Lecture. Key concepts
|
|
|
- Angela Collins
- 5 years ago
- Views:
Transcription
1 Dr.Puntarica Suwanprathes Physiology Department Faculty of Medicine Siriraj Hospital Mahidol University 1 2 version 2005 Lecture 1. Basic principle 2. Mechanic of breathing (x2) 3. Lung volume 4. Pulmonary circulation 5. Control of ventilation (x2) 6. Blood gas diffusion Blood gas and ph (Yr III) (Total: 11 hrs +1 hr) Name: ป ณฑร กา ส วรรณประเทศ office: ต กจ ฑาธ ช 1 7. Blood gas transport Tel: ext: Metabolism 4 Key concepts กระบวนการท างานของระบบหายใจ หล กการทางฟ ส กส ในสร รว ทยาระบบหายใจ โครงสร างของปอด โครงสร างของทรวงอก หน าท อ นๆ ของปอด 5 6
2 ENERGY chemical reaction O 2 chemical reaction metabolism (conversion of energy forms) 7 CO 2 ENERGY 8 Multi-cellular organism simple diffusion cell membrane unicellular organism 9 10 evolution supply O 2 get rid of CO
3 MATCHING Ventilation Blood flow Air pump supply get rid of Ventilation-perfusion ratio V/Q ratio = 0.8 Blood pump Breathing or Respiration In general: Physiology: External Respiration Transport mechanism Internal Respiration 15 p.456 Respiration processes breathing external respiration pulmonary ventilation diffusion blood-gas tansportation diffusion internal respiration or cellular respiration 16 get rid of CO2 supply O 2 PaO 2 = 100 mm.hg PaCO 2 =40mm.Hg Partial Pressure of Gas Gas % pressure or tension Unit: mmhg ABG 17 18
4 Left ventricle reservoir Biochemical reaction Gas exchange Filtration Air conditioning 19 Airway defense mechanism 20 Respiratory Structure Ventilation Diffusion Perfusion 21 URI Upper respiratory tract nasal cavity trachea Lower respiratory tract lower part of trachea main bronchai + lungs Thoracic cavity 22 Respiratory Structure 2 zones 1. Conducting zone 2. Respiratory zone 23 Structures of the lungs Respiratory tract airways 23 generations Weibel conducting zone anatomical dead space 16 generations Respiratory zone respiratory unit acinus 7 generations 24
5 Pharynx Nasal cavity nose Trachea Nostril Larynx terminal bronchioles Right lung Left lung No gas exchange acinus 5 mm Anatomical dead space 25 ~ μ 26 Trachea wind pipe Tracheal rings: C-shaped, cartilagenous rings (keep trachea open) Bronchus (primary, 1 O ) first branch off the trachea similar in structure to the trachea smaller bronchi, less cartilage Bronchioles *** no cartilage smooth muscles dominates lumen diameter is regulated by the ANS Sympth: diameter Parasymp: diameter 27 Right Lungs Left: 2 lobes Cardiac notch. Right: 3 lobes Left are made of collections of 2 O bronchi and 3 O bronchi, bronchioles, alveoli and other structures 28 Alveoli respiratory bronchioles alveolar ducts alveolar sacs alveoli gas exchange 5 mm million (30 million 2-3 yrs 8 yrs) diameter ~ μ surface area m 2 (40 times more than BSA: body surface area) 30
6 Alveolus Types 2 pneumocytes Types 1 pneumocytes interstital fluid alveolar fluid lining with pulmonary surfactant macrophages Alveolar capillary membrane alveolus 0.2 μ Alveolar capillary membrane Alveolar epithelium Type I: alveolar epithelial cell or squamous pneumocytes μ thick about 90% of alveolar surface plays a role in gas exchange Type II: alveolar epithelial cell or granular pneumocyte secrete surfactant, which reduce the surface tension assist pulmonary extension in respiration. macrophage or dust cell phagocytoses airborne particles, microorganisms and pulmonary cell debris and keep the alveolar surface clean 33 Left ventricle reservoir Filtration Biochemical reaction Air conditioning Airway defense mechanism 34 Air conditioning Filtration warming moisturizing filtering nose, nasal turbinate: particles > 10 μm nasopharynx-larynx: particles < 10 μm trachea, bronchi: particles 2-10 μm alveolar duct, alveoli: particles μm expired air: particles < 0.5 μm 35 36
7 mucous membrane covered with cilia Filtration hair dust particles eddy current Turbulent precipitation mucus Turbulent precipitation mucus Terminal bronchioles ciliated nasal septum epithelial ciliary escalator turbinates membranes pharyngeal wall Airway defense mechanisms Airway defense mechanisms Lungs the largest surface area of the body in contact with the environment Mucocilliary transport susceptible to damage by foreign materials dust particles pollen airborne pollutants gateway for infection bacteria viruses fungal spores 39 Phagocytic macrophage 40 Mucocilliary transport cells with microvilli 2 - ciliated cells ciliated cells beat at 20 cycle/sec mucociliated escalator mm/min (in small airways) 5-20 mm/min (in trachea and main bronchi) paralysis of cilia from noxious agents (eg. sulphur dioxide, ) smoke cold air many drugs (eg. general anaesthetics) 41 dust particle gel layer sol layer mucus mucus gland globlet cell 42
8 Phagocytic macrophage macrophage phagocytic macrophages dust cells dust particles bacteria debris etc. ingest and transport to Bronchioles mucocilliary clearance Lymphatic system or CVS 43 high density of blood supply nose nasopharynx Warming nasal cavity nasal septum turbinates Humidification lower trachea Air temp. close to body temp. 44 Key concepts 1) physic of gases 2) partial pressure of gases 3) lung volumes and capacities 4) minute ventilation and alveolar ventilation PACO 2 5) alveolar ventilation 45 PAO 2 46 Physics of gases gas gas particles are always in motion random movement travel in straight lines unless they collide other particles or the walls of the container pressure 47 48
9 Boyle s law gas particles temp pressure volume 49 temp.: constant volume = constant pressure 50 Charles's Law pressure: constant volume = constant x temperature 51 absolute (Kelvin) degree (273 o K= 0 o C) volume: constant pressure = constant x temperature 52 Gas Law Boyle s law + Charles s law pressure, volume, temperature PV = nrt PV = nr = constant T P 1 V 1 = P 2 V 2 T 1 T 2 n = mols R = gas constant R = mmhg-l/k-mol) P = mm.hg V =L T = Kelvin 53 Partial Pressure of Gas Gas % pressure or tension Unit: mmhg 54
10 Dalton s law of partial pressure Partial Pressure of Gas P A P B P C Definition:. each gas Partial Pressure of Gas P A P B P C gas mixture (A+ B +C) total gas pressure (Ptot) gas mixture gas A gas B gas C partial pressure of gas X (Px) partial pressure or tension % or concentration of gas X 55 gas mixture gas A gas B gas C PA PB PC = PA + PB + PC e.g. (50%) (30%) (20%) Ptot = 100 mmhg Ptot = 200 mmhg Ptot = 760 mmhg 56 Ptot = 760 mmhg Atmospheric pressure (P B ) or 1 ATP Partial Pressure of Gas gas mixture gas A gas B gas C 50% 30% 20% if Ptot = 100 mmhg if Ptot = 760 mmhg Px = Ptot. Fx Fx PC = 20 mmhg PC = 20 x fractional concentration of gas x 57 gas A PA gas B gas C + + = PB PC gas mixture (A+ B +C) PA + PB + PC Px = Ptot. Fx < 1 Px = partial pressure P = total dry gas pressure Fx = fractional concentration of gas x X% The vapor pressure of water sea level water Gas saturated with water vapor H 2 O H 2 O H 2 O Atmospheric pressure (P B ) = 760 mm.hg (1 ATP) Total pressure = summation of partial pressure of each gases PB = PO 2 + PCO 2 + PN 2 + PH 2 O vapor pressure H 2 O of water 59 60
11 humidified air PB = PO 2 + PCO 2 + PN 2 + PH 2 O Temp.? water vapor partial pressure 37 o 37 0 C, PH 2 O = C, PH 2 O = C, PH 2 O = 30 mmhg water vapor at body temperature = 47 mm.hg 61 ***Body 37 0 C, PH 2 O = 47 mmhg PO 2 + PCO 2 + PN 2 = PB - 47 = 713 mmhg 62 dry gas Px = (760 47) Fx e.g. alveolar air (% of dry gas) O 2 = 14% CO 2 = 5.6% N 2 = 80.4% e.g. PACO2 = PAO 2 = (760-47) x 5.6 ~ 40 mm.hg 100 (760-47) x 14 ~ 100 mm.hg Pulmonary Function Test Spirometer PFT Spirometer Spirometry Spirogram Volume-displacement spirometer displacement of the bell etc. * Flow-sensing spirometer 65 66
12 Volume-displacement spirometer mid-twentieth century based on the simple mechanical principle.air, exhale from the lung, will cause displacement of a closed chamber that is partially submerged in water 67 counterbalance cylinder water pen weight Rotating drum inspiration 68 Flow-sensing spirometer Pulmonary capacities Pulmonary volume add water 400 ml ml. capacities volume B add water 600 ml. volume A Lung volumes Spirogram Pulmonary volumes (500 ml) Tidal Volume (3000 ml) Inspiratory Reserve Volume (1100 ml) Expiratory Reserve Volume (1200 ml) Residual Volume Pulmonary capacities Inspiratory Capacity Vital Capacity Functional Residual Capacity Total Lung Capacity (resting expiration level) 71 volumes capacities 72
13 Residual Volume B A Expiratory Reserve Volume Tidal volume Inspiratory Reserve Volume resting expiration level ventilation rest, Tidal volume ~ 500 ml. (TV or V T ) 350 ml. 150 ml. alveoli alveolar air conducting airways anatomical dead space 75 (V D ) Dead space Definition:... 3 types: Anatomical dead space, VD 2. Alveolar dead space 3. Physiological dead space 76 Anatomical dead space Alveolar dead space No gas exchange dead space or Dead space volume ~ 150 ml Alveolar dead space diffusion no diffusion gas exchange Alveolar volume or Alveolar air ~ 350 ml 77 Causes: no blood flow blood flow (uneven V/Q) *** note: in normal lungs very small!!! 78
14 Physiological dead space Anatomical dead space Alveolar dead space*** Minutes Ventilation VT Minute Volume MV or Minute Ventilation V T definition:.. MV = TV x RR Unit: Liter / minute V T = V T x RR Respiratory Minute Volume Minute Volume MV 81 at rest: TV ~ 500 ml RR ~ count / minute MV ~ 6000 ml (6 L) to 10,000ml (10 L) 82 Alveolar Ventilation Alveolar Ventilation No gas exchange VA definition:.. dead space or Dead space volume ~ 150 ml Unit: Liter / minute gas exchange Alveolar air 83 Alveolar volume or Alveolar air ~ 350 ml 84
