphical representation of lung capacities
Name Lab Partners Lab 3. The Respiratory System (designed by Heather E. M. Liwanag with T.M. Williams) Part 1. Lung Volumes and Capacities Objectives 1. Obtain graphical representation of lung capacities
Clinical Engineering. Equipment (Heart-lung machines)
 Clinical Engineering Clinical Engineering Equipment (Heart-lung machines) Syed Mohd Nooh Bin Syed Omar Open Heart Surgery Coronary artery bypass grafting (CABG) Repair or replace valves (Stenosis @ Regurgitation)
Clinical Engineering Clinical Engineering Equipment (Heart-lung machines) Syed Mohd Nooh Bin Syed Omar Open Heart Surgery Coronary artery bypass grafting (CABG) Repair or replace valves (Stenosis @ Regurgitation)
Yanal. Jumana Jihad. Jamil Nazzal. 0 P a g e
 2 Yanal Jumana Jihad Jamil Nazzal 0 P a g e note: this sheet was written and corrected according to the records from section 2 so you may find differences in the arrangement of topics from the records
2 Yanal Jumana Jihad Jamil Nazzal 0 P a g e note: this sheet was written and corrected according to the records from section 2 so you may find differences in the arrangement of topics from the records