15 Alveolar Ventilation VA V A = (V T - V D ) x RR = ( ) x 12 (or x 20) = 4,200 ml/min (or 7,000 ml/min) = 4.2 L/min (or 7 L/min ) CO 2 O 2 V A ~ 3-7L,average = 5L VA ~ 70% VT Respired air end-tidal sample 14% 5.6% inspired air 20.94% 0.04% alveolar air expired air 16.3% 4.5% dead space air alveolar air %O 2 VD PACO 2 PACO 2 VECO 2 %CO VA VT = PACO 2 - PECO 2 PACO 2 VD VT = PACO 2 - PECO 2 PACO 2 (~ mmhg) FECO 2 x VT = (FICO 2 x VD) + (FACO 2 x VA) C R %CO 2 expired air inspired air 4.5% 0.04% TV = 450 ml alveolar air 5.6% 89 Anatomical dead space VD ~ 150 ml 90
16 PACO 2 VECO 2 VA constant Abnormal in Alveolar Ventilation If VA Alveolar hypoventilation Alveolar hyperventilation hyperventilation PaCO 2 PaCO 2 If VA hypoventilation Key concepts 2 circulation 1) pulmonary circulation compare with systemic circulation 2) pulmonary vascular resistance (PVR) Bronchial circulation 3) passive and active changes of PVR 4) ventilation-perfusion ratio Alveoli 95 Pulmonary circulation 96
17 deoxygenated blood mixed venous blood 3cm, length 5 cm Pulmonary artery Pulmonary circulation *** Alveolar capillaries Systemic circulation Bronchial circulation oxygenated blood Bronchial artery Function Pulmonary circulation SYSTEM Right lung vessels 1) Reservior 5 parts working system 2) Pump Upper body vessels 3) Distributing system pulm. artery (150 ml) Left lung vessels 4) Exchange system pulm. capillaries bed (~75 ml) =SV p.510 Tracheobronchial tree 97 Lower body vessels Note: pulmonary blood volume ~500 ml 5) Collecting system pulm. venules vein (270 ml) 98 Pulmonary circulation Pulmonary artery 24/9 (mean=14) Pulmonary capillaries Pulmonary vein Pulmonary circulation low pressure *** System circulation 100 1/7 Systemic vein /0 120/ Systemic circulation Systemic artery (Aorta) 120/80 (mean=100) 2 14 pulm. capillaries bed 10 5 Unit: mmhg 99 Systemic capillaries p.510 Unit: mmhg 100 Pulmonary circulation Pulmonary circulation Outer layer thinner smooth muscle Elastic white fibrous tissue Lesser circulation Endothelial cells Physiological functions Gas exchange Filter Blood reservoir for left ventricle Supply nutrients to lung itself Fluid exchange low pressure Angiotensin converting enzyme low resistance low vasomotor tone highly distensible
18 Exchange system diffusion area diffusion distance pulm. capillaries bed pulmonary capillaries bed network oriented thin-film coated look (thick ~ 0.1 μ) total exchanging areas ~ 70m 2 (40 times BSA) 103 pulm. capillaries pressure if pressure e.g. Lt. ventricle failure Pulmonary congestion H 2 O Lung compliance plasma protein < colloidal osmotic pressure (25 mmhg) 104 Pulmonary circulation Pulmonary capillaries Unit: mmhg Ohm s law: Resistance = Driving pressure Blood flow vascular resistance = pulm. arterial pr. left atrium pr. PVR = PPA - PLA Q 6 L/min Blood flow mm.hg L/min cardiac output 105 PVR = Pulmonary artery 24/9 (mean= 14) PPA - PLA Q Systemic vein PVR = = C.O. = 1 mmhg/l/min / /0 Systemic capillaries 9 30 Pulmonary vein Systemic circulation Systemic artery (Aorta) 120/80 (mean= 100) R = = 16.6 mmhg/l/min 106 Pulmonary circulation: 1 mmhg/l/min 0.06 mmhg/ml/sec Resistance ~ 0.06 mmhg ml/sec Systemic circulation: 16.6 mmhg/l/min mmhg/ml/sec Resistance ~ 1 mmhg ml/sec 16 times 107 Pulmonary vascular resistance Alternation of pulmonary vascular resistance 1. Passive change (change in environment) pulmonary blood flow lung volume (during inspiration- expiration) 2. Active change Hypoxia PACO 2 pressure in Lt. Atrium chemicals 108
19 Passive change Pulmonary blood flow rest collapse normal blood flow: 5-6 L/min during exercise blood flow e.g. exercise PVR = PPA - PLA Q dilate blood flow l/min or more BUT PVR slightly 109 recruitment distension 110 Passive change Passive change pulmonary arterial or venous pressure recruitment Pulmonary vascular resistance distension Lung volume normal CO CO p Pulmonary blood vessel location alveolar vessels extra-alveolar vessels alveolar vessels Alveolar vessels capillaries small arterioles venules extra-alveolar vessels Factor: Intrapleural pressure Extra-alveolar vessels capillaries *** small arterioles small venules pulmonary arteries pulmonary veins capillaries Pulmonary arteries Pulmonary veins corner vessels corner vessels Factor: Lung volume
20 capillary alveolar vessels extra-alveolar vessels Alveolar vessels capillaries small arterioles venules Factor: Intrapleural pressure Extra-alveolar vessels Pulmonary arteries Pulmonary veins inspiration lung volume vessels are compressed R capillaries Breath in expiration lung volume vessels distend R 115 Factor: Lung volume distend more - pr. 116 Pulmonary vascular resistance over all Effects of lung volume on pulmonary vascular resistance *** alveolar vessels extra-alveolar vessels *** FRC Active change Local Hypoxia Active change Hypoxemia ventilation PAO 2 Systemic Hypoxia PaO 2 (eg. High altitude) arteriolar constriction local HYPOXIA H + local response arteriolar constriction resistance O 2 pulm. vasoconstriction recruitment resistance..to e V/Q ratio Pulmonary arterial pressure shift blood 119 if chronic: pulmonary hypertension 120
21 Ventilation-Perfusion Relationships Ventilation-Perfusion Relationships Ideal lung 121 Factor 2: Rate? Blood flow concentartion = V/Q (gm/l) alveolar ventilation Model: 1 lung unit Factor 1: Rate? V (gm/min) con n Diffusion con n 122 Ventilation-Perfusion Relationships concentration = V/Q (gm/l) O 2 concentration in any lung unit (or PO 2 ) = ventilation blood flow Normal V/Q ratio PaO 2 = 100 mmhg PaCO 2 = 40 mmhg Ventilation-perfusion ratio V/Q ratio 123 Decreasing V/Q ratio Increasing V/Q ratio 124 V/Q ratio V/Q ratio alveolar PO 2 & PCO 2 arterial blood ventilation blood flow = 4 L/min = L/min In rest: O 2 consumption = 250 ml/min CO 2 production = 200 ml/min ventilation blood flow = 4 L/min = L/min rate 4 L/min matching If: V/Q ratio change? mismatch or uneven matching abnormal of Gas exchange air blood rate 5 L/min 125 PaO 2 & PaCO 2 126
22 Distribution of Distribution of Distribution of p.519 gravity Distribution of non-uniform distribution apex gravity Distribution of non-uniform distribution gravity 30 cm vary in hydrostatic pressure base > apex apex vary in hydrostatic pressure base > apex base 30 cm.h 2 O or 23 mm.hg 30 cm 30 cm.h 2 O or 23 mm.hg effect to regional blood flow *** blood flow to base > apex 129 base effect to regional blood flow *** blood flow to base > apex cm.H 2 O Distribution of apex non-uniform distribution gravity (wt.) vary in intrapleural pressure base (- pr.) < apex -10cm.H 2 O Distribution of apex 30 cm non-uniform distribution gravity (wt.) vary in intrapleural pressure base (- pr.) < apex 30 FRC: intrapleural pressure Base: -2.5cm.H 2 O apex: -10cm.H 2 O cm.h 2 O base initial base< cm.h 2 O FRC: intrapleural pressure Base: -2.5cm.H 2 O apex: -10cm.H 2 O initial base < apex when inspiration: *** ventilation to Base > Apex 131 when inspiration: *** ventilation to base > apex 132
23 slope p.521 *** higher C L more steep A2 B2 B1 = A1 volume *** V P V P higher C L more steep p Distribution of Distribution FRC: intrapleural pressure apex: -10cm.H 2 O base: cm.h 2 O less - cm.h 2 O FRC: intrapleural pressure apex: -10cm.H 2 O base: cm.h 2 O less - cm.h 2 O RV: intrapleural pressure apex: less negative base: + cm.h 2 RV: intrapleural pressure apex: less negative 30 cm base: + cm.h 2 O + cm.h 2 O base 30 cm small airways collapse!!! dynamic compression of airway *** when inspiration: *** ventilation to Apex > Base cm.h 2 O base small airways collapse!!! dynamic compression of airway *** when inspiration: *** ventilation to apex > base 136 Distribution of gravity perfusion: lesser apex transmural pr. alveoli: dilate zone 1 higher V/Q ratio press capillaries ventilation > perfusion dead space like effect lower V/Q ratio zone 2 zone 3 gravity ventilation = perfusion perfusion: greater arterial blood pr. Distribution of ***ventilation 1/3 blood flow 0.6 press alveoli base ventilation < perfusion venous-admixture effect or shut like effect 137 Base Apex 138 p.523 p.520
24 p Key concepts 1) Fick s law of diffusion 2) factors which limit gas transfer 3) diffusion capacity gas gaseous phase dissolved gas exert pressure*** equilibrium volume of dissolved gas partial pressure solubility 142 Graham s law diffusion rate or diffusion constant (D) = solubility Gaseous medium Liquid medium Gaseous medium MW CO 2 diffusion rate O 2 diffusion rate 5.6 = x = CO 2 diffusion rate O 2 diffusion rate = MW O 2 MW CO 2 = = Liquid medium CO 2 solubility O 2 solubility = = CO 2 diffusion rate faster than O 2 20 times 144
25 Solubility of Gas Henry s law CO 2 =PO 2. αo 2 CO 2 : concentration of O 2 (ml. O 2 /ml. solution) PO 2 : partial pressure or tension of O 2 (mm.hg) αo 2 : solubility coefficient of O 2 (ml. O 2 in 1 ml. solution / 1 ATP) 37 0 C : αo 2 = αco 2 = diffuse faster 145 equilibrium dissolved gas Low pressure equilibrium Low concentration Double the pressure equilibrium Double the concentration volume = partial pressure x solubility coefficient of dissolved gas (solubility) or concentration in solution 146 volume = partial pressure x solubility coefficient of dissolved gas or concentration constant in solution Diffusion concentration gas X in A > B Pressure gradient volume α partial pressure of that gas of dissolved gas A B gas mixture (A+ B +C) PA + PB + PC independence 147 partial pressure A > B diffuse from A to equilibrium A = B 148 Gas diffusion in Lungs PACO 2 40 mmhg PAO mmhg Duffusion rate: in gaseous medium Duffusion rate: in liquid medium PVCO 2 46 mmhg FACTORS: Diffusion rate Diffusion capacities PVO 2 40 mmhg
26 in gaseous medium diffusion rate: faster Graham s law Diffusion rate molecular wt.: lighter diffusion rate α 1 square root of density CO 2 diffusion rate = molecular wt. of O 2 alveolar duct diffusion distance ~1 mm alveolar-capillary interface O 2 diffusion rate molecular wt. of CO 2 = 32 = almost complete in sec. (80%) 152 Diffusion rate in liquid medium solubility pressure gradient or concentration gradient Henry s law volume α partial pressure of that gas of dissolved gas diffusion rate α solubility Diffusion rate O 2 > CO 2 in gaseous medium Graham s law CO 2 > O 2 in liquid medium Henry s law CO 2 diffusion rate = = 24.3 O 2 diffusion rate CO 2 diffusion rate = 5.6 x = 20.6 O 2 diffusion rate 6.6 x FACTORS: Diffusion rate Fick s law (Law of diffusion) V gas α A. D. (P 1 -P 2 ) T solubility MW V = diffusion rate A = area of diffusion D = diffusion constant T = length of diffusion path P 1 -P 2 = difference in partial pressure 155 Pressure difference across membrane difference in partial pressure alveoli pulm. capillary blood A diffusion rate time in pulmonary capillary = 0.75 sec. diffusion time = 0.25 sec. during exercise??? B 75 ml = 6 L/min pulm. blood flow 156
27 PvO 2 40 mmhg PvCO 2 45 mmhg O 2 CO 2 equilibrium PaO mmhg PaCO 2 40 mmhg PaO 2.. sec normal alveolar-capillary block severe Hypoxemia mixed venous PO Diffusion capacities Diffusion capacities diffusion P: 1 mmhg V (ml) time: 1 min alveolar-capillary membrane O 2 Gas volume: ml time: 1 min pr. gradient: 1 mmhg ml/min/mmhg 159 alveolar-capillary membrane 160 Diffusion capacities V gas α A. D. (P 1 -P 2 ) T can not measure V gas = D L. (P 1 -P 2 ) D L = V gas P 1 - P 2 Diffusion capacities mean P of capillary gas Diffusion capacities Measuring: Diffusion capacities O 2 CO DO 2 DcO Affinity: Single-breath method CO = 0.3% 1 breath: TLC breath-holding: 10 sec mean P of alveolar gas 161 exhale completely 162
28 Diffusion capacities DL = V gas P 1 -P 2 DO 2 exercise DCO = V CO P A CO -P C CO DO 2 = DCO x 1.23 DO 2 Normal value: DCO = 25 ml/min/mmhg DO 2 = 31 ml/min/mmhg 163 aging pulm. edema pulm. emphysema 164 Impaired diffusion! arterial blood gas tension? mild. rest exercise alveoli PaO 2 PaCO Light micrograph 166 Key concepts 1) O 2 and CO 2 transport in blood 2) Oxyhemoglobin dissociation curve 3) P50 4) O 2 capacity 5) O 2 content (CaO 2 or CvO 2 ) 6) %saturation of Hb with O 2 (%SaO 2 ) 7) O 2 delivery (DaO 2 ) 8) O 2 consumption (VO 2 ) 9) O 2 extract! 10) CO 2 production (VCO 2 )
29 Gas transportation CaO 2 PaO 2 O 2 capacity transport of O 2 CO 2 %SaO 2 CvO 2 VCO 2 DaO 2 VO2 2 Q CaO 2 loading Dissolved in plasma dissolved O 2 2. Combination with Hemoglobin Oxyhemoglobin 171 Dissolved in plasma 3% Henry s law volume α partial pressure of that gas of dissolved gas blood 100 ml PO 2 1 mmhg dissolved O ml Po 2 in arterial blood = 100 mmhg dissolved O 2 = 0.3 ml / 100 ml.blood 172 dissolved O 2 = 0.3 ml/ 100 ml.blood O 2 consumption (at rest) = 250 ml/min Combination with Hemoglobin 97% O 2 Hemoglobin (Hb) Oxyhemoglobin If use only dissolved O 2..? cardiac output = 250 x 100 ml/min = 83.3 L/min 0.3 BUT cardiac output (at rest) = 5-6 L/min 173 Hb + O 2 HbO 2 reversible reaction total O 2 carrying capacity times 174
30 Hemoglobin 4 polypeptide chains or subunit Globin protein saturation Hemoglobin Hb + O 2 HbO 2 reversible reaction deoxyhemoglobin (reduced Hb) oxyhemoglobin Heme (iron-porphyrin compound) Hb 4 +4O 2 Hb 4 O 8 conjugated protein 1Hbmolecule = 4 subunits Heme O oxygenation (0.01 sec.) 176 Hemoglobin Gas transportation in blood saturation Hb + O 2 HbO 2 reversible reaction O 2 oxygenation Hb 4 + O 2 Hb 4 O 2 Hb 4 + O 2 Hb 4 O 4 Hb 4 + O 2 Hb 4 O 6 Hb 4 + O 2 Hb 4 O 8 dissolved O 2 /CO 2 exert pressure Binding O 2 /CO 2 (chemical reaction) Oxygen capacity Oxygen content % hemoglobin saturation Oxygen delivery Oxygen consumption Oxygen content Oxygen capacity % hemoglobin saturation oxygen content = dissolved O 2 + oxyhemoglobin oxyhemoglobin = oxygen content - dissolved O %saturation of Hb = O 2 combine with Hb with O 2 O 2 capacity of Hb (or %SaO 2 ) X
31 ย Oxygen saturation %SaO 2 refer to the amount of oxygen being carried in the red blood cells size? Htc.? Pulse Oximeter.by utilizing selected wavelengths of light to noninvasively determine the saturation of deoxygenated and oxygenated hemoglobin 181 p Physiological shunt Physiological shunt (2-4% C.O.) 1. Bronchial artery: (lung parenchyma terminal bronchiole) PAO 2 O 2 sat. = 97.4% alveolar-arterial oxygen gradient pulmonary vein 2. Coronary vein: left atrium 2-4% CO bronchial artery coronary vein O 2 sat. = 97% PaO Thebesian vein left ventricle 184 Oxygen capacity of Hb In normal: Hb 15 gm/ 100ml. blood Hb 1 gm O ml (max.) Oxygen capacity = O 2 (max.) combine with Hb in 100ml. blood = 15 x 1.34 = 20.1 ml in 100ml. blood O ml ~ 20 vol% 15gm% 185 Oxygen content CaO 2 O 2 content = totalo 2 in blood (arterial blood) = dissolved O 2 + oxyhemoglobin 0.3 ml = (PO 2 x 0.003) + (O 2 capacity) x Hb x%sao mmhg = 1.34 x ml = 20.1 ml 19.8 ml A-V shunt 100% saturation ~ 20 ml 97% saturation 97% of (20.1 ml) = 19.5 ml 186
32 O 2 saturation of Hb %SaO 2 Oxygen content = dissolved O 2 + oxyhemoglobin oxyhemoglobin = Oxygen content - dissolved O 2 O 2 capacity of Hb %saturation of Hb = O 2 combine with Hb with O X O 2 capacity of Hb (or %SaO 2 ) 187 Oxygen content CvO 2 O 2 content = totalo 2 in blood (venous blood) = dissolved O 2 + oxyhemoglobin = (PO 2 x0.003) + (O 2 capacity) x Hb x %SvO 2 O 2 combine with Hb 40 mmhg = % saturation = % of (20.1 ml) = ml = ml = 15 ml 188 DO 2 Oxygen delivery O 2 content = total O 2 in blood (arterial blood) Venous blood PO 2 = 40 mmhg in 100ml. blood Arterial blood PO 2 = 100 mmhg ~ 20 ml (in 100 ml. blood) dissolved O 2 = ml = 0.12 ml dissolved O 2 = ml = 0.3 ml Q = 5 L/min cells Oxyhemoglobin = ml ~ 15 ml Oxyhemoglobin = 19.5 ml ~ 20 ml ~ 5 ml O 2 Q x (x10) (unit: L/min) or 250 ml/min 189 (if C.O. = 5000 ml/min) 190 DO 2 CaO 2 VO 2 Oxygen consumption in 100ml. blood oxygen content Arterial blood ~ 20 ml cells ~ 5 ml Venous blood ~ 15 ml 191 O 2 content in 100ml. blood Arterial blood ~ 20 ml cells ~ 5 ml Venous blood ~ 15 ml VO 2 Q = 5 L/min in 100ml. blood cells use ~ 5 ml C.O. = 5000 ml/min 5000 x 5 ml = 250 ml 100 Oxygen consumption 192
33 Oxyhemoglobin dissociation curve dissociation separation different PO 2 O 2 dissociation release O 2 from HbO 2 Hb + O 2 HbO 2 reversible reaction O 2 dissolved O 2 oxyhemoglobin %SaO 2 PO 2 O 2 capacity of Hb (~250 PO 2 100, 90, 80 mmhg 194 %SaO 2 Oxyhemoglobin dissociation curve Sigmoidal S shape curve Arterial blood Venous blood Oxyhemoglobin dissociation curve v a O 2 50% SaO 2 pressure %SaO 2 O 2 dissociation curve p.563 Oxyhemoglobin dissociation curve a Gas transportation in blood v unloading loading associated part or flat part oxyhemoglobin binding O 2 (chemical reaction) dissociated part or steep part dissolved O 2 PO 2 %SaO O 2 O 2 O 2 O 2 O 2 198
34 Factors affecting O 2 dissociation curve 1. PCO 2 2. H + concentration 3. temperature 4. 2,3 diaphsphoglyceric acid (2,3 DPG) in RBC ( β chain of oxyhemoglobin) Shift of O 2 dissociation curve shift to the left shift to the right curve shifts reflect altered affinity of Hb for O %SaO p.565 Factors O 2 affinity to Hb release O 2 Factors P50 Shift to left Shift to right O 2 affinity to Hb Normal o C, ph 7.4 PCO 2 40 mmhg Shift to right release O 2 PCO 2 ph Bohr effect 201 P50 O 2 affinity to Hb *** 202 Effect of 2,3 diaphosphoglyceric acid (2,3 DPG) 2,3 DPG RBC HbO 2 + 2,3 DPG Hb-2,3 DPG + O 2 2,3 DPG shift to right = HbO 2 release O 2 O 2 affinity to Hb 6 gm Hb/100 ml blood hypoxia (>2-3 hrs) 2,3 DPG anemia blood (in Blood bank) hypoxemia chronic lung diseases exercise p.566
35 a tasteless odorless gas that is a byproduct of combustion the early symptoms are quite nonspecific! anemia eg. motion sickness or heat exhaustion and include prolonged headache, nausea, dizziness, and vomiting Dissolved in plasma dissolved CO 2 (6%) 2. Diffuse to RBC dissolved CO 2 in intracellular fluid react with NH 2 -group carbaminohemogloblin react with H 2 O bicarbonate 207 Dissolved in plasma dissolved CO 2 (6%) Henry s law volume α partial pressure of that gas of dissolved gas solubility-20 times : CO 2 > O 2 in blood 100 ml: PCO 2 1 mmhg 20x(0.003) = 0.06 Dissolved CO ml 208 react with H 2 O bicarbonate in plasma slow in plasma (88%)*** in RBC *** (500 times faster) in RBC CA CO 2 + H 2 O H 2 CO 3 H + + HCO 3 Carbonic acid Bicarbonate CA: carbonic anhydrase 209 react with NH 2 - (amino group) carbaminohemogloblin in plasma in plasma in RBC CO 2 +R-NH 2 RNHCOOH RNHCOO + H + plasma protein carbamino compounds (6%) in RBC CO 2 + HbO 2 carbamino hemoglobin + O 2 protein part HbCO in Hb 2 210
36 Venous blood PCO 2 = 46 mmhg dissolved CO 2 = 46 x 0.06 ml = 2.7 ml Bicarbonate carbaminohb = 50.3 ml ~ 53 ml ~ 4 ml or ml/min (if C.O. = ml/min) average 210 ml/min in 100ml. blood CO 2 Arterial blood PCO 2 = 40 mmhg dissolved CO 2 = 40 x 0.06 ml = 2.4 ml Bicarbonate = 43.8 ml carbaminohb = 2.6 ml ~ 49 ml 211 VCO 2 Carbon dioxide production Carbondioxide content Arterial blood ~ 49 ml in 100ml. blood cells ~ 4 ml Venous blood ~ 53 ml 212 in 100ml. blood Carbondioxide content Arterial blood ~ 49 ml VCO 2 cells ~ 4 ml cells release in 100ml. blood C.O. = 5000 ml/min Venous blood ~ 53 ml ~ 4 ml 5000 x 4 ml 100 = 200 ml Carbondioxide production 213 tissue dissolved CO 2 CO 2 CO 2 +R-NH 2 RNHCOOH RNHCOO + H + *** RBC capillary CO 2 + H 2 O H 2 CO 3 H + + HCO 3 O 2 dissolved CO 2 (HbCO 2 ) CO 2 + HbO 2 carbaminohb + O 2 CO 2 pulm. capillary oxygenation p.568 H 2 O Cl - Chloride shift CO 2 + H 2 O H 2 CO 3 CA HHb= reduced Hb plasma Haldane effect HCO 3 + H + H + + HbO 2 *** buffered H + Hb - + O Peripheral blood 2 de-oxygenation plasma higher ph affinity to CO Haldane effect Carbon dioxide dissociation curve PO 2 carbaminohb: HbCO 2 release CO2 Oxygenation (@ lungs) ph HbCO 2 + O 2 HbO 2 + CO 2 53 vol% 49 vol% 4vol% affinity to CO 2 expired air arterial blood venous blood dissolved CO
37 more steep *** p
αo 2 : solubility coefficient of O 2
 Version 2006 Dr. Puntarica Suwanprathes 1) Fick s law of diffusion 2) facts which limit gas transfer 3) diffusion capacity gas volume gaseous phase dissolved gas exert pressure*** Solubility of Gas C =P.
Version 2006 Dr. Puntarica Suwanprathes 1) Fick s law of diffusion 2) facts which limit gas transfer 3) diffusion capacity gas volume gaseous phase dissolved gas exert pressure*** Solubility of Gas C =P.
Respiratory System Physiology. Dr. Vedat Evren
 Respiratory System Physiology Dr. Vedat Evren Respiration Processes involved in oxygen transport from the atmosphere to the body tissues and the release and transportation of carbon dioxide produced in
Respiratory System Physiology Dr. Vedat Evren Respiration Processes involved in oxygen transport from the atmosphere to the body tissues and the release and transportation of carbon dioxide produced in
82 Respiratory Tract NOTES
 82 Respiratory Tract NOTES RESPIRATORY TRACT The respiratory tract conducts air to the lungs where gaseous exchange occurs. It is separated into air-conducting and respiratory (where gas exchange occurs)
82 Respiratory Tract NOTES RESPIRATORY TRACT The respiratory tract conducts air to the lungs where gaseous exchange occurs. It is separated into air-conducting and respiratory (where gas exchange occurs)
Section Two Diffusion of gases
 Section Two Diffusion of gases Lecture 5: Partial pressure and the composition of gasses in air. Factors affecting diffusion of gases. Ventilation perfusion ratio effect on alveolar gas concentration.
Section Two Diffusion of gases Lecture 5: Partial pressure and the composition of gasses in air. Factors affecting diffusion of gases. Ventilation perfusion ratio effect on alveolar gas concentration.
Unit II Problem 4 Physiology: Diffusion of Gases and Pulmonary Circulation
 Unit II Problem 4 Physiology: Diffusion of Gases and Pulmonary Circulation - Physical principles of gases: Pressure of a gas is caused by the movement of its molecules against a surface (more concentration
Unit II Problem 4 Physiology: Diffusion of Gases and Pulmonary Circulation - Physical principles of gases: Pressure of a gas is caused by the movement of its molecules against a surface (more concentration
Section Three Gas transport
 Section Three Gas transport Lecture 6: Oxygen transport in blood. Carbon dioxide in blood. Objectives: i. To describe the carriage of O2 in blood. ii. iii. iv. To explain the oxyhemoglobin dissociation
Section Three Gas transport Lecture 6: Oxygen transport in blood. Carbon dioxide in blood. Objectives: i. To describe the carriage of O2 in blood. ii. iii. iv. To explain the oxyhemoglobin dissociation
Physiology Unit 4 RESPIRATORY PHYSIOLOGY
 Physiology Unit 4 RESPIRATORY PHYSIOLOGY In Physiology Today Respiration External respiration ventilation gas exchange Internal respiration cellular respiration gas exchange Respiratory Cycle Inspiration
Physiology Unit 4 RESPIRATORY PHYSIOLOGY In Physiology Today Respiration External respiration ventilation gas exchange Internal respiration cellular respiration gas exchange Respiratory Cycle Inspiration
Gas exchange. Tissue cells CO2 CO 2 O 2. Pulmonary capillary. Tissue capillaries
 Gas exchange Pulmonary gas exchange Tissue gas exchange CO 2 O 2 O 2 Tissue cells CO2 CO 2 Pulmonary capillary O 2 O 2 CO 2 Tissue capillaries Physical principles of gas exchange Diffusion: continuous
Gas exchange Pulmonary gas exchange Tissue gas exchange CO 2 O 2 O 2 Tissue cells CO2 CO 2 Pulmonary capillary O 2 O 2 CO 2 Tissue capillaries Physical principles of gas exchange Diffusion: continuous
Respiration (revised 2006) Pulmonary Mechanics
 Respiration (revised 2006) Pulmonary Mechanics PUL 1. Diagram how pleural pressure, alveolar pressure, airflow, and lung volume change during a normal quiet breathing cycle. Identify on the figure the
Respiration (revised 2006) Pulmonary Mechanics PUL 1. Diagram how pleural pressure, alveolar pressure, airflow, and lung volume change during a normal quiet breathing cycle. Identify on the figure the
CHAPTER 6. Oxygen Transport. Copyright 2008 Thomson Delmar Learning
 CHAPTER 6 Oxygen Transport Normal Blood Gas Value Ranges Table 6-1 OXYGEN TRANSPORT Oxygen Dissolved in the Blood Plasma Dissolve means that the gas maintains its precise molecular structure About.003
CHAPTER 6 Oxygen Transport Normal Blood Gas Value Ranges Table 6-1 OXYGEN TRANSPORT Oxygen Dissolved in the Blood Plasma Dissolve means that the gas maintains its precise molecular structure About.003
Respiration - Human 1
 Respiration - Human 1 At the end of the lectures on respiration you should be able to, 1. Describe events in the respiratory processes 2. Discuss the mechanism of lung ventilation in human 3. Discuss the
Respiration - Human 1 At the end of the lectures on respiration you should be able to, 1. Describe events in the respiratory processes 2. Discuss the mechanism of lung ventilation in human 3. Discuss the
Chapter 17 The Respiratory System: Gas Exchange and Regulation of Breathing
 Chapter 17 The Respiratory System: Gas Exchange and Regulation of Breathing Overview of Pulmonary Circulation o Diffusion of Gases o Exchange of Oxygen and Carbon Dioxide o Transport of Gases in the Blood
Chapter 17 The Respiratory System: Gas Exchange and Regulation of Breathing Overview of Pulmonary Circulation o Diffusion of Gases o Exchange of Oxygen and Carbon Dioxide o Transport of Gases in the Blood
Lesson 9.1: The Importance of an Organ Delivery System
 Lesson 9.1: The Importance of an Organ Delivery System Animals require a continuous supply of oxygen (O 2 ) for cellular respiration, and they must expel carbon dioxide (CO 2 ), the waste product of this
Lesson 9.1: The Importance of an Organ Delivery System Animals require a continuous supply of oxygen (O 2 ) for cellular respiration, and they must expel carbon dioxide (CO 2 ), the waste product of this
 Question 1: Define vital capacity. What is its significance? Vital capacity is the maximum volume of air that can be exhaled after a maximum inspiration. It is about 3.5 4.5 litres in the human body. It
Question 1: Define vital capacity. What is its significance? Vital capacity is the maximum volume of air that can be exhaled after a maximum inspiration. It is about 3.5 4.5 litres in the human body. It
I Physical Principles of Gas Exchange
 Respiratory Gases Exchange Dr Badri Paudel, M.D. 2 I Physical Principles of Gas Exchange 3 Partial pressure The pressure exerted by each type of gas in a mixture Diffusion of gases through liquids Concentration
Respiratory Gases Exchange Dr Badri Paudel, M.D. 2 I Physical Principles of Gas Exchange 3 Partial pressure The pressure exerted by each type of gas in a mixture Diffusion of gases through liquids Concentration
Respiratory System. Prepared by: Dorota Marczuk-Krynicka, MD, PhD
 Respiratory System Prepared by: Dorota Marczuk-Krynicka, MD, PhD Lungs: Ventilation Perfusion Gas Exchange - Diffusion 1. Airways and Airway Resistance (AWR) 2. Mechanics of Breathing and Lung (Elastic)
Respiratory System Prepared by: Dorota Marczuk-Krynicka, MD, PhD Lungs: Ventilation Perfusion Gas Exchange - Diffusion 1. Airways and Airway Resistance (AWR) 2. Mechanics of Breathing and Lung (Elastic)
Chapter 13 The Respiratory System
 Chapter 13 The Respiratory System by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Atmosphere Tissue cell External respiration Alveoli of lungs 1 Ventilation or gas exchange between the atmosphere
Chapter 13 The Respiratory System by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Atmosphere Tissue cell External respiration Alveoli of lungs 1 Ventilation or gas exchange between the atmosphere
Chapter 16 Respiratory System
 Introduction Chapter 16 Respiratory System The respiratory system consists of tubes that filter incoming air and transport it to alveoli where gases are exchanged. Think pair share: what organs are associated
Introduction Chapter 16 Respiratory System The respiratory system consists of tubes that filter incoming air and transport it to alveoli where gases are exchanged. Think pair share: what organs are associated
Collin County Community College. Lung Physiology
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 9 Respiratory System 1 Lung Physiology Factors affecting Ventillation 1. Airway resistance Flow = Δ P / R Most resistance is encountered
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 9 Respiratory System 1 Lung Physiology Factors affecting Ventillation 1. Airway resistance Flow = Δ P / R Most resistance is encountered
Introduction. Respiration. Chapter 10. Objectives. Objectives. The Respiratory System
 Introduction Respiration Chapter 10 The Respiratory System Provides a means of gas exchange between the environment and the body Plays a role in the regulation of acidbase balance during exercise Objectives
Introduction Respiration Chapter 10 The Respiratory System Provides a means of gas exchange between the environment and the body Plays a role in the regulation of acidbase balance during exercise Objectives
RESPIRATORY GAS EXCHANGE
 RESPIRATORY GAS EXCHANGE Alveolar PO 2 = 105 mmhg; Pulmonary artery PO 2 = 40 mmhg PO 2 gradient across respiratory membrane 65 mmhg (105 mmhg 40 mmhg) Results in pulmonary vein PO 2 ~100 mmhg Partial
RESPIRATORY GAS EXCHANGE Alveolar PO 2 = 105 mmhg; Pulmonary artery PO 2 = 40 mmhg PO 2 gradient across respiratory membrane 65 mmhg (105 mmhg 40 mmhg) Results in pulmonary vein PO 2 ~100 mmhg Partial
AIIMS, New Delhi. Dr. K. K. Deepak, Prof. & HOD, Physiology AIIMS, New Delhi Dr. Geetanjali Bade, Asst. Professor AIIMS, New Delhi
 Course : PG Pathshala-Biophysics Paper 13 : Physiological Biophysics Module 17 : Gas transport and pulmonary circulation Principal Investigator: Co-Principal Investigator: Paper Coordinator: Content Writer:
Course : PG Pathshala-Biophysics Paper 13 : Physiological Biophysics Module 17 : Gas transport and pulmonary circulation Principal Investigator: Co-Principal Investigator: Paper Coordinator: Content Writer:
Table of Contents. By Adam Hollingworth
 By Adam Hollingworth Table of Contents Oxygen Cascade... 2 Diffusion... 2 Laws of Diffusion... 2 Diffusion & Perfusion Limitations... 3 Oxygen Uptake Along Pulmon Capillary... 4 Measurement of Diffusing
By Adam Hollingworth Table of Contents Oxygen Cascade... 2 Diffusion... 2 Laws of Diffusion... 2 Diffusion & Perfusion Limitations... 3 Oxygen Uptake Along Pulmon Capillary... 4 Measurement of Diffusing
Respiratory physiology II.
 Respiratory physiology II. Learning objectives: 29. Pulmonary gas exchange. 30. Oxygen transport in the blood. 31. Carbon-dioxide transport in the blood. 1 Pulmonary gas exchange The transport mechanism
Respiratory physiology II. Learning objectives: 29. Pulmonary gas exchange. 30. Oxygen transport in the blood. 31. Carbon-dioxide transport in the blood. 1 Pulmonary gas exchange The transport mechanism
Breathing: The normal rate is about 14 to 20 times a minute. Taking in of air is called Inspiration and the forcing out of air is called Expiration.
 Biology 12 Respiration Divisions of Respiration Breathing: entrance and exit of air into and out of the lungs External Respiration: exchange of gases(o2 and CO2) between air (in alveoli) and blood Internal
Biology 12 Respiration Divisions of Respiration Breathing: entrance and exit of air into and out of the lungs External Respiration: exchange of gases(o2 and CO2) between air (in alveoli) and blood Internal
respiratory cycle. point in the volumes: 500 milliliters. for men. expiration, up to 1200 milliliters extra makes breathing Respiratory
 10 II. RESPIRATORY VOLUMES, CAPACITIES & PULMONARY FUNCTION TESTS Respiratory volume is the term used for various volumes of air moved by or associated with the lungs at a given point in the respiratory
10 II. RESPIRATORY VOLUMES, CAPACITIES & PULMONARY FUNCTION TESTS Respiratory volume is the term used for various volumes of air moved by or associated with the lungs at a given point in the respiratory
Chapter 13 The Respiratory System
 VI edit Pag 451-499 Chapter 13 The Respiratory System V edit. Pag 459-509 Tissue cell Alveoli of lungs Atmosphere 1 External respiration Ventilation or gas exchange between the atmosphere and air sacs
VI edit Pag 451-499 Chapter 13 The Respiratory System V edit. Pag 459-509 Tissue cell Alveoli of lungs Atmosphere 1 External respiration Ventilation or gas exchange between the atmosphere and air sacs
Chapter 11: Respiratory System Review Assignment
 Name: Date: Mark: / 45 Chapter 11: Respiratory System Review Assignment Multiple Choice = 45 Marks Identify the choice that best completes the statement or answers the question. 1. Which of the following
Name: Date: Mark: / 45 Chapter 11: Respiratory System Review Assignment Multiple Choice = 45 Marks Identify the choice that best completes the statement or answers the question. 1. Which of the following
Respiratory System Review
 KEY THIS TEST WILL BE COMPLETED IN ONE CLASS PERIOD MONDAY, MARCH 10. 2014 Respiratory System Review Name A. Directions: Fill in the blank with the appropriate vocabulary word or words (several examples
KEY THIS TEST WILL BE COMPLETED IN ONE CLASS PERIOD MONDAY, MARCH 10. 2014 Respiratory System Review Name A. Directions: Fill in the blank with the appropriate vocabulary word or words (several examples
Gases and Respiration. Respiration Overview I
 Respiration Overview I Respiration Overview II Gas Laws Equation of State: PV = nrt Same volumes of different gases have same # of molecules BTPS: body temp, atmospheric pressure, saturated ATPS: ambient
Respiration Overview I Respiration Overview II Gas Laws Equation of State: PV = nrt Same volumes of different gases have same # of molecules BTPS: body temp, atmospheric pressure, saturated ATPS: ambient
Alveolus and Respiratory Membrane
 Alveolus and Respiratory Membrane thin membrane where gas exchange occurs in the lungs, simple squamous epithelium (Squamous cells have the appearance of thin, flat plates. They fit closely together in
Alveolus and Respiratory Membrane thin membrane where gas exchange occurs in the lungs, simple squamous epithelium (Squamous cells have the appearance of thin, flat plates. They fit closely together in
Respiratory system & exercise. Dr. Rehab F Gwada
 Respiratory system & exercise Dr. Rehab F Gwada Objectives of lecture Outline the major anatomical components & important functions of the respiratory system. Describe the mechanics of ventilation. List
Respiratory system & exercise Dr. Rehab F Gwada Objectives of lecture Outline the major anatomical components & important functions of the respiratory system. Describe the mechanics of ventilation. List
Human Biology Respiratory System
 Human Biology Respiratory System Respiratory System Responsible for process of breathing Works in cooperation with Circulatory system Three types: 1. Internal Respiration 2. External Respiration 3. Cellular
Human Biology Respiratory System Respiratory System Responsible for process of breathing Works in cooperation with Circulatory system Three types: 1. Internal Respiration 2. External Respiration 3. Cellular
By: Aseel Jamil Al-twaijer. Lec : physical principles of gas exchange
 By: Aseel Jamil Al-twaijer Lec : physical principles of gas exchange Date:30 /10/2017 this lecture is about the exchange of gases between the blood and the alveoli. I might add some external definitions
By: Aseel Jamil Al-twaijer Lec : physical principles of gas exchange Date:30 /10/2017 this lecture is about the exchange of gases between the blood and the alveoli. I might add some external definitions
alveoli Chapter 42. Gas Exchange elephant seals gills AP Biology
 alveoli Chapter 42. Gas Exchange gills elephant seals Gas exchange O 2 & CO 2 exchange exchange between environment & cells provides O 2 for aerobic cellular respiration need moist membrane need high
alveoli Chapter 42. Gas Exchange gills elephant seals Gas exchange O 2 & CO 2 exchange exchange between environment & cells provides O 2 for aerobic cellular respiration need moist membrane need high
IV. FROM AQUATIC TO ATMOSPHERIC BREATHING: THE TRACHEA & THE LUNG
 GAS EXCHANGE AND TRANSPORT I. INTRODUCTION: Heterotrophs oxidize carbon cmpds using O 2 to generate CO 2 & H 2 O. This is cellular respiration II. HOW GAS ENTERS A CELL A. The composition of air: 79% N
GAS EXCHANGE AND TRANSPORT I. INTRODUCTION: Heterotrophs oxidize carbon cmpds using O 2 to generate CO 2 & H 2 O. This is cellular respiration II. HOW GAS ENTERS A CELL A. The composition of air: 79% N
Gas Exchange Respiratory Systems
 alveoli gills Gas Exchange Respiratory Systems elephant seals 2008-2009 Why do we need a respiratory system? respiration for respiration Need O 2 in for aerobic cellular respiration make ATP Need CO 2
alveoli gills Gas Exchange Respiratory Systems elephant seals 2008-2009 Why do we need a respiratory system? respiration for respiration Need O 2 in for aerobic cellular respiration make ATP Need CO 2
Chapter 23. Gas Exchange and Transportation
 Chapter 23 Gas Exchange and Transportation What is air? Mixture of gasses 78.6 % nitrogen 20.9% oxygen 0.04% carbon dioxide 0 4% water vapor depending on temperature and humidity and minor gases argon,
Chapter 23 Gas Exchange and Transportation What is air? Mixture of gasses 78.6 % nitrogen 20.9% oxygen 0.04% carbon dioxide 0 4% water vapor depending on temperature and humidity and minor gases argon,
(Slide 1) Lecture Notes: Respiratory System
 (Slide 1) Lecture Notes: Respiratory System I. (Slide 2) The Respiratory Tract A) Major structures and regions of the respiratory Tract/Route INTO body 1) nose 2) nasal cavity 3) pharynx 4) glottis 5)
(Slide 1) Lecture Notes: Respiratory System I. (Slide 2) The Respiratory Tract A) Major structures and regions of the respiratory Tract/Route INTO body 1) nose 2) nasal cavity 3) pharynx 4) glottis 5)
PICU Resident Self-Study Tutorial The Basic Physics of Oxygen Transport. I was told that there would be no math!
 Physiology of Oxygen Transport PICU Resident Self-Study Tutorial I was told that there would be no math! INTRODUCTION Christopher Carroll, MD Although cells rely on oxygen for aerobic metabolism and viability,
Physiology of Oxygen Transport PICU Resident Self-Study Tutorial I was told that there would be no math! INTRODUCTION Christopher Carroll, MD Although cells rely on oxygen for aerobic metabolism and viability,
AP Biology. Chapter 42. Gas Exchange. Optimizing gas exchange. Gas exchange. Gas exchange in many forms. Evolution of gas exchange structures
 alveoli Chapter 42. Gas Exchange gills elephant seals Gas exchange & C exchange exchange between environment & cells provides for aerobic cellular respiration need moist membrane need high surface area
alveoli Chapter 42. Gas Exchange gills elephant seals Gas exchange & C exchange exchange between environment & cells provides for aerobic cellular respiration need moist membrane need high surface area
GAS EXCHANGE & PHYSIOLOGY
 GAS EXCHANGE & PHYSIOLOGY Atmospheric Pressure Intra-Alveolar Pressure Inspiration 760 mm HG at Sea Level (= 1 atm) Pressure due to gases (N2, O2, CO2, Misc.) Pressure inside the alveolus (air sac) Phrenic
GAS EXCHANGE & PHYSIOLOGY Atmospheric Pressure Intra-Alveolar Pressure Inspiration 760 mm HG at Sea Level (= 1 atm) Pressure due to gases (N2, O2, CO2, Misc.) Pressure inside the alveolus (air sac) Phrenic
Breathing oxygenates the blood to allow food to be respired
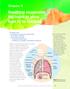 Chapter 6 Breathing oxygenates the blood to allow food to be respired This chapter covers: the structure of the human gas exchange system the mechanism of breathing gas exchange in the alveoli the concept
Chapter 6 Breathing oxygenates the blood to allow food to be respired This chapter covers: the structure of the human gas exchange system the mechanism of breathing gas exchange in the alveoli the concept
Respiratory System. Part 2
 Respiratory System Part 2 Respiration Exchange of gases between air and body cells Three steps 1. Ventilation 2. External respiration 3. Internal respiration Ventilation Pulmonary ventilation consists
Respiratory System Part 2 Respiration Exchange of gases between air and body cells Three steps 1. Ventilation 2. External respiration 3. Internal respiration Ventilation Pulmonary ventilation consists
AP Biology. Gas Exchange Respiratory Systems. Gas exchange. Why do we need a respiratory system? Optimizing gas exchange. Gas exchange in many forms
 alveoli Gas Exchange Respiratory Systems gills elephant seals 2008-2009 Why do we need a respiratory system? Need O 2 in food respiration for respiration for aerobic cellular respiration make ATP Need
alveoli Gas Exchange Respiratory Systems gills elephant seals 2008-2009 Why do we need a respiratory system? Need O 2 in food respiration for respiration for aerobic cellular respiration make ATP Need
Lung Volumes and Ventilation
 Respiratory System ssrisuma@rics.bwh.harvard.edu Lung Volumes and Ventilation Minute ventilation Volume of an inspired or expired air per minute = tidal volume (V T ) x respiratory rate Dead space ventilation
Respiratory System ssrisuma@rics.bwh.harvard.edu Lung Volumes and Ventilation Minute ventilation Volume of an inspired or expired air per minute = tidal volume (V T ) x respiratory rate Dead space ventilation
Physical Chemistry of Gases: Gas Exchange Linda Costanzo, Ph.D.
 Physical Chemistry of Gases: Gas Exchange Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Application of the gas laws to pulmonary physiology. 2. How to
Physical Chemistry of Gases: Gas Exchange Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Application of the gas laws to pulmonary physiology. 2. How to
Outline - Respiratory System. Function of the respiratory system Parts of the respiratory system Mechanics of breathing Regulation of breathing
 Respiratory system Function Outline - Respiratory System I. II. III. IV. Respiratory System The function of the respiratory system is to bring in oxygen to the body and remove carbon dioxide. Function
Respiratory system Function Outline - Respiratory System I. II. III. IV. Respiratory System The function of the respiratory system is to bring in oxygen to the body and remove carbon dioxide. Function
Assignments for Life Processes(Respiration)
 Assignments for Life Processes(Respiration) 1 Question 1 Why do organisms need food? Organisms need food for obtaining energy to perform the vital functions. Question 2 What is a respiratory substrate?
Assignments for Life Processes(Respiration) 1 Question 1 Why do organisms need food? Organisms need food for obtaining energy to perform the vital functions. Question 2 What is a respiratory substrate?
Lung Volumes and Capacities
 Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
Lung Volumes and Capacities Normally the volume of air entering the lungs during a single inspiration is approximately equal to the volume leaving on the subsequent expiration and is called the tidal volume.
RESPIRATORY PHYSIOLOGY. Anaesthesiology Block 18 (GNK 586) Prof Pierre Fourie
 RESPIRATORY PHYSIOLOGY Anaesthesiology Block 18 (GNK 586) Prof Pierre Fourie Outline Ventilation Diffusion Perfusion Ventilation-Perfusion relationship Work of breathing Control of Ventilation 2 This image
RESPIRATORY PHYSIOLOGY Anaesthesiology Block 18 (GNK 586) Prof Pierre Fourie Outline Ventilation Diffusion Perfusion Ventilation-Perfusion relationship Work of breathing Control of Ventilation 2 This image
HCO - 3 H 2 CO 3 CO 2 + H H H + Breathing rate is regulated by blood ph and C02. CO2 and Bicarbonate act as a ph Buffer in the blood
 Breathing rate is regulated by blood ph and C02 breathing reduces plasma [CO2]; plasma [CO2] increases breathing. When C02 levels are high, breating rate increases to blow off C02 In low C02 conditions,
Breathing rate is regulated by blood ph and C02 breathing reduces plasma [CO2]; plasma [CO2] increases breathing. When C02 levels are high, breating rate increases to blow off C02 In low C02 conditions,
RESPIRATORY REGULATION DURING EXERCISE
 RESPIRATORY REGULATION DURING EXERCISE Respiration Respiration delivery of oxygen to and removal of carbon dioxide from the tissue External respiration ventilation and exchange of gases in the lung Internal
RESPIRATORY REGULATION DURING EXERCISE Respiration Respiration delivery of oxygen to and removal of carbon dioxide from the tissue External respiration ventilation and exchange of gases in the lung Internal
Oxygen and Carbon dioxide Transport. Dr. Laila Al-Dokhi
 Oxygen and Carbon dioxide Transport Dr. Laila Al-Dokhi Objectives 1. Understand the forms of oxygen transport in the blood, the importance of each. 2. Differentiate between O2 capacity, O2 content and
Oxygen and Carbon dioxide Transport Dr. Laila Al-Dokhi Objectives 1. Understand the forms of oxygen transport in the blood, the importance of each. 2. Differentiate between O2 capacity, O2 content and
Pulmonary Circulation Linda Costanzo Ph.D.
 Pulmonary Circulation Linda Costanzo Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The differences between pressures in the pulmonary and systemic circulations. 2. How
Pulmonary Circulation Linda Costanzo Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The differences between pressures in the pulmonary and systemic circulations. 2. How
2. State the volume of air remaining in the lungs after a normal breathing.
 CLASS XI BIOLOGY Breathing And Exchange of Gases 1. Define vital capacity. What is its significance? Answer: Vital Capacity (VC): The maximum volume of air a person can breathe in after a forced expiration.
CLASS XI BIOLOGY Breathing And Exchange of Gases 1. Define vital capacity. What is its significance? Answer: Vital Capacity (VC): The maximum volume of air a person can breathe in after a forced expiration.
The Physiologic Basis of DLCO testing. Brian Graham Division of Respirology, Critical Care and Sleep Medicine University of Saskatchewan
 The Physiologic Basis of DLCO testing Brian Graham Division of Respirology, Critical Care and Sleep Medicine University of Saskatchewan Objectives Review gas transport from inhaled gas to the rest of the
The Physiologic Basis of DLCO testing Brian Graham Division of Respirology, Critical Care and Sleep Medicine University of Saskatchewan Objectives Review gas transport from inhaled gas to the rest of the
Chapter 23. Gas Exchange and Transportation
 Chapter 23 Gas Exchange and Transportation What is air? Mixture of gasses 78.6 % nitrogen 20.9% oxygen 0.04% carbon dioxide 0 4% water vapor depending on temperature and humidity other minor gases argon,
Chapter 23 Gas Exchange and Transportation What is air? Mixture of gasses 78.6 % nitrogen 20.9% oxygen 0.04% carbon dioxide 0 4% water vapor depending on temperature and humidity other minor gases argon,
Respiration. The ins and outs
 Respiration The ins and outs Functions 1. To bring O 2 into the body and transfer it to the blood stream 2. To remove CO 2 Circulation and respiration work together to achieve these functions Why Do We
Respiration The ins and outs Functions 1. To bring O 2 into the body and transfer it to the blood stream 2. To remove CO 2 Circulation and respiration work together to achieve these functions Why Do We
Blood gas adventures at various altitudes. Friedrich Luft Experimental and Clinical Research Center, Berlin-Buch
 Blood gas adventures at various altitudes Friedrich Luft Experimental and Clinical Research Center, Berlin-Buch Mount Everest 8848 M Any point in bird watching here? Respiration is gas exchange: the process
Blood gas adventures at various altitudes Friedrich Luft Experimental and Clinical Research Center, Berlin-Buch Mount Everest 8848 M Any point in bird watching here? Respiration is gas exchange: the process
Gaseous exchange. Grade 11
 z Gaseous exchange Grade 11 z Terminology 1. Breathing 2. Gaseous exchange 3. Diffusion 4. Spongy mesophyll cells 5. Tracheae 6. Gills 7. Alveoli 8. Larynx 9. Diaphragm 10. Endothelium 1. Pleura 2. Squamous
z Gaseous exchange Grade 11 z Terminology 1. Breathing 2. Gaseous exchange 3. Diffusion 4. Spongy mesophyll cells 5. Tracheae 6. Gills 7. Alveoli 8. Larynx 9. Diaphragm 10. Endothelium 1. Pleura 2. Squamous
Chapter 23: Respiratory System
 Chapter 23: Respiratory System I. Functions of the Respiratory System A. List and describe the five major functions of the respiratory system: 1. 2. 3. 4. 5. II. Anatomy and Histology of the Respiratory
Chapter 23: Respiratory System I. Functions of the Respiratory System A. List and describe the five major functions of the respiratory system: 1. 2. 3. 4. 5. II. Anatomy and Histology of the Respiratory
CHAPTER 17 BREATHING AND EXCHANGE OF GASES
 268 BIOLOGY CHAPTER 17 BREATHING AND EXCHANGE OF GASES 17.1 Respiratory Organs 17.2 Mechanism of Breathing 17.3 Exchange of Gases 17.4 Transport of Gases 17.5 Regulation of Respiration 17.6 Disorders of
268 BIOLOGY CHAPTER 17 BREATHING AND EXCHANGE OF GASES 17.1 Respiratory Organs 17.2 Mechanism of Breathing 17.3 Exchange of Gases 17.4 Transport of Gases 17.5 Regulation of Respiration 17.6 Disorders of
RESPIRATION III SEMESTER BOTANY MODULE II
 III SEMESTER BOTANY MODULE II RESPIRATION Lung Capacities and Volumes Tidal volume (TV) air that moves into and out of the lungs with each breath (approximately 500 ml) Inspiratory reserve volume (IRV)
III SEMESTER BOTANY MODULE II RESPIRATION Lung Capacities and Volumes Tidal volume (TV) air that moves into and out of the lungs with each breath (approximately 500 ml) Inspiratory reserve volume (IRV)
Pulmonary Circulation
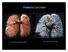 Pulmonary Circulation resin cast of pulmonary arteries resin cast of pulmonary veins Blood Flow to the Lungs Pulmonary Circulation Systemic Circulation Blood supply to the conducting zone provided by the
Pulmonary Circulation resin cast of pulmonary arteries resin cast of pulmonary veins Blood Flow to the Lungs Pulmonary Circulation Systemic Circulation Blood supply to the conducting zone provided by the
VENTILATION AND PERFUSION IN HEALTH AND DISEASE. Dr.HARIPRASAD VS
 VENTILATION AND PERFUSION IN HEALTH AND DISEASE Dr.HARIPRASAD VS Ventilation Total ventilation - total rate of air flow in and out of the lung during normal tidal breathing. Alveolar ventilation -represents
VENTILATION AND PERFUSION IN HEALTH AND DISEASE Dr.HARIPRASAD VS Ventilation Total ventilation - total rate of air flow in and out of the lung during normal tidal breathing. Alveolar ventilation -represents
I. Gas Exchange Respiratory Surfaces Respiratory Surface:
 I. Gas Exchange Respiratory Surfaces Respiratory Surface: Common characteristics of respiratory surfaces: a) Moist: allows for the RAPID diffusion of dissolved gasses across its surface. Whereas the respiratory
I. Gas Exchange Respiratory Surfaces Respiratory Surface: Common characteristics of respiratory surfaces: a) Moist: allows for the RAPID diffusion of dissolved gasses across its surface. Whereas the respiratory
CHAPTER 3: The respiratory system
 CHAPTER 3: The respiratory system Practice questions - text book pages 56-58 1) When the inspiratory muscles contract, which one of the following statements is true? a. the size of the thoracic cavity
CHAPTER 3: The respiratory system Practice questions - text book pages 56-58 1) When the inspiratory muscles contract, which one of the following statements is true? a. the size of the thoracic cavity
Then the partial pressure of oxygen is x 760 = 160 mm Hg
 1 AP Biology March 2008 Respiration Chapter 42 Gas exchange occurs across specialized respiratory surfaces. 1) Gas exchange: the uptake of molecular oxygen (O2) from the environment and the discharge of
1 AP Biology March 2008 Respiration Chapter 42 Gas exchange occurs across specialized respiratory surfaces. 1) Gas exchange: the uptake of molecular oxygen (O2) from the environment and the discharge of
Respiratory Physiology. ED Primary Teaching
 Respiratory Physiology ED Primary Teaching Functions of the respiratory system Gas exchange with O2 and CO2 Surfactant production Defence - IgA and macrophages Filer - pollutants and thromboembolism Metabolises
Respiratory Physiology ED Primary Teaching Functions of the respiratory system Gas exchange with O2 and CO2 Surfactant production Defence - IgA and macrophages Filer - pollutants and thromboembolism Metabolises
Fysiologie van de ademhaling - gasuitwisseling
 What you will learn in this lecture... Lessenreeks co s 014-015 Fysiologie van de ademhaling - gasuitwisseling Professor Dr. Steffen Rex Department of Anesthesiology University Hospitals Leuven Department
What you will learn in this lecture... Lessenreeks co s 014-015 Fysiologie van de ademhaling - gasuitwisseling Professor Dr. Steffen Rex Department of Anesthesiology University Hospitals Leuven Department
CHAPTER 3: The cardio-respiratory system
 : The cardio-respiratory system Exam style questions - text book pages 44-45 1) Describe the structures involved in gaseous exchange in the lungs and explain how gaseous exchange occurs within this tissue.
: The cardio-respiratory system Exam style questions - text book pages 44-45 1) Describe the structures involved in gaseous exchange in the lungs and explain how gaseous exchange occurs within this tissue.
Respiratory Physiology Gaseous Exchange
 Respiratory Physiology Gaseous Exchange Session Objectives. What you will cover Basic anatomy of the lung including airways Breathing movements Lung volumes and capacities Compliance and Resistance in
Respiratory Physiology Gaseous Exchange Session Objectives. What you will cover Basic anatomy of the lung including airways Breathing movements Lung volumes and capacities Compliance and Resistance in
P215 Respiratory System, Part 2
 P15 Respiratory System, Part Gas Exchange Oxygen and Carbon Dioxide constant need for oxygen constant production of carbon dioxide exchange (and movement) lung alveoli pulmonary arteries pulmonary capillaries
P15 Respiratory System, Part Gas Exchange Oxygen and Carbon Dioxide constant need for oxygen constant production of carbon dioxide exchange (and movement) lung alveoli pulmonary arteries pulmonary capillaries
Recitation question # 05
 Recitation and Lab # 05 The goal of this recitations / labs is to review material related to the CV and respiratory lectures for the second test of this course. Info required to answer this recitation
Recitation and Lab # 05 The goal of this recitations / labs is to review material related to the CV and respiratory lectures for the second test of this course. Info required to answer this recitation
UNIT 9 - RESPIRATORY SYSTEM LECTURE NOTES
 UNIT 9 - RESPIRATORY SYSTEM LECTURE NOTES 9.01 GENERAL FUNCTIONS OF THE RESPIRATORY SYSTEM A. Brings oxygenated air to the alveoli B. Removes air containing carbon dioxide C. Filters, warms, and humidifies
UNIT 9 - RESPIRATORY SYSTEM LECTURE NOTES 9.01 GENERAL FUNCTIONS OF THE RESPIRATORY SYSTEM A. Brings oxygenated air to the alveoli B. Removes air containing carbon dioxide C. Filters, warms, and humidifies
system. and then into the tissues. Diffusion of wastes such as Carbon Dioxide from tissues into blood and out of blood into the lungs.
 Respiratory System 1.Exchange Why do of we gases breathe? into the Think blood of all and the tissues. reasons Diffusion why we of Oxygen need a respiratory into blood from the lungs system. and then into
Respiratory System 1.Exchange Why do of we gases breathe? into the Think blood of all and the tissues. reasons Diffusion why we of Oxygen need a respiratory into blood from the lungs system. and then into
Respiratory Lecture Test Questions Set 3
 Respiratory Lecture Test Questions Set 3 1. The pressure of a gas: a. is inversely proportional to its volume b. is unaffected by temperature changes c. is directly proportional to its volume d. does not
Respiratory Lecture Test Questions Set 3 1. The pressure of a gas: a. is inversely proportional to its volume b. is unaffected by temperature changes c. is directly proportional to its volume d. does not
Physiology of Respiration
 Physiology of Respiration External Respiration = pulmonary ventilation breathing involves 2 processes: inspiration expiration Inspiration an active process involves contraction of diaphragm innervated
Physiology of Respiration External Respiration = pulmonary ventilation breathing involves 2 processes: inspiration expiration Inspiration an active process involves contraction of diaphragm innervated
2.1.1 List the principal structures of the
 physiology 2.1.1 List the principal structures of the The principle structures of the respiratory are: Nose/Mouth used for inhalation of oxygen-rich air and expelling carbon dioxide rich air Pharynx -
physiology 2.1.1 List the principal structures of the The principle structures of the respiratory are: Nose/Mouth used for inhalation of oxygen-rich air and expelling carbon dioxide rich air Pharynx -
Circulatory And Respiration
 Circulatory And Respiration Composition Of Blood Blood Heart 200mmHg 120mmHg Aorta Artery Arteriole 50mmHg Capillary Bed Venule Vein Vena Cava Heart Differences Between Arteries and Veins Veins transport
Circulatory And Respiration Composition Of Blood Blood Heart 200mmHg 120mmHg Aorta Artery Arteriole 50mmHg Capillary Bed Venule Vein Vena Cava Heart Differences Between Arteries and Veins Veins transport
Essential Skills Course Acute Care Module. Respiratory Day 2 (Arterial Blood Gases) Pre course Workbook
 Essential Skills Course Acute Care Module Respiratory Day 2 (Arterial Blood Gases) Pre course Workbook Acknowledgements This pre course workbook has been complied and updated with reference to the original
Essential Skills Course Acute Care Module Respiratory Day 2 (Arterial Blood Gases) Pre course Workbook Acknowledgements This pre course workbook has been complied and updated with reference to the original
Respiration. Chapter 39
 Respiration Chapter 39 Impacts, Issues Up in Smoke Smoking immobilizes ciliated cells and kills white blood cells that defend the respiratory system; highly addictive nicotine discourages quitting 39.1
Respiration Chapter 39 Impacts, Issues Up in Smoke Smoking immobilizes ciliated cells and kills white blood cells that defend the respiratory system; highly addictive nicotine discourages quitting 39.1
Chapter 15. Lecture and Animation Outline
 Chapter 15 Lecture and Animation Outline To run the animations you must be in Slideshow View. Use the buttons on the animation to play, pause, and turn audio/text on or off. Please Note: Once you have
Chapter 15 Lecture and Animation Outline To run the animations you must be in Slideshow View. Use the buttons on the animation to play, pause, and turn audio/text on or off. Please Note: Once you have
Then the partial pressure of oxygen is. b) Gases will diffuse down a pressure gradient across a respiratory surface if it is: i) permeable ii) moist
 1 AP Biology March 2008 Respiration Chapter 42 Gas exchange occurs across specialized respiratory surfaces. 1) Gas exchange: Relies on the diffusion of gases down pressure gradients. At sea level, atmosphere
1 AP Biology March 2008 Respiration Chapter 42 Gas exchange occurs across specialized respiratory surfaces. 1) Gas exchange: Relies on the diffusion of gases down pressure gradients. At sea level, atmosphere
Life 24 - Blood and Circulation Raven & Johnson Ch 52 & 53 (parts)
 1 Life 24 - Blood and Circulation Raven & Johnson Ch 52 & 53 (parts) Objectives 1: Understand the importance of oxygen carrier molecules in respiration 2: Describe the characteristics and locations of
1 Life 24 - Blood and Circulation Raven & Johnson Ch 52 & 53 (parts) Objectives 1: Understand the importance of oxygen carrier molecules in respiration 2: Describe the characteristics and locations of
RESPIRATORY SYSTEM OF RABBIT:
 RESPIRATION The term respiration means exchange of gases (particularly oxygen and carbon dioxide) between an organism and its medium. Physiologically, the term respiration may be defined as a biochemical
RESPIRATION The term respiration means exchange of gases (particularly oxygen and carbon dioxide) between an organism and its medium. Physiologically, the term respiration may be defined as a biochemical
Section 01: The Pulmonary System
 Section 01: The Pulmonary System Chapter 12 Pulmonary Structure and Function Chapter 13 Gas Exchange and Transport Chapter 14 Dynamics of Pulmonary Ventilation HPHE 6710 Exercise Physiology II Dr. Cheatham
Section 01: The Pulmonary System Chapter 12 Pulmonary Structure and Function Chapter 13 Gas Exchange and Transport Chapter 14 Dynamics of Pulmonary Ventilation HPHE 6710 Exercise Physiology II Dr. Cheatham
Pco2 *20times = 0.6, 2.4, so the co2 carried in the arterial blood in dissolved form is more than the o2 because of its solubility.
 Physiology, sheet #9 Oxygen, is first dissolved in the plasma and the cytosol of the rbc, we have around blood constitutes 7% of our body weight, oxygen, in the capillaries is present in the rbc s and
Physiology, sheet #9 Oxygen, is first dissolved in the plasma and the cytosol of the rbc, we have around blood constitutes 7% of our body weight, oxygen, in the capillaries is present in the rbc s and
Respiratory Anatomy and Physiology. Respiratory Anatomy. Function of the Respiratory System
 Respiratory Anatomy and Physiology Michaela Dixon Clinical Development Nurse PICU BRHFC Respiratory Anatomy Function of the Respiratory System - In conjunction with the cardiovascular system, to supply
Respiratory Anatomy and Physiology Michaela Dixon Clinical Development Nurse PICU BRHFC Respiratory Anatomy Function of the Respiratory System - In conjunction with the cardiovascular system, to supply
1 CHAPTER 17 BREATHING AND EXCHANGE OF GASES https://biologyaipmt.com/
 1 CHAPTER 17 BREATHING AND EXCHANGE OF GASES https://biologyaipmt.com/ CHAPTER 17 BREATHING AND EXCHANGE OF GASES Oxygen (O2) is utilised by the organisms to indirectly break down nutrient molecules like
1 CHAPTER 17 BREATHING AND EXCHANGE OF GASES https://biologyaipmt.com/ CHAPTER 17 BREATHING AND EXCHANGE OF GASES Oxygen (O2) is utilised by the organisms to indirectly break down nutrient molecules like
GASEOUS EXCHANGE 17 JULY 2013
 GASEOUS EXCHANGE 17 JULY 2013 Lesson Description In this lesson we: Discuss what is gaseous exchange? Consider requirements of an efficient gaseous exchange surface. Look at diversity in gas exchange systems.
GASEOUS EXCHANGE 17 JULY 2013 Lesson Description In this lesson we: Discuss what is gaseous exchange? Consider requirements of an efficient gaseous exchange surface. Look at diversity in gas exchange systems.
Respiratory system. Premedical - Biology
 Respiratory system Premedical - Biology Composition of atmosphere Nitrogen (N 2 ) 840 ppmv (78.084%) Oxygen (O 2 ) 209,460 ppmv (20.946%) Carbon dioxide (CO 2 ) 387 ppmv (0.0387%) Argon (Ar), Neon (Ne),
Respiratory system Premedical - Biology Composition of atmosphere Nitrogen (N 2 ) 840 ppmv (78.084%) Oxygen (O 2 ) 209,460 ppmv (20.946%) Carbon dioxide (CO 2 ) 387 ppmv (0.0387%) Argon (Ar), Neon (Ne),
PROBLEM SET 9. SOLUTIONS April 23, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
25/4/2016. Physiology #01 Respiratory system Nayef Garaibeh Rawan Alwaten
 25/4/2016 Physiology #01 Respiratory system Nayef Garaibeh Rawan Alwaten Respiratory System Introduction: - We breath while we are sleeping, talking, working and resting. - Respiratory diseases are abundant
25/4/2016 Physiology #01 Respiratory system Nayef Garaibeh Rawan Alwaten Respiratory System Introduction: - We breath while we are sleeping, talking, working and resting. - Respiratory diseases are abundant
Monday, ! Today: Respiratory system! 5/20/14! Transport of Blood! What we ve been covering! Circulatory system! Parts of blood! Heart! tubing!
 Monday, 5.19.14! What we ve been covering! Circulatory system! Parts of blood! Heart! tubing! Transport of Blood! What is transported! Nutrients! Oxygen! Carbon Dioxide! Hormones! Antibodies! What it is/does!
Monday, 5.19.14! What we ve been covering! Circulatory system! Parts of blood! Heart! tubing! Transport of Blood! What is transported! Nutrients! Oxygen! Carbon Dioxide! Hormones! Antibodies! What it is/does!
The Respiratory System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 13 The Respiratory System Slides 13.1 13.30 Lecture Slides in PowerPoint by Jerry L. Cook Organs of the Respiratory system
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 13 The Respiratory System Slides 13.1 13.30 Lecture Slides in PowerPoint by Jerry L. Cook Organs of the Respiratory system
Respiratory System Study Guide, Chapter 16
 Part I. Clinical Applications Name: Respiratory System Study Guide, Chapter 16 Lab Day/Time: 1. A person with ketoacidosis may hyperventilate. Explain why this occurs, and explain why this hyperventilation
Part I. Clinical Applications Name: Respiratory System Study Guide, Chapter 16 Lab Day/Time: 1. A person with ketoacidosis may hyperventilate. Explain why this occurs, and explain why this hyperventilation
4. For external respiration to occur effectively, you need three parameters. They are:
 Self Assessment Module D Name: ANSWER KEY 1. Hypoxia should be assumed whenever the PaO 2 is below 45 mm Hg. 2. Name some clinical conditions that will result in hyperventilation (respiratory alkalosis).
Self Assessment Module D Name: ANSWER KEY 1. Hypoxia should be assumed whenever the PaO 2 is below 45 mm Hg. 2. Name some clinical conditions that will result in hyperventilation (respiratory alkalosis).
Rodney Shandukani 14/03/2012
 Rodney Shandukani 14/03/2012 OXYGEN THERAPY Aerobic metabolism accounts for 90% of Oxygen consumption by tissues. generates ATP by oxidative phosphorylation. Oxygen cascade: Oxygen exerts a partial pressure,
Rodney Shandukani 14/03/2012 OXYGEN THERAPY Aerobic metabolism accounts for 90% of Oxygen consumption by tissues. generates ATP by oxidative phosphorylation. Oxygen cascade: Oxygen exerts a partial pressure,
